Postnasal Drip: Causes, Symptoms, and Treatment Options
Complete guide to understanding postnasal drip, its causes, symptoms, and effective treatment strategies.
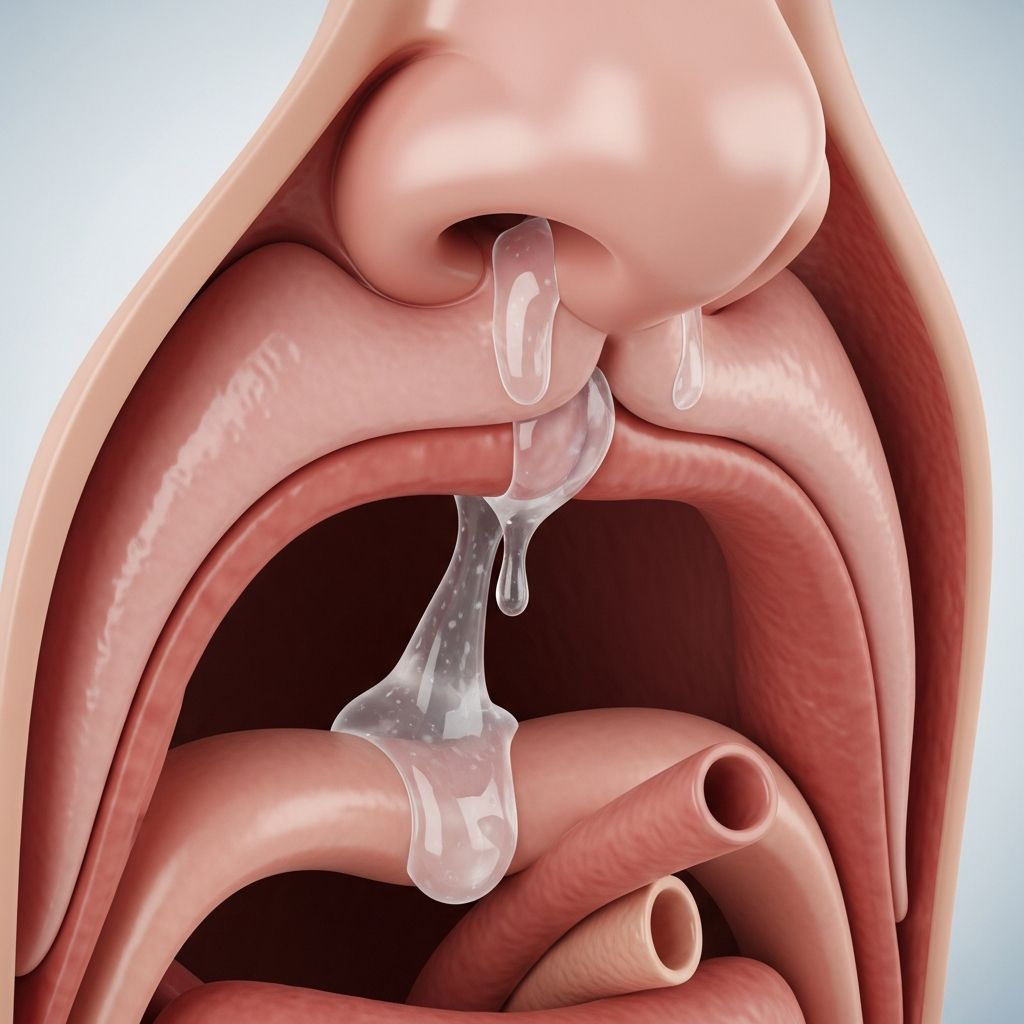
What Is Postnasal Drip?
Postnasal drip is a condition in which mucus from the nasal cavity and sinuses drains backward into the throat. This drainage occurs when normal nasal clearance mechanisms are obstructed or when the body produces excess mucus. While mucus production is a normal and protective function, excessive amounts or abnormally thick secretions can cause discomfort and various symptoms.
The sensation of postnasal drip—feeling nasal secretions passing into the pharynx—is caused either by obstruction of normal drainage in the nasal cavity or increased secretion from the paranasal sinuses. Understanding this distinction is important because it helps guide treatment decisions.
Common Causes of Postnasal Drip
Postnasal drip can develop from numerous underlying conditions. Identifying the cause is essential for effective treatment, as management strategies differ depending on the underlying issue.
Rhinitis and Nasal Inflammation
One of the most common causes of postnasal drip is rhinitis, which involves swelling of the inner lining of the nose. Rhinitis can be allergic or non-allergic in nature. Allergic rhinitis occurs when the nasal lining becomes inflamed in response to allergen exposure, while non-allergic rhinitis—also called vasomotor rhinitis—occurs when the nose becomes overly sensitive to environmental triggers such as pollution, temperature changes, or humidity variations.
Sinus Infections
Sinusitis, or inflammation of the sinuses, represents another significant cause of postnasal drip. Sinus infections can be acute (short-term) or chronic (long-term) and typically develop following viral infections or due to bacterial colonization. Patients with sinusitis often experience thick, discolored nasal secretions that appear yellow or green, along with facial pressure, nasal congestion, and reduced sense of smell.
Allergic Reactions
Allergies are among the most prevalent causes of postnasal drip. Seasonal allergies, environmental allergens, and food sensitivities—particularly dairy products—can trigger excessive mucus production and nasal congestion. Allergic reactions cause the nasal lining to swell and produce additional mucus as a protective response.
Additional Contributing Factors
Other causes of postnasal drip include:
- Gastroesophageal reflux disease (GERD), where stomach acid reflux causes swelling and mucus production in the nose and throat
- Bacterial infections that lead to sinus inflammation and altered mucus composition
- Medications that thicken mucus secretions
- Age-related changes in mucus production and nasal function
- Anatomical factors such as nasal polyps or structural abnormalities
Recognizing Postnasal Drip Symptoms
Postnasal drip produces a range of symptoms that vary in severity and type depending on the underlying cause and individual characteristics. Common manifestations include:
- Feeling of mucus dripping down the back of the throat
- Frequent swallowing and throat clearing
- Raspy or gurgling speech
- Sore, irritated, or inflamed throat
- Sensation of a lump in the throat
- Persistent cough, particularly at night
- Nasal congestion and rhinorrhea (runny nose)
- Nasal stiffness or uncomfortable nasal sensations
Mucus Characteristics
The appearance and consistency of nasal secretions provide important clues about the underlying cause. Thin, clear secretions typically indicate viral infections, colds, or allergies. When secretions become thick and discolored (appearing yellow or green), this suggests a developing or active bacterial sinus infection. The viscosity of postnasal drip correlates with specific accompanying symptoms: patients with serous (thin) drainage tend to experience more rhinorrhea, while those with mucoid (thick) drainage report greater throat discomfort.
Associated Symptoms
Postnasal drip frequently occurs alongside other nasal and respiratory symptoms. Research indicates that approximately one-third of patients with postnasal drip experience cough, a prevalence higher than observed in the general population. The relationship between postnasal drip and cough involves sensory hypersensitivity rather than direct mechanical irritation from mucus. Additional accompanying symptoms may include nasal stiffness, itching sensations, and throat discomfort, with some patients experiencing multiple concurrent symptoms.
Diagnosis of Postnasal Drip
Accurate diagnosis of postnasal drip begins with a detailed clinical history and physical examination. However, identifying the underlying cause can be challenging, as not all patients present clearly identifiable triggers or conditions.
Evaluation Methods
Healthcare providers use several diagnostic approaches:
- Detailed symptom history: Describing when symptoms occur, duration, daily patterns, and associated complaints helps narrow potential causes
- Nasal endoscopy: Using a small camera to visualize the nasal cavity and throat
- Allergy testing: When allergies are suspected as the underlying cause
- Imaging studies: Such as CT scans or radiography, particularly when sinusitis or lung involvement is suspected
- Specialist referral: An ear, nose, and throat doctor (ENT or otolaryngologist) can perform more detailed examinations and tests
Treatment Options for Postnasal Drip
Treatment for postnasal drip depends entirely on the identified underlying cause. A multimodal approach combining lifestyle modifications, medications, and sometimes procedural interventions often yields the best results.
Lifestyle Modifications and Self-Care
Initial management typically includes empirical treatments such as lifestyle correction and saline washing. These approaches include:
- Saline nasal irrigation using salt water solutions to flush nasal passages
- Increasing hydration to help thin secretions
- Using humidifiers to maintain adequate air moisture
- Avoiding known triggers such as allergens, irritants, or problematic foods
- Sleeping with the head elevated to reduce drainage into the throat during sleep
Pharmacological Treatment
Antihistamines and Decongestants: First-generation antihistamines combined with decongestants (such as pseudoephedrine) represent an effective treatment approach, with approximately 71.6% of patients experiencing positive symptom response. However, older sedating antihistamines may thicken secretions, whereas newer non-drowsy antihistamines do not produce this effect.
Nasal Sprays: Several types of medicated nasal sprays can provide relief:
- Steroid nasal sprays reduce inflammation and mucus production
- Antihistamine sprays block allergic responses
- Anticholinergic sprays decrease mucus secretion
- Cromolyn sprays prevent allergic reactions
Allergy Management: For patients with allergic rhinitis, treatment options include avoiding identified allergens, taking oral or inhaled medications, receiving allergy immunotherapy (desensitization through allergy shots), or using oral steroids in cases of severe allergic inflammation.
Procedural Interventions
For patients who do not respond adequately to medical management, several office-based or surgical procedures may be considered:
- Inferior turbinate reduction: Shrinks the inner lining of the nasal passages to improve drainage and reduce mucus contact with tissues
- Posterior nasal nerve ablation: Removes or disables nerves that stimulate excess mucus production
- Sinus surgery: May be necessary when sinusitis is the underlying cause and medical management has failed
Managing Symptom Recurrence
Clinical evidence indicates that approximately 25.9% of postnasal drip patients experience symptom recurrence after initial treatment. Patients with certain clinical characteristics—particularly those with nasal stiffness or persistent baseline symptoms—show significantly higher recurrence rates. Nasal stiffness is typically associated with anatomical factors that may cause underlying postnasal drip, explaining why these patients experience rapid symptom return upon medication discontinuation.
Understanding Idiopathic Postnasal Drip
In some cases, despite thorough evaluation, the underlying cause of postnasal drip cannot be clearly identified. This condition, termed chronic idiopathic postnasal drip, affects patients who experience persistent symptoms without clear diagnostic findings. These patients often undergo multiple clinical visits and receive various treatments without obtaining a definitive diagnosis. Recognition of idiopathic postnasal drip as a distinct clinical entity helps guide appropriate management and prevents unnecessary repeated testing and interventions.
Frequently Asked Questions
Q: Can postnasal drip cause serious complications?
A: While postnasal drip itself is usually not serious, the sensation of thick mucus in the throat can cause sore throat, sleep disruption from nighttime coughing, and throat clearing discomfort. Underlying conditions like sinusitis or GERD may require treatment to prevent complications.
Q: How long does postnasal drip typically last?
A: Duration depends on the underlying cause. Postnasal drip from viral infections may resolve in one to two weeks, while allergic or idiopathic postnasal drip may persist chronically without treatment.
Q: Are there natural remedies for postnasal drip?
A: Yes, saline nasal irrigation, staying hydrated, using humidifiers, and avoiding known triggers are effective natural approaches. These work best when combined with medical treatment for the underlying cause.
Q: When should I see a doctor for postnasal drip?
A: Consult a healthcare provider if postnasal drip persists for more than two weeks, significantly impacts quality of life, or is accompanied by facial pain, fever, or discolored nasal discharge suggesting infection.
Q: Can food allergies cause postnasal drip?
A: Yes, food sensitivities—particularly to dairy products—can trigger nasal mucus production and postnasal drip symptoms in some individuals.
References
- Clinical Aspects of Chronic Idiopathic Postnasal Drip: An Entity Not Widely Recognized — National Center for Biotechnology Information (NCBI), U.S. National Library of Medicine. 2024. https://pmc.ncbi.nlm.nih.gov/articles/PMC11215627/
- Post-Nasal Drip — American Academy of Otolaryngology–Head and Neck Surgery (ENT Health). 2021. https://www.enthealth.org/wp-content/uploads/2021/09/Post-nasal_Drip_2021.pdf
- Postnasal Drip — Chiu J, Rowan NR. JAMA Otolaryngology–Head & Neck Surgery. 2025;151(4):417. doi:10.1001/jamaoto.2024.5136. https://jamanetwork.com/journals/jamaotolaryngology/fullarticle/2830355
Read full bio of Sneha Tete











