Pancreatitis Symptoms: 8 Key Signs Of Pain, Nausea & More
Recognizing the signs of acute and chronic pancreatitis: Pain, digestive issues, and when to seek urgent care for this pancreatic inflammation.
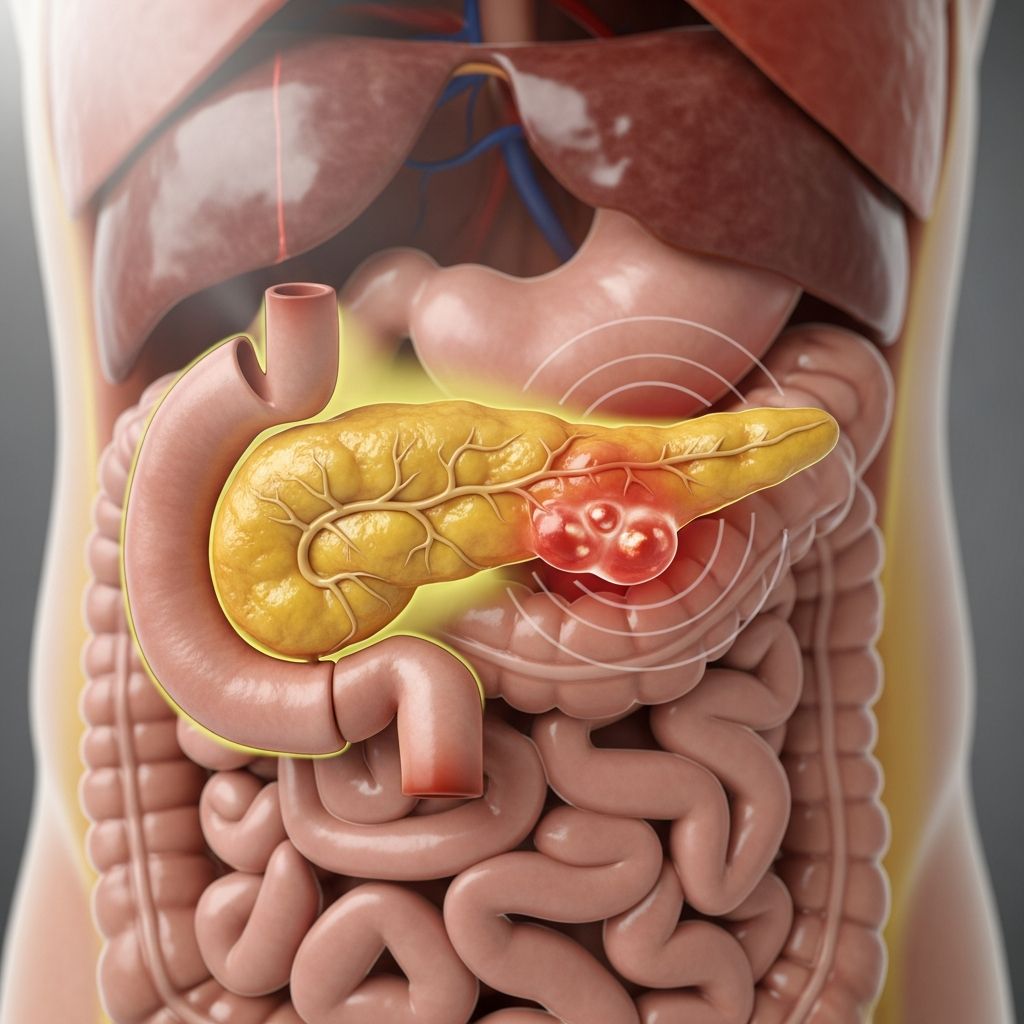
Pancreatitis Symptoms: What to Know About Pain, Nausea, and More
Pancreatitis is inflammation of the pancreas, a vital organ behind the stomach that produces digestive enzymes and hormones like insulin. This condition can be acute, onsetting suddenly and severely, or chronic, developing gradually with lasting damage. Recognizing symptoms early is crucial, as acute cases affect about 275,000 U.S. hospital stays annually, with 20% severe, while chronic cases lead to 86,000 stays. Common culprits include gallstones and excessive alcohol use.
What Is Pancreatitis?
The pancreas aids digestion by releasing enzymes into the small intestine to break down fats, proteins, and carbohydrates, and regulates blood sugar via insulin and glucagon. In pancreatitis, these enzymes activate prematurely within the pancreas, causing it to digest itself, leading to swelling, pain, and potential complications. Acute pancreatitis is typically short-term and reversible with treatment, while chronic involves irreversible scarring and reduced function.
Pancreatitis Symptoms
Symptoms vary by type but often center on abdominal discomfort. Pain is the hallmark, described as penetrating or burning.
Symptoms of Acute Pancreatitis
Acute pancreatitis strikes suddenly with intense upper abdominal pain, often radiating to the back, lasting days. It feels like one of the worst pains possible. Accompanying signs include:
- Sudden, severe epigastric pain spreading to back, chest, or sides
- Nausea and vomiting, sometimes with anorexia
- Fever, rapid heartbeat, sweating, and weakness
- Tender abdomen, possibly with guarding or distension
Pain worsens when lying down or eating, easing when leaning forward or sitting up. Alcohol-related cases may develop slower. Severe cases show Cullen’s sign (periumbilical bruising) or Grey-Turner’s sign (flank bruising), indicating hemorrhage.
Symptoms of Chronic Pancreatitis
Chronic pancreatitis features persistent or recurrent upper abdominal pain radiating to the back, varying in intensity and worsening after meals. The pancreas’s damage impairs enzyme and insulin production, causing:
- Constant or episodic pain with relief periods
- Steatorrhea: greasy, oily, floating stools from poor fat digestion
- Diarrhea, unintended weight loss, and nutrient deficiencies
- Blood sugar elevation, new or worsening diabetes
Symptoms progress slowly; some are asymptomatic until diagnosed incidentally. Smoking exacerbates it, raising pancreatic cancer risk.
Acute vs. Chronic Pancreatitis: Key Differences
Acute pancreatitis is a sudden inflammatory episode, often resolving with care, while chronic is ongoing damage. Use this table for comparison:
| Aspect | Acute Pancreatitis | Chronic Pancreatitis |
|---|---|---|
| Onset | Sudden, severe | Gradual, recurrent |
| Pain | Intense, constant, radiates to back | Intermittent or constant, post-meal worsening |
| Digestive Symptoms | Nausea, vomiting | Oily stools, diarrhea, weight loss |
| Duration/Outcome | Days to weeks, often reversible | Months to years, irreversible |
| Complications | Necrosis, infection, organ failure | Diabetes, malnutrition, cancer risk |
When to See a Doctor
Seek immediate care for severe abdominal pain with nausea, vomiting, fever, rapid pulse, or jaundice—these signal potential life-threatening issues. For chronic symptoms like persistent pain, oily stools, or unexplained weight loss, consult a doctor promptly. High-risk individuals (heavy drinkers, gallstone patients) should monitor closely. Emergency signs include dizziness, distension, or breathing issues.
Causes of Pancreatitis
Gallstones block pancreatic ducts in 40-70% of acute cases; alcohol causes 30% acutely and 50-70% chronically. Other triggers:
- High triglycerides, medications, infections
- Genetic factors, autoimmune issues, trauma
- ERCP procedures or hypercalcemia
Idiopathic cases occur in 10-30%.
How Pancreatitis Is Diagnosed
Diagnosis combines history, exams, and tests. Blood checks amylase/lipase (elevated 3x normal suggests it). Imaging like CT/MRI shows swelling or fluid. Ultrasound detects gallstones; EUS or MRCP for ducts. Stool tests assess chronic malabsorption.
Pancreatitis Treatment
Acute treatment is supportive: IV fluids, pain meds, NPO (nothing by mouth) initially, then low-fat diet. Address causes—gallstone removal, alcohol cessation. Chronic management includes enzyme supplements, insulin if needed, pain control, and antioxidants. Surgery for complications like pseudocysts or cancer screening. Lifestyle: quit smoking, limit alcohol, manage weight.
Pancreatitis Complications
Acute: necrosis (20% severe), infection, pseudocysts, organ failure. Chronic: exocrine insufficiency (malnutrition), endocrine (diabetes), pseudocysts, cancer (increased risk).
Pancreatitis Prevention
Avoid excess alcohol, manage gallstones/cholesterol, control triglycerides. Heavy drinkers should limit to <3 drinks/day women, <4 men, ideally abstain. Healthy diet, no smoking.
Frequently Asked Questions (FAQs)
What does pancreatitis pain feel like?
It’s severe upper abdominal pain radiating to the back, worse lying down, better leaning forward. Acute is sudden and piercing; chronic recurrent.
How long does acute pancreatitis last?
Symptoms last days to weeks with treatment; full recovery varies.
Can pancreatitis go away on its own?
Mild acute cases may, but medical care is essential to prevent severity.
Does chronic pancreatitis cause weight loss?
Yes, from malabsorption and poor nutrient uptake.
Is pancreatitis curable?
Acute often yes; chronic is managed, not cured.
References
- Pancreatitis – Acute and Chronic — American College of Gastroenterology. Accessed 2026. https://gi.org/topics/pancreatitis-acute-and-chronic/
- Pancreatitis – symptoms, causes and treatment — healthdirect.gov.au (Australian Government). Accessed 2026. https://www.healthdirect.gov.au/pancreatitis
- Pancreatitis: Symptoms, Causes & Treatment — Cleveland Clinic. 2023-10-17. https://my.clevelandclinic.org/health/diseases/8103-pancreatitis
- Acute Pancreatitis — StatPearls, NCBI Bookshelf, NIH. 2023-07-04. https://www.ncbi.nlm.nih.gov/books/NBK482468/
Read full bio of Sneha Tete











