Pitted Keratolysis Pathology: Understanding the Infection
Explore the bacterial pathology, mechanisms, and clinical manifestations of pitted keratolysis.
Pitted Keratolysis: Understanding the Pathology
Pitted keratolysis, also known as keratolysis plantare sulcatum or ringed keratolysis, is a superficial bacterial skin infection characterized by distinctive crater-like pits and malodorous odor. The condition represents a unique pathological process involving bacterial degradation of the stratum corneum and keratin-rich structures of the epidermis. Understanding the pathology of this infection is essential for dermatologists, podiatrists, and healthcare providers to effectively diagnose, treat, and prevent this common yet often overlooked condition.
Overview of Pitted Keratolysis Pathology
Pitted keratolysis is fundamentally a bacterial dermatosis that involves the keratin-rich, weight-bearing areas of the feet and, less commonly, the palms. Unlike other infectious skin conditions caused by extrinsic organisms, such as tinea pedis (which is fungal in nature), pitted keratolysis results from an overgrowth of the patient’s own skin flora under specific environmental conditions. This distinction is critical in understanding the pathological mechanism, as the infection does not represent an invasion by foreign pathogens but rather a dysbiosis of normal cutaneous bacteria.
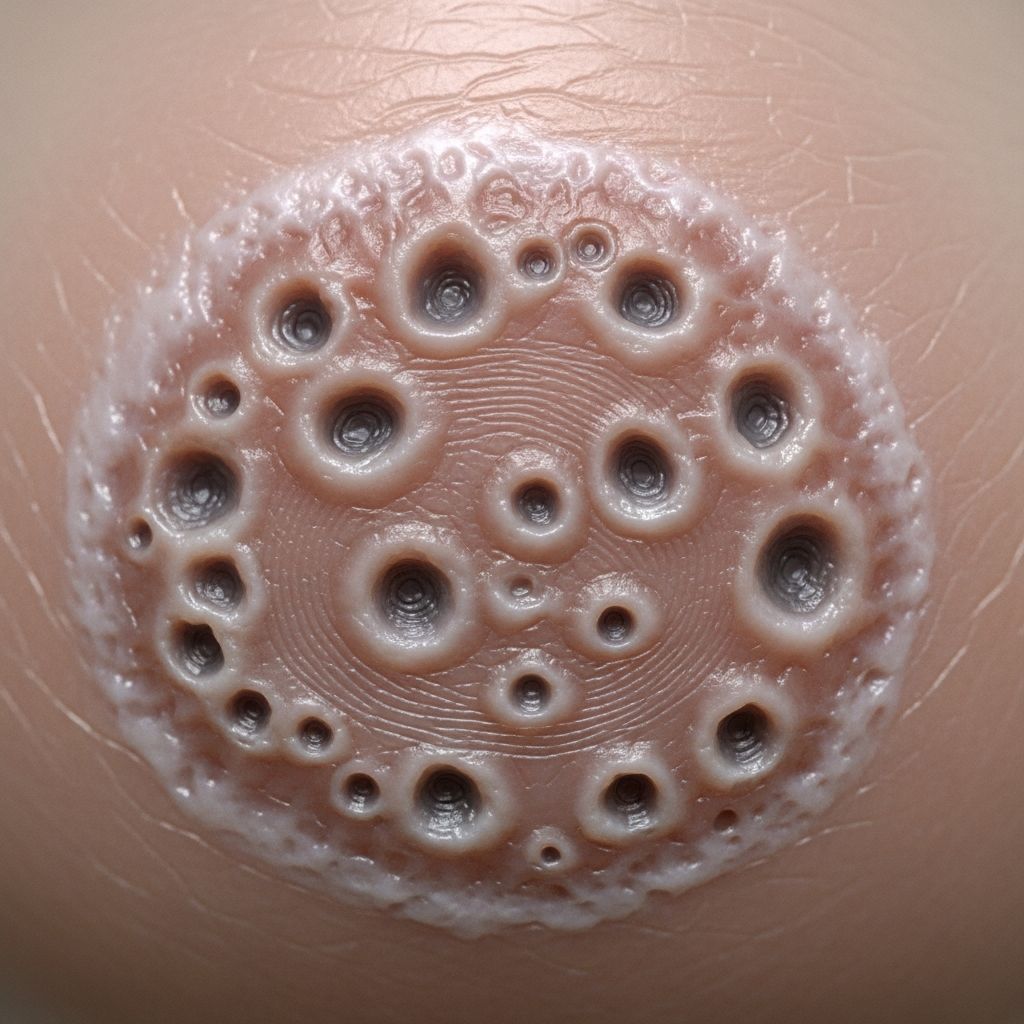
The pathological hallmark of pitted keratolysis is the formation of multiple small depressions or pits in the stratum corneum, typically ranging from 0.5 to 7 millimeters in diameter. These crater-like lesions may appear individually or cluster together, sometimes merging to form larger erosions in the skin. The pits tend to be more noticeable and pronounced when the affected skin is wet, highlighting the moisture-dependent nature of this condition’s manifestation.
Bacterial Etiology and Microbiology
The primary causative agents of pitted keratolysis are bacteria from the genus Corynebacterium, along with other gram-positive bacteria. The most commonly implicated species include Corynebacterium minutissimum, Corynebacterium fimi, and various other Corynebacterium species that naturally inhabit human skin. These bacteria are not considered pathogenic in the traditional sense; rather, they become problematic when environmental conditions favor their excessive proliferation.
The bacterial species responsible for pitted keratolysis share a common characteristic: they produce proteolytic enzymes known as keratinolytic enzymes or proteases. These enzymes are capable of degrading keratin and other structural proteins found in the stratum corneum. The presence of these enzymes is the fundamental mechanism underlying the pathological process of pit formation and tissue destruction.
Enzymatic Mechanism of Tissue Destruction
The pathological process of pitted keratolysis centers on the production of bacterial enzymes that dissolve and degrade the stratum corneum. The stratum corneum, also known as the horny layer, is the outermost layer of the epidermis composed primarily of dead keratinocytes and keratin protein. When Corynebacterium species produce their proteolytic enzymes, these enzymes break down the structural integrity of the stratum corneum, resulting in the characteristic pitting and erosion observed clinically.
The enzymatic degradation process is highly specific to the stratum corneum because this layer is composed almost entirely of keratin and dead skin cells that have undergone keratinization. The proteases produced by Corynebacterium species have evolved to specifically target these keratin structures, making the stratum corneum particularly vulnerable to bacterial colonization and degradation. This explains why pitted keratolysis primarily affects weight-bearing areas such as the soles of the feet and palms of the hands—these areas experience the greatest moisture accumulation and skin maceration.
Sulfur Compound Production and Malodor
One of the most characteristic and troublesome features of pitted keratolysis pathology is the production of sulfur-containing compounds that create a foul odor. As the proteolytic enzymes degrade the stratum corneum and keratin proteins, bacterial metabolism produces sulfur by-products as part of the catabolic process. These volatile sulfur compounds, including dimethyl disulfide and other mercaptans, are responsible for the distinctive unpleasant foot odor that often accompanies pitted keratolysis.
The sulfur compounds are generated during the bacterial degradation of sulfur-containing amino acids (particularly methionine and cysteine) present in keratin proteins. This metabolic byproduct is not merely an incidental consequence of the infection but rather an integral part of the pathological process. The intensity of the malodor often correlates with the degree of bacterial colonization and the extent of stratum corneum degradation, making it a clinically useful indicator of disease severity.
Environmental Factors in Pathological Development
Moisture and Hyperhidrosis
The development and progression of pitted keratolysis pathology are fundamentally dependent on elevated moisture levels within the stratum corneum and surrounding microenvironment. Hyperhidrosis (excessive sweating) creates an ideal environment for bacterial proliferation by maintaining prolonged moisture in weight-bearing areas of the feet. When sweat persists on the skin surface for extended periods, it leads to maceration—a pathological process where the stratum corneum becomes softened, hydrated, and more permeable to bacterial invasion and colonization.
The moisture-dependent nature of pitted keratolysis explains why the condition is more prevalent in individuals who wear occlusive footwear that restricts air circulation and creates warm, moist microenvironments. Shoes that limit airflow trap perspiration against the skin, creating ideal conditions for bacterial overgrowth and enzymatic activity. This is particularly significant in occupational settings where individuals wear enclosed footwear for extended periods, such as farmers, soldiers, and athletes.
pH Alterations
In addition to moisture, alterations in skin pH contribute significantly to the pathological development of pitted keratolysis. Normal skin surface maintains a slightly acidic pH of approximately 4.5 to 5.5. However, in areas prone to pitted keratolysis, factors such as prolonged moisture exposure, sweat accumulation, and bacterial colonization can elevate the local skin pH toward neutral or slightly alkaline levels. This elevated pH favors the growth and metabolic activity of Corynebacterium species while simultaneously reducing the antimicrobial activity of the skin’s natural acid mantle.
The pH elevation creates a pathologically favorable microenvironment that supports bacterial proliferation while compromising the skin’s natural protective mechanisms. This interaction between elevated pH and bacterial overgrowth represents a critical factor in the transition from asymptomatic colonization to clinically evident disease.
Poor Hygiene and Maceration
Poor hygiene practices and inadequate foot care contribute to pathological development by allowing bacterial colonization to persist and expand. When skin hygiene is compromised, dead skin cells accumulate, providing additional substrate for bacterial proteolytic enzymes. Maceration of the stratum corneum due to prolonged moisture exposure further compromises the skin barrier, allowing deeper bacterial penetration and more extensive enzymatic degradation.
Pathological Characteristics of Lesions
Stratum Corneum Involvement
The pathological process of pitted keratolysis is confined entirely to the stratum corneum and does not extend into deeper dermal structures. This superficial nature of the infection is crucial for understanding both the clinical presentation and the treatment response. The bacterial enzymes degrade the stratum corneum in a selective manner, creating multiple small indentations rather than causing true ulceration or deeper tissue destruction.
The pits characteristic of this condition represent areas where the stratum corneum has been partially or completely degraded by bacterial enzymes. The appearance of these pits may vary depending on the hydration state of the skin. When the affected area is wet, capillary forces cause the pits to become more pronounced and darker in appearance, making them more visually apparent. This moisture-dependent visibility is an important diagnostic feature that distinguishes pitted keratolysis from other superficial skin conditions.
Erosion and Pit Coalescence
In advanced cases of pitted keratolysis, individual pits may coalesce or merge together to form larger erosions in the skin. This coalescence represents progressive bacterial degradation of larger areas of the stratum corneum. The pattern of coalescence typically reflects the distribution of bacterial colonization and the intensity of enzymatic activity in affected areas. Without appropriate treatment, the pits may progress from discrete, isolated lesions to a confluent erosive process affecting substantial portions of the plantar surface.
Inflammation Status and Immune Response
A distinctive pathological feature of pitted keratolysis is the relative absence of significant inflammation. Unlike many other bacterial skin infections that are characterized by erythema (redness) and edema (swelling), pitted keratolysis typically does not produce a pronounced inflammatory response. The stratum corneum, being composed of dead cells with limited ability to mount inflammatory responses, does not generate the typical signs of infection such as redness or swelling.
The lack of inflammation represents an important pathological distinction that can assist in clinical diagnosis. The absence of erythema and swelling, combined with the characteristic odor and visible pitting, helps differentiate pitted keratolysis from other infectious and inflammatory foot conditions. However, in some cases, secondary inflammation may develop if the skin becomes macerated and irritated or if secondary bacterial colonization occurs.
Risk Factors and Predisposing Conditions
Occupational and Behavioral Factors
The pathology of pitted keratolysis is significantly influenced by occupational activities and behavioral patterns that increase exposure to moisture and occlusive footwear. Individuals in professions requiring prolonged use of enclosed footwear—such as military personnel, farmers, miners, and athletes—experience higher rates of infection due to sustained creation of the moist, warm microenvironment required for pathological bacterial proliferation.
Host Factors
Certain host factors predispose individuals to developing pitted keratolysis pathology. Immunocompromised individuals, those with diabetes, overweight individuals, and those with poor hygiene have increased susceptibility to symptomatic disease. Additionally, research indicates that pitted keratolysis occurs more frequently in males than females, suggesting possible contributions from sex-related differences in sweat production, footwear practices, or cutaneous microbiota composition.
Genetic and familial factors may also influence pathological susceptibility. Studies have documented familial clustering of pitted keratolysis, suggesting that genetic predispositions and/or similar environmental exposures within families may contribute to disease development.
Clinical Manifestations of Pathological Process
Symptomatic Versus Asymptomatic Disease
Interestingly, pitted keratolysis pathology can manifest as either symptomatic or asymptomatic disease. Many individuals with characteristic pit formation and bacterial colonization experience no symptoms other than the malodor. In symptomatic cases, patients may report pruritus (itching), pain during walking, and the burning sensation associated with the affected areas. When symptoms do occur, they may be related to secondary maceration, irritation of the degraded stratum corneum, or associated hyperhidrosis rather than to the bacterial infection itself.
Frequently Asked Questions
Q: What exactly causes the pit formation in pitted keratolysis?
A: Pit formation results from bacterial enzymes (proteases) produced by Corynebacterium species degrading and dissolving the stratum corneum, the outermost layer of skin composed primarily of dead keratinocytes and keratin protein. This enzymatic degradation creates the characteristic crater-like indentations.
Q: Why does pitted keratolysis primarily affect the feet?
A: The feet are primarily affected because they experience the greatest moisture accumulation from sweating, are often confined in occlusive footwear, and have weight-bearing areas where sweat and moisture concentrate, creating ideal conditions for bacterial overgrowth and enzymatic activity.
Q: Can pitted keratolysis affect areas other than the feet?
A: While rare, pitted keratolysis can affect the palms of the hands, particularly in individuals with certain occupations such as rice paddy farmers who work in moist conditions. The pathological process is identical in these locations but occurs much less frequently.
Q: Why is there often no inflammation in pitted keratolysis despite it being a bacterial infection?
A: Because the infection is limited to the stratum corneum—composed of dead cells incapable of mounting inflammatory responses—pitted keratolysis typically does not produce the redness and swelling associated with other bacterial skin infections. The lack of living cells in the affected layer limits inflammatory signaling.
Q: How do sulfur compounds contribute to the pathological process?
A: Sulfur compounds are produced as metabolic byproducts when bacterial enzymes degrade sulfur-containing amino acids in keratin proteins. These volatile compounds create the characteristic foul odor and indicate active bacterial degradation of the stratum corneum.
Understanding Disease Pathology for Clinical Management
Comprehending the underlying pathology of pitted keratolysis is essential for effective clinical management. The superficial nature of the infection, the moisture-dependent environment required for disease development, and the specific enzymatic mechanisms of tissue destruction all inform treatment strategies and preventive approaches. Recognition of the pathological mechanisms helps clinicians predict which patients are at highest risk, understand why certain environments promote disease development, and implement targeted interventions addressing the specific pathological factors driving bacterial overgrowth and tissue degradation.
References
- Pitted Keratolysis: Symptoms, Treatment, and More — WebMD. 2024. https://www.webmd.com/skin-problems-and-treatments/what-is-pitted-keratolysis
- Keratolysis, Pitted — Unbound Medicine, 5-Minute Clinical Consult. 2024. https://www.unboundmedicine.com/5minute/view/5-Minute-Clinical-Consult/1688695/3.0/Keratolysis_Pitted
- Pitted Keratolysis: Symptoms, Causes, and Treatment Options — Anderson Podiatry Center. 2024. https://andersonpodiatrycenter.com/2024/12/02/do-you-have-stinky-itchy-feet-you-may-have-pitted-keratolysis/
- Pitted Keratolysis: Causes, Symptoms, and How to Treat It — Medical News Today. 2024. https://www.medicalnewstoday.com/articles/326911
- Pitted Keratolysis: What It Is, Causes & Treatment — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/23285-pitted-keratolysis
- Pitted Keratolysis: an Infective Cause of Foot Odour — National Center for Biotechnology Information (NCBI/PMC). 2014. https://pmc.ncbi.nlm.nih.gov/articles/PMC4401600/
- What is Pitted Keratolysis? — Primary Care Dermatology Society. 2024. https://www.pcds.org.uk/files/pils/Pitted-keratolysis-PDF.pdf
- Pitted Keratolysis: Symptoms, Causes, and Treatment — DermNet. 2022. https://dermnetnz.org/topics/pitted-keratolysis
Read full bio of Sneha Tete