Plaque Psoriasis on Scalp: Symptoms and Treatment
Understand plaque psoriasis on the scalp: causes, symptoms, treatments, and expert tips for effective management and relief.
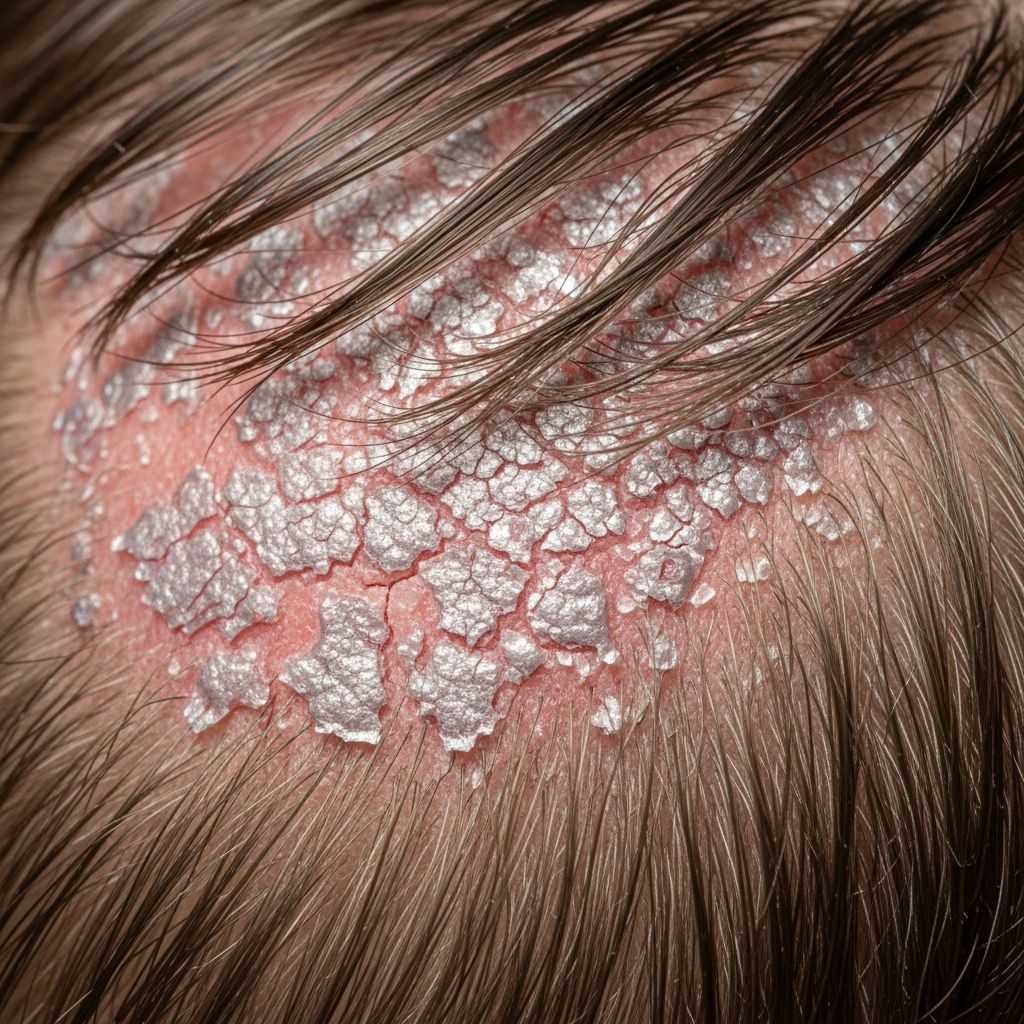
Plaque Psoriasis on Scalp: Symptoms, Causes, and Treatments
Plaque psoriasis is the most common form of psoriasis, affecting up to 80-90% of people with the condition. When it occurs on the scalp, it presents unique challenges due to hair coverage and daily washing routines. This chronic autoimmune disease causes rapid skin cell turnover, leading to thick, scaly patches. Scalp plaque psoriasis impacts millions worldwide, often starting in early adulthood, and requires targeted management for relief.
What Is Scalp Psoriasis?
Scalp psoriasis, specifically plaque type, manifests as red, inflamed patches covered with silvery-white scales on the scalp. Unlike dandruff, these plaques are thicker and more persistent. The condition can extend beyond the hairline to the forehead, neck, ears, and even the upper back. According to the National Psoriasis Foundation, scalp psoriasis affects about 45-56% of all psoriasis patients at some point.
The plaques form because the immune system triggers skin cells to grow too quickly—up to 10 times faster than normal. This buildup creates visible lesions that itch, burn, or bleed when scratched. Severity ranges from mild (small patches) to severe (covering the entire scalp), influencing treatment choices.
Symptoms of Plaque Psoriasis on the Scalp
Recognizing symptoms early is key to managing scalp plaque psoriasis. Common signs include:
- Red or salmon-colored patches: Inflamed skin under the hair, often with defined borders.
- Silvery-white scales: Thick, dry buildup that flakes off, resembling severe dandruff.
- Itching and soreness: Intense pruritus leading to scratching, which worsens plaques and risks infection.
- Burning or stinging sensation: Particularly around the ears or hairline.
- Dry skin and cracking: Plaques may crack and bleed, especially in dry climates.
- Temporary hair loss: Due to severe scratching or thick plaques, though hair usually regrows.
Symptoms often worsen in winter due to low humidity and less sun exposure. Stress, infections, or skin injuries can trigger flares. In children, plaques may appear thinner and less scaly.
Causes and Risk Factors
Plaque psoriasis on the scalp stems from a combination of genetic, immune, and environmental factors. T-cells (a type of white blood cell) mistakenly attack healthy skin cells, causing inflammation and overproduction.
Key risk factors include:
- Genetics: Family history increases risk; if one parent has psoriasis, the child has a 10-25% chance.
- Triggers: Stress, cold weather, smoking, heavy alcohol use, infections (like strep throat), and skin trauma (Koebner phenomenon).
- Other conditions: Linked to obesity, diabetes, heart disease, and psoriatic arthritis (affecting 30% of patients).
It’s not contagious, but immune dysregulation plays a central role, as confirmed by studies from the American Academy of Dermatology.
How Is Scalp Psoriasis Diagnosed?
Diagnosis typically relies on clinical examination by a dermatologist. No single test confirms it, but doctors assess:
- Appearance and location of plaques.
- Patient history of triggers and family psoriasis.
- Symptom duration and response to prior treatments.
If needed, a skin biopsy rules out conditions like seborrheic dermatitis, fungal infections, or eczema. Dermoscopy or Wood’s lamp exams may aid visualization under hair. Early diagnosis prevents complications like secondary infections.
Treatment Options for Scalp Plaque Psoriasis
Treatment aims to reduce inflammation, remove scales, and slow cell growth. Options are tailored by severity:
Topical Treatments
First-line for mild cases. Applied directly to the scalp.
- Corticosteroids: Clobetasol foam or solution reduces inflammation quickly (e.g., Temovate). Use 2-4 weeks to avoid side effects like skin thinning.
- Vitamin D analogs: Calcipotriene (Dovonex) slows cell growth; often combined with steroids.
- Retinoids: Tazarotene gel normalizes skin turnover.
- Calcineurin inhibitors: Tacrolimus ointment for sensitive areas like ears.
- Salicylic acid shampoos: Loosens scales (e.g., Neutrogena T/Sal).
Phototherapy
UVB light slows skin cell growth. Scalp-specific devices or excimer laser target plaques. Sessions 2-3 times weekly; effective for moderate cases but requires clinic visits.
Systemic Medications
For severe or widespread psoriasis:
- Oral retinoids: Acitretin reduces plaques but causes dry skin.
- Methotrexate or cyclosporine: Immunosuppressants for rapid control.
Biologics
Injected or infused drugs target immune pathways (e.g., IL-17/IL-23 inhibitors like secukinumab or guselkumab). Highly effective for scalp psoriasis, with 70-90% clearance rates in trials.
| Treatment Type | Examples | Best For | Potential Side Effects |
|---|---|---|---|
| Topical | Clobetasol, Calcipotriene | Mild scalp plaques | Skin thinning, irritation |
| Phototherapy | UVB, Excimer laser | Moderate cases | Burns, increased skin cancer risk |
| Systemic | Methotrexate, Acitretin | Severe, widespread | Liver damage, birth defects |
| Biologics | Secukinumab, Ixekizumab | Refractory severe | Infection risk, injection reactions |
Home Remedies and Lifestyle Tips
Complement medical treatments with these strategies:
- Gentle shampoos: Coal tar (MG217) or ketoconazole reduces scaling.
- Moisturize: Coconut oil or aloe vera soothes dry scalp.
- Scale removal: Apply oil overnight, comb gently in morning.
- Avoid triggers: Manage stress via yoga/meditation; quit smoking.
- Diet: Anti-inflammatory foods like fatty fish, berries; limit alcohol.
- Sun exposure: 10-15 minutes daily, with protection.
Over-the-counter options like hydrocortisone provide mild relief but consult a doctor first.
When to See a Doctor
Seek care if:
- Plaques spread or don’t improve with OTC treatments.
- Severe pain, pus, or fever indicates infection.
- Hair loss persists or joint pain emerges (psoriatic arthritis sign).
- Emotional distress from appearance affects quality of life.
Dermatologists offer personalized plans; telehealth options expand access.
Living with Scalp Psoriasis
Though incurable, scalp plaque psoriasis is manageable. Track flares in a journal, join support groups like the National Psoriasis Foundation, and prioritize mental health. New therapies continue to improve outcomes, with many achieving clear skin.
Frequently Asked Questions (FAQs)
What does plaque psoriasis on the scalp look like?
Red, raised patches with thick silvery scales, often itchy and extending to ears or neck.
Is scalp psoriasis the same as dandruff?
No, dandruff is milder flaking from seborrheic dermatitis; psoriasis plaques are thicker and inflamed.
Can scalp psoriasis cause hair loss?
Temporarily yes, from scratching or thick scales, but hair regrows with treatment.
How long does it take for treatments to work?
Topicals: 2-4 weeks; biologics: 12-16 weeks for full effect.
Is scalp psoriasis curable?
No, but remissions are common with consistent management.
References
- Psoriasis Clinical Guideline — American Academy of Dermatology. 2024-01-15. https://www.aad.org/member/clinical-quality/guidelines/psoriasis
- Scalp Psoriasis: Symptoms, Causes, and Treatment — National Psoriasis Foundation. 2025-03-10. https://www.psoriasis.org/scalp/
- Diagnosis and Management of Psoriasis — National Institute for Health and Care Excellence (NICE). 2023-11-22. https://www.nice.org.uk/guidance/cg153
- Biologics for Moderate-to-Severe Plaque Psoriasis — PubMed (DOI: 10.1001/jamadermatol.2022.5557). 2024-06-01. https://pubmed.ncbi.nlm.nih.gov/35788645/
- Psoriasis: Practice Essentials — Medscape (StatPearls, NCBI). 2025-09-05. https://www.ncbi.nlm.nih.gov/books/NBK547890/
Read full bio of Sneha Tete











