Pancreatitis: Symptoms, Causes & Treatment
Understand pancreatitis: acute and chronic inflammation, symptoms, causes, diagnosis, and treatment options.
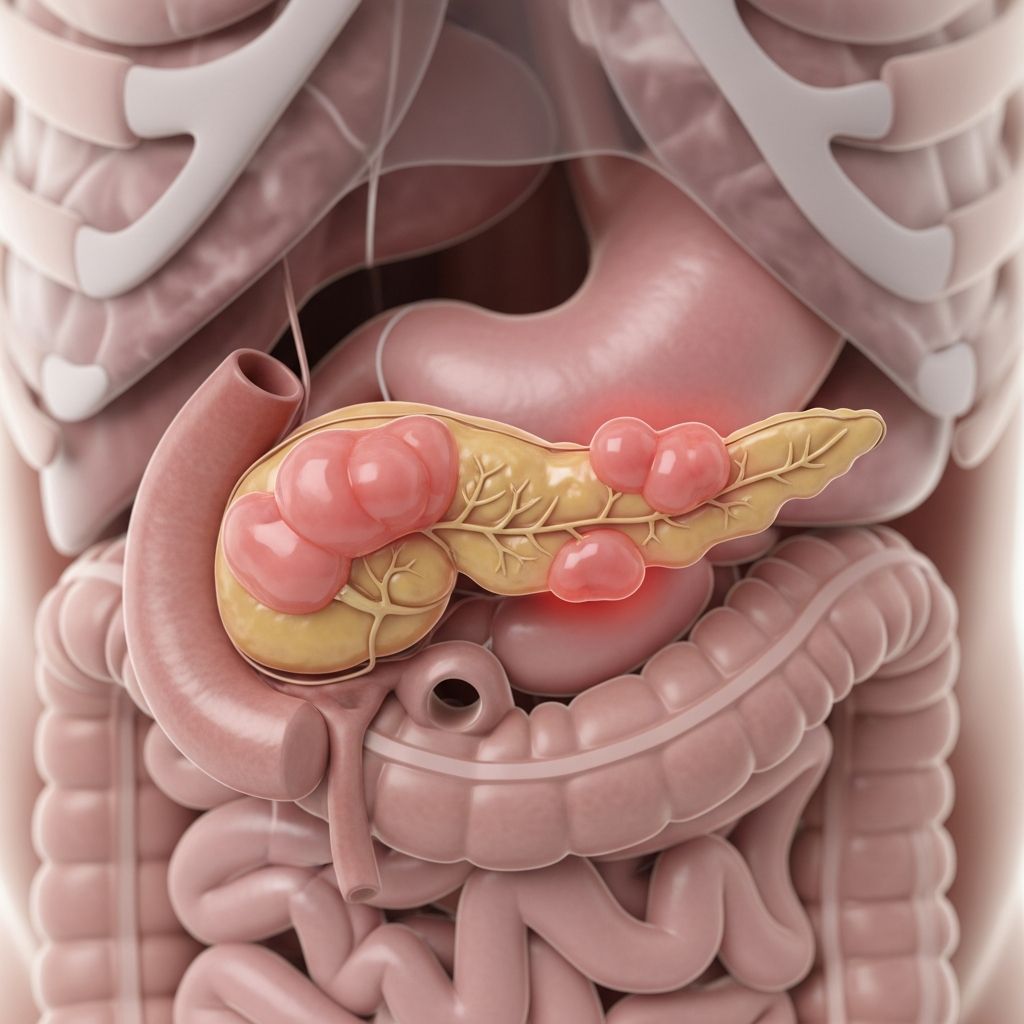
Understanding Pancreatitis
Pancreatitis is a painful inflammation of the pancreas, a vital organ located in the middle of your abdomen behind the stomach. This condition occurs when pancreatic enzymes become activated within the pancreas itself, causing inflammation and damage to pancreatic tissue. Pancreatitis can develop suddenly (acute pancreatitis) or persist over a long period (chronic pancreatitis), each presenting distinct characteristics, progression patterns, and treatment approaches.
The pancreas plays a crucial role in your digestive system and overall health by producing enzymes that aid digestion and hormones like insulin that regulate blood sugar levels. When the pancreas becomes inflamed, these essential functions are compromised, leading to various symptoms and complications that require prompt medical attention and specialized care.
Types of Pancreatitis
Acute Pancreatitis
Acute pancreatitis develops suddenly and typically resolves within a few weeks with appropriate treatment. Most cases of acute pancreatitis present as mild to moderate inflammation that responds well to conservative management. However, approximately 1 in 5 cases progresses to severe acute pancreatitis, which can result in serious complications and potentially life-threatening situations.
The severity of acute pancreatitis varies considerably among patients, and healthcare providers cannot always predict which cases will develop complications. Factors influencing severity include the extent of pancreatic damage, the presence of infection, and the development of fluid collections or tissue necrosis.
Chronic Pancreatitis
Chronic pancreatitis involves long-term inflammation of the pancreas, leading to permanent structural and functional changes in pancreatic tissue. Unlike acute pancreatitis, chronic pancreatitis develops gradually over months or years and causes progressive damage. While complications develop more slowly than in acute pancreatitis, they are generally manageable with appropriate medical and surgical interventions, and most are not directly life-threatening.
Chronic pancreatitis often results from prolonged inflammation caused by alcohol use, genetic factors, or autoimmune conditions. Research indicates that 80 to 90 percent of patients with chronic pancreatitis experience chronic pain related to pancreatic duct obstruction, necessitating comprehensive pain management strategies.
Symptoms of Pancreatitis
Acute Pancreatitis Symptoms
The most common presentation of acute pancreatitis is sudden onset of severe abdominal pain, typically beginning under the left rib cage or in the middle of the abdomen. This pain may radiate to the back and intensifies after eating, particularly foods high in fat. Additional symptoms accompanying acute pancreatitis include:
– Severe upper abdominal pain that radiates to the back- Nausea and vomiting- Fever- Rapid pulse- Abdominal tenderness and bloating- Loss of appetite
Chronic Pancreatitis Symptoms
Chronic pancreatitis symptoms typically develop gradually and may include chronic abdominal pain, digestive problems, and weight loss. Patients often experience recurring episodes of pain and gradually decreasing pancreatic function over time. Key symptoms include:
– Chronic abdominal pain in the upper left portion of the abdomen- Persistent digestive problems- Unintentional weight loss- Fatty, greasy stools- Loss of appetite- Progressive pancreatic insufficiency
Causes of Pancreatitis
Pancreatitis results from various triggers that activate pancreatic enzymes prematurely. Understanding the underlying cause is essential for effective treatment and prevention of recurrent episodes.
Common Causes of Acute Pancreatitis
– Gallstones blocking the pancreatic duct- Alcohol consumption- Medications (certain antibiotics, diuretics, corticosteroids)- Hypertriglyceridemia (elevated blood fat levels)- Abdominal trauma or surgery- Infections- High calcium levels in the blood- Certain genetic conditions- Unknown causes (idiopathic)
Common Causes of Chronic Pancreatitis
– Chronic alcohol use- Autoimmune pancreatitis- Genetic mutations affecting pancreatic function- Cystic fibrosis- Tobacco smoking- Chronic obstruction of the pancreatic duct- Hereditary pancreatitis- Recurrent acute pancreatitis episodes
Complications of Pancreatitis
Acute Pancreatitis Complications
While most cases of acute pancreatitis resolve without significant complications, severe cases can develop serious conditions including:
– Acute necrotizing fluid collection (necrosis of pancreatic tissue)- Walled-off pancreatic necrosis- Infected pancreatic tissue- Fluid collections around the pancreas (pseudocysts)- Organ failure- Severe systemic inflammation- Death in severe cases
Chronic Pancreatitis Complications
Chronic pancreatitis leads to progressive complications that develop over time, including:
– Chronic pain requiring ongoing management- Pancreatic insufficiency affecting digestion and nutrition absorption- Diabetes from loss of insulin-producing cells- Pancreatic cancer risk increases with duration of disease- Malabsorption and nutritional deficiencies- Chronic opioid dependence from pain management- Psychological complications from chronic pain- Bile duct obstruction- Pancreatic ductal strictures
Diagnosis of Pancreatitis
Diagnostic Criteria
Acute pancreatitis diagnosis requires meeting specific criteria established by medical professionals. The definition involves three key components, and a diagnosis is confirmed when at least two of the following three criteria are present:
– Classic abdominal pain characteristic of pancreatitis- Elevated pancreatic enzymes (amylase and lipase) at least three times the upper limit of normal in blood tests- Imaging findings showing pancreatic inflammation and swelling on CT scan, MRI, or ultrasound
Blood Tests
Pancreatic blood tests measure elevated levels of pancreatic enzymes, primarily amylase and lipase. These enzymes are released when pancreatic tissue is damaged. Significantly elevated levels—at least three times higher than normal—strongly suggest pancreatitis and help differentiate it from other abdominal conditions.
Imaging Tests
CT Scan — Computed tomography imaging can identify pancreatic swelling, inflammation, and complications including fluid around the pancreas, abscesses, or pseudocysts. CT imaging is particularly valuable for assessing the severity of acute pancreatitis and detecting complications requiring intervention.
ERCP (Endoscopic Retrograde Cholangiopancreatography) — During ERCP, a tube is inserted down the throat into the stomach and then into the small intestine. Dye is injected to visualize the bile and pancreatic ducts on X-rays, allowing physicians to identify obstructions or abnormalities.
Endoscopic Ultrasound — A scope is inserted down the throat into the stomach, and sound waves produce detailed images of abdominal organs. This technique can reveal gallstones and diagnose chronic pancreatitis when invasive testing might worsen the condition.
Magnetic Resonance Cholangiopancreatography (MRCP) — This non-invasive imaging technique uses magnetic resonance imaging to visualize the pancreatic and bile ducts without requiring endoscopy or dye injection.
MRI — Magnetic resonance imaging provides detailed cross-sectional images showing pancreatic structure, inflammation, and fluid collections without using radiation.
Treatment of Pancreatitis
Acute Pancreatitis Treatment
The mainstay of treatment for acute pancreatitis relies on three fundamental pillars that address the immediate needs of the inflamed pancreas and support the body’s healing process:
1. Aggressive Fluid Hydration
Early aggressive hydration is critical in acute pancreatitis management. Treatment typically begins with an initial fluid bolus followed by intravenous maintenance fluids at rates of 250 to 500 mL per hour. Adequate hydration helps prevent organ dysfunction, reduces complications, and supports pancreatic recovery. Fluid management is carefully monitored and adjusted based on individual patient response and clinical parameters.
2. Early Nutritional Support
Healthcare providers prioritize early nutrition initiation, ideally within the first 24 hours of hospitalization. Oral feeding, when tolerated, is preferred over intravenous nutrition. A low-fat, high-protein diet is typically recommended. If oral feeding isn’t possible, tube feeding may be initiated to ensure adequate nutritional support during the recovery period.
3. Pain Management
Effective pain control is essential for patient comfort and recovery. Medications are administered to manage pain while healthcare providers address the underlying inflammation. Pain management strategies vary based on individual patient needs and response to initial treatments.
Treatment for Complications
When severe acute pancreatitis develops fluid collections, infections, or other complications, intervention becomes necessary. If pancreatic necrosis becomes infected, or if fluid collections grow large enough to compress the stomach, small bowel, or bile ducts causing jaundice, medical or surgical intervention is required to prevent serious complications and support patient recovery.
Chronic Pancreatitis Treatment
Non-Surgical Management
Initial treatment of chronic pancreatitis focuses on managing pain and supporting pancreatic function through non-surgical approaches. Key strategies include:
Enzyme Replacement — Pancreatic enzyme supplements compensate for reduced enzyme production, improving digestion and nutrient absorption. These medications are taken with meals to enhance digestive function and nutritional status.
Chronic Pain Management — Multiple approaches address chronic pancreatitis pain, including medications, celiac plexus blockade (injection of anesthetic around nerves supplying the pancreas), splanchnic radiofrequency ablation, and spinal cord stimulation. These interventions target different pain pathways to provide comprehensive relief.
Risk Factor Modification — A critical component of chronic pancreatitis management involves eliminating alcohol consumption, the most significant modifiable risk factor. Smoking cessation is also essential, along with dietary modifications to reduce pancreatic stress.
Surgical and Advanced Treatments
When conservative management fails to control symptoms adequately, several surgical options may be considered:
Total Pancreatectomy with Islet Autotransplantation — This procedure involves complete removal of the pancreas followed by transplantation of insulin-producing islet cells. Candidates undergo comprehensive evaluation including mixed meal testing to assess pancreatic function, glucose tolerance assessment, and differential pain block testing to determine pain origin before proceeding with surgery.
Partial Pancreatic Resection — Depending on the location and extent of disease, partial removal of the pancreas may alleviate symptoms while preserving some pancreatic function.
Whipple Procedure (Pancreaticoduodenectomy) — This extensive surgical procedure may be performed for pancreatic cancer, severe chronic pancreatitis with ductal obstruction, or large cysts, involving removal of the pancreatic head, part of the small intestine, and surrounding tissue.
Endoscopic Interventions — Minimally invasive endoscopic procedures can relieve ductal obstructions, remove stones, or place stents to improve pancreatic duct drainage without requiring major surgery.
Living with Pancreatitis
Dietary Recommendations
Dietary management plays a crucial role in pancreatitis recovery and management. A low-fat, high-protein diet is recommended for patients with pancreatitis. Foods to avoid include fried foods, full-fat dairy products, fatty meats, and foods high in triglycerides. Focus on lean proteins, whole grains, fruits, vegetables, and healthy fats in moderation to support pancreatic health and reduce symptom recurrence.
Recovery Timeline for Acute Pancreatitis
Mild acute pancreatitis typically requires hospitalization for 3 to 5 days. Patients gradually resume eating and are discharged once they tolerate oral intake and pain is controlled. Severe cases with complications may require extended hospitalization lasting 1-2 weeks or longer, depending on the extent of pancreatic damage and infection management.
Prevention Strategies
Preventing pancreatitis recurrence involves addressing underlying causes. Limit alcohol consumption or abstain completely, maintain healthy triglyceride levels through diet and medication if necessary, avoid medications known to trigger pancreatitis, and manage gallstone disease through appropriate medical or surgical intervention when indicated.
Frequently Asked Questions
Q: What is the difference between acute and chronic pancreatitis?
A: Acute pancreatitis develops suddenly and usually resolves within weeks with treatment. Chronic pancreatitis develops gradually over years and causes permanent pancreatic damage, requiring long-term management and monitoring.
Q: How long does it take to recover from acute pancreatitis?
A: Mild acute pancreatitis typically resolves in 3-5 days with hospitalization. Severe cases with complications may require longer recovery periods lasting weeks or months, depending on the extent of pancreatic damage and infection.
Q: Can pancreatitis be prevented?
A: While not all pancreatitis can be prevented, you can reduce risk by limiting or eliminating alcohol, managing gallstone disease, maintaining healthy triglyceride levels, and avoiding medications known to trigger pancreatitis when possible.
Q: Is pancreatitis life-threatening?
A: Most cases of acute pancreatitis are not life-threatening when treated appropriately. However, severe acute pancreatitis can be serious and potentially fatal without proper medical intervention. Chronic pancreatitis is generally manageable and not directly life-threatening, though complications require ongoing treatment.
Q: What foods should I avoid with pancreatitis?
A: Avoid fried foods, full-fat dairy, fatty meats, foods high in triglycerides, and spicy foods. Focus on lean proteins, whole grains, fruits, and vegetables while limiting fat intake to support pancreatic recovery and reduce symptom recurrence.
Q: Can I resume alcohol consumption after recovering from pancreatitis?
A: This depends on the cause of your pancreatitis. If alcohol was the trigger, complete abstinence is strongly recommended. If caused by other factors like gallstones, moderate alcohol consumption may be acceptable, but discuss this with your healthcare provider.
Q: What imaging tests diagnose pancreatitis?
A: CT scans, MRI, ultrasound, ERCP, and endoscopic ultrasound can all diagnose pancreatitis. Your healthcare provider will select appropriate imaging based on your specific situation and clinical presentation.
Q: Are there new treatments available for chronic pancreatitis?
A: Yes, treatment options continue to evolve, including advanced pain management techniques, minimally invasive endoscopic procedures, and surgical innovations like robotic-assisted surgery and islet autotransplantation for carefully selected patients.
References
- Pancreatitis: Symptoms, Causes & Treatment — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/8103-pancreatitis
- Pancreatic Diseases – Cleveland Clinic — Cleveland Clinic Digestive Disease Institute. 2024. https://my.clevelandclinic.org/departments/digestive/depts/pancreatic-diseases
- Pancreatitis Symptoms, Causes, Treatment and More — Cleveland Clinic Butts and Guts Podcast. 2024. https://my.clevelandclinic.org/podcasts/butts-and-guts/pancreatitis-symptoms-causes-treatment-and-more
- What fluids should I order for my patient with acute pancreatitis? — Cleveland Clinic Journal of Medicine. 2024. https://www.ccjm.org/content/91/8/466
- The Best (and Worst) Foods for Pancreatitis Pain — Cleveland Clinic Health Hub. 2024. https://health.clevelandclinic.org/best-and-worst-foods-for-pancreatitis-pain
- Approaches to the Treatment of Chronic Pancreatitis — Cleveland Clinic Medical Education. 2024. https://www.youtube.com/watch?v=9iBZ6AzduyM
Read full bio of Sneha Tete











