Surgical Approaches for Pediatric Eye Muscle Misalignment
Understanding recession and resection procedures for children with strabismus
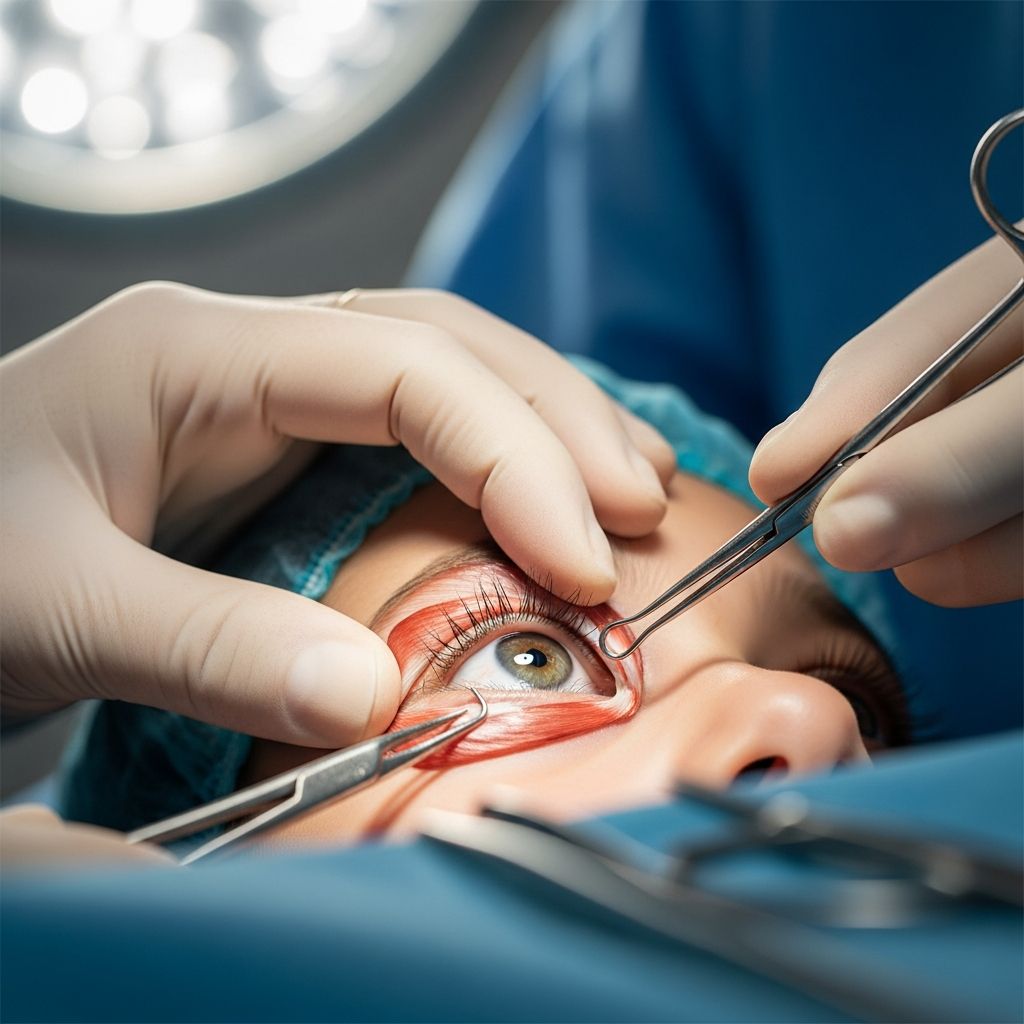
Eye muscle misalignment in children, known as strabismus, affects approximately 3-4% of the pediatric population. When nonsurgical interventions fail to correct the deviation, surgical correction becomes necessary to restore proper eye alignment and prevent long-term visual complications. Two fundamental surgical techniques form the foundation of strabismus management: muscle recession and muscle resection. Understanding these procedures, their applications, and their outcomes is essential for parents and healthcare providers involved in pediatric eye care.
Understanding Muscle Recession and Resection Techniques
Strabismus surgery works by altering the position and function of the extraocular muscles that control eye movement. The two primary surgical methods differ fundamentally in how they modify muscle mechanics.
Muscle Recession involves weakening an overacting muscle by repositioning its attachment point further back on the eye surface. During this procedure, the surgeon detaches the muscle from its original insertion site and reattaches it posteriorly (toward the back of the eye). This increased distance from the muscle’s action point reduces its mechanical force, effectively weakening its pull on the eyeball. Recession is the preferred initial approach for muscles that are overacting or pulling the eye in an unwanted direction.
Muscle Resection strengthens an underacting muscle by shortening its length and reattaching it at its original position. The surgeon creates a new suture point along the muscle, removes or folds the excess tissue between this point and the eye, and reattaches the shortened muscle to the eyeball. This technique effectively increases the muscle’s contractile strength and pulling force, making it useful for correcting muscles that are not functioning adequately.
Clinical Indications and Patient Selection Criteria
The choice between recession and resection—or combinations of both—depends on several clinical factors including the magnitude of deviation, the specific muscles involved, and the patient’s age at presentation.
Determining Appropriate Surgical Magnitude
For children with moderate-angle deviations up to 25 prism diopters, unilateral lateral rectus recession demonstrates high efficacy. Studies show that unilateral lateral rectus recession can successfully treat exotropia angles between 15 and 25 prism diopters, with success rates ranging from approximately 72-90% depending on the specific angle and surgical precision. Treatment protocols typically involve:
- 7 mm recession for deviations of 15 prism diopters or less
- 8 mm recession for deviations between 16-20 prism diopters
- 9 mm recession for deviations between 21-25 prism diopters
For larger residual deviations exceeding 15 prism diopters, bilateral surgical procedures generally produce more predictable and substantial corrections. Bilateral lateral rectus resection of 5, 6, and 7 mm yields mean corrections of approximately 19.75, 28.75, and 33.5 prism diopters respectively.
Age Considerations in Surgical Planning
The timing and approach to strabismus surgery in children varies based on age. Young children (typically under 5 years) often demonstrate higher surgical success rates with unilateral procedures, achieving success rates as high as 86.2% in some cohorts. This may reflect differences in neuromuscular plasticity, healing responses, or the natural history of the condition in younger patients. However, the precise mechanisms underlying these age-related differences remain incompletely understood, and randomized controlled trials comparing outcomes across different age groups are warranted.
Management of Residual and Recurrent Deviation
Despite optimal initial surgical planning, some children develop residual esotropia (inward deviation) or exotropia (outward deviation) that persists or recurs after the first surgery. Approximately 25-30% of patients may require additional surgical intervention.
Sequential Surgical Strategies
When initial medial rectus recession fails to achieve adequate alignment, lateral rectus resection becomes a logical second-stage procedure. Research examining children who underwent subsequent lateral rectus resection following initial medial rectus recession found that:
- Unilateral lateral rectus resection of 4-7 mm corrects approximately 10.5-14.9 prism diopters on average
- Bilateral lateral rectus resection provides significantly greater correction, with each additional millimeter of resection producing approximately 7.3 additional prism diopters of correction
- Residual deviations larger than 15 prism diopters respond better to bilateral rather than unilateral surgery
The timing between initial and secondary surgery varies considerably, with mean intervals of approximately 24 months between procedures, though some children may require intervention within 2 months of initial surgery while others may not need a second procedure for over 10 years.
Managing Variable Surgical Responses
Individual responses to strabismus surgery can be remarkably variable on a case-by-case basis, even when using standardized surgical magnitudes. Unilateral resection procedures show somewhat less predictable outcomes than bilateral approaches, suggesting inherent biological variability in how individual extraocular muscles respond to surgical modification. This variability underscores the importance of careful preoperative planning, precise surgical technique, and systematic postoperative monitoring to identify inadequate corrections early.
Surgical Outcomes and Success Metrics
| Procedure Type | Deviation Range | Mean Correction | Success Rate |
|---|---|---|---|
| Unilateral Lateral Rectus Recession (4 mm) | Up to 15 PD | 12.0 PD | 86.2% |
| Unilateral Lateral Rectus Recession (5 mm) | Up to 15 PD | 13.3 PD | 86.2% |
| Unilateral Lateral Rectus Recession (6 mm) | Up to 15 PD | 14.9 PD | 86.2% |
| Bilateral Lateral Rectus Resection (5 mm) | 16-30 PD | 19.75 PD | Higher predictability |
| Bilateral Lateral Rectus Resection (6 mm) | 16-30 PD | 28.75 PD | Higher predictability |
| Bilateral Lateral Rectus Resection (7 mm) | Larger deviations | 33.5 PD | Higher predictability |
Success in strabismus surgery is typically defined as achieving a postoperative deviation of 10 prism diopters or less, representing functional eye alignment from the patient’s perspective. Complications remain relatively uncommon, with proper surgical technique and patient selection, though overcorrection to consecutive esotropia occurs in approximately 3.4% of cases undergoing unilateral procedures.
Surgical Technique Considerations
The technical execution of recession and resection procedures involves several standardized steps. Under general anesthesia, the surgeon makes a fornix incision to access the extraocular muscles. For recession, the muscle is carefully disinserted from the sclera and reattached at the predetermined distance posteriorly using absorbable sutures (typically 6-0 Vicryl). For resection, the new insertion point is marked along the muscle belly, excess muscle is removed or folded via plication, and the shortened muscle is reattached at its original anatomical insertion site. The precision of surgical measurement and suture placement directly impacts the magnitude of the refractive effect achieved.
Adjunctive Procedures and Pattern Deviations
In approximately 10-15% of cases, additional surgical modifications may be necessary to address associated vertical deviations or oblique dysfunction. Inferior oblique muscle surgery can be combined with lateral rectus resection in selected patients. Lateral rectus offset procedures address pattern strabismus (differences in alignment between upgaze and downgaze)—surgical modifications that fine-tune the vertical component of eye alignment alongside the primary horizontal correction.
Long-Term Outcomes and Recurrence Patterns
Published follow-up studies extending 2-3 years after unilateral lateral rectus recession demonstrate sustained success in the majority of patients. Mean postoperative deviations typically measure 3.5 prism diopters for distance fixation and 1.6 prism diopters for near fixation in successful cases. However, some patients demonstrate recurrence of deviation over extended follow-up periods, with longer-term recurrence rates tending to be lower in bilateral procedures compared to unilateral approaches.
Clinical Decision-Making Framework
Contemporary surgical decision-making integrates multiple factors into a comprehensive treatment plan:
- Deviation magnitude largely determines whether unilateral or bilateral surgery is appropriate
- Patient age influences expected success rates and choice of approach
- Muscle function assessment determines whether recession, resection, or combination procedures are needed
- Previous surgical history guides selection of muscles and magnitudes for secondary procedures
- Associated patterns or vertical deviations may necessitate adjunctive surgical modifications
Future Directions in Strabismus Management
While recession and resection techniques remain the gold standard for pediatric strabismus correction, ongoing research continues to refine surgical outcomes. Comparative studies examining unilateral lateral rectus recession against combination recession-resection approaches demonstrate similar efficacy for specific deviation ranges, though longer follow-up may reveal differences in recurrence patterns. Adjustable suture techniques, when feasible, offer additional refinement opportunities by allowing fine-tuning of the refractive effect in the immediate postoperative period.
Large randomized controlled trials comparing surgical approaches across different age groups remain needed to fully elucidate age-related factors influencing outcomes. Improved understanding of the biological and biomechanical factors underlying variable individual responses to standard surgical magnitudes could potentially enable more personalized surgical planning.
Frequently Asked Questions
What is the difference between recession and resection?
Recession weakens a muscle by moving its attachment point backward on the eye, while resection strengthens a muscle by shortening it and reattaching at the original position. Recession is used for overacting muscles; resection for underacting muscles.
Are both eyes always treated surgically?
Not necessarily. Unilateral surgery on one eye’s lateral rectus can correct many moderate deviations. Bilateral procedures (operating on both eyes) are typically reserved for larger deviations exceeding 15 prism diopters.
What is the success rate for these procedures?
Success rates vary from approximately 72-90% depending on the specific procedure and deviation magnitude. Young children may achieve rates as high as 86.2% with unilateral procedures.
Can strabismus return after surgery?
Yes, residual or recurrent deviation occurs in some patients, requiring additional intervention. The timing of recurrence varies from months to years. Bilateral procedures may show lower long-term recurrence rates.
What complications can occur?
Serious complications are uncommon with proper technique. Overcorrection to consecutive esotropia occurs in approximately 3.4% of unilateral procedures. Intraoperative and postoperative complications remain rare.
References
- Surgical Management of Residual or Recurrent Esotropia Following Maximal Medial Rectus Recession — JAMA Ophthalmology, American Medical Association. 2004. https://jamanetwork.com/journals/jamaophthalmology/fullarticle/426931
- Unilateral Lateral Rectus Recession is an Effective Surgery for Treating Moderate Angle of Intermittent Exotropia in Young Children — PMC/NIH National Center for Biotechnology Information. 2020. https://aapos.org/glossary/strabismus-surgery
- Eye Muscle Repair: MedlinePlus Medical Encyclopedia — National Library of Medicine, U.S. National Institutes of Health. 2024. https://medlineplus.gov/ency/article/002961.htm
Read full bio of Sneha Tete