Peristomal Intestinal Metaplasia: Diagnosis And Treatment
Rare skin condition around stomas where skin cells transform into intestinal-like tissue, often decades after surgery.
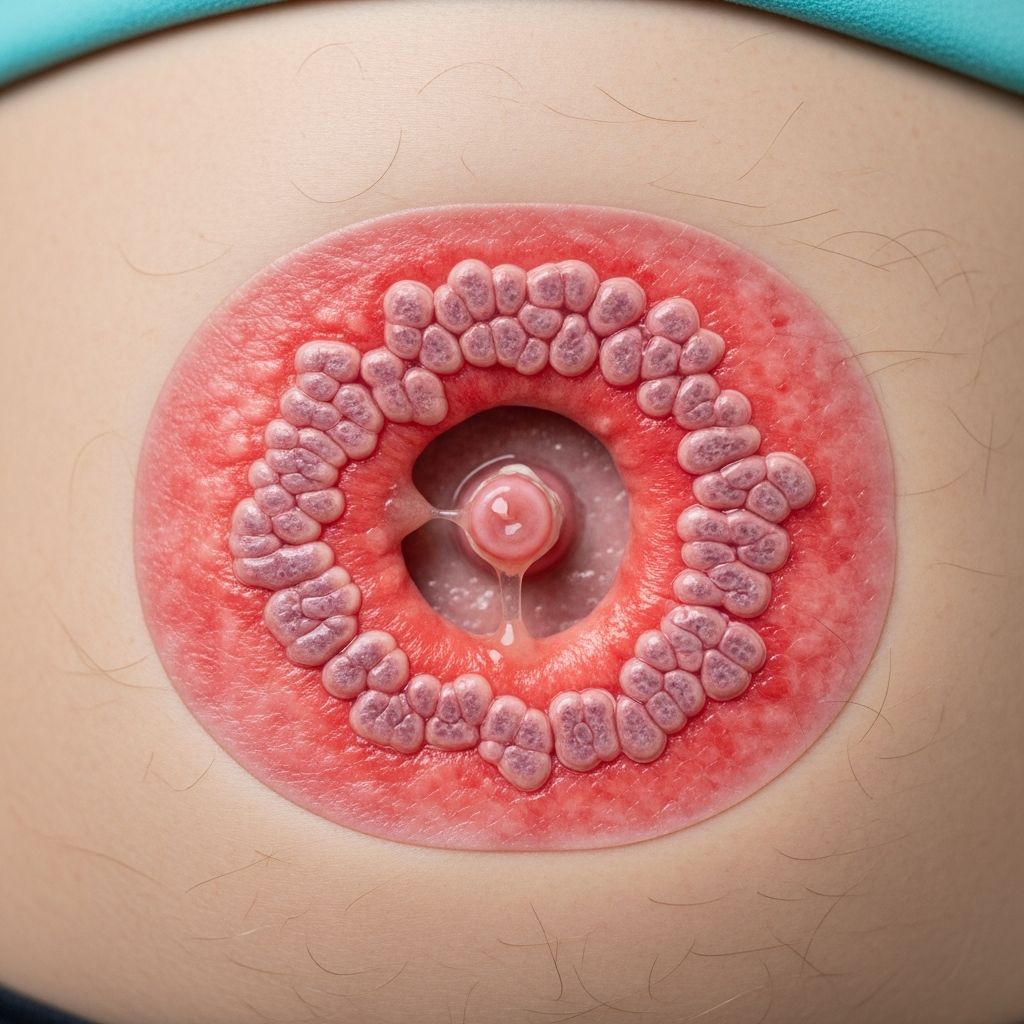
Peristomal intestinal metaplasia
Author: Dr. Reviewed by: August 2025
Peristomal intestinal metaplasia (PIM) is a rare dermatological condition characterized by the transformation of skin cells surrounding an ostomy stoma into cells resembling intestinal mucosa. This metaplastic change manifests as glandular structures identical to colonic crypts embedded within the epidermis, typically presenting decades after stoma creation.
What is peristomal intestinal metaplasia?
Peristomal intestinal metaplasia refers to the abnormal replacement of normal squamous epithelial cells in the peristomal skin with mucin-secreting columnar cells organized into tubular glands that mimic the architecture of intestinal epithelium. These glands produce mucin and may secrete alkaline fluid, leading to clinical features such as moist, velvety plaques or nodules around the stoma.
The condition is histologically defined by scattered colonic crypt-like structures within variably intact epidermis, distinguishing it from other peristomal dermatoses. PIM is benign but requires differentiation from malignancy due to its glandular appearance.
Who gets peristomal intestinal metaplasia?
PIM predominantly affects patients with long-standing stomas, with a median time to onset of approximately 30 years post-surgery. Reported cases show a strong association with inflammatory bowel disease (IBD), particularly ulcerative colitis, accounting for 50% of documented instances, of which 80% involve ulcerative colitis histories.
- Patients with ileostomies or colostomies from IBD surgeries (e.g., proctocolectomy).
- Individuals over 60–70 years old at presentation, reflecting delayed onset.
- History of chronic peristomal irritation from fecal exposure, adhesives, or bile salts.
Risk is higher in those with prolonged stoma duration, suggesting age-related decline in skin resistance to metaplastic changes.
What causes peristomal intestinal metaplasia?
The precise etiology remains hypothetical, but two primary theories dominate:
- Surgical implantation: During ostomy creation, suture passage through bowel mucosa and skin may implant viable intestinal cells into the dermis. These cells proliferate slowly over decades, evading immune clearance.
- Chemical induction: Chronic exposure to bile salts and fecal irritants in stoma effluent activates signaling pathways (e.g., NF-κB), promoting epithelial migration and transdifferentiation of skin cells into intestinal phenotype.
The significant delay (30–60+ years) challenges pure implantation theory, implicating cumulative irritation and senescence in skin barrier function. Unlike gastric or esophageal intestinal metaplasia linked to H. pylori or reflux, PIM lacks infectious triggers but shares chronic inflammation as a driver.
What are the clinical features of peristomal intestinal metaplasia?
PIM typically presents insidiously as:
- Moist, erythematous plaques or nodules encircling the stoma, often velvety or papillomatous.
- Alkaline mucous secretion causing maceration, irritation, or peristomal ulcers.
- Mild pruritus, weeping, or overgrowth resembling hypergranulation tissue.
- Absence of systemic symptoms; local discomfort from leakage or pouching issues predominates.
Lesions measure 1–5 cm, confined to peristomal skin, without invasion. Differential includes peristomal pyoderma gangrenosum, malignancy, or infection, necessitating biopsy.
Pathology of peristomal intestinal metaplasia
Histopathology confirms diagnosis:
- Irregular tubular glands lined by mucin-filled goblet cells within the epidermis/dermis.
- CK7+/CK20+ immunostaining matching colonic epithelium.
- Absence of atypia, dysplasia, or invasion distinguishes from adenocarcinoma.
Mucin stains (Alcian blue/PAS) highlight glandular secretion. Serial biopsies may show progression if untreated.
How is peristomal intestinal metaplasia diagnosed?
Diagnosis relies on:
| Step | Description |
|---|---|
| Clinical exam | Inspect for glandular, moist peristomal changes unresponsive to standard care. |
| Biopsy | 4mm punch biopsy of lesion edge for histopathology and IHC. |
| Exclude differentials | Rule out infection, PG, or SCC via culture/swab and imaging if needed. |
Endoscopy or imaging assesses stoma integrity.
What is the treatment for peristomal intestinal metaplasia?
No standardized therapy exists; management is individualized:
- Conservative: Optimize pouching, barrier creams to minimize irritation.
- Destructive: Serial electrosurgery or CO2 laser ablation effectively resolves lesions by destroying glandular elements, with recurrence prevented by repeat sessions.
- Topical: 5-FU or imiquimod for superficial cases, though evidence is anecdotal.
- Stoma revision: Rarely, for refractory or ulcerated PIM.
Response to electrosurgery supports secretory factor elimination hypothesis.
What is the outcome for peristomal intestinal metaplasia?
PIM is benign with no reported malignant transformation. Complete resolution follows aggressive ablation in case series. Long-term surveillance (annual biopsy) recommended due to rarity and dysplasia risk analogy to GI metaplasia.
Prevention of peristomal intestinal metaplasia
- Minimize surgical trauma during stoma creation.
- Protect peristomal skin with barriers from day one.
- Regular ostomy nurse follow-up for early lesion detection.
- Avoid chronic fecal stasis or leaks.
Related topics
- Parastomal pyoderma gangrenosum
- Stoma complications
- Cutaneous metastases
- Intestinal metaplasia (gastric)
Frequently asked questions
Q: Is peristomal intestinal metaplasia cancerous?
A: No, PIM is a benign metaplastic process without malignant potential reported in literature. However, biopsy excludes dysplasia.
Q: How common is PIM?
A: Exceedingly rare; fewer than 20 cases documented, mostly in IBD stoma patients.
Q: Can PIM be reversed without surgery?
A: Electrosurgery achieves resolution; topicals may help mildly. Stoma care prevents progression.
Q: Why does it appear so late after stoma surgery?
A: Likely due to slow proliferation of implanted cells or age-related skin changes reducing resistance.
References
- Intestinal Metaplasia: Stages, Symptoms, Treatment & What it Is — Cleveland Clinic. 2023-05-15. https://my.clevelandclinic.org/health/diseases/22215-intestinal-metaplasia
- Peristomal intestinal metaplasia with response to serial electrosurgery — PMC (NCBI). 2024-02-20. https://pmc.ncbi.nlm.nih.gov/articles/PMC10876460/
- Cutaneous intestinal metaplasia: An unusual cause of peristomal ulceration — PubMed (NCBI). 2019-12-17. https://pubmed.ncbi.nlm.nih.gov/31846090/
- Cutaneous intestinal metaplasia — Wiley Online Library. 2019-11-01. https://onlinelibrary.wiley.com/doi/pdf/10.1111/cup.13631
- What Is Intestinal Metaplasia? Causes & Risks — Patient Power. 2024-01-10. https://www.patientpower.info/gastric-cancer/intestinal-metaplasia
Read full bio of medha deb










