Pilonidal Disease: Causes, Symptoms, and Treatment
Complete guide to pilonidal disease: understanding symptoms and exploring effective treatment options.
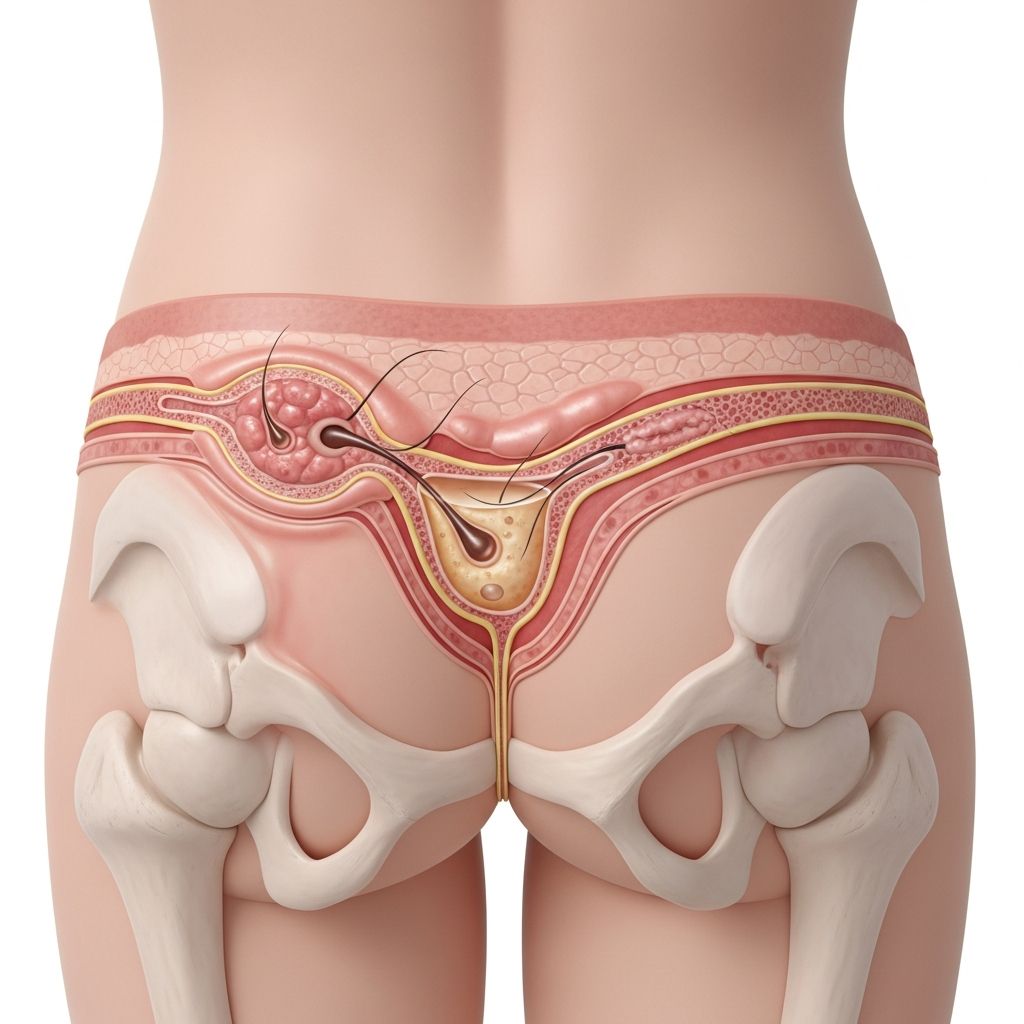
Pilonidal Disease: Overview
Pilonidal disease is a chronic skin condition that develops in the gluteal cleft, the crease between the buttocks. The condition involves the formation of small tunnels (sinuses) or lumps (cysts) in this area. Pilonidal disease is a reaction to hair in the gluteal cleft, in which unattached hairs injure or pierce the skin, resulting in a foreign body reaction. The exact cause is not entirely known, though the condition affects approximately 70,000 people annually.
This condition most commonly affects young adults and can significantly impact quality of life if left untreated. Pilonidal disease can lead to recurring issues, chronic pain, and infections if not properly managed. Understanding the nature of this condition, its symptoms, and available treatment options is essential for anyone experiencing symptoms or seeking preventive care.
Causes and Risk Factors
Pilonidal disease develops when hair in the gluteal cleft becomes problematic. The primary mechanism involves unattached hairs that injure or pierce the skin, creating a foreign body reaction. This typically results from ingrown hairs or skin debris trapped in the skin, leading to inflammation.
Several factors may contribute to the development of pilonidal disease:
- Deep gluteal cleft anatomy that traps hair and moisture
- Poor hygiene in the affected area
- Excessive body hair growth in the region
- Friction and moisture from prolonged sitting
- Family history or genetic predisposition
- Male gender (more common in men than women)
- Age, with higher prevalence in young adults
Symptoms and Clinical Presentation
Pilonidal disease may present differently depending on whether the cyst or abscess is infected. Patients may not experience any symptoms unless the area becomes infected.
Early Stage Symptoms
In its early stages, pilonidal disease may present as a small, painless lump near the tailbone. Many patients experience no noticeable symptoms until the condition progresses or becomes infected.
Active Infection Symptoms
When pilonidal disease becomes infected and develops into an abscess, symptoms become more pronounced:
- Pain and Discomfort: Persistent tenderness near the tailbone, especially when sitting or moving
- Swelling and Redness: Inflammation and redness around the affected area
- Pus or Blood Drainage: Oozing of pus or blood from a small opening in the skin, often with a foul odor
- Fever: Fever and chills if an infection is present
- Visible Cyst or Abscess: A noticeable lump or swelling that may be tender to the touch
- Hair Protrusion: Presence of hair protruding from the cyst or abscess
Chronic Disease Presentation
Patients with chronic disease most often present with chronic draining sinus disease in the intergluteal fold. In severe cases, complex disease is usually accompanied by foul-smelling drainage and makes it difficult for the patient to sit due to increased pain. Other signs of infection may include fatigue, nausea, and fever.
Diagnosis
Diagnosing pilonidal disease is typically straightforward and based on clinical presentation.
Diagnostic Process
To diagnose pilonidal disease, your doctor will complete a symptom history and physical examination. Most patients with pilonidal disease present with midline pits in the gluteal cleft, although they may also have surrounding cellulitis or abscess. The physical examination for suspected pilonidal disease should involve an anal examination to rule out fistula.
Imaging and Laboratory Tests
In most cases, radiographic imaging is unlikely to be necessary for diagnosis. However, imaging tests such as ultrasound or MRI may be used in more severe cases to evaluate the size and complexity of the cyst or abscess. Your doctor may take a swab if there is pus to determine which bacteria are causing the infection.
Differential Diagnosis
The differential diagnosis includes several conditions that may present similarly to pilonidal disease:
- Hidradenitis suppurativa
- Infected skin furuncles
- Crohn disease
- Perianal fistula
Treatment Options
The treatment process for pilonidal disease involves a combination of medical therapies, lifestyle modifications, and surgical interventions, depending on the severity of the condition.
Conservative Treatment for Non-Infected Disease
Pilonidal disease without abscess is best managed by frequent shaving or hair removal. For mild cases, conservative approaches may help reduce irritation and prevent recurrence:
- Hair Removal: Hair removal from the gluteal cleft via shaving or laser epilation is a key treatment. The optimal frequency of shaving is unclear, but the American Society of Colon and Rectal Surgeons (ASCRS) recommends at least weekly shaving
- Laser Epilation: A local anesthetic and more than one treatment session may be needed when opting for laser epilation
- Hygiene Measures: Improved hygiene and keeping the area clean and free of hair
- Warm Compresses: Warm compresses may help reduce irritation
Phenol Application
Local application of phenol is an effective treatment option that has been shown to resolve the condition in at least 67% of patients and prevent recurrences in at least 80%. Fewer than 15% of patients experience minor complications. Typically, one to four treatments of hair removal, cyst curettage, and phenol application into the cyst and tracts can result in complete resolution of the condition.
Drainage of Abscesses
The treatment for an abscess is drainage. An incision is made that allows pus to drain, reducing inflammation and pain. This procedure can usually be done in a health care provider’s office. However, chronic abscesses are usually due to cavities that have retained infection and create ongoing drainage.
Surgical Interventions for Chronic Disease
Excision and primary closure or healing by secondary intention, including marsupialization, are primary therapy options for chronic pilonidal disease with sinuses. Although primary closure has been shown to have faster healing and less time off work than healing by secondary intention, recurrence rates are slightly higher.
Flap-Based Surgical Approaches
Flap-based approaches can be used for patients with complex or recurrent disease who require a wide excision. These approaches include:
- Rhomboid flap
- Limberg flap
- Karydakis flap
- Cleft-lift procedure
Minimally Invasive Techniques
For advanced cases, minimally invasive techniques such as endoscopic pilonidal sinus treatment may be used to ensure effective treatment with minimal discomfort and downtime. These techniques provide an alternative to more extensive surgical procedures in select cases.
Complications of Untreated Disease
If left untreated, pilonidal disease can lead to significant complications. The condition can lead to recurrent infections and abscesses, resulting in chronic pain and complications such as cellulitis or systemic infections. Pilonidal disease can become a chronic condition with frequent flare-ups, affecting a person’s ability to perform everyday activities and maintain their quality of life.
When to Seek Medical Attention
It is important to seek medical attention as soon as symptoms appear. Early diagnosis and treatment can prevent the condition from worsening and reduce the risk of complications. If you think your pilonidal sinus or cyst is infected, see a doctor as soon as possible or go to your local hospital emergency department.
Frequently Asked Questions
Q: What exactly is pilonidal disease?
A: Pilonidal disease is a chronic condition involving small tunnels (sinuses) or lumps (cysts) that form in the crease between the buttocks. It results from a foreign body reaction to unattached hairs that injure or pierce the skin.
Q: How common is pilonidal disease?
A: Pilonidal disease has an annual incidence of about 70,000 cases and most commonly affects young adults.
Q: What are the first signs of pilonidal disease?
A: In early stages, pilonidal disease may present as a small, painless lump near the tailbone. Many people have no symptoms until the area becomes infected.
Q: How is pilonidal disease diagnosed?
A: Diagnosis is typically based on a symptom history and physical examination. Imaging tests such as ultrasound or MRI are usually not necessary but may be used in complex cases.
Q: Can pilonidal disease be treated without surgery?
A: Yes. For non-infected disease, conservative treatments including weekly hair removal, phenol application (which resolves disease in 67% of cases), warm compresses, and improved hygiene can be effective.
Q: What happens if pilonidal disease is left untreated?
A: Untreated pilonidal disease can lead to recurrent infections, abscesses, chronic pain, cellulitis, systemic infections, and frequent flare-ups that affect daily activities and quality of life.
Q: How often should I shave the affected area?
A: The American Society of Colon and Rectal Surgeons recommends hair removal at least weekly to prevent pilonidal disease recurrence.
Q: What surgical options are available for chronic pilonidal disease?
A: Surgical options include excision with primary closure, healing by secondary intention, marsupialization, and flap-based approaches such as rhomboid, Limberg, Karydakis, and cleft-lift procedures.
Q: Can pilonidal disease recur after treatment?
A: Yes, recurrence is possible, though rates vary by treatment method. Primary closure has faster healing but slightly higher recurrence rates compared to healing by secondary intention.
Q: When should I seek emergency medical care for pilonidal disease?
A: You should seek immediate medical attention if you suspect your pilonidal sinus or cyst is infected, as infections can lead to serious complications.
References
- Pilonidal Disease Treatment in Reston VA — Virginia Surgery Group. Accessed January 2026. https://virginiasurgerygroup.com/services/pilonidal-disease/
- Pilonidal Disease Management: Guidelines from the ASCRS — American Academy of Family Physicians (AAFP). November 1, 2019. https://www.aafp.org/pubs/afp/issues/2019/1101/p582.html
- What Is Pilonidal Disease? Causes, Symptoms, and Treatment Options — Texas Colon & Rectal Surgery. Accessed January 2026. https://www.txcolon.com/blog/1302694-what-is-pilonidal-disease-causes-symptoms-and-treatment-options/
- Understanding Pilonidal Cysts: Symptoms and Treatment — WCEI Blog. Accessed January 2026. https://blog.wcei.net/pilonidal-cyst-symptoms-treatment
- Pilonidal Disease – Symptoms and Treatment — Healthdirect. Australian Department of Health. Accessed January 2026. https://www.healthdirect.gov.au/pilonidal-disease
- Pilonidal Disease — American Society of Colon and Rectal Surgeons (ASCRS). Accessed January 2026. https://fascrs.org/Web/Web/Patients/Diseases-and-Conditions/A-Z/Pilonidal-Disease.aspx
- Pilonidal Cyst: Firm Nodule Near Anus — Dermatology Advisor. Accessed January 2026. https://www.dermatologyadvisor.com/ddi/pilonidal-cyst/
Read full bio of Sneha Tete













