Phaeohyphomycosis Pathology: Comprehensive Diagnostic Guide
Detailed histopathological analysis of phaeohyphomycosis, a dematiaceous fungal infection affecting skin and deeper tissues.
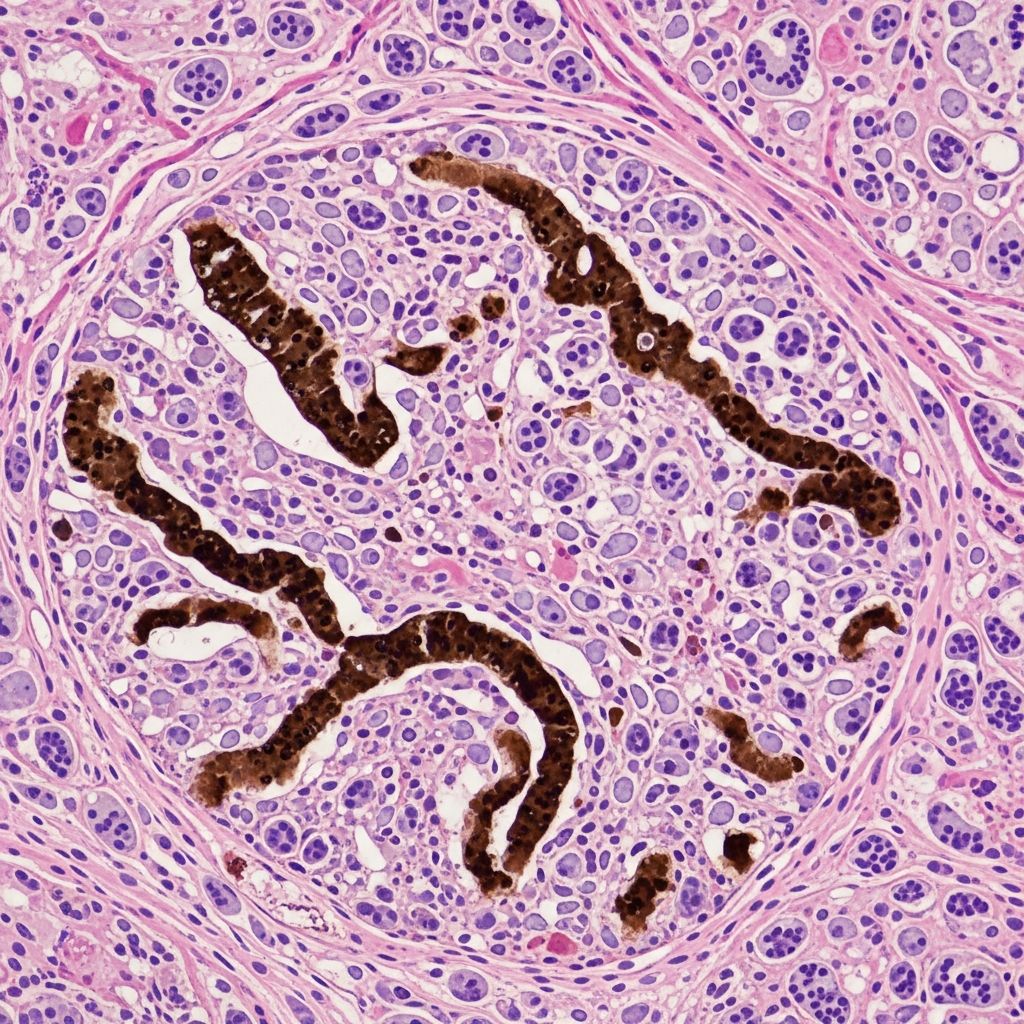
Phaeohyphomycosis pathology
Phaeohyphomycosis refers to a group of mycoses (fungal infections) that are dematiaceous, which means they are pigmented. The pigment is due to their ability to deposit melanin in their cell walls. These infections can manifest in superficial, cutaneous, subcutaneous, or systemic forms, primarily caused by traumatic inoculation of saprophytic dematiaceous fungi from soil, wood, or decomposing vegetation.
Clinical features
Clinically, phaeohyphomycosis often presents as solitary subcutaneous cysts or abscesses, typically sparing the overlying skin. Lesions may appear as papulonodules, verrucous plaques, hyperkeratotic areas, ulcerated plaques, cysts, abscesses, pyogranulomas, non-healing ulcers, or sinuses. In subcutaneous forms, which are the most common, patients may report a history of trauma, though minor injuries can go unnoticed, especially in occupations like farming.
Systemic involvement can affect paranasal sinuses, eyes, bones, or the central nervous system, particularly in immunocompromised individuals. However, cases occur in immunocompetent hosts, highlighting the opportunistic nature of these fungi. Melanin in the fungal cell walls acts as a virulence factor by inhibiting phagocytosis, enabling persistence in tissues.
Histology
Low power
Scanning power view of phaeohyphomycosis reveals a deeply extending granulomatous pattern, often with areas of necrosis. Centrally, an abscess or cystic nodule may form. Frequently, a foreign body such as a wood splinter is evident, corresponding to the traumatic inoculation history. The epidermis commonly exhibits pseudoepitheliomatous hyperplasia, a reactive change mimicking squamous cell carcinoma.
This granulomatous inflammation involves the dermis and extends into the subcutis, forming a wedge-shaped or nodular pattern. Dense mononuclear infiltrates, including lymphocytes, histiocytes, and multinucleated giant cells, predominate. Abscess formation with neutrophilic collections is common in active lesions.
Medium power
At medium magnification, the granulomatous nature becomes apparent, with aggregates of epithelioid histiocytes and foreign body giant cells surrounding areas of suppuration or necrosis. Fungal elements begin to emerge as irregularly shaped, pigmented structures within the inflammatory milieu. These may appear toruloid (yeast-like chains) or irregularly swollen, distinguishing them from regular hyphae.
The inflammatory response is pyogranulomatous, blending granulomatous features with suppurative necrosis. Giant cells often engulf fungal hyphae or yeast forms, indicating an attempt at containment. Vascular proliferation and fibrosis may accompany chronic lesions.
High power
High-power examination highlights the characteristic fungal morphology: septate, branching hyphae with thick, refractile, brown-pigmented walls. These dematiaceous hyphae measure 2-6 μm in width, showing parallel walls, septations, and occasional acute-angle branching. Yeast-like cells or pseudohyphae may also be present, varying in size and shape without forming muriform bodies, which differentiates phaeohyphomycosis from chromoblastomycosis.
The pigmentation is due to melanin, best appreciated in unstained sections or with melanin-specific stains. Hyphae can be extracellular or intracellular within giant cells or macrophages. Surrounding inflammation includes plasma cells and eosinophils in some cases.
Fungal organisms
Dematiaceous fungi responsible for phaeohyphomycosis belong to genera such as Exophiala, Phialophora, Cladophialophora, Bipolaris, Exserohilum, Curvularia, and Alternaria. These saprophytic organisms grow as dark-walled septate mycelium in tissues, unlike the sclerotic bodies in chromoblastomycosis or grains in mycetoma.
In tissue, the fungi appear as brown-pigmented hyphae, yeast cells, or combinations thereof. Culture on Sabouraud’s dextrose agar is essential for speciation, which guides therapy due to varying antifungal susceptibilities. For instance, Cladophialophora boppii has been reported in subcutaneous cases resolving with prolonged azole therapy.
Differential diagnosis
The histopathological differential includes other dematiaceous fungal infections, mycobacterial infections, and foreign body reactions. Key distinctions:
- Chromoblastomycosis: Features muriform (sclerotic) bodies, copper penny-like structures, absent in phaeohyphomycosis.
- Eumycetoma: Shows fungal grains amidst grains and actinomycotic filaments, not irregular hyphae.
- Sporotrichosis: Asteroid bodies and narrower, non-pigmented hyphae.
- Mycobacterial granulomas: Acid-fast bacilli on Ziehl-Neelsen stain; lacks pigmentation.
- Foreign body granuloma: No fungal elements; polarizing material like wood splinters.
Special stains aid differentiation: Grocott-Gomori methenamine silver (GMS) highlights fungal walls black against green background; periodic acid-Schiff (PAS) stains glycogen in walls magenta; Fontana-Masson confirms melanin.
Special stains
- Grocott-Gomori methenamine silver (GMS): Essential for visualizing fungal hyphae and yeast as black structures on a green background. Highlights septations and branching.
- Periodic acid-Schiff (PAS): Stains fungal walls magenta, useful in pigmented and non-pigmented fungi. Complements GMS.
- Fontana-Masson: Specific for melanin, turning dematiaceous fungi brown-black, confirming pigmentation.
These stains enhance detection in subtle cases, where routine H&E may miss sparse organisms. Immunohistochemistry is not routinely used but molecular PCR can speciate fungi if culture fails.
Electron microscopy
Transmission electron microscopy reveals thick electron-dense cell walls due to melanin deposition. Septate hyphae show cross-walls, and the melanin layer protects against host defenses. Rarely used diagnostically, it confirms ultrastructure in research settings.
Clinical correlation and management
Diagnosis integrates histopathology, culture, and clinical history. Treatment cornerstone is surgical debridement plus azoles (itraconazole, voriconazole, posaconazole). Alternatives include terbinafine, amphotericin B, or echinocandins like caspofungin for refractory cases. Duration often exceeds 6-12 months, with monitoring via imaging or biopsy.
Prognosis is good for localized cutaneous/subcutaneous disease but poor for CNS involvement. Recurrence risks persist without complete excision.
Frequently Asked Questions
What is phaeohyphomycosis?
A rare fungal infection by dematiaceous (pigmented) fungi, presenting as hyphae/yeast in tissues without sclerotic bodies.
Who is at risk?
Anyone with trauma exposure, especially immunocompromised; immunocompetent cases occur via minor injuries.
How is it diagnosed?
Biopsy showing pigmented septate hyphae on H&E, confirmed by GMS/PAS/Fontana-Masson, plus culture.
What does it look like histologically?
Granulomatous inflammation with abscesses, pseudoepitheliomatous hyperplasia, and brown hyphae/giant cells.
How is it treated?
Surgical excision + itraconazole/voriconazole; prolonged therapy for systemic disease.
Table: Comparison of Dematiaceous Fungal Infections
| Condition | Tissue Morphology | Clinical Presentation | Key Stain |
|---|---|---|---|
| Phaeohyphomycosis | Hyphae, yeast-like cells | Cysts, abscesses, nodules | GMS, Fontana-Masson |
| Chromoblastomycosis | Muriform bodies | Verrucous plaques | PAS |
| Eumycetoma | Grains | Sinuses, swelling | GMS |
This table summarizes key histopathological and clinical differences for rapid reference in diagnostic pathology.
References
- Cutaneous Phaeohyphomycosis Presenting as a Progressive… — PMC/NCBI. 2020-12-01. https://pmc.ncbi.nlm.nih.gov/articles/PMC7735003/
- Subcutaneous phaeohyphomycosis caused by Cladophialophora boppii — Indian Journal of Dermatology, Venereology and Leprology. 2013-01-01. https://ijdvl.com/subcutaneous-phaeohyphomycosis-caused-by-cladophialophora-boppii/
- Phaeohyphomycosis — DynaMed. 2024-01-01. https://www.dynamed.com/condition/phaeohyphomycosis
- Phaeohyphomycosis — MSD Manuals Professional Edition. 2025-01-01. https://www.msdmanuals.com/professional/infectious-diseases/fungal-infections/phaeohyphomycosis
- Phaeohyphomycosis pathology — DermNet NZ. 2011-01-01. https://dermnetnz.org/topics/phaeohyphomycosis-pathology
Read full bio of medha deb










