Primary Cutaneous Diffuse Large B-Cell Lymphoma Pathology
Detailed pathology of primary cutaneous diffuse large B-cell lymphoma, leg type: histology, immunohistochemistry, and prognostic insights for clinicians.
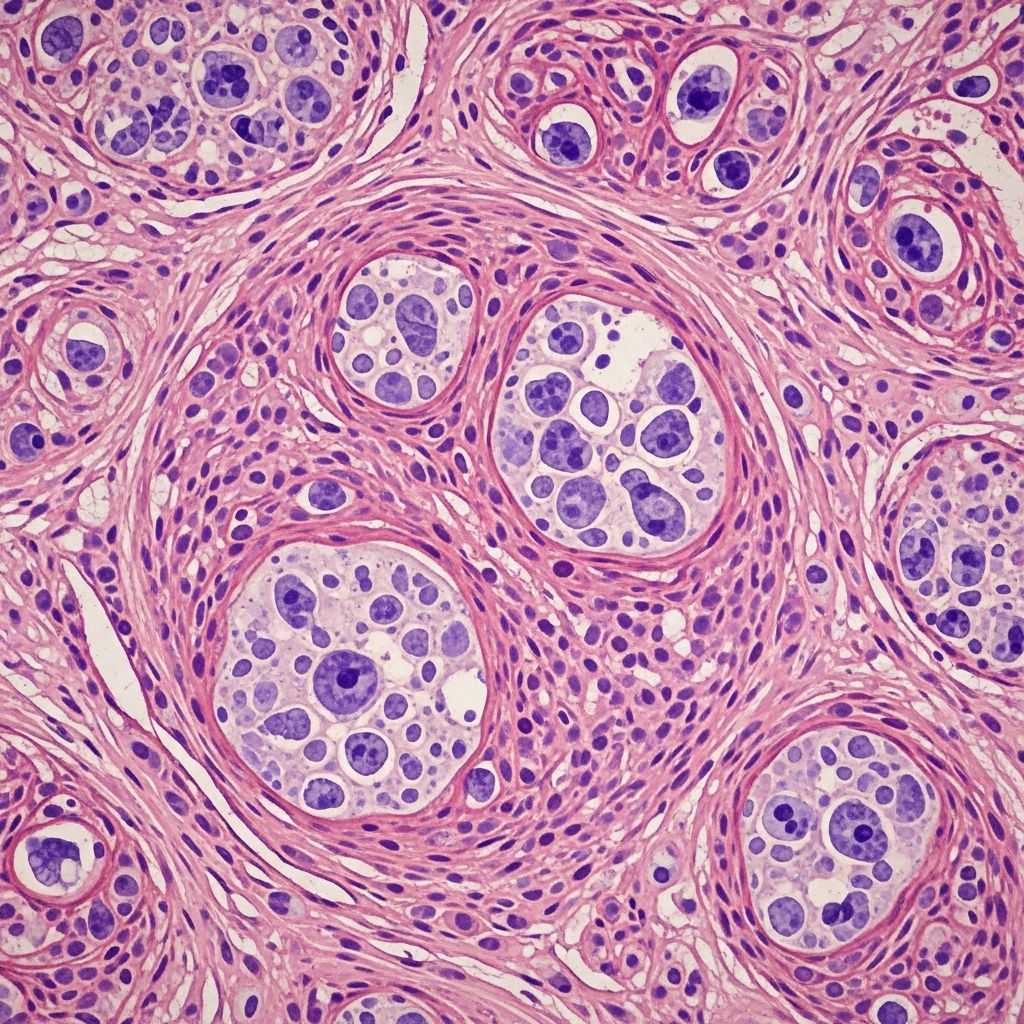
Primary cutaneous diffuse large B-cell lymphoma (PCLBCL) represents an aggressive subtype of cutaneous B-cell lymphoma characterized by large neoplastic B-cells. It is subcategorized into leg type and other variants, with the leg type carrying a particularly poor prognosis due to frequent relapses and extracutaneous spread.
What is primary cutaneous diffuse large B-cell lymphoma?
Primary cutaneous diffuse large B-cell lymphoma encompasses rare, aggressive lymphomas originating in the skin without extracutaneous involvement at diagnosis. The World Health Organization-European Organization for Research and Treatment of Cancer (WHO-EORTC) classification distinguishes primary cutaneous diffuse large B-cell lymphoma,
leg type
(PCLBCL-LT), from other forms and from systemic counterparts. PCLBCL-LT typically affects elderly patients, presenting as nodules or tumors predominantly on the lower legs, with a 5-year disease-specific survival rate of approximately 41%.The ‘leg type’ designation reflects its predilection for the legs (72% of cases), advanced age at onset (mean 76 years), high Bcl-2 expression (85%), and adverse outcomes, especially with multiple lesions. In contrast, ‘other’ variants lack these leg-centric features and may have better prognoses.
Clinical features
PCLBCL-LT manifests as rapidly growing, reddish-brown nodules or tumors, often multiple, on the lower legs of elderly individuals (mean age 76 years). Systemic B symptoms, elevated serum lactate dehydrogenase (LDH), and extracutaneous dissemination occur in advanced cases. Prognostic factors include leg location, multiple skin lesions, and older age, with multivariate analysis confirming leg involvement and lesion multiplicity as predictors of mortality.
- Age: Predominantly elderly (>70 years)
- Sex: Slight female predominance
- Site: Lower legs (72%); rarely arms or trunk
- Lesions: Single or multiple violaceous nodules/tumors
- Prognosis: 5-year survival 41%; worse with multiple leg lesions
Histology of primary cutaneous diffuse large B-cell lymphoma
Histologically, PCLBCL-LT shows a
dense, diffuse infiltrate
of atypical large B-cells extending from the dermis into the subcutaneous tissue (panniculitis-like). Scanning magnification reveals a bottom-heavy pattern with superficial and deep dermal involvement (figure 1 equivalent: dense cellular infiltrate).Medium power highlights sheets of large centroblast-like and immunoblast-like cells with non-cleaved nuclei, open chromatin, and prominent nucleoli (figures 2-5 equivalents).
Crush artefact
is frequent, manifesting as smudged nuclear contours—a non-specific but suggestive feature of high-grade lymphoid malignancy.High power confirms pleomorphic large lymphocytes: centroblasts (oval nuclei, vesicular chromatin, 2-3 nucleoli) and immunoblasts (eccentric nuclei, single large nucleolus). Mitotic figures abound, reflecting high proliferation. Necrosis or ulceration may be present in advanced lesions.
Key histological patterns
- Dense dermal/subcutaneous infiltrate: Nodular or diffuse
- Cell morphology: Centroblast/immunoblast predominance
- Grading: High-grade (large cell >80%)
- Artefacts: Crush, tingible body macrophages
Immunohistochemistry
Immunophenotyping is crucial for diagnosis. Neoplastic cells express
CD20+
(pan-B marker),BCL2+
(diffuse, 85-100%), andMUM1/IRF4+
(post-germinal center origin). BCL6 is variably positive, whileCD10-
distinguishes it from follicle center lymphoma.Proliferation index (Ki-67) exceeds 70-90%, indicating aggressiveness. CD79a, PAX5, and MUM1 co-expression support activated B-cell phenotype. Negativity for CD5, CD23, cyclin D1, and CD138 aids differential diagnosis.
| Marker | Expression in PCLBCL-LT | Differential Value |
|---|---|---|
| CD20 | Positive (diffuse) | Confirms B-cell lineage |
| BCL2 | Positive (85-100%) | Poor prognosis; vs. follicle center (negative) |
| MUM1 | Positive (diffuse) | Activated B-cell type |
| BCL6 | Variable | Partial germinal center affinity |
| CD10 | Negative | Excludes follicle center lymphoma |
| Ki-67 | >70% | High proliferation |
Cytogenetics
Genetic aberrations include
MYD88 mutations
(common in activated B-cell lymphomas), losses ofCDKN2A/B
, and amplifications of18q21 (BCL2 locus)
. Unlike systemic DLBCL, t(14;18) IGH-BCL2 is rare. Clonal immunoglobulin heavy chain (IGH) rearrangements confirm monoclonality. These changes drive aggressive behavior and extracutaneous spread.Electron microscopy
Rarely utilized, electron microscopy reveals large lymphoid cells with abundant cytoplasm, prominent nucleoli, and rough endoplasmic reticulum, consistent with immunoblast differentiation. This modality is obsolete in routine practice due to IHC superiority.
Diagnosis
Diagnosis integrates clinicopathology: elderly patient with leg nodules, dense large B-cell infiltrate (centroblast/immunoblast), CD20+/BCL2+/MUM1+/CD10-, and high Ki-67. Exclude systemic lymphoma via staging (PET-CT, bone marrow). Molecular IGH rearrangement supports clonality.
Differential diagnosis
PCLBCL-LT overlaps with other cutaneous/systemic lymphomas. Key discriminators:
- Primary cutaneous follicle center lymphoma (PCFCL): Head/neck, CD10+/BCL6+, BCL2-, better prognosis
- Systemic DLBCL: Extracutaneous at onset, similar IHC but staging differentiates
- Plasmablastic lymphoma: CD138+, CD20 variable, HHV8+/-
- T-cell rich B-cell lymphoma: >90% T-cells background
- EBV+ DLBCL elderly: EBV+, systemic symptoms
- Marginal zone lymphoma: Small cells, indolent
Leg location, BCL2/MUM1 co-expression, and multiple lesions favor PCLBCL-LT.
Management
Treatment involves
R-CHOP
(rituximab, cyclophosphamide, doxorubicin, vincristine, prednisone), yielding improved short-term survival despite advanced age. Radiation for localized disease; multi-agent chemoimmunotherapy for advanced. Prognosis poor: 41% 5-year survival, worse with leg/multiple lesions.Frequently Asked Questions (FAQs)
Q: What is the hallmark location for PCLBCL, leg type?
A: Predominantly lower legs (72% of cases), in elderly patients.
Q: Which IHC markers define PCLBCL-LT?
A: CD20+, BCL2+, MUM1+, CD10-; high Ki-67.
Q: What is the 5-year survival rate?
A: Approximately 41%, poorer with multiple leg lesions.
Q: How does it differ from follicle center lymphoma?
A: Leg type has BCL2+/MUM1+, CD10-; PCFCL is CD10+/BCL2-, head/neck.
Q: Is crush artefact diagnostic?
A: Suggestive but non-specific; common in high-grade lymphomas.
References
- Primary cutaneous diffuse large B-cell lymphoma, leg type: clinicopathologic features and prognostic analysis in 60 cases — Arch Dermatol (Grange et al.). 2007-09-01. https://pubmed.ncbi.nlm.nih.gov/17875875/
- Primary cutaneous diffuse large B cell lymphoma pathology — DermNet NZ. Accessed 2026. https://dermnetnz.org/topics/primary-cutaneous-diffuse-large-b-cell-lymphoma-pathology
- Primary cutaneous diffuse large B-cell lymphoma, leg type — Arch Pathol Lab Med (Wilcox et al.). 2012-08-01. https://pubmed.ncbi.nlm.nih.gov/22849734/
Read full bio of medha deb












