Periodontal Disease: Causes, Symptoms & Treatment
Complete guide to understanding, preventing, and treating periodontal disease and gum disease.
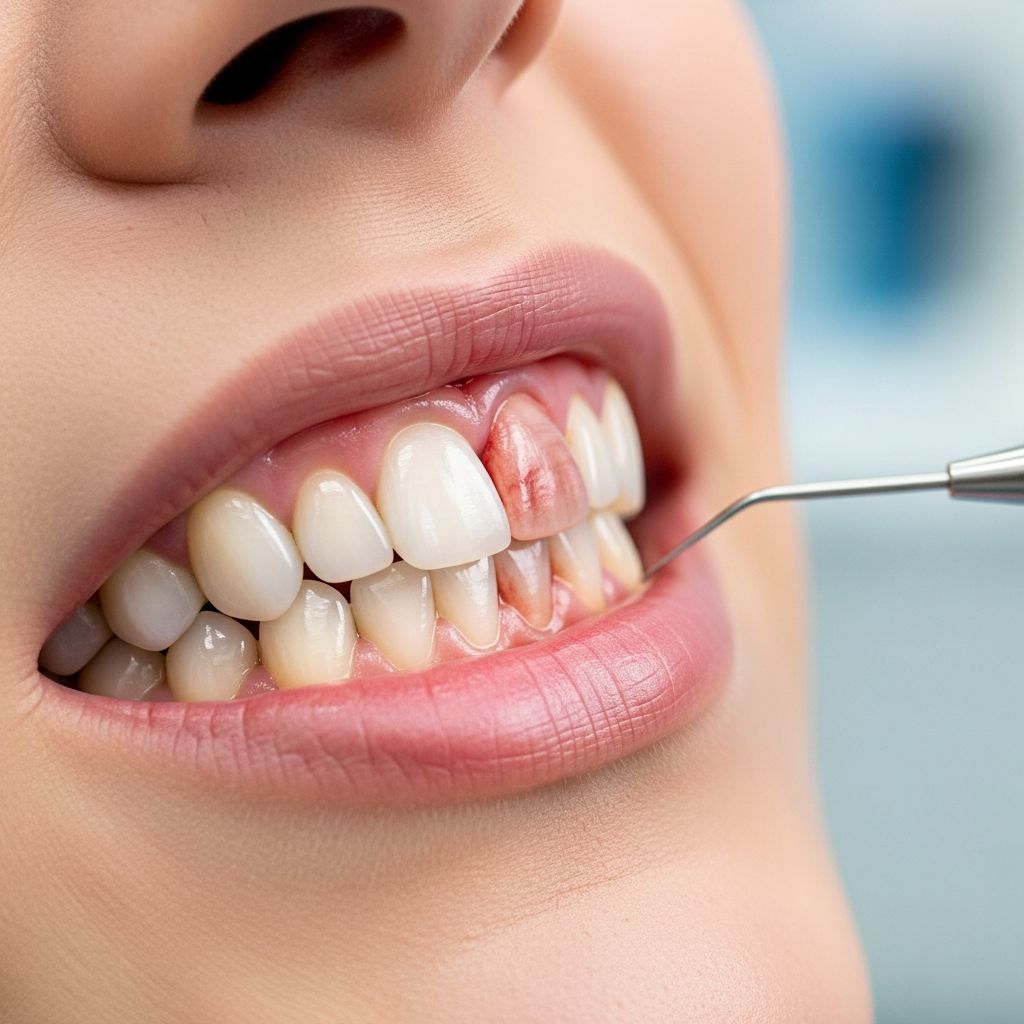
Understanding Periodontal Disease: A Complete Overview
Periodontal disease, commonly referred to as gum disease, represents inflammation and infection of the tissues that support your teeth. This condition affects millions of individuals worldwide and stands as one of the most prevalent chronic inflammatory conditions globally. The disease progresses through distinct stages, from mild gingivitis to severe periodontitis, with varying degrees of reversibility depending on when treatment begins.
The tissues that comprise the periodontal system include your gums, alveolar bone, cementum, and the periodontal ligament. When bacteria accumulate on your teeth and gums, they trigger an immune response that can lead to tissue destruction if left untreated. Understanding the nature of periodontal disease is essential for recognizing early warning signs and seeking timely treatment.
The Four Stages of Gum Disease
Periodontal disease develops progressively through four distinct stages, each with increasing severity and complexity:
Stage 1: Gingivitis
Gingivitis represents the earliest stage of gum disease, characterized by inflammation of the gingival tissues without bone loss. At this stage, the condition remains reversible with appropriate intervention. Common signs include red, swollen, and bleeding gums, particularly during brushing or flossing. Approximately half of all adults older than 30 experience some form of gum disease, making gingivitis remarkably prevalent in the adult population.
Stage 2: Mild Periodontitis
When gingivitis progresses without treatment, it advances to mild periodontitis. At this stage, bone loss begins around the teeth, creating small periodontal pockets where bacteria can accumulate. Gum recession may become apparent, and patients might notice increased sensitivity or persistent bad breath.
Stage 3: Moderate Periodontitis
Moderate periodontitis involves more significant bone loss and deeper periodontal pockets. The supporting structures continue to deteriorate, potentially affecting multiple teeth. Teeth may begin to feel loose or shift position, and professional intervention becomes increasingly important to halt disease progression.
Stage 4: Advanced Periodontitis
Advanced periodontitis represents the most severe stage, with substantial bone loss, deep pockets, and significant damage to the periodontal structures. At this stage, teeth may become severely loose or require extraction. Professional treatment becomes critical to prevent tooth loss and manage the infection.
Recognizing Symptoms of Periodontal Disease
Early detection of periodontal disease significantly improves treatment outcomes. Being aware of the warning signs allows you to seek professional care before the condition becomes severe.
Early Warning Signs
Early symptoms of gum disease include swollen, tender, and reddish or purplish gums. You may notice visible plaque buildup on your teeth, particularly along the gum line. Bleeding during brushing or flossing represents one of the most common early indicators of periodontal disease. Additionally, some individuals experience persistent bad breath that doesn’t resolve with regular oral hygiene practices.
Progressive Symptoms
As the disease worsens, additional symptoms emerge. You may observe loose or shifting teeth as the supporting bone deteriorates. Pus along the gum line indicates active infection, and gum recession becomes more pronounced. Some patients report changes in their bite or difficulty chewing certain foods. These progressive symptoms warrant immediate professional attention.
Understanding the Causes of Periodontal Disease
Multiple factors contribute to the development and progression of periodontal disease. Understanding these causes helps explain why some individuals develop the condition while others maintain healthy gums throughout their lives.
Dental Plaque: The Primary Culprit
Buildup of dental plaque represents the number one cause of periodontal disease. Plaque contains numerous bacterial species that can infect your gums and supporting tissues. When plaque isn’t removed through regular brushing and flossing, it hardens into calculus (tartar), which can only be removed by professional cleaning. This bacterial accumulation triggers an inflammatory response that damages gum tissue and, eventually, the underlying bone.
Genetic Factors
In some individuals, genetics play a significant role in periodontal disease development by altering the way their immune system responds to bacteria. People with genetic predisposition may be more susceptible to gum disease even with excellent oral hygiene practices. If you have a family history of periodontal disease, maintaining vigilant oral care and scheduling regular professional cleanings becomes even more important.
Additional Risk Factors
Several other factors increase the likelihood of developing periodontal disease. Postmenopausal status is considered a risk factor for periodontitis, as hormonal changes affect immune response and tissue health. Smoking significantly increases periodontal disease risk and complicates treatment outcomes. Systemic diseases such as diabetes, cardiovascular disease, and respiratory conditions elevate periodontal risk. Additionally, certain medications, stress, poor nutrition, and hormonal fluctuations during pregnancy can contribute to gum disease development.
Diagnosis and Professional Assessment
Professional diagnosis of periodontal disease involves a comprehensive examination by a dentist or periodontist. During your dental visit, your healthcare provider will assess your gum health through visual examination and probing. They measure the depth of periodontal pockets using a calibrated probe, with deeper pockets indicating more advanced disease.
Dental X-rays play a crucial role in diagnosing periodontal disease. These images clearly show areas of bone loss in detail, allowing your dentist to assess the extent of damage. By comparing current X-rays with older ones, your provider can determine how quickly bone has been lost and evaluate disease progression over time. This information helps guide treatment planning and predict treatment outcomes.
Treatment Options for Periodontal Disease
The appropriate treatment for periodontal disease depends on the severity of your condition and several other individual factors. Your dentist or periodontist will develop a customized treatment plan addressing your specific needs.
Nonsurgical Treatments
Dental Cleaning and Improved Oral Hygiene
People with very early periodontal disease (gingivitis) may reverse the condition through routine professional dental cleaning combined with improved oral hygiene. Because no bone loss has occurred at this stage, this conservative approach eliminates harmful oral bacteria before the disease progresses further. Professional cleanings remove plaque and calculus that home care cannot address, while patient education ensures effective daily oral hygiene practices.
Scaling and Root Planing
For patients with more advanced gingivitis or mild periodontitis, scaling and root planing represent important nonsurgical treatments. Scaling removes plaque and calculus from tooth surfaces and below the gum line. Root planing smooths the root surface, making it more difficult for bacteria to reattach and promoting gum reattachment. These procedures require local anesthesia and may be completed in multiple appointments.
Antibiotic Therapy
Dentists may prescribe antibiotics to control bacterial infection and reduce inflammation. Antibiotics may be administered orally or placed directly into periodontal pockets as part of adjunctive therapy. These medications support the body’s immune system in fighting the infection while other treatments address the underlying problem.
Surgical Treatments
Flap Surgery (Pocket Reduction Surgery)
For more advanced periodontitis, flap surgery may be necessary. During this procedure, a periodontist makes incisions in the gum tissue to access deeper areas beneath the gum line. This allows for thorough removal of bacteria and calculus that cannot be reached through nonsurgical means. The procedure also reshapes bone and gum tissue to reduce the depth of periodontal pockets, making future plaque removal easier.
Bone Grafting
A dental bone graft uses your own bone, donated bone, or synthetic bone to rebuild areas damaged by gum disease. The graft serves as scaffolding that holds space until your body can regenerate new bone. Periodontists often perform bone grafting in combination with other procedures to restore lost bone support around teeth.
Guided Tissue Regeneration (GTR)
Guided tissue regeneration represents an advanced technique that periodontists typically use in combination with bone grafts. During GTR, a periodontist places an artificial membrane between your gums and newly placed bone grafting material. Because soft tissue regenerates faster than bone, the membrane keeps that space open, allowing new bone to grow rather than soft tissue filling the defect. This procedure significantly improves the chances of bone regeneration and tooth preservation.
Gum Grafting
If you’ve lost gum tissue to periodontal disease, your dentist may recommend gum graft surgery, also called tissue grafting. This procedure covers exposed teeth roots and adds thickness to the gum line. During the procedure, a periodontist adds tissue to areas of gum recession. This tissue may come from the roof of your mouth, or your provider may obtain it from a licensed bone and tissue bank. Gum grafting improves both function and aesthetics while reducing tooth sensitivity.
Recovery and Aftercare Following Treatment
Recovery time varies depending on the type of treatment received. If you undergo scaling and root planing, you won’t need significant downtime and can return to normal activities immediately. However, if you undergo procedures for advanced periodontal disease such as flap surgery, bone grafts, or gum grafts, you’ll need anywhere from one to four weeks to recover.
Following treatment, maintaining excellent oral hygiene at home becomes absolutely critical. Your periodontist will provide specific instructions for caring for treated areas during the healing phase. Regular follow-up appointments allow your provider to monitor healing and adjust your care plan as needed. Possible complications following gum disease treatment include infection, continued bone loss, or recurrence of periodontal pockets, though these remain relatively uncommon with proper aftercare.
Can Periodontal Disease Be Cured?
Gum disease isn’t curable, but it is manageable with appropriate treatment and consistent oral hygiene. The reason lies in the nature of the damage caused by advanced periodontal disease. Once you lose structural support around your teeth through bone loss, you typically don’t recover all of it, even with treatment. However, when treated early enough, gingivitis is reversible. At this earliest stage, before bone loss occurs, removing plaque and improving oral hygiene can completely resolve the condition.
When periodontal treatment has already progressed to involve bone loss, the disease becomes too advanced to reverse completely. However, periodontal treatment can substantially reduce infection and rebuild your bone and tissue to some degree. The goal of treatment at advanced stages shifts from cure to management—stopping disease progression, preserving remaining teeth, and maintaining oral function and health.
Treatment Success Rates and Long-Term Outcomes
Periodontal disease treatment has impressive success rates that can reach 95% in some instances. These rates vary based on several factors, including the specific procedure performed, the stage of disease at treatment, and how carefully a person cares for their teeth and gums following treatment. Patients who commit to improved oral hygiene and regular professional maintenance experience significantly better long-term outcomes than those who don’t maintain these practices.
Prevention: Your Best Defense Against Periodontal Disease
In most cases, you can prevent gum disease through consistent and proper oral hygiene. A comprehensive prevention strategy includes brushing your teeth twice daily with fluoride toothpaste, flossing daily to remove plaque from between teeth, and scheduling regular professional cleanings.
However, some people are more prone to gum disease due to genetics or other health conditions. In these instances, you may need more frequent cleanings with your dental hygienist. Additional preventive measures include avoiding tobacco products, managing stress, maintaining good nutrition, and managing systemic diseases like diabetes. If you have swollen, tender, or bleeding gums, tell your dentist promptly. They can help you eliminate infection and get back on track to healthy teeth and gums.
The Importance of Early Detection and Treatment
The sooner you treat gum disease, the less likely you are to lose teeth and the more successfully you can manage the condition. Early detection and intervention represent the most critical factors in preserving your natural teeth and maintaining good oral health throughout your lifetime. At its earliest stage, gingivitis is completely reversible. As the disease progresses to periodontitis, treatment becomes more complex and less likely to achieve complete reversal, though management becomes increasingly important.
Key Takeaways About Periodontal Disease
Periodontal disease represents a serious but manageable condition affecting the tissues that support your teeth. The disease progresses through distinct stages, from reversible gingivitis to irreversible periodontitis involving bone loss. Early detection through professional examinations and awareness of warning signs allows for timely intervention. While periodontal disease cannot be completely cured once bone loss occurs, it can be effectively managed through a combination of professional treatment and consistent home care. Prevention through proper oral hygiene and regular professional cleanings remains your best defense against this common but preventable condition.
Frequently Asked Questions
Q: What is the difference between gingivitis and periodontitis?
A: Gingivitis is the earliest stage of gum disease involving inflammation without bone loss, and it is reversible with proper treatment. Periodontitis represents a more advanced stage where bone loss has occurred around the teeth, causing permanent damage. Once bone loss occurs, the condition cannot be completely reversed, though it can be managed.
Q: Can I reverse periodontal disease at home?
A: Early-stage gingivitis may improve with improved oral hygiene and professional cleaning, but once periodontal disease progresses to periodontitis with bone loss, you cannot reverse it completely through home care alone. Professional treatment is necessary for advanced stages, though excellent home care supports treatment outcomes.
Q: How often should I see a dentist if I have periodontal disease?
A: The frequency depends on the severity of your condition and your individual risk factors. Most people with periodontal disease benefit from professional cleanings more frequently than the standard twice-yearly visits, with some requiring visits every three months or more frequently for optimal management.
Q: What are the long-term consequences of untreated periodontal disease?
A: Untreated periodontal disease leads to progressive bone loss, tooth mobility, and eventual tooth loss. Additionally, emerging research suggests links between periodontal disease and other serious health conditions including cardiovascular disease, diabetes complications, and respiratory infections.
Q: Is periodontal disease preventable?
A: Yes, in most cases periodontal disease is preventable through consistent proper oral hygiene, regular professional cleanings, and managing risk factors. However, some individuals have genetic predisposition to periodontal disease and may require more aggressive prevention strategies.
References
- Periodontal Disease (Gum Disease): Causes, Symptoms & Treatment — Cleveland Clinic. 2025. https://my.clevelandclinic.org/health/diseases/21482-gum-periodontal-disease
- Gum Disease Treatment — Cleveland Clinic. 2025. https://my.clevelandclinic.org/health/treatments/10907-gum-disease-treatment
- Gingivitis: Symptoms & How To Treat It — Cleveland Clinic. 2025. https://my.clevelandclinic.org/health/diseases/10950-gingivitis-and-periodontal-disease-gum-disease
- Periodontitis: Symptoms, Causes & Treatment — Cleveland Clinic. 2025. https://my.clevelandclinic.org/health/diseases/16620-periodontitis
- What is a Periodontist? Definition & Types of Periodontics — Cleveland Clinic. 2025. https://my.clevelandclinic.org/health/articles/23461-periodontics-periodontist
- Antiviral T cells present in mouth found to worsen periodontitis progression — Cleveland Clinic Lerner Research Institute. 2025-05-23. https://www.lerner.ccf.org/news/article/?title=Antiviral+T+cells+present+in+mouth+found+to+worsen+periodontitis+progression
- A need to educate postmenopausal women of their periodontal health — National Center for Biotechnology Information, U.S. National Library of Medicine. 2013. https://pmc.ncbi.nlm.nih.gov/articles/PMC3713756/
Read full bio of medha deb











