Pleurisy: Expert Guide To Symptoms, Causes, And Treatment
Understand pleurisy symptoms, causes, diagnosis, treatment, and prevention for sharp chest pain relief.
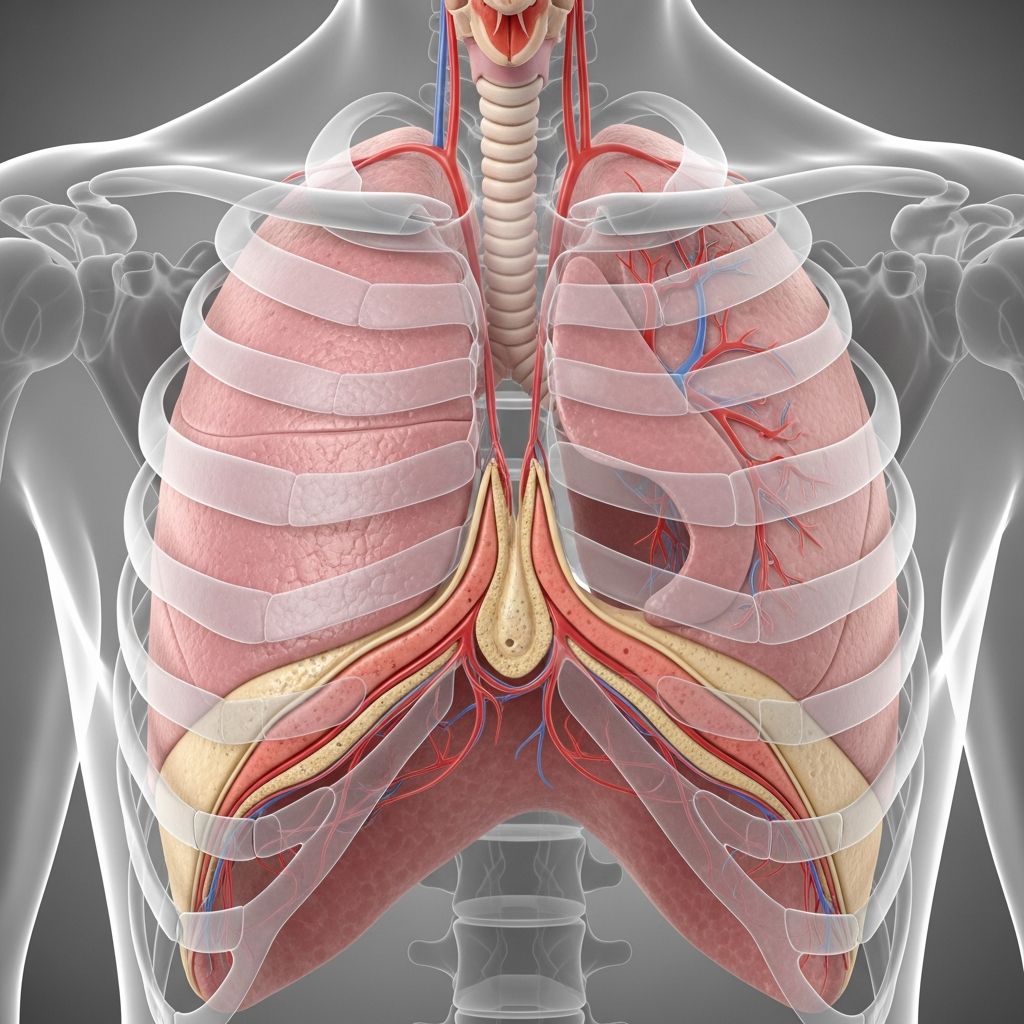
Pleurisy Overview
Pleurisy, also known as pleuritis, is the inflammation of the pleura, the thin membranes that line the lungs and chest cavity, leading to sharp chest pain worsened by breathing, coughing, or movement.
What Is Pleurisy?
The pleura consists of two layers: the visceral pleura covering the lungs and the parietal pleura lining the chest wall and diaphragm. A small amount of pleural fluid between these layers allows smooth lung movement during respiration. In pleurisy, inflammation causes these layers to rub together, producing pain and sometimes a detectable friction rub.
Pleurisy can be dry, with minimal fluid and direct friction, or wet, involving pleural effusion where excess fluid accumulates, potentially compressing the lung.
Pleurisy Symptoms
The hallmark symptom of pleurisy is sharp, stabbing chest pain that intensifies with deep breaths, coughing, sneezing, or chest movement. Pain may localize to one side or radiate to the shoulder, neck, or abdomen.
Other common symptoms include:
- Shortness of breath or rapid breathing (tachypnea)
- Cough, which may be dry or productive
- Fever and chills, especially if infection-related
- Fatigue and unexplained weight loss in chronic cases
- Bluish lips or fingernails (cyanosis) in severe cases
- Pleural friction rub, a grating sound heard via stethoscope
Symptoms vary by cause and severity; mild cases may present only as cough or discomfort, while severe ones mimic heart attack or pulmonary embolism.
What Causes Pleurisy?
Pleurisy rarely occurs alone; it typically results from underlying conditions irritating the pleura. Common causes include:
- Infections: Viral (e.g., flu, COVID-19), bacterial (pneumonia, tuberculosis), or fungal
- Autoimmune diseases: Lupus, rheumatoid arthritis, Sjögren’s syndrome
- Pulmonary issues: Pulmonary embolism, pneumothorax, asbestosis
- Trauma: Rib fractures, chest injuries, or recent surgery
- Other: Cancer (lung, mesothelioma), pancreatitis, heart attack aftermath, kidney failure, drug reactions
In some cases, no cause is identified (idiopathic pleurisy).
Pleurisy Diagnosis
Diagnosis begins with medical history and physical exam, focusing on pleuritic pain and friction rub detection via stethoscope.
Key tests include:
- Chest X-ray to identify effusion, pneumonia, or collapse
- CT scan or ultrasound for detailed imaging
- Blood tests for infection markers, autoimmune antibodies
- Electrocardiogram (ECG) to rule out heart issues
- Thoracentesis (fluid aspiration) for analysis if effusion present
- Bronchoscopy or biopsy in suspected cancer
Differentiating pleurisy from mimics like heart attack or pneumothorax is critical.
Pleurisy Treatment
Treatment targets the underlying cause while managing symptoms. Pain relief is primary using NSAIDs (ibuprofen) or prescription analgesics; opioids for severe pain.
| Condition | Treatment Approach |
|---|---|
| Viral infection | Supportive care; resolves in 1-2 weeks |
| Bacterial pneumonia | Antibiotics |
| Autoimmune | Corticosteroids, immunosuppressants |
| Pleural effusion | Thoracentesis or chest tube drainage |
| Pulmonary embolism | Anticoagulants |
Supplemental oxygen aids breathing; hospitalization for complications like empyema (infected effusion).
Complications of Pleurisy
Untreated pleurisy risks:
- Pleural effusion: Fluid buildup easing friction but compressing lungs
- Atelectasis: Lung collapse from pressure
- Empyema: Pus-filled effusion requiring drainage and antibiotics
- Pneumothorax: Lung collapse from air leak
- Chronic pain or scarring in recurrent cases
Addressing the root cause prevents progression.
Pleurisy Prevention
Preventive measures focus on reducing risk factors:
- Vaccinations against flu, pneumonia, COVID-19
- Prompt treatment of respiratory infections
- Autoimmune disease management
- Smoking cessation to lower lung cancer/asbestosis risk
- Anticoagulation for clot-prone individuals
- Protective gear to avoid chest trauma
Early intervention minimizes pleurisy development.
When to See a Doctor for Pleurisy
Seek immediate care for sudden severe chest pain, especially with shortness of breath, fever, coughing blood, or rapid heartbeat—these signal emergencies like embolism or pneumothorax.
Consult a doctor for persistent pain > few days, worsening symptoms, or risk factors like recent infection/travel.
Frequently Asked Questions (FAQs)
What is the main symptom of pleurisy?
Sharp chest pain worsening with breathing, coughing, or movement.
How long does pleurisy last?
Viral cases resolve in 1-2 weeks with treatment; others depend on cause.
Can pleurisy go away on its own?
Yes, mild viral pleurisy often self-resolves, but medical evaluation is essential.
Is pleurisy contagious?
No, but underlying infections like pneumonia may be.
Can pleurisy cause shortness of breath?
Yes, from pain, effusion, or lung compression.
References
- Pleurisy | Definition, Causes, & Treatment — Britannica. 2023. https://www.britannica.com/science/pleurisy
- Pleurisy | Research Starters — EBSCO. Accessed 2026. https://www.ebsco.com/research-starters/consumer-health/pleurisy
- Pleurisy: What It Is, Symptoms, Causes & Treatment — Healthgrades. 2024. https://resources.healthgrades.com/right-care/lungs-breathing-and-respiration/pleurisy
- Pleurisy – Symptoms and causes — Mayo Clinic. 2024-10-15. https://www.mayoclinic.org/diseases-conditions/pleurisy/symptoms-causes/syc-20351863
- Pleurisy — Healthdirect (Australian Government). 2025. https://www.healthdirect.gov.au/pleurisy
- Pleural Effusion – StatPearls — NCBI Bookshelf / NIH. 2023-10-15. https://www.ncbi.nlm.nih.gov/books/NBK448189/
Read full bio of medha deb











