Papular Mucinosis Pathology: Essential Guide To Diagnosis
Detailed pathology of papular mucinosis, from localised papules to generalised scleromyxoedema with mucin deposits.
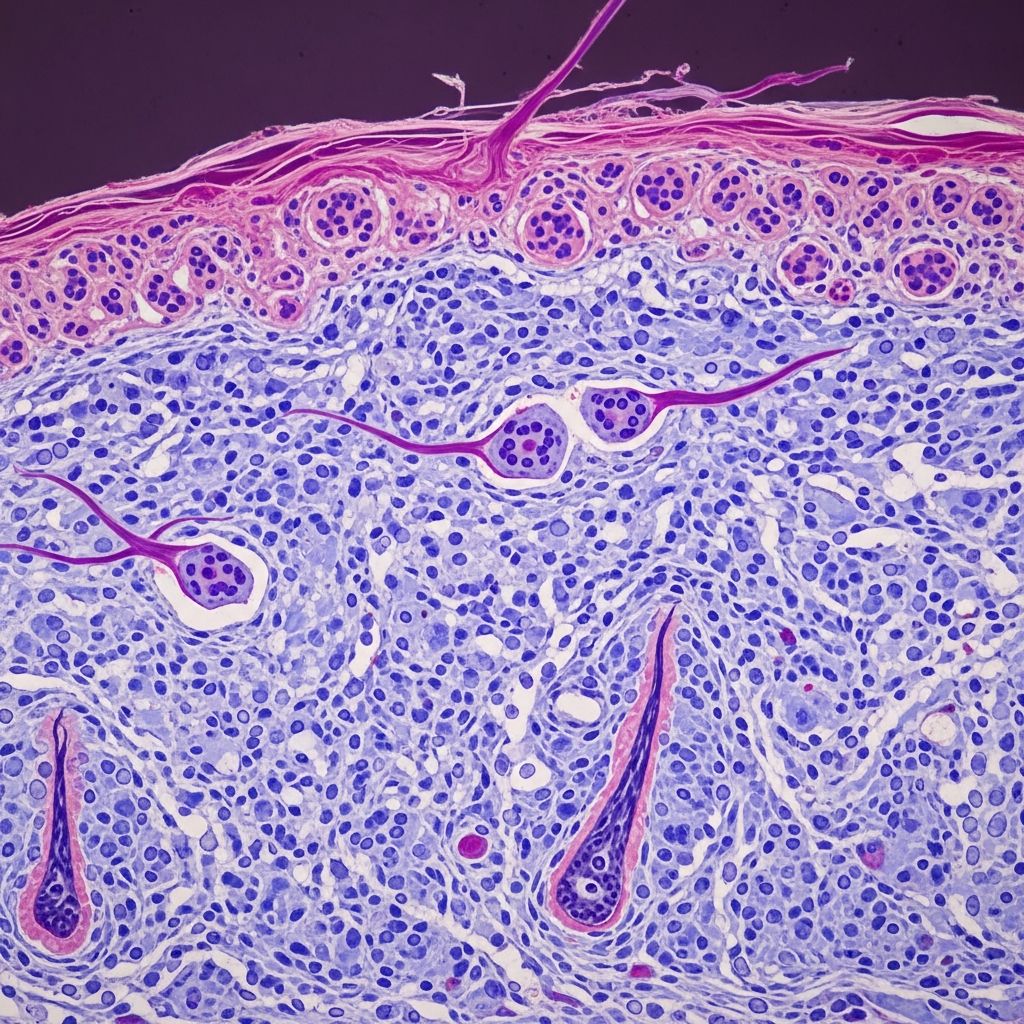
Papular mucinosis pathology
Author: Dr Ian McColl, Dermatopathologist, Pathodermatopathology, Auckland, New Zealand.
DermNet NZ Editor: Dr Martin Keighley, Dermatologist, Hamilton, New Zealand. Last updated: December 2023.
What is papular mucinosis?
Papular mucinosis, also known as lichen myxoedematosus, is a rare dermatological condition characterised by abnormal mucin deposition within the dermis of the skin. Mucin, a gel-like substance primarily composed of glycosaminoglycans such as hyaluronic acid, accumulates due to dysregulated fibroblast activity. This leads to the formation of distinctive cutaneous lesions ranging from discrete papules in localised forms to widespread thickening in generalised variants.
The disorder encompasses a spectrum of presentations. Localised papular mucinosis typically manifests as firm, waxy, flesh-coloured papules confined to specific areas, often without systemic involvement. In contrast, the generalised form, termed scleromyxoedema, features profuse papules arranged in linear or reticulate patterns across the body, accompanied by progressive dermal fibrosis and frequent association with monoclonal gammopathy.
Histopathologically, the hallmark is increased mucin in the dermis, best highlighted by histochemical stains like colloidal iron or Alcian blue at pH 2.5. Early lesions show subtle superficial dermal mucinosis, while advanced stages reveal fibroblast proliferation, collagen bundles, and thickened dermis. This condition must be differentiated from other mucinoses, such as those linked to thyroid disease, through clinical correlation and laboratory evaluation.
Clinical features
Papular mucinosis presents with varied morphologies depending on the subtype. Localised forms often appear as 2–4 mm dome-shaped or flat-topped papules, translucent or waxy, commonly on the trunk, extremities, or acral sites. They may coalesce into plaques or nodules but lack systemic symptoms.
- Discrete papular mucinosis: Scattered papules on trunk and arms.
- Acral persistent papular mucinosis (APPM): Persistent flesh-coloured papules on dorsal hands, wrists, and forearms; asymptomatic and chronic.
- Self-healing papular mucinosis: Transient lesions resolving spontaneously, seen in juvenile or adult forms.
The generalised scleromyxoedema variant is more severe, with symmetric 2–3 mm papules in linear arrays on the face, neck, arms, hands, and legs. Facial involvement leads to leonine facies due to furrowed thickening around the glabella and nose. Skin induration mimics scleroderma, with reduced joint mobility, erythema, and pruritus. Extracutaneous features include monoclonal paraproteinaemia (IgG lambda in ~80% cases), oesophageal dysmotility, pulmonary hypertension, and rarely plasma cell dyscrasia progression.
Unlike thyroid-associated pretibial myxoedema, papular mucinosis shows no thyroid dysfunction and features fibroblast hyperplasia. Lesions are chronic, with localised forms persisting cosmetically and generalised types potentially fatal from systemic complications.
Histology of papular mucinosis
Microscopic examination reveals a characteristic triad: mucin deposition, fibroblast proliferation, and collagen alterations. Early lesions display focal mucin pools in the superficial dermis, subtle and potentially overlooked without special stains.
In established lesions:
- Epidermis: Normal, acanthotic (thickened), or atrophic; no significant changes like hyperkeratosis.
- Dermis: Diffuse mucin throughout papillary and reticular dermis, staining metachromatically with toluidine blue or Alcian blue. Fibroblasts are increased and stellate, producing excess glycosaminoglycans. Collagen fibres are thickened, clumped, and vertically oriented, contributing to sclerosis.
- Infiltrate: Sparse superficial perivascular lymphocytes and plasma cells; no significant inflammation.
Scanning power view shows uniform dermal expansion by pale mucinous material with scattered fibroblasts (figures 1–2). High power highlights stringy mucin separating collagen bundles, with enlarged, irregular fibroblasts.


Special stains for papular mucinosis
Histochemical stains confirm mucin nature:
| Stain | Result | Purpose |
|---|---|---|
| Colloidal iron (Perls) | Blue staining of mucin | Highlights hyaluronic acid-rich mucin |
| Alcian blue (pH 2.5) | Blue mucin deposits | Demonstrates acid mucopolysaccharides |
| Toluidine blue | Metachromatic (red-purple) | Confirms glycosaminoglycan composition |
| Hyaluronidase digestion | Abolishes staining | Differentiates from sulphated mucins (e.g., pretibial myxoedema) |
These stains are crucial as routine H&E may underestimate mucin in early or subtle cases. Immunohistochemistry shows increased CD34+ fibroblasts, but is not diagnostic.
Differential diagnosis
Papular mucinosis mimics other mucin-depositing disorders:
- Focal mucinosis: Solitary lesion; lacks fibroblast proliferation and collagen changes; no clinical papules elsewhere.
- Generalised/pretibial myxoedema: Thyroid disease association; mucin without fibroblasts; epidermal hyperkeratosis, follicular plugging.
- Dermatan sulphate mucinosis: Deeper reticular dermis involvement; resistant to hyaluronidase.
- Scleroderma/morphea: Thicker collagen without mucin; Raynaud phenomenon.
- Lichen simplex chronicus: Hypergranulosis, acanthosis; itch history.
Clinicopathological correlation is essential, with serum protein electrophoresis to exclude gammopathy in generalised forms.
Variants of lichen myxoedematosus
Lichen myxoedematosus (LM) classifies into localised and generalised:
Localised LM
Monoclonal gammopathy and thyroid disease absent:
- Discrete papular: Widespread but non-sclerotic papules.
- Acral persistent papular mucinosis: Hands/forearms; flesh papules persisting years; favourable prognosis.
- Self-healing: Resolves spontaneously; juvenile (arthralgias) or adult.
- Infantile: Rare, early-onset papules.
- Nodular: Limb/trunk nodules; mild papules.
Generalised (scleromyxoedema)
Generalised papules with sclerosis, monoclonal gammopathy (83%), systemic risks.
Management
Treatment targets symptoms and underlying factors:
- Localised: Topical/intralesional corticosteroids (e.g., halobetasol); CO2 laser; observation if asymptomatic.
- Generalised: IV immunoglobulin (effective); retinoids, methotrexate, thalidomide; treat gammopathy (chemotherapy if progressing).
Prognosis varies: localised benign; scleromyxoedema guarded due to extracutaneous disease.
Frequently asked questions
What causes papular mucinosis?
Unknown; generalised linked to IgG lambda paraprotein stimulating fibroblasts.
Is papular mucinosis curable?
Localised often persistent but benign; generalised managed but not cured; self-healing variants resolve.
Does it affect internal organs?
Primarily skin in localised; generalised may involve oesophagus, lungs, heart.
How is it diagnosed?
Biopsy with mucin stains; exclude thyroid/gammopathy.
What is the outlook?
Localised cosmetic; generalised variable, monitor for malignancy.
References
- Papular mucinosis pathology — DermNet NZ. 2023-12. https://dermnetnz.org/topics/papular-mucinosis-pathology
- Papular mucinosis — PubMed/NCBI (via PMC). 2024. https://pmc.ncbi.nlm.nih.gov/articles/PMC12440319/
- Lichen Myxedematosus — Next Steps in Dermatology. 2023. https://nextstepsinderm.com/jdd-corner/lichen-myxedematosus/
- Acral Persistent Papular Mucinosis in the United States — NIH/PMC. 2024. https://pmc.ncbi.nlm.nih.gov/articles/PMC12440319/
- Papular Mucinosis: A Clinicopathologic Study — JAMA Dermatology. 2005. https://jamanetwork.com/journals/jamadermatology/fullarticle/542778
Read full bio of medha deb










