Peptic Ulcer Disease: Symptoms, Causes & Treatment Guide
Understand the causes, symptoms, diagnosis, and effective treatments for peptic ulcer disease to manage pain and prevent complications.
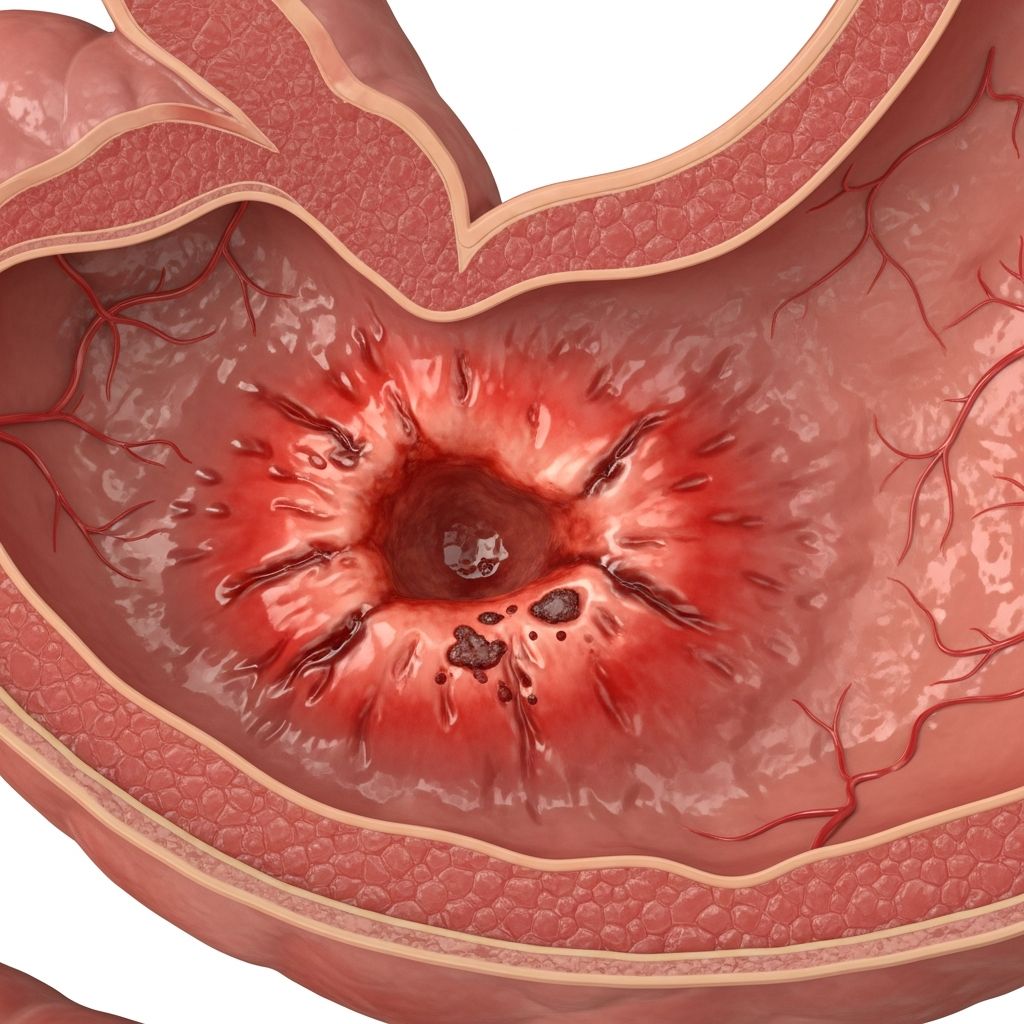
Peptic Ulcer Disease
Peptic ulcer disease (PUD) is a common gastrointestinal condition characterized by sores or erosions in the inner lining of the stomach (gastric ulcers) or the upper part of the small intestine, known as the duodenum (duodenal ulcers). These ulcers develop when the protective mucosal layer is damaged, allowing gastric acid and pepsin to erode deeper layers, leading to pain and potential complications. Affecting millions worldwide, PUD impacts about 10% of individuals presenting with upper abdominal pain in primary care settings.
Symptoms of Peptic Ulcer Disease
The hallmark symptom of peptic ulcer disease is epigastric pain, a burning or gnawing sensation in the upper abdomen. For gastric ulcers, pain typically occurs within 15-30 minutes after eating, while duodenal ulcer pain arises 2-3 hours post-meal or at night, often relieved by food or antacids. Other common symptoms include bloating, belching, nausea, vomiting, and early satiety.
- Burning abdominal pain: Most frequent, worsens on an empty stomach for duodenal ulcers.
- Nausea and vomiting: Can signal complications like bleeding.
- Weight loss: Due to pain-avoidant eating habits.
- Bloody stools or vomit: Indicates bleeding ulcers, a medical emergency.
Silent ulcers may occur in older adults or those on NSAIDs, presenting only with complications. Complications affect 73% with bleeding, 9% with perforation, and 3% with obstruction, contributing to 10,000 annual U.S. deaths.
Causes of Peptic Ulcer Disease
The primary causes are Helicobacter pylori (H. pylori) infection and nonsteroidal anti-inflammatory drug (NSAID) use. H. pylori, a gram-negative bacillus, accounts for 90% of duodenal and 70-90% of gastric ulcers by inflaming the mucosa, impairing bicarbonate secretion, and promoting acidity. It affects 42% of PUD cases and is more common in lower socioeconomic groups, acquired in childhood.
NSAIDs like aspirin and ibuprofen inhibit prostaglandins, reducing mucosal protection and increasing acid damage, responsible for 36% of cases. Other risk factors include smoking, alcohol, stress, family history, and comorbidities like cirrhosis or Crohn’s disease.
| Risk Factor | Prevalence in PUD | Mechanism |
|---|---|---|
| H. pylori infection | 42-90% | Mucosal inflammation, hypochlorhydria |
| NSAID use | 24-36% | Prostaglandin inhibition |
| Smoking | Variable | Impaired healing |
| Family history | Increased risk | Genetic predisposition |
Diagnosis of Peptic Ulcer Disease
Diagnosis begins with history and physical exam focusing on epigastric tenderness. Testing for H. pylori is recommended for all PUD patients using urea breath test, stool antigen, or serology. Endoscopy is definitive, allowing visualization, biopsy for H. pylori or malignancy, and intervention for bleeding. Barium swallow may be used if endoscopy is unavailable.
- Urea breath test: Non-invasive, high sensitivity for active infection.
- Endoscopy: Gold standard, especially for sinister symptoms like weight loss or bleeding.
- Biopsy: Confirms H. pylori and rules out cancer in gastric ulcers.
For bleeding ulcers, urgent endoscopy reduces transfusion needs and surgery.
Treatment of Peptic Ulcer Disease
Treatment targets causes and symptoms with proton pump inhibitors (PPIs) like omeprazole healing 80-100% of ulcers in 4 weeks (8 weeks for large gastric ulcers). H. pylori eradication uses triple therapy: PPI + two antibiotics (e.g., clarithromycin, amoxicillin, metronidazole) for 10-14 days, reducing recurrence from 50-60% to 0-2%.
NSAID ulcers heal in 95% upon discontinuation; misoprostol or PPI prophylaxis if continued. Refractory ulcers (>5mm after 8-12 weeks PPI) require addressing persistent H. pylori, NSAIDs, or comorbidities.
| Regimen | Components | Duration |
|---|---|---|
| Triple Therapy | PPI + Clarithromycin + Amoxicillin/Metronidazole | 10-14 days |
| PPI Monotherapy | Omeprazole 20-40mg daily | 4-8 weeks |
| NSAID Prophylaxis | Misoprostol or PPI | With NSAID use |
Surgery (vagotomy, gastrectomy) for unresponsive cases or complications.
Prevention of Peptic Ulcer Disease
Prevent H. pylori via hygiene; test and treat in high-risk groups. Use NSAIDs judiciously, prefer COX-2 inhibitors, or add PPI/misoprostol. Smoking cessation and alcohol moderation aid healing. Maintenance PPI for high-risk patients post-eradication.
When to See a Doctor
Seek care for persistent epigastric pain, black stools, vomiting blood, or unexplained weight loss. Urgent evaluation for severe pain suggesting perforation.
Frequently Asked Questions (FAQs)
What is peptic ulcer disease?
A condition with sores in the stomach or duodenum lining due to acid erosion, mainly from H. pylori or NSAIDs.
Can peptic ulcers be cured?
Yes, PPIs heal most within 4-8 weeks; H. pylori eradication prevents recurrence.
Do stress or spicy foods cause ulcers?
No, they exacerbate but don’t cause; primary culprits are H. pylori and NSAIDs.
How is H. pylori tested?
Via breath test, stool antigen, blood test, or endoscopy biopsy.
What are complications of untreated PUD?
Bleeding (73%), perforation (9%), obstruction (3%), increased mortality.
References
- Peptic Ulcer Disease – StatPearls — NCBI Bookshelf, NIH. 2023-07-17. https://www.ncbi.nlm.nih.gov/books/NBK534792/
- Peptic Ulcer Disease: A Review — JAMA Network. 2023-11-07. https://jamanetwork.com/journals/jama/fullarticle/2825337
- Peptic Ulcer Disease — American Academy of Family Physicians (AAFP). 2007-10-01. https://www.aafp.org/pubs/afp/issues/2007/1001/p1005.html
- Symptoms & Treatments for Peptic Ulcer Disease — Cleveland Clinic. 2023. https://my.clevelandclinic.org/health/diseases/10350-peptic-ulcer-disease
Read full bio of Sneha Tete











