Prostatectomy: Purpose, Types, Procedure, Risks & Recovery
Complete guide to prostatectomy surgery: types, procedures, risks, and recovery timelines.
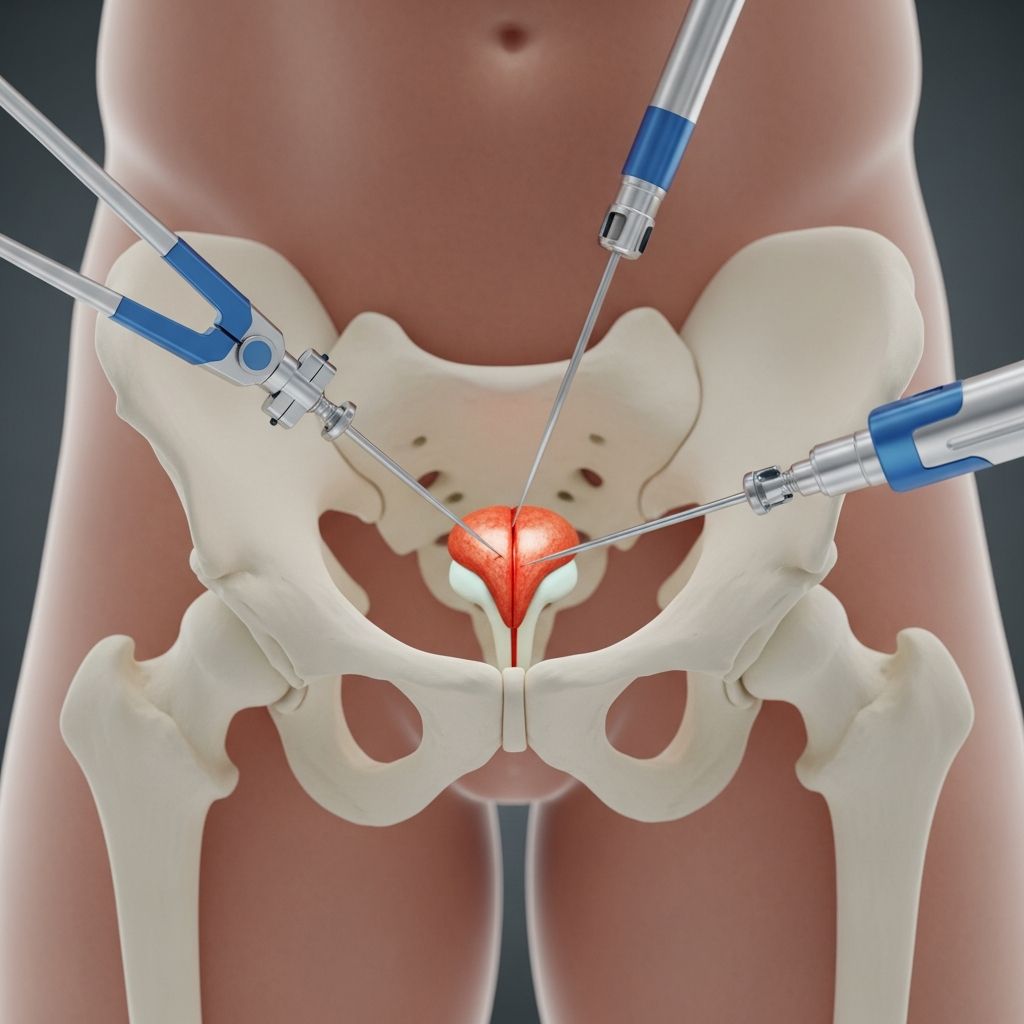
Understanding Prostatectomy: A Comprehensive Guide
A prostatectomy is a surgical procedure in which a urologist removes all or part of your prostate gland to treat prostate cancer or benign prostatic hyperplasia (BPH), a non-cancerous enlargement of the prostate. This procedure is one of the most common treatments for men experiencing serious prostate conditions. Understanding the different types, how the procedure is performed, potential risks, and what to expect during recovery can help you make informed decisions about your healthcare.
The Prostate Gland: Structure and Function
To better understand prostatectomy, it’s helpful to know the anatomy of the prostate gland. Your prostate has two distinct parts: an inner portion that tends to grow as you age, and an outer portion that forms a protective capsule. Think of it like an orange, where the inner portion resembles the fruit and the outer part is similar to the peel. This anatomical understanding is crucial because different surgical approaches target these parts differently, depending on your condition and treatment goals.
Types of Prostatectomy
There are two primary types of prostatectomy procedures, each designed for different conditions and treatment goals:
Simple Prostatectomy
A simple prostatectomy is typically performed to treat benign prostatic hyperplasia (BPH) when the enlarged inner portion of the prostate is causing urinary obstruction. During this procedure, the surgeon removes only the inner portion of the prostate while leaving the outer capsule intact. This is similar to scooping out the fruit of an orange while leaving the peel behind. The surgeon makes a vertical incision in the lower abdomen and carefully removes the inner tissue through this opening. The outer portion of the prostate remains in place, which generally helps preserve more normal urinary and sexual function compared to radical procedures.
Radical Prostatectomy
A radical prostatectomy involves the complete removal of the entire prostate gland. This procedure is typically recommended for men with prostate cancer. During a radical prostatectomy, the surgeon not only removes the entire prostate but also removes surrounding fat and tissues that may contain cancer cells. This often includes the seminal vesicles, which are glands that help produce ejaculate, and sometimes nearby lymph nodes. The surgeon then reattaches your urethra to your bladder using surgical stitches and cuts the vas deferens, the tube that transports semen from your testicles to your urethra.
Surgical Approaches for Prostatectomy
Modern prostatectomy can be performed using several different surgical techniques, each with distinct advantages and considerations.
Open Prostatectomy
In an open prostatectomy, the surgeon makes a larger surgical incision to directly access and remove the prostate. For a simple prostatectomy, the surgeon typically makes a vertical incision in the lower abdomen. For radical prostatectomy, the incision usually runs vertically between the belly button and pubic bone (suprapubic approach). In some cases, the surgeon may choose to make an incision in the skin between the anus and scrotum (perineal approach), though this is less commonly used. The incision typically measures between 6 and 12 inches, allowing the urologist excellent visibility of the prostate and surrounding tissues. After removing the necessary tissue, the surgeon closes the incision with stitches or small metal staples and may place a surgical drain to remove excess blood or fluid during the immediate recovery period.
Laparoscopic Prostatectomy
Laparoscopic surgery represents a less invasive alternative to traditional open surgery. During laparoscopic procedures, the surgeon makes two to four small incisions, each typically less than half an inch in length. A thin rod with a camera at the end, called a laparoscope, is inserted through one incision to provide visualization of the surgical area. Specialized surgical tools are inserted through the other small incisions to perform the necessary tissue removal. This minimally invasive approach generally results in less postoperative pain, smaller scars, and faster recovery times compared to open surgery.
Robotic Prostatectomy
Robotic prostatectomy represents the most advanced surgical approach currently available. The urologist uses robotic surgical equipment to perform the procedure with enhanced precision and control. For a single-port robotic prostatectomy, the surgeon makes just one small incision, typically around three-quarters of an inch. For multi-port procedures, several tiny incisions of similar size are created. The laparoscope and robotic instruments are inserted through these minimal openings. Robotic surgery typically offers superior visualization, greater precision in tissue removal, and often results in less postoperative pain compared to open procedures. Recent innovations include single-port transvesical approaches, where the surgeon accesses the prostate through the bladder itself, offering anatomical advantages and potentially better preservation of urinary and sexual function.
The Surgical Team and Preparation
A specialized team of healthcare providers performs your prostatectomy. The team typically includes your urologist, an anesthesiologist, surgical nurses, and operating room technicians. Before the procedure begins, the anesthesiologist will sedate you with general anesthesia, ensuring you remain asleep, still, and free from pain throughout the surgery. Once you’re under anesthesia, a healthcare provider will insert a urinary catheter—a small, flexible tube that drains urine from your bladder into a collection bag. This catheter remains in place during surgery and typically continues for a period during your recovery.
The Prostatectomy Procedure: Step-by-Step
Open Prostatectomy Procedure
During an open prostatectomy, the urologist uses a sharp, sterile scalpel to carefully make a vertical incision in your lower abdomen. The specific location depends on your condition and the surgeon’s preference. Once the incision is made, providing clear visualization of the prostate and surrounding tissues, the surgeon carefully removes the targeted prostate tissue. For simple prostatectomy, this involves removing just the inner portion. For radical prostatectomy, the entire gland is removed along with surrounding tissues. The surgeon carefully preserves critical structures including nerves important for erectile function when possible. Once tissue removal is complete, the incision is closed using stitches or small metal staples. A surgical drain may be placed to remove blood and fluid accumulation during recovery.
Robotic Prostatectomy Procedure
During a robotic prostatectomy, the urologist makes one or several tiny incisions (typically no larger than three-quarters of an inch) depending on whether a single-port or multi-port approach is used. Through these minimal openings, the surgeon inserts a laparoscope and robotic surgical equipment. The robotic system provides enhanced three-dimensional visualization and precise instrument control, allowing the surgeon to remove the prostate gland and seminal vesicles from surrounding tissues with exceptional accuracy. The surgeon then carefully reattaches your urethra to your bladder using small sutures, preserving the integrity of your urinary system. If indicated, the surgeon may also remove and examine lymph nodes for cancer involvement. Once the procedure is complete, the incisions are closed with sutures, and a surgical drain may be placed if necessary.
Potential Risks and Complications
Like all surgical procedures, prostatectomy carries certain risks that you should discuss thoroughly with your urologist. Common potential complications include:
Incontinence: Urinary incontinence, or involuntary leakage of urine, is one of the most common complications. This can range from occasional slight leakage to more significant loss of bladder control. Most men experience temporary incontinence immediately after surgery, which typically improves over weeks to months as the urinary sphincter strengthens.
Erectile Dysfunction: Prostatectomy can affect sexual function due to nerve involvement during surgery. Even with nerve-sparing techniques, some men experience erectile dysfunction. Modern surgical innovations and techniques are increasingly focused on preserving erectile function and improving sexual outcomes.
Bleeding and Infection: As with any surgery, there is a risk of excessive bleeding during or after the procedure and potential surgical site infection. Your surgical team takes specific measures to minimize these risks.
Anesthesia Risks: General anesthesia carries inherent risks, though serious complications are rare in healthy individuals undergoing routine procedures.
Blood Clots: There is a small risk of deep vein thrombosis (blood clots in the legs) following surgery, which can be prevented through appropriate postoperative care and mobility.
Recovery After Prostatectomy
Immediate Recovery
After your prostatectomy is complete, you’ll be moved to a recovery room where healthcare providers monitor your vital signs and overall condition as you wake from anesthesia. Your surgical team will manage your pain with appropriate medications. You should expect some discomfort following the procedure, though robotic prostatectomy typically causes less pain than open surgery. A urinary catheter remains in place, draining urine into a collection bag. Surgical drains, if placed, are typically removed within a few days as fluid accumulation decreases.
Timeline for Recovery
Most people can expect to recover from prostatectomy within four to ten weeks, though this timeline varies depending on the surgical approach used and individual healing factors. Laparoscopic and robotic procedures typically allow faster recovery compared to open surgery. During the first few weeks, you should expect some discomfort, fatigue, and limitations on physical activity. Your healthcare team will provide specific instructions regarding wound care, when you can return to normal activities, and any activity restrictions. Many patients return to light activities within 2-3 weeks and resume more normal activities within 4-6 weeks. Your urinary catheter will be removed once you demonstrate the ability to urinate normally, which typically occurs several days to a few weeks after surgery.
Long-Term Recovery Considerations
Complete recovery extends beyond the immediate postoperative period. Urinary continence typically improves significantly over three to six months as your urinary sphincter strengthens. Sexual function may take several months to return, and some men benefit from medications or other interventions to support erectile function. Your urologist will schedule follow-up appointments to monitor your recovery, address any concerns, and assess the success of cancer treatment if applicable. Open communication with your healthcare team about your recovery progress is essential for optimal outcomes.
Frequently Asked Questions About Prostatectomy
Q: How long does a prostatectomy procedure take?
A: Surgical time varies depending on the approach and complexity. Open procedures typically take 1-2 hours, while robotic procedures may take 2-3 hours. Your surgeon can provide more specific estimates based on your individual circumstances.
Q: Will I need a blood transfusion during prostatectomy?
A: Most modern prostatectomies result in minimal blood loss, and transfusions are rarely necessary. Your surgical team takes specific measures to minimize bleeding during the procedure.
Q: Can I have sexual relations after prostatectomy?
A: Many men can resume sexual activity several weeks after surgery once they’ve fully healed. However, sexual function may be affected by the procedure. Your urologist can discuss strategies to support sexual health during recovery.
Q: What are the advantages of robotic prostatectomy over open surgery?
A: Robotic surgery typically offers smaller incisions, less postoperative pain, faster recovery, reduced scarring, and potentially better preservation of urinary and sexual function due to enhanced precision.
Q: Will my prostate cancer recur after prostatectomy?
A: Prostatectomy provides excellent cancer control for localized prostate cancer. Your urologist will monitor PSA levels and overall health during follow-up appointments to detect any recurrence early.
Q: How long does the urinary catheter stay in place?
A: The catheter typically remains for 1-2 weeks after surgery, though this varies based on your surgical approach and individual healing. Your healthcare team will remove it once you demonstrate normal urinary function.
Choosing Your Surgical Approach
The best prostatectomy approach for you depends on several factors including your specific condition, cancer staging (if applicable), overall health, surgeon expertise, and your personal preferences regarding recovery time and outcomes. Simple procedures for BPH may be performed using various techniques, while radical prostatectomy for cancer requires careful consideration of oncologic principles alongside functional outcomes. Your urologist can discuss the advantages and disadvantages of each approach in the context of your individual situation, helping you make an informed decision about your surgical treatment.
References
- Prostatectomy: Purpose, Types, Procedure, Risks & Recovery — Cleveland Clinic. Updated 2024. https://my.clevelandclinic.org/health/treatments/24294-prostatectomy
- Laparoscopic Prostatectomy — Cleveland Clinic Journal of Medicine, Vol. 71, No. 2. 2004. https://www.ccjm.org/content/ccjom/71/2/113.full.pdf
- Robotic Radical Prostatectomy in Patients with a Hostile Surgical Abdomen — Cleveland Clinic Consult QD. https://consultqd.clevelandclinic.org/robotic-radical-prostatectomy-in-patients-with-a-hostile-surgical-abdomen
- Single-Port Transvesical Partial Prostatectomy: A Novel Technique for Prostate Cancer — Cleveland Clinic Consult QD. https://consultqd.clevelandclinic.org/novel-technique-for-prostate-cancer-single-port-transvesical-partial-prostatectomy
- Robotic & Image Guided Surgery Program Highlights — Cleveland Clinic Department of Urology. https://my.clevelandclinic.org/departments/urology-kidney/depts/robotic-laparoscopic-surgery
- At a Glance: Single-Port Robot-Assisted Transvesical Prostatectomies — Cleveland Clinic Consult QD. https://consultqd.clevelandclinic.org/at-a-glance-single-port-robot-assisted-transvesical-prostatectomies
- Robot-Assisted Simple Prostatectomy for Benign Prostatic Hyperplasia — Cleveland Clinic Consult QD. https://consultqd.clevelandclinic.org/robot-assisted-simple-prostatectomy-for-benign-prostatic-hyperplasia-video
Read full bio of Sneha Tete













