Polymorphic Eruption Of Pregnancy: Symptoms And Treatment
Understanding the itchy rash of late pregnancy: causes, symptoms, diagnosis, and safe treatments for relief.
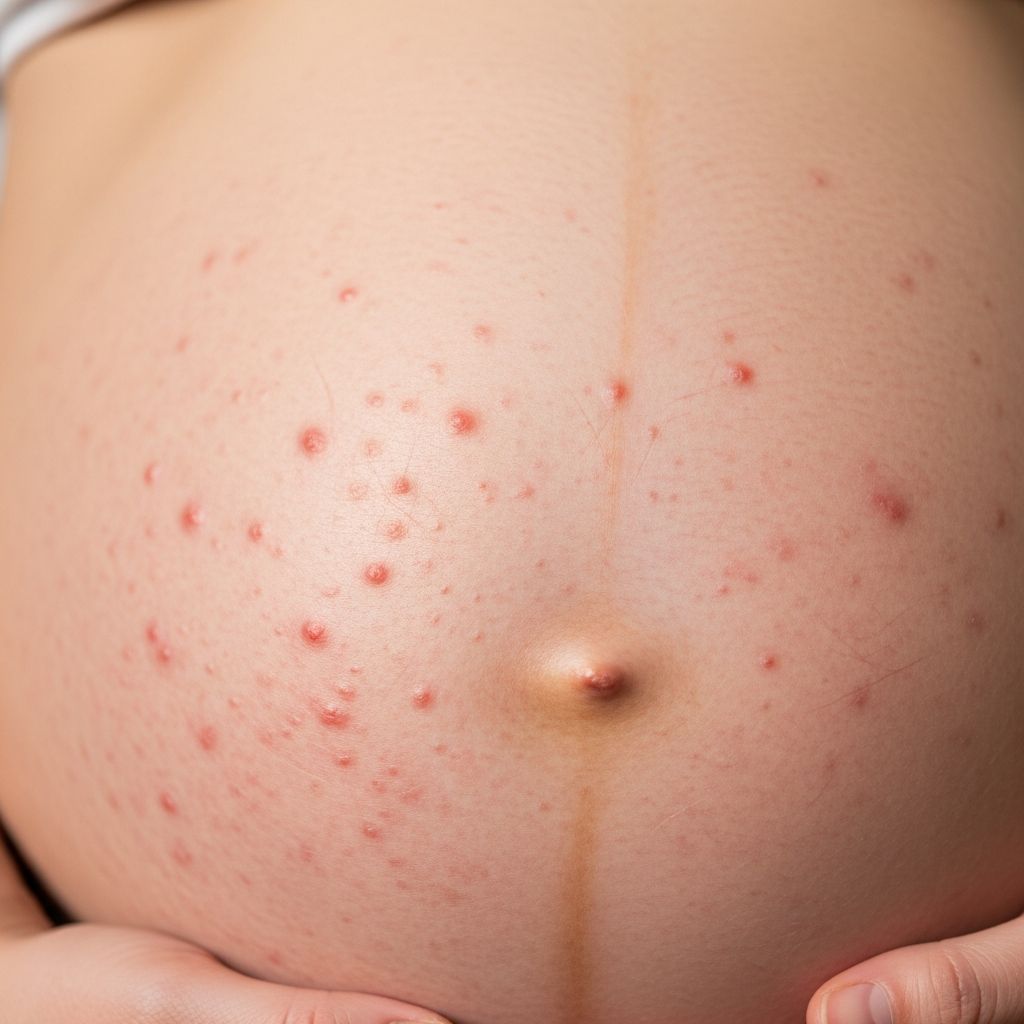
Polymorphic Eruption of Pregnancy
Polymorphic eruption of pregnancy (PEP), also known as pruritic urticarial papules and plaques of pregnancy (PUPPP), is the most common dermatosis associated with pregnancy, affecting approximately 1 in 160 pregnancies. It manifests as an intensely pruritic (itchy) rash typically emerging in the third trimester, starting within abdominal stretch marks (striae) and spreading to other areas.
What is polymorphic eruption of pregnancy?
Polymorphic eruption of pregnancy is a benign, self-limiting inflammatory skin disorder unique to pregnancy. Characterized by polymorphic (varied) lesions including papules, plaques, and occasionally vesicles, it causes significant discomfort due to intense itching that often disrupts sleep, though excoriations (scratch marks) are uncommon. The condition spares the face, palms, and soles, and is more prevalent in primigravidae (first pregnancies) and multiple gestations like twins.
Who gets polymorphic eruption of pregnancy?
PEP primarily affects women in their first pregnancy, with a higher incidence in those carrying multiples due to greater abdominal distension. It occurs in about 1 in 160 pregnancies overall, usually in the last few weeks of the third trimester, though 15% of cases start immediately postpartum. Risk factors include rapid abdominal skin stretching, which is more pronounced in primiparous women and twin pregnancies.
- Primigravidae (first-time mothers): Higher risk due to less skin elasticity from prior pregnancies.
- Multiple pregnancies: Increased abdominal distension leads to connective tissue damage.
- Third trimester: 85% onset before delivery, 15% postpartum.
What causes polymorphic eruption of pregnancy?
The exact cause remains unknown, but the leading theory attributes it to mechanical stretching of abdominal skin, damaging connective tissue within striae and exposing antigens that trigger an immune response. This is supported by the rash’s initial appearance in striae distensae. Alternative hypotheses include:
- Increased fetal cell trafficking (chimerism) in maternal circulation, targeting damaged collagen-rich skin.
- Hormonal influences, such as elevated progesterone levels and increased progesterone receptor immunoreactivity in lesional skin.
- Placental factors promoting fibroblast proliferation in maternal skin.
No infectious, allergic, or autoimmune etiology has been confirmed, and laboratory tests are typically normal with negative direct immunofluorescence.
What are the clinical features of polymorphic eruption of pregnancy?
The rash begins with small, pink or erythematous papules within abdominal striae, often surrounded by a pale halo. These coalesce into urticarial (hive-like) plaques, sometimes with central vesicles. Intense pruritus is hallmark, spreading to thighs, buttocks, and proximal extremities, but rarely involving the breasts, face, palms, or soles. Patients may develop hundreds of lesions, with onset disrupting sleep.
| Feature | Description |
|---|---|
| Onset | Third trimester (last 2-3 weeks) or immediate postpartum |
| Initial site | Abdomen, within striae around umbilicus (spares periumbilical area) |
| Spread | Thighs, buttocks, arms; spares face, palms, soles |
| Lesion types | Papules, plaques, vesicles; erythematous with pale halos |
| Symptoms | Severe pruritus, sleep disturbance; minimal excoriation |
How is the diagnosis made?
Diagnosis is clinical, based on characteristic history (late pregnancy onset in striae) and morphology. No specific laboratory tests exist; biopsies show nonspecific findings like dermal edema, mild spongiosis, and perivascular lymphohistiocytic infiltrate. Differentiation from mimics requires consideration of distribution and timing.
Differential diagnosis
- Pemphigoid gestationis: Starts periumbilically with urticarial plaques progressing to blisters; positive immunofluorescence; earlier onset.
- Atopic eruption of pregnancy: Flexural involvement, personal/family atopy history; eczematous.
- Prurigo of pregnancy:
- Drug eruption/urticaria/viral exanthem: Systemic symptoms or different distribution.
Skin biopsy may be performed if atypical; direct immunofluorescence rules out autoimmune bullous diseases.
What is the basic pathology?
Histopathology is nonspecific. Early lesions show upper dermal edema, focal spongiosis, and perivascular lymphocytic infiltrate resembling arthropod bites. Older lesions display eczematous changes. No acanthosis, parakeratosis, or viral inclusions.
Treatment of polymorphic eruption of pregnancy
Treatment is symptomatic, focusing on itch relief, as PEP is self-limiting. Emollients and bath oils are first-line to hydrate skin and reduce irritation. Topical corticosteroids (mild to moderate potency, e.g., hydrocortisone or betamethasone) applied to affected areas provide rapid relief.
- Mild cases: Emollients, soap substitutes, mild topical steroids.
- Moderate-severe: Medium-potency steroids; oral antihistamines (e.g., chlorpheniramine, safe in pregnancy).
- Refractory: Short-course oral prednisolone (0.5-1 mg/kg/day), tapering post-delivery.
All treatments prioritize safety for mother and fetus. Avoid high-potency steroids long-term.
Complications of polymorphic eruption of pregnancy
PEP poses no maternal or fetal risks; it does not associate with preterm birth, low birth weight, or other adverse outcomes. Rarely, newborns may exhibit a mild, transient rash. Persistent postpartum symptoms may relate to retained placental tissue.
Prevention of polymorphic eruption of pregnancy
No proven prevention exists. Early emollient use and monitoring high-risk women (primigravidae, multiples) may mitigate severity, though evidence is anecdotal.
Prognosis and outcome for polymorphic eruption of pregnancy
The rash resolves spontaneously within 15 days to 4-6 weeks postpartum, rarely persisting longer if placental remnants are present. Recurrence in subsequent pregnancies is uncommon (<10%), possibly due to immune tolerance.
Frequently Asked Questions (FAQs)
Is polymorphic eruption of pregnancy harmful to the baby?
No, PEP is benign and does not affect fetal outcomes. Rarely, a mild rash may appear on the newborn but resolves quickly.
Can polymorphic eruption of pregnancy recur in future pregnancies?
Recurrence is rare, occurring in fewer than 10% of cases, more likely in first pregnancies.
When does the rash usually start?
Typically in the last 2-3 weeks of pregnancy, starting in abdominal striae.
Is treatment safe during pregnancy?
Yes, emollients, mild-moderate topical steroids, and select oral antihistamines are safe for mother and baby.
Does polymorphic eruption of pregnancy require delivery induction?
No, it is not an indication for early delivery; it resolves post-delivery.
References
- Polymorphic eruption of pregnancy: Review of literature — PubMed/NCBI. 2016-12-07. https://pubmed.ncbi.nlm.nih.gov/27960565/
- Polymorphic Eruption of Pregnancy — Merck Manuals Professional Edition. 2023. https://www.merckmanuals.com/professional/gynecology-and-obstetrics/antenatal-complications/polymorphic-eruption-of-pregnancy
- Polymorphic eruption of pregnancy — DermNet NZ. 2023. https://dermnetnz.org/topics/polymorphic-eruption-of-pregnancy
- Pruritic Urticarial Papules and Plaques of Pregnancy — NCBI Bookshelf/StatPearls. 2023-08-08. https://www.ncbi.nlm.nih.gov/books/NBK539700/
- Polymorphic eruption of pregnancy (PEP) — European Academy of Dermatology and Venereology (EADV). 2023-10. https://eadv.org/wp-content/uploads/2023/10/PREGNANCY-Polymorphic-eruption-of-pregnancy-PEP.pdf
Read full bio of Sneha Tete