Permanent Pacemaker: Surgery, Types & What It Is
Learn about permanent pacemakers, how they work, types, surgery, recovery, and living with a pacemaker.
What Is a Permanent Pacemaker?
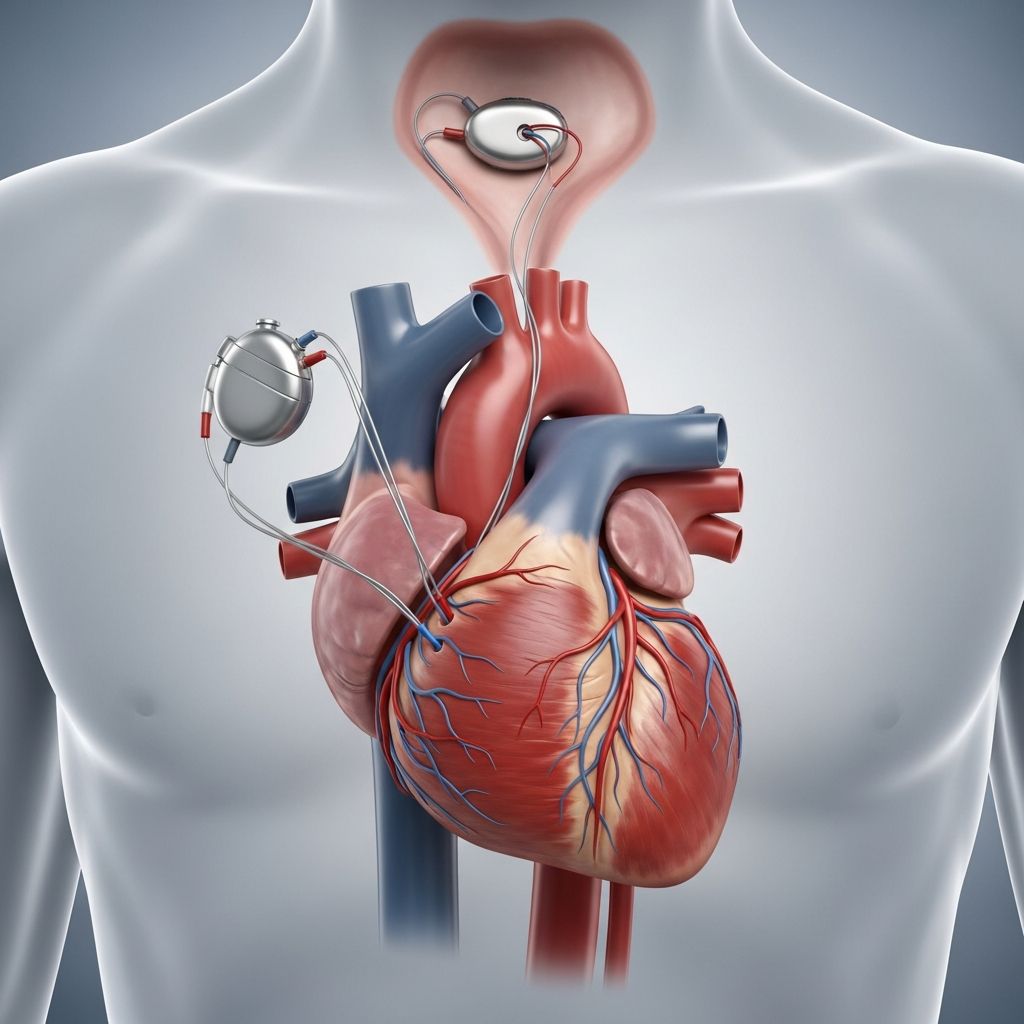
A permanent pacemaker is a small, battery-powered device implanted in the body to help regulate abnormal heart rhythms. It sends electrical impulses to the heart muscle to maintain a steady heartbeat, especially in people who have slow heart rates (bradycardia) or irregular heartbeats. The device is designed to improve quality of life and prevent complications from heart rhythm disorders.
How Does a Pacemaker Work?
A pacemaker monitors the heart’s electrical activity and delivers electrical pulses when the heart rate is too slow or irregular. It consists of two main parts:
- Pulse Generator: Contains the battery and electronic circuitry.
- Leads (Wires): Connect the pulse generator to the heart, transmitting electrical signals.
The pacemaker senses when the heart is beating too slowly or irregularly and sends a small electrical impulse to stimulate the heart muscle, ensuring a regular rhythm.
Types of Pacemakers
There are several types of pacemakers, each suited for different heart conditions:
- Single-Chamber Pacemaker: One lead is placed in either the right atrium or right ventricle.
- Double-Chamber Pacemaker: Two leads are placed—one in the right atrium and one in the right ventricle.
- Biventricular Pacemaker: Three leads are used to pace both ventricles, often for people with heart failure.
- Leadless Pacemaker: A small, self-contained device implanted directly into the heart, without leads.
When Is a Permanent Pacemaker Needed?
A permanent pacemaker may be recommended for people with:
- Bradycardia (slow heart rate)
- Heart block (delayed or blocked electrical signals)
- Sick sinus syndrome (abnormal heart rhythm)
- Heart failure (in some cases)
- Other arrhythmias that do not respond to medication
Pacemaker Implantation Procedure
The pacemaker implantation procedure is typically performed under local anesthesia, with sedation to help you relax. The procedure usually takes 2 to 5 hours, depending on the type of pacemaker and the approach used.
Endocardial (Transvenous) Approach
This is the most common method:
- A small incision is made in the upper chest.
- The lead(s) are inserted through a vein and guided to the heart using fluoroscopy (real-time X-ray).
- The lead tip is attached to the heart muscle, and the other end is connected to the pulse generator, which is placed in a pocket under the skin.
Epicardial Approach
This method is less common and may be used in certain cases:
- The pacemaker is placed in the abdomen.
- The leads are attached to the outer surface of the heart.
Catheter-Based Approach (Leadless Pacemaker)
This minimally invasive method is used for leadless pacemakers:
- A catheter is inserted through a vein in the leg.
- The pacemaker is guided to the heart and implanted directly into the right ventricle.
What Happens During the Procedure?
During the pacemaker implantation:
- Sticky patches (electrodes) are placed on your chest, back, and heart to monitor your heart rhythm.
- A blood pressure cuff and a small clip on your finger monitor your blood pressure and oxygen levels.
- The doctor uses fluoroscopy to guide the leads into place.
- After the leads are in place, the pulse generator is connected and placed under the skin.
- A chest X-ray is taken to check the position of the pacemaker and leads.
Device Clinic Visit
Before you go home, you will visit the Device Clinic:
- You will sit in a reclining chair.
- Electrodes are placed on your chest and connected to a computer.
- A nurse uses a programmer device over your pacemaker to adjust the settings as determined by your doctor.
Risks and Complications
Pacemaker procedures are generally safe, but as with any surgery, there are potential risks:
- Infection at the implant site
- Bleeding or bruising
- Pneumothorax (collapsed lung)
- Lead dislodgement
- Allergic reaction to anesthesia
- Device malfunction
Recovery and Aftercare
Most people go home the same day or the next day after the procedure. Recovery typically involves:
- Resting for a few days
- Avoiding strenuous activities for a few weeks
- Keeping the incision site clean and dry
- Following your doctor’s instructions for medication and follow-up appointments
Living with a Pacemaker
Most people with a pacemaker can lead normal, active lives. Tips for living with a pacemaker include:
- Carry your pacemaker ID card at all times.
- Inform healthcare providers about your pacemaker before any medical procedures.
- Avoid strong magnetic fields and certain electronic devices.
- Attend regular follow-up appointments to check the device’s function.
- Report any unusual symptoms, such as dizziness, fainting, or palpitations.
Frequently Asked Questions (FAQs)
Q: How long does a pacemaker last?
A: Most pacemakers last 5 to 15 years, depending on usage and battery life. Your doctor will monitor the battery and replace the device when needed.
Q: Can I travel with a pacemaker?
A: Yes, you can travel with a pacemaker. Inform airport security about your device, and carry your pacemaker ID card.
Q: Can I exercise with a pacemaker?
A: Most people can exercise with a pacemaker, but consult your doctor before starting any new exercise program.
Q: What should I avoid with a pacemaker?
A: Avoid strong magnetic fields, certain electronic devices, and activities that could cause trauma to the implant site.
Q: How often do I need to see my doctor?
A: Regular follow-up appointments are important to check the device’s function and battery life. Your doctor will recommend a schedule based on your needs.
References
- Pacemaker Implant Procedure — Cleveland Clinic. 2023. https://my.clevelandclinic.org/-/scassets/files/org/heart/patient-education/hvti-files/pacemaker.pdf
- Pacemaker and Defibrillator Lead Extraction Center — Cleveland Clinic. 2023. https://my.clevelandclinic.org/departments/heart/depts/pacemaker-defibrillator
- Pacemaker Implant Procedure — Cleveland Clinic Abu Dhabi. 2023. https://www.clevelandclinicabudhabi.ae/en/health-hub/health-resource/medication-devices-and-supplements/pacemaker-implant-procedure
Read full bio of Sneha Tete













