Pericarditis: Complete Guide To Symptoms, Causes & Treatment
Comprehensive guide to pericarditis: symptoms, causes, diagnosis, treatment, and prevention of heart sac inflammation.
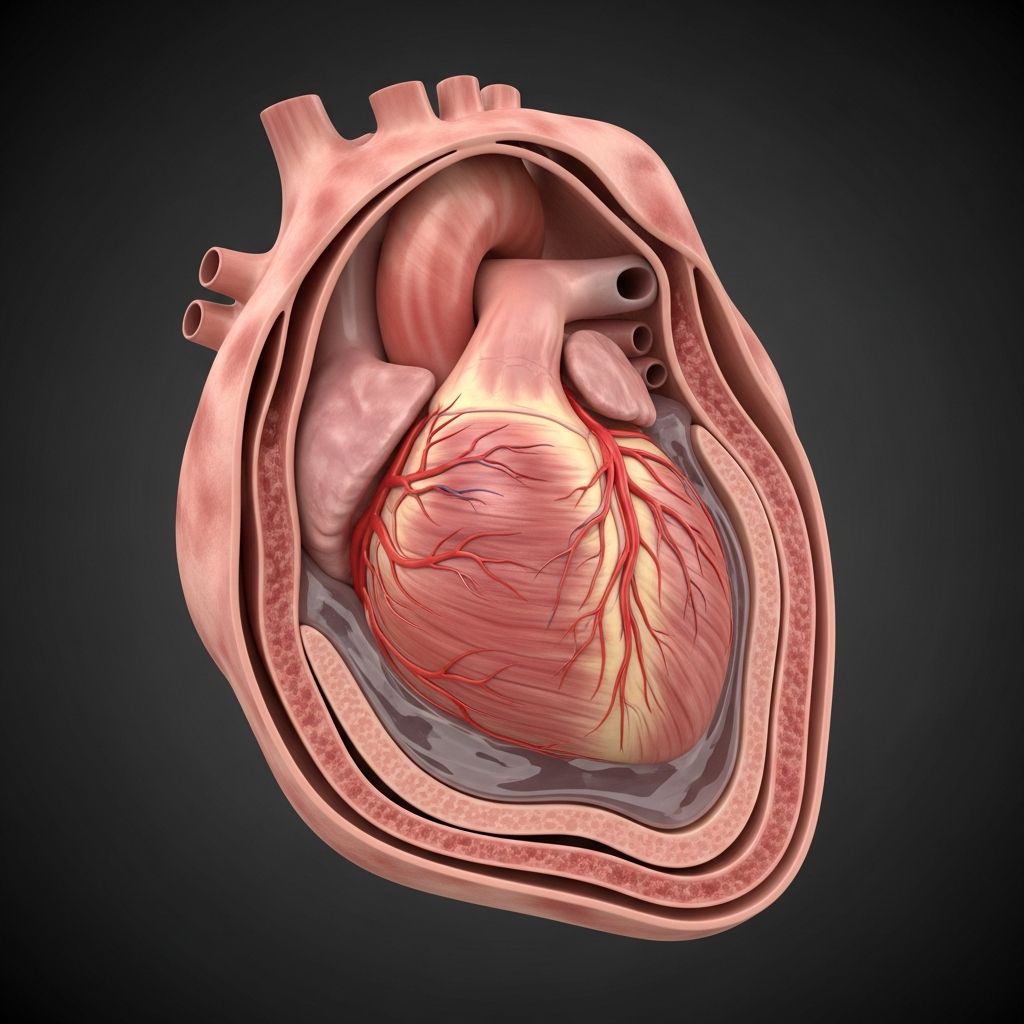
Pericarditis Overview
Pericarditis is inflammation of the pericardium, the thin sac-like membrane surrounding the heart that holds it in place and protects it from infection or injury. This condition often causes sharp chest pain and can range from mild and self-resolving to severe with complications like fluid buildup or heart compression.
What Is the Pericardium?
The pericardium is a double-layered fibroelastic sac enveloping the heart, consisting of an inner visceral layer adherent to the epicardium and an outer parietal layer separated by 15-50 mL of serous fluid that reduces friction during heartbeats. This structure cushions the heart, prevents overexpansion, and serves as a barrier against infection and malignancy. Inflammation disrupts this fluid balance, leading to painful rubbing of layers and potential effusion.
Pericarditis Symptoms
The hallmark symptom of pericarditis is sharp, stabbing chest pain, typically located in the middle or left chest, radiating to shoulders or neck, worsening when lying down or breathing deeply, and improving when leaning forward. Other common signs include:
- Shortness of breath or fatigue
- Fever, persistent cough, or night sweats
- Irregular heartbeat (palpitations)
- A high-pitched ‘friction rub’ sound heard via stethoscope when leaning forward
In severe cases with large pericardial effusion, low blood pressure, shock, or cardiac tamponade may occur, compressing the heart and impairing pumping—a medical emergency. Up to 90% of patients report chest discomfort.
Causes of Pericarditis
Pericarditis arises from infectious or non-infectious triggers, with many cases idiopathic (unknown cause). Causes are grouped as follows:
Infectious Causes
- Viral infections (most common in developed countries, e.g., coxsackievirus, COVID-19)
- Bacterial (e.g., tuberculosis in endemic areas, staphylococcus)
- Fungal or parasitic (rare, in immunocompromised)
Non-Infectious Causes
- Heart attack, surgery, or procedures (post-MI Dressler’s syndrome)
- Autoimmune diseases (e.g., lupus, rheumatoid arthritis)
- Cancer (lung, breast), radiation therapy, or uremia
- Trauma, medications (e.g., hydralazine), or kidney failure
Risk increases post-heart injury, viral illness, or in males aged 20-50.
Types of Pericarditis
Pericarditis is classified by duration and recurrence:
- Acute: Sudden onset, lasts <4-6 weeks
- Incessant: Persists 4-6 weeks to <3 months despite treatment
- Chronic: Lasts >3 months
- Recurrent: New episode after 4-6 weeks symptom-free; affects 15-30%
Associated syndromes include effusive-constrictive (effusion + constriction) or constrictive pericarditis (thickened sac restricts filling).
Diagnosis
Diagnosis requires at least two of four criteria: typical chest pain, pericardial friction rub, ECG changes (diffuse ST elevation, PR depression), or new/large effusion. Steps include:
- Physical exam for rub, fever, or muffled sounds
- ECG: Stage I concave ST elevation (vs. convex in MI), PR depression in multiple leads
- Echocardiogram: Detects effusion, tamponade signs (chamber collapse)
- Blood tests: Elevated CRP/ESR (inflammation), troponin (if myopericarditis)
- Advanced: CT/MRI for etiology, pericardiocentesis if tamponade or purulent
Differentiate from MI (ECG, troponin), PE, or pneumonia.
Treatment
Treatment targets inflammation and cause; most acute cases resolve with rest and meds. First-line:
- High-dose NSAIDs (ibuprofen 600-800mg TID) or aspirin for 1-2 weeks
- Colchicine (0.5mg BID) for 3 months to prevent recurrence (reduces risk by 50%)
Second-line if refractory:
- Corticosteroids (prednisone 0.2-0.5mg/kg) cautiously, as they increase recurrence
- Immunosuppressants (azathioprine, IVIG) for autoimmune/recurrent
For complications:
- Pericardiocentesis/drain for tamponade or large effusion
- Antibiotics/antifungals for infection; pericardiectomy for constriction
Hospitalize high-risk patients (fever, subacute, effusion, trauma, anticoagulation).
Complications
Untreated pericarditis risks:
- Pericardial effusion: Fluid buildup; rapid/large leads to tamponade (hypotension, shock)
- Constrictive pericarditis: Scarred sac impairs filling; 30% risk post-bacterial/TB
- Myopericarditis: Myocardial involvement (elevated troponin)
| Complication | Risk Factors | Management |
|---|---|---|
| Cardiac Tamponade | Rapid effusion, cancer, infection | Urgent drainage |
| Constrictive Pericarditis | Bacterial/TB, radiation | Surgical pericardiectomy |
| Recurrence | Incomplete treatment, steroids | Colchicine prophylaxis |
Prognosis and Recovery
Acute pericarditis has excellent prognosis; 80-90% resolve in weeks with treatment. Recovery varies by cause/health: mild cases self-resolve with rest; severe may take months. Recurrence risk 15-30%; monitor with follow-up echo/ECG. Chronic cases or post-TB have higher constriction risk (up to 30%). Most patients return to normal activity post-recovery.
Prevention
Prevent by treating underlying conditions (e.g., prompt viral care, TB screening). Post-cardiac injury/surgery, early anti-inflammatories reduce risk. Colchicine prevents recurrence in high-risk. Lifestyle: Avoid triggers like certain meds; vaccinate against viruses.
When to See a Doctor
Seek immediate care for chest pain mimicking heart attack (call 911). Urgent evaluation for new pain worsening with position/breathing, fever, dyspnea, or palpitations.
Frequently Asked Questions (FAQs)
What does pericarditis chest pain feel like?
Sharp, stabbing pain in the chest or left side, worse lying down or breathing deeply, better leaning forward.
Is pericarditis life-threatening?
Usually not; most cases mild. But tamponade or constriction can be emergencies requiring intervention.
How long does pericarditis last?
Acute: <4-6 weeks; full recovery 1-3 months with treatment.
Can COVID-19 cause pericarditis?
Yes, as a viral trigger, especially post-vaccination or infection.
Can pericarditis be cured?
Yes, most acute cases resolve fully; chronic/recurrent managed long-term.
References
- What Is Pericarditis? — American Heart Association. 2023. https://www.heart.org/en/health-topics/pericarditis/what-is-pericarditis
- Pericarditis – StatPearls — NCBI Bookshelf / NIH. 2023-08-08. https://www.ncbi.nlm.nih.gov/books/NBK431080/
- What Is Pericarditis? — JAMA Network. 2023. https://jamanetwork.com/journals/jama/fullarticle/2830037
- Pericarditis: Symptoms, Causes and Treatment — Cleveland Clinic. 2023-11-09. https://my.clevelandclinic.org/health/diseases/17353-pericarditis
- Acute Pericarditis: Rapid Evidence Review — American Academy of Family Physicians (AAFP). 2024-05-01. https://www.aafp.org/pubs/afp/issues/2024/0500/acute-pericarditis.html
Read full bio of Sneha Tete











