Psoriatic Arthritis Pictures: Visual Guide to Symptoms
See real images of psoriatic arthritis symptoms, from skin plaques to swollen joints, to better understand this autoimmune condition.
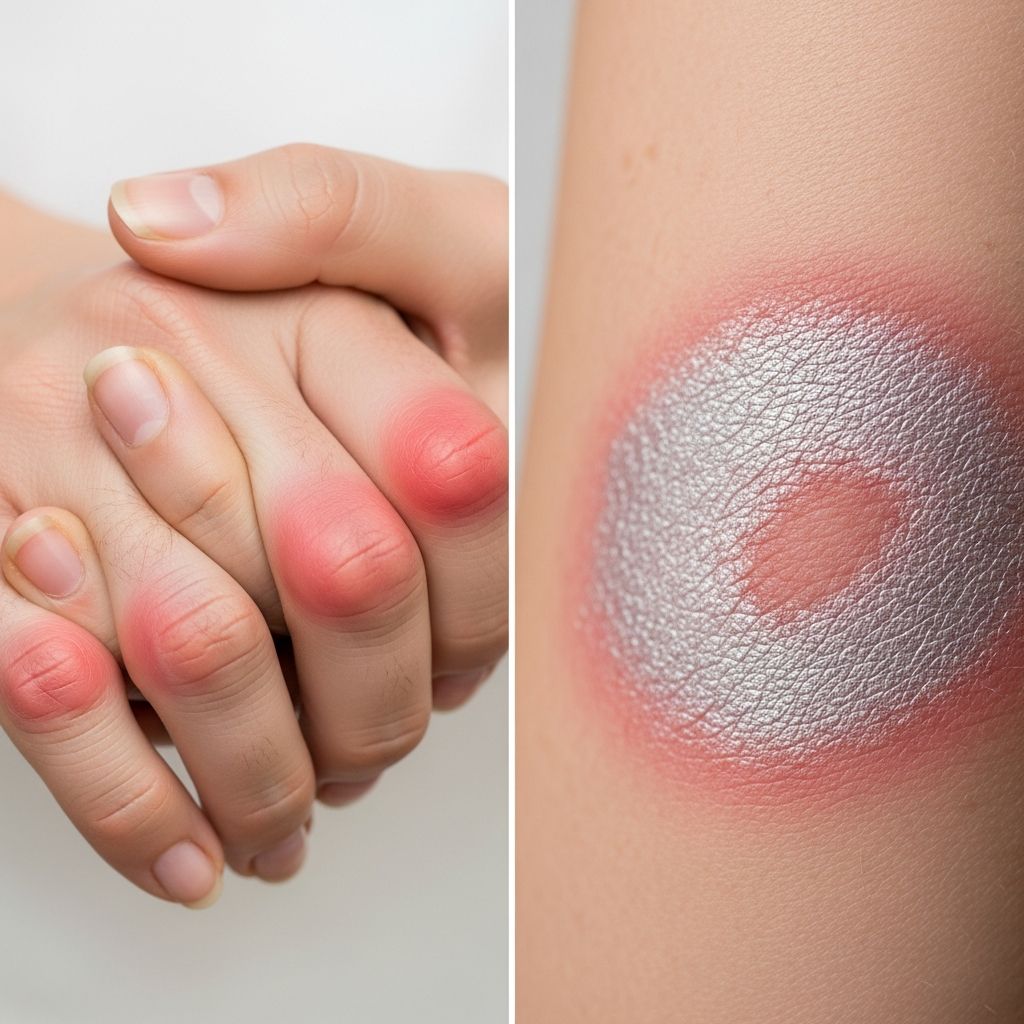
Psoriatic Arthritis Pictures: What This Autoimmune Disease Looks Like
Psoriatic arthritis (PsA) affects up to 30% of people with psoriasis, causing painful inflammation in joints, tendons, and skin. Unlike rheumatoid arthritis, PsA often spares the small joints of the hands initially and features distinctive “sausage digits.” This visual guide showcases real-world examples of PsA symptoms through patient photos and medical illustrations, helping you recognize early warning signs.
According to the National Psoriasis Foundation, PsA is an autoimmune condition where the immune system attacks healthy tissues, leading to joint damage if untreated. Early diagnosis through visual symptom recognition can prevent irreversible deformities. These images highlight the five main PsA subtypes: asymmetric oligoarticular, symmetric polyarticular, distal interphalangeal predominant, spondylitis, and arthritis mutilans.
Sausage Fingers (Dactylitis): The Classic PsA Sign
Dactylitis, or “sausage finger,” occurs when inflammation affects an entire finger or toe, causing uniform swelling. This affects 30-50% of PsA patients and differentiates PsA from other arthritides. The swelling results from flexor tenosynovitis combined with joint synovitis.

- Key features: Entire digit swelling (not just joints)
- Pain level: Often severe, worse at night
- Common sites: Toes (50% of cases), fingers
- Duration: Weeks to months without treatment
Treatment typically involves NSAIDs, corticosteroids, or biologics like TNF inhibitors. Studies show 70% improvement with early DMARD therapy. Visual tip: Look for shiny, tense skin over the swollen digit.
Nail Psoriasis: Pitting, Onycholysis, and Oil Drop Changes
Nail involvement occurs in 80% of PsA patients vs. 40% with skin psoriasis alone. Nail pitting (small depressions) correlates strongly with enthesitis and disease severity. Onycholysis (nail lifting) and the “oil drop” (salmon patch) are diagnostic hallmarks.

| Nail Finding | PsA Prevalence | Clinical Significance |
|---|---|---|
| Pitting | 60-70% | Strongest predictor of PsA development in psoriasis patients |
| Onycholysis | 50% | Nail separates from bed; prone to infection |
| Oil drop | 30% | Translucent yellow discoloration under nail |
| Hyperkeratosis | 40% | Thickened nail bed debris |
The American College of Rheumatology notes nail disease predicts worse joint outcomes. Treatments include topical steroids, systemic retinoids, or biologics targeting IL-17/IL-23 pathways.
Psoriasis Plaques on Elbows, Knees, and Scalp
Classic plaque psoriasis precedes PsA in 70% of cases. Silver-white scales over erythematous bases most commonly affect extensor surfaces. Scalp psoriasis affects 50% of PsA patients and often goes undiagnosed.

Auspitz sign: Pinpoint bleeding when scales removed. Koebner phenomenon: New lesions at trauma sites. Guttate psoriasis (small drop-like lesions) often follows streptococcal infection and may herald PsA onset.
Topical Treatments for Plaque Psoriasis
- Corticosteroids (clobetasol 0.05%)
- Vitamin D analogs (calcipotriene)
- Calcineurin inhibitors (tacrolimus)
- Combination therapy most effective
Enthesitis: Inflammation Where Tendons Meet Bone
Enthesitis (Achilles tendon, plantar fascia) affects 50% of PsA patients. Unlike RA, PsA preferentially targets tendon insertion sites. Plantar fasciitis-like heel pain is common.

- Common sites: Achilles (25%), plantar fascia (20%), elbow epicondyles
- Imaging: Ultrasound shows enthesophytes and thickening
- MRI findings: Bone marrow edema at insertion sites
IL-23 inhibitors show particular efficacy for enthesitis. Physical therapy and orthotics help manage symptoms.
Swollen, Deformed Joints: The Arthritis Component
PsA causes synovial inflammation leading to joint effusion, tenderness, and eventual deformity. The DIP joints (fingertip joints) are classically affected, unlike RA which spares them.

Five PsA patterns:
- Asymmetric oligoarthritis (most common, 40%)
- Symmetric polyarthritis (25%, RA-like)
- DIP predominant (15%)
- Spinal disease (25%, overlaps ankylosing spondylitis)
- Arthritis mutilans (5%, most destructive)
Eye Involvement: Uveitis and Conjunctivitis
Anterior uveitis affects 7-25% of PsA patients, causing painful red eye, photophobia, and blurred vision. Acute, unilateral episodes require urgent ophthalmology referral.

- Topical steroids: Prednisolone acetate 1%
- Cycloplegics: Cyclopentolate for pain relief
- Systemic biologics: Reduce uveitis recurrence
How PsA Is Diagnosed from These Visual Findings
No single test diagnoses PsA. CASPAR criteria require inflammatory musculoskeletal disease plus ≥3 points from:
- Current psoriasis (2 points)
- Personal/family psoriasis history (1 point)
- Nail dystrophy (1 point)
- Negative RF (1 point)
- Dactylitis (1 point)
Imaging: X-rays show pencil-in-cup deformity; MRI/ultrasound detect early synovitis and enthesitis before X-ray changes.
Treatment Options Based on Symptom Patterns
| Symptom | First-Line | Second-Line | Biologics |
|---|---|---|---|
| Dactylitis | NSAIDs | Local steroid injection | TNF/IL-17 inhibitors |
| Nail disease | Intralesional steroids | Methotrexate | IL-23 inhibitors |
| Enthesitis | NSAIDs + PT | Sulfasalazine | Secukinumab (IL-17) |
| Skin plaques | Topicals | Phototherapy | Ixekizumab |
Frequently Asked Questions About Psoriatic Arthritis
Can you have psoriatic arthritis without skin psoriasis?
Yes, 15-30% of PsA patients have no visible skin psoriasis, though microscopic skin involvement usually exists. Nail changes often provide the clue.
How is PsA different from osteoarthritis?
PsA causes inflammatory swelling (warm, red joints) while osteoarthritis features bony enlargement (Heberden’s nodes) without systemic symptoms. PsA patients are younger at onset.
Will PsA cripple my hands like rheumatoid arthritis?
Early aggressive treatment prevents most deformities. Only 5% develop arthritis mutilans (severe destruction). Modern biologics preserve joint function in 80% of patients.
Is dactylitis always permanent?
No, 70% resolve with treatment. Recurrent episodes signal active disease needing systemic therapy escalation.
Can diet help my psoriatic arthritis symptoms?
Anti-inflammatory Mediterranean diet reduces flares in observational studies. Weight loss improves biomechanics and drug efficacy. No specific “PsA diet” exists.
Bottom line: These visual examples empower early recognition of PsA. Consult rheumatology if you notice sausage digits, nail pitting with joint pain, or inflammatory back pain with psoriasis family history. Early intervention prevents joint destruction.
References
- Classification criteria for psoriatic arthritis — Taylor W, et al. Arthritis & Rheumatism. 2006-09-01. https://acrjournals.onlinelibrary.wiley.com/doi/10.1002/art.21563
- Psoriatic arthritis: from pathogenesis to therapy — Ritchlin CT, et al. Arthritis Research & Therapy. 2021-04-15. https://arthritis-research.biomedcentral.com/articles/10.1186/s13075-021-02459-x
- 2019 Update of ASAS-EULAR recommendations — Smolen JS, et al. Annals of the Rheumatic Diseases. 2020-06-01. https://ard.bmj.com/content/79/6/685
- Nail disease in psoriatic arthritis — National Psoriasis Foundation. 2023-11-12. https://www.psoriasis.org/psoriatic-arthritis/
- Enthesitis in psoriatic arthritis — American College of Rheumatology. 2024-02-28. https://www.rheumatology.org/I-Am-A/Patient-Caregiver/Diseases-Conditions/Psoriatic-Arthritis
Read full bio of medha deb











