Piriformis Syndrome: Symptoms, Causes and Treatment
Understanding piriformis syndrome: causes, symptoms, diagnosis, and effective treatment options.
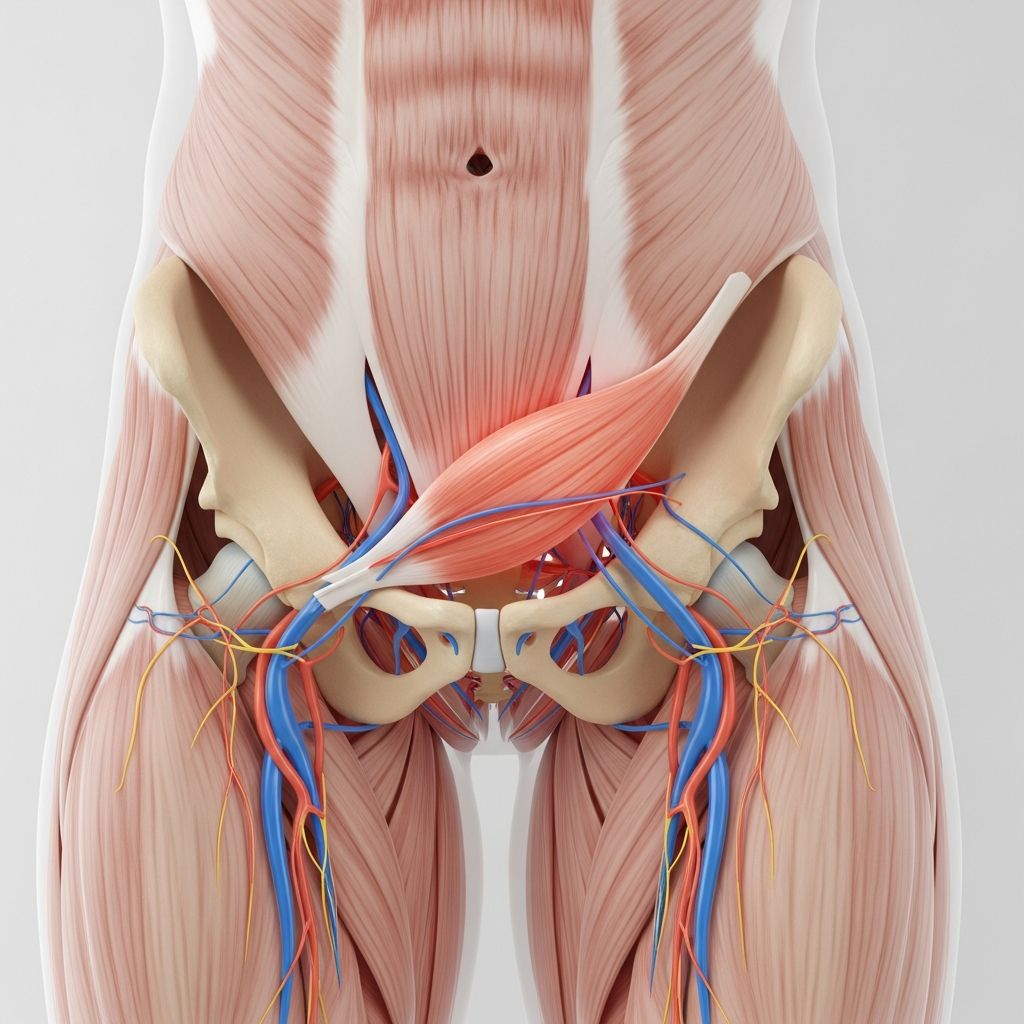
Understanding Piriformis Syndrome
Piriformis syndrome occurs when your piriformis muscle compresses your sciatic nerve and results in inflammation. This condition can cause pain or numbness in your buttock and down the back of your leg. It can happen on one side of your body or both sides, though single-sided occurrences are more common. While piriformis syndrome shares similarities with sciatica and both affect the sciatic nerve, they are distinct conditions with different underlying causes and mechanisms.
The key distinction between piriformis syndrome and sciatica is the source of nerve compression. A herniated disk or spinal stenosis causes traditional sciatica, with symptoms that tend to affect the lower back and can travel down through the buttocks and leg. Piriformis syndrome, by contrast, only involves the piriformis muscle pressing on one specific area of the sciatic nerve in the buttock. Although the pain may feel similar to sciatica, it occurs in a more localized area.
What Is the Piriformis Muscle?
The piriformis is a small, deep muscle located in the buttock region. This muscle plays a crucial role in hip movement and rotation. When functioning properly, the piriformis allows your hip to rotate and helps stabilize the hip joint. However, when this muscle becomes inflamed, tight, or goes into spasm, it can compress or irritate the sciatic nerve that runs beneath or through it, leading to piriformis syndrome symptoms.
Causes of Piriformis Syndrome
Anything that makes the piriformis press on the sciatic nerve can cause piriformis syndrome. Understanding these causes is essential for both prevention and treatment. The condition can develop from various factors, and healthcare providers often categorize piriformis syndrome into two main types:
Primary Piriformis Syndrome
Sometimes, abnormal anatomy causes piriformis syndrome, which healthcare providers call primary piriformis syndrome. This type results from structural or anatomical variations present from birth. For example, a person can be born with a sciatic nerve that takes an abnormal path in their body. Additionally, some individuals may have an unusually formed piriformis muscle or sciatic nerve that predisposes them to developing this condition.
Secondary Piriformis Syndrome
The most common causes of piriformis syndrome fall into the secondary category and include:
- Prolonged sitting or pressure on the buttocks
- Repetitive strain from activities like running or climbing stairs
- Tight hip muscles from poor posture or muscle imbalances
- Hip or buttock injuries or trauma
- Carrying objects in back pockets, particularly wallets in hip pockets
- Sacroiliac joint dysfunction affecting muscle tension
- Decreased core muscle strength, particularly in the buttocks
Piriformis Syndrome Symptoms
Piriformis syndrome symptoms occur in the butt, hip or upper leg. People often describe the feeling in various ways depending on the severity and individual presentation. Recognizing these symptoms early can help you seek appropriate treatment.
Common Symptoms
The primary symptom of piriformis syndrome is pain, which usually develops in the glutes, hip, or upper thigh. The quality of the pain may be described as:
- Aching sensation in the buttock or hip
- Shooting pain down the back of the leg
- Burning pain radiating from the buttock
- Numbness or tingling in the affected area
- Weakness in the leg or foot
If the sciatic nerve becomes entrapped, additional symptoms may develop, including weakness, numbness, or tingling that extends down the back of the leg. Some patients experience foot numbness or tingling, especially if the nerve is compressed further down.
Symptoms That Worsen With Certain Activities
Symptoms may get worse during certain activities and situations, such as:
- Sitting for extended periods, particularly on hard surfaces
- Walking, especially on uneven terrain
- Climbing stairs or hills
- Running or engaging in high-impact activities
- Driving for long distances
- Lying on the affected side
Diagnosis of Piriformis Syndrome
Diagnosing piriformis syndrome can be difficult and often involves ruling out other causes. There are no specific piriformis syndrome tests, but a healthcare provider will conduct a thorough evaluation to reach an accurate diagnosis.
Diagnostic Approach
A healthcare provider will typically:
- Review your medical history and symptoms
- Perform a physical examination, including hip rotation tests and piriformis stretch assessments
- Test for pain on internal rotation of the hip against resistance
- Assess for pain reproduction with seated piriformis stretch
- Order imaging or testing to identify other problems that might be causing your symptoms
Tests to Rule Out Other Conditions
A healthcare provider may order tests to identify other problems that might be causing your symptoms. These tests include:
- Magnetic Resonance Imaging (MRI) to visualize soft tissues and identify nerve compression
- Electrodiagnostic nerve testing to identify entrapment location in refractory cases
- X-rays to rule out bone-related issues
- Electromyography (EMG) to assess nerve function
Treatment Options for Piriformis Syndrome
Piriformis syndrome treatment may include various approaches, from conservative to interventional options. The good news is that piriformis syndrome resolves quickly with lifestyle changes and simple treatments in most cases. Symptoms often improve in days or weeks with appropriate management.
Conservative Treatment Approaches
Conservative treatment is recommended as the first option and includes:
- Rest and activity modification: Avoid activities that strain the piriformis muscle, such as running, jumping, or excessive stair climbing
- Ice and heat therapy: Apply ice during the acute phase to reduce inflammation, then heat to ease muscle tension
- Over-the-counter medications: Non-steroidal anti-inflammatory medications such as ibuprofen may help manage pain and inflammation
- Proper posture: Maintain ergonomic positioning to reduce muscle strain
Physical Therapy and Exercise
Physical therapy is highly useful for treating piriformis syndrome and preventing its recurrence. Physical therapy treatment may include strengthening and stretching exercises to reduce muscle spasms and tension and promote sciatic nerve mobilization. A consistent regimen of stretching and exercise can significantly improve symptoms. The goal is to loosen the piriformis, so it’s not irritating the sciatic nerve.
Therapists may use additional modalities such as ultrasound, electrical muscle stimulation, and heat and cold therapy. Physical therapy treatment plans are individualized for each patient based on the severity of their symptoms and overall health and may last several weeks.
Interventional Pain Management
When conservative care isn’t sufficient, interventional techniques may be offered:
- Piriformis muscle injections: Using a local anesthetic and corticosteroid to reduce inflammation and break the pain cycle
- Botox injections: To temporarily paralyze and relax the piriformis muscle
- Nerve blocks: For longer-term pain relief, especially in chronic cases
Surgical Treatment
Piriformis syndrome surgery is usually not recommended unless all other therapies fail. Surgery for this condition may involve removing scar tissue or other sources of pressure on the nerve. If your piriformis syndrome is severe and doesn’t respond to any conservative or interventional treatment, you may benefit from surgery.
Prognosis and Recovery
Most cases of piriformis syndrome have a favorable prognosis when managed appropriately. The condition tends to resolve quickly with proper treatment, with symptoms often improving in days or weeks. However, the condition tends to come back, especially in people who don’t follow their healthcare provider’s instructions. Severe cases that aren’t treated properly can greatly reduce a person’s ability to function well.
Prevention Strategies
To prevent piriformis syndrome, including recurrent (repeat) episodes, consider some of the following strategies:
- Maintain good posture throughout the day, especially when sitting
- Take regular breaks from sitting, particularly during long work sessions
- Avoid carrying heavy objects in back pockets, especially wallets in hip pockets
- Strengthen core muscles through regular exercise
- Stretch hip muscles regularly, especially before and after physical activity
- Use proper ergonomics at your workspace
- Warm up before exercise and cool down afterward
- Avoid high-impact activities if you’re prone to this condition
- Maintain a healthy weight to reduce stress on hip muscles
- Sleep on your back or unaffected side to avoid pressure on the piriformis
Managing Symptoms at Home
If you have piriformis syndrome, certain adjustments can help you manage the symptoms when they occur:
- Apply ice packs for 15-20 minutes several times daily during the acute phase
- Use heat therapy after the acute phase to relax muscles
- Avoid sitting for prolonged periods; use a cushion if sitting is necessary
- Perform gentle stretching exercises as recommended by your healthcare provider
- Use over-the-counter pain relievers as directed
- Modify your activities to avoid aggravating the condition
- Practice proper lifting techniques to avoid straining the muscle
- Consider using a standing desk or adjustable work surface
When to Contact Your Healthcare Provider
If you have piriformis syndrome, call your healthcare provider if you experience any of the following:
- Symptoms that persist beyond a few weeks despite home treatment
- Severe pain that interferes with daily activities or sleep
- An injury led to the pain
- Progressive weakness or numbness in your leg or foot
- Loss of bladder or bowel control
- Fever accompanying your symptoms
- Symptoms that worsen despite treatment
- Difficulty walking or balance problems
Frequently Asked Questions
Q: How long does piriformis syndrome typically last?
A: Most episodes of piriformis syndrome resolve within days or weeks with appropriate treatment. However, the condition can recur, especially if preventive measures are not followed and underlying causes are not addressed.
Q: Is piriformis syndrome the same as sciatica?
A: No. While both conditions can affect the sciatic nerve and cause similar symptoms, they are different. Sciatica is typically caused by a herniated disk or spinal stenosis affecting the lower back, whereas piriformis syndrome involves compression by the piriformis muscle in the buttock.
Q: Can piriformis syndrome be cured?
A: Yes, piriformis syndrome is manageable and treatable. Most cases respond well to conservative treatment including rest, stretching, physical therapy, and lifestyle modifications. Surgery is rarely needed and is typically considered only when all other treatments fail.
Q: What percentage of sciatica cases are due to piriformis syndrome?
A: According to medical literature, piriformis syndrome may account for 0.5% to 17% of cases of sciatica and low back pain, with the variation depending on the population studied and diagnostic criteria used.
Q: Are women more likely to develop piriformis syndrome?
A: Yes, piriformis syndrome affects more women than men and is particularly common in middle-aged patients.
Q: Can I exercise with piriformis syndrome?
A: Yes, appropriate exercise is beneficial. However, avoid high-impact activities like running, jumping, and excessive stair climbing that may strain the muscle. Focus on gentle stretching, strengthening exercises, and low-impact activities like walking and swimming. Always consult your healthcare provider before starting a new exercise routine.
Q: What ergonomic changes can help prevent piriformis syndrome?
A: Maintain proper posture, use ergonomic chairs with good lumbar support, take frequent breaks from sitting, avoid pressure on the buttocks, and keep your workspace at an appropriate height for your body.
Conclusion
Piriformis syndrome occurs when the piriformis muscle presses on the sciatic nerve, resulting in inflammation and pain, numbness, or tingling in your butt, hip, or upper leg. Most episodes go away in a few days or weeks with rest and simple treatments such as stretching, physical therapy, and lifestyle modifications. The condition can recur if preventive measures are not followed, but understanding the causes and implementing appropriate prevention strategies can significantly reduce the risk of future episodes. If an injury led to the pain or if symptoms last more than a few weeks, it is important to talk to your healthcare provider to ensure proper diagnosis and treatment.
References
- Piriformis Syndrome: Symptoms, Causes and Treatment — Cleveland Clinic. 2022-07-13. https://my.clevelandclinic.org/health/diseases/23495-piriformis-syndrome
- What is Piriformis Syndrome and How Can It Be Treated? — ASAP Pain Docs. https://www.asappaindocs.com/articles/what-piriformis-syndrome-and-how-can-it-be-treated
- Is Your Leg Pain Sciatica or Something Else? — Cleveland Clinic. https://health.clevelandclinic.org/is-your-leg-pain-sciatica-or-something-else
- Sciatica: What It Is, Causes, Symptoms, Treatment & Pain Relief — Cleveland Clinic. https://my.clevelandclinic.org/health/diseases/12792-sciatica
- 7 Best Stretches & Exercises for Piriformis Syndrome — Cleveland Clinic. https://health.clevelandclinic.org/piriformis-syndrome-stretches-exercises
- Piriformis Syndrome – FPnotebook — Family Practice Notebook. https://mobile.fpnotebook.com/Ortho/Neuro/PrfrmsSyndrm.htm
Read full bio of medha deb











