Prostate Biopsy: 5 Key Facts And What To Expect
Complete guide to prostate biopsy procedures, types, risks, and what to expect.
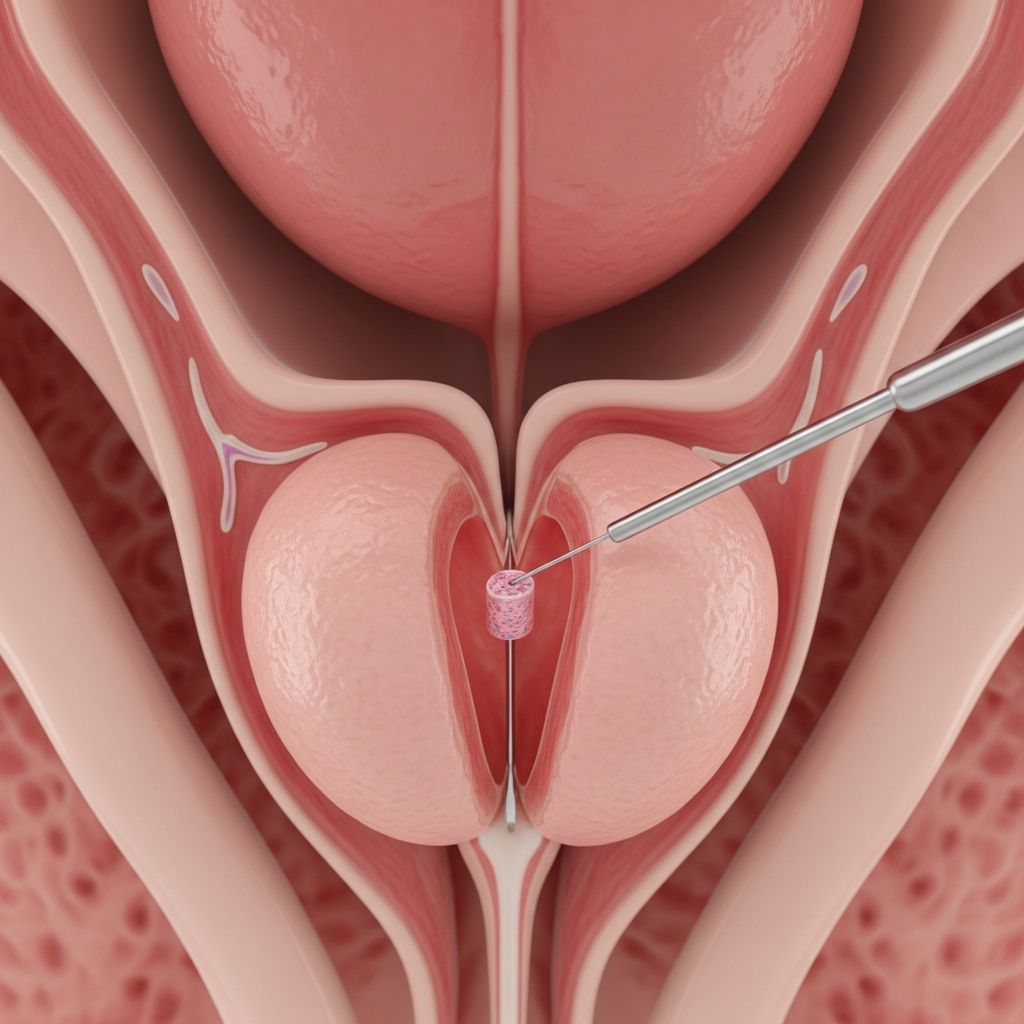
A prostate biopsy is a medical procedure used to diagnose or rule out prostate cancer. It involves taking small tissue samples from the prostate gland for examination under a microscope. This procedure is typically recommended when men have an elevated prostate-specific antigen (PSA) level or an abnormal digital rectal examination. Understanding what to expect during a prostate biopsy can help alleviate anxiety and prepare you for the procedure.
What Is a Prostate Biopsy?
A prostate biopsy is a diagnostic procedure that allows physicians to obtain tissue samples from the prostate gland to evaluate for the presence of cancer cells. The prostate is a small, walnut-shaped gland located beneath the bladder in men that produces fluid that makes up part of semen. When cancer risk is suspected, a biopsy provides definitive information about whether cancer is present and its severity.
The procedure is performed under ultrasound guidance, which allows the physician to visualize the prostate and precisely direct the biopsy needle. Typically, 12 or more samples of tissue are collected during the procedure to ensure thorough evaluation of the gland.
Why Your Doctor May Recommend a Prostate Biopsy
Your urologist may recommend a prostate biopsy for several reasons:
- Elevated PSA levels detected in blood tests
- Abnormal findings during a digital rectal examination
- Suspicious areas identified on imaging studies such as ultrasound or MRI
- Family history of prostate cancer
- Symptoms suggestive of prostate cancer
The decision to undergo a biopsy is made collaboratively between you and your physician after discussing your individual risk factors and test results.
Types of Prostate Biopsy Procedures
There are two primary approaches to performing a prostate biopsy, each with distinct advantages and considerations.
Transrectal Biopsy
The transrectal biopsy has been the most common method for performing prostate biopsies for the past 30 years. In this approach, an ultrasound probe is inserted into the rectum to visualize the prostate gland. A biopsy needle guide is attached to the ultrasound probe, and the needle is passed through the rectal wall into the prostate tissue to collect samples. This procedure can be performed safely in an office setting with only local numbing medication.
While this technique is well-established and relatively quick, it carries certain risks. Passing needles through the rectal wall can transfer rectal bacteria directly into the prostate, potentially causing infection. These infections can range from simple urinary tract infections to serious bloodborne infections, including sepsis. To minimize infection risk, urologists typically prescribe antibiotics to men undergoing transrectal biopsy. However, even with antibiotic use, infections occur in approximately 5% of men undergoing this procedure. Additionally, antibiotic administration carries its own risks, including allergic reactions, gastrointestinal upset, and contribution to bacterial resistance.
Transperineal Biopsy
The transperineal biopsy represents a safer alternative approach that has gained increased adoption in recent years. Instead of passing needles through the rectal wall, this technique involves accessing the prostate through the perineum—the area of skin located between the scrotum and rectum. When needles pass through skin rather than the rectal wall, the risk of infectious complications is substantially minimized, so much so that antibiotics are not required.
Historically, the transperineal approach was limited to operating room settings under general or spinal anesthesia because multiple needle passes through the skin could cause significant patient discomfort. However, innovative techniques developed by urologists at Johns Hopkins now allow transperineal biopsies to be performed in office settings using only local anesthesia. The key advancement involves using a novel needle guide that reduces the number of needle passes needed to obtain required tissue samples while maintaining patient comfort.
The transperineal approach also provides access to areas of the prostate that may not be adequately reached through the traditional transrectal method, potentially improving diagnostic accuracy.
Preparation for Your Prostate Biopsy
Proper preparation is essential for ensuring the safety and success of your procedure. Your physician will provide specific instructions, but general preparation typically includes:
- Informing your doctor of all medications you take, particularly blood thinners
- Temporarily discontinuing certain medications as advised by your physician
- Arranging transportation to and from the procedure since sedation may be used
- Fasting for a specified period if sedation will be administered
- Completing any required pre-procedure antibiotics as prescribed
- Discussing any allergies with your medical team
Your physician may also recommend a cleansing enema before the procedure if undergoing a transrectal biopsy.
What to Expect During the Procedure
Understanding what happens during a prostate biopsy can help reduce anxiety. The procedure typically follows these steps:
Positioning: You will be positioned on your side or in a dorsal lithotomy position (lying on your back with knees bent and spread) depending on the biopsy approach.
Anesthesia: Local anesthesia is applied to numb the area. For transrectal biopsies, numbing medicine is injected into the area around the prostate. For transperineal biopsies performed in the office, local anesthesia numbs the perineal skin.
Ultrasound Guidance: An ultrasound probe is inserted to visualize the prostate gland. This imaging allows your physician to precisely direct the biopsy needle.
Tissue Sampling: Using the ultrasound guidance, the biopsy needle is passed into the prostate to collect tissue samples. You may hear a clicking sound and feel slight pressure with each sample collection.
Sample Collection: Typically, 12 or more tissue samples are collected from different areas of the prostate to ensure thorough evaluation.
Completion: Once adequate samples are collected, the instruments are removed and the procedure is complete.
The entire procedure usually takes 15 to 30 minutes.
Recovery and Aftercare
Recovery from a prostate biopsy is generally straightforward. Most men can return to normal activities immediately, though some restrictions may apply during the first few days:
- Rest for the remainder of the day following the procedure
- Avoid strenuous activities and heavy lifting for several days
- Stay well-hydrated by drinking plenty of water
- Expect mild discomfort, which can be managed with over-the-counter pain relievers
- Avoid sexual activity for a few days
You may notice slight bleeding or spotting in your urine, stool, or semen for several days after the procedure. This is normal and typically resolves within a week.
Understanding Your Results
Pathologists analyze the tissue samples under a microscope and assign a Gleason score if cancer is identified. The Gleason score ranges from 2 to 10 and indicates how quickly the cancer may grow and spread. Your physician will discuss the results with you and recommend appropriate next steps based on your specific findings.
Results are typically available within one to two weeks of the procedure. Your physician will schedule a follow-up appointment to discuss findings and treatment options if cancer is detected.
Risks and Complications
While prostate biopsy is generally a safe procedure, potential complications include:
- Infection of the urinary tract or prostate
- Prolonged or excessive bleeding
- Difficulty urinating immediately after the procedure
- Blood in urine, stool, or semen
- Allergic reactions to anesthesia or medications
- Mild discomfort or pain
The transperineal approach significantly reduces infection risk compared to the transrectal method, particularly because it eliminates the need for prophylactic antibiotics.
Comparing Biopsy Approaches
| Feature | Transrectal Biopsy | Transperineal Biopsy |
|---|---|---|
| Infection Risk | ~5% with antibiotics | Minimal without antibiotics |
| Antibiotic Use | Required | Not required |
| Setting | Office or operating room | Office with local anesthesia (modern technique) |
| Patient Discomfort | Minimal to moderate | Minimal with modern guided technique |
| Prostate Access | Standard areas | All areas including difficult-to-reach regions |
Advanced Diagnostic Technologies
Modern prostate cancer management often combines biopsy results with additional diagnostic information. Genomic testing on biopsy samples can provide information about cancer behavior and aggressiveness. Advanced imaging techniques such as PSMA-PET scans can help identify metastatic disease and guide treatment decisions. These complementary approaches help physicians develop personalized treatment strategies that balance cancer control with quality of life considerations.
Frequently Asked Questions
Is a prostate biopsy painful?
A prostate biopsy causes minimal pain when performed with proper anesthesia. You may feel pressure or mild discomfort, but the procedure should not be severely painful. Local anesthesia numbs the area adequately for patient comfort during the procedure.
How long does a prostate biopsy take?
Most prostate biopsies are completed within 15 to 30 minutes, depending on the approach used and the number of samples collected.
Can I drive after my biopsy?
If only local anesthesia is used, you may be able to drive if you feel comfortable. However, if sedation is administered, you will need someone to drive you home and should not operate a vehicle for the remainder of the day.
What if my biopsy results are negative?
A negative biopsy means no cancer was found in the samples obtained. However, it does not completely rule out cancer, as the samples collected represent only a portion of the prostate. Your physician may recommend continued monitoring with PSA tests and periodic follow-up examinations.
How soon can I return to sexual activity?
Most physicians recommend waiting a few days before resuming sexual activity to allow proper healing and minimize infection risk. Ask your physician for specific recommendations based on your individual situation.
What should I do if I develop signs of infection after my biopsy?
Contact your physician immediately if you develop fever, severe pain, inability to urinate, or excessive bleeding. These may indicate infection or other complications requiring medical attention.
Is the transperineal biopsy available everywhere?
The modern office-based transperineal biopsy technique is an innovative approach pioneered at specialized centers like Johns Hopkins and is becoming more widely available as urologists adopt this safer methodology.
Next Steps and Follow-Up Care
After your biopsy, your physician will schedule a follow-up appointment to discuss results and next steps. If cancer is detected, you may be referred to a multidisciplinary team of specialists including radiation oncologists, medical oncologists, and other healthcare providers to develop a personalized treatment plan. If no cancer is found, your physician will discuss ongoing monitoring strategies appropriate for your individual risk profile.
Prostate biopsy remains an essential diagnostic tool in evaluating suspected prostate cancer. Whether performed using the traditional transrectal approach or the innovative transperineal technique, this procedure provides crucial information to guide treatment decisions and ultimately improve patient outcomes.
References
- Transperineal Prostate Biopsy Explained — Johns Hopkins Medicine. 2019-04-01. https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/prostate-biopsy
- Johns Hopkins Prostate Cancer Multidisciplinary Clinic — Johns Hopkins Medicine. 2024-11-07. https://www.hopkinsmedicine.org/health/treatment-tests-and-therapies/prostate-cancer-treatment
Read full bio of Sneha Tete