Prostatectomy: What to Expect During Surgery and Recovery
Complete guide to prostate removal surgery: procedures, recovery timeline, and what patients should know.
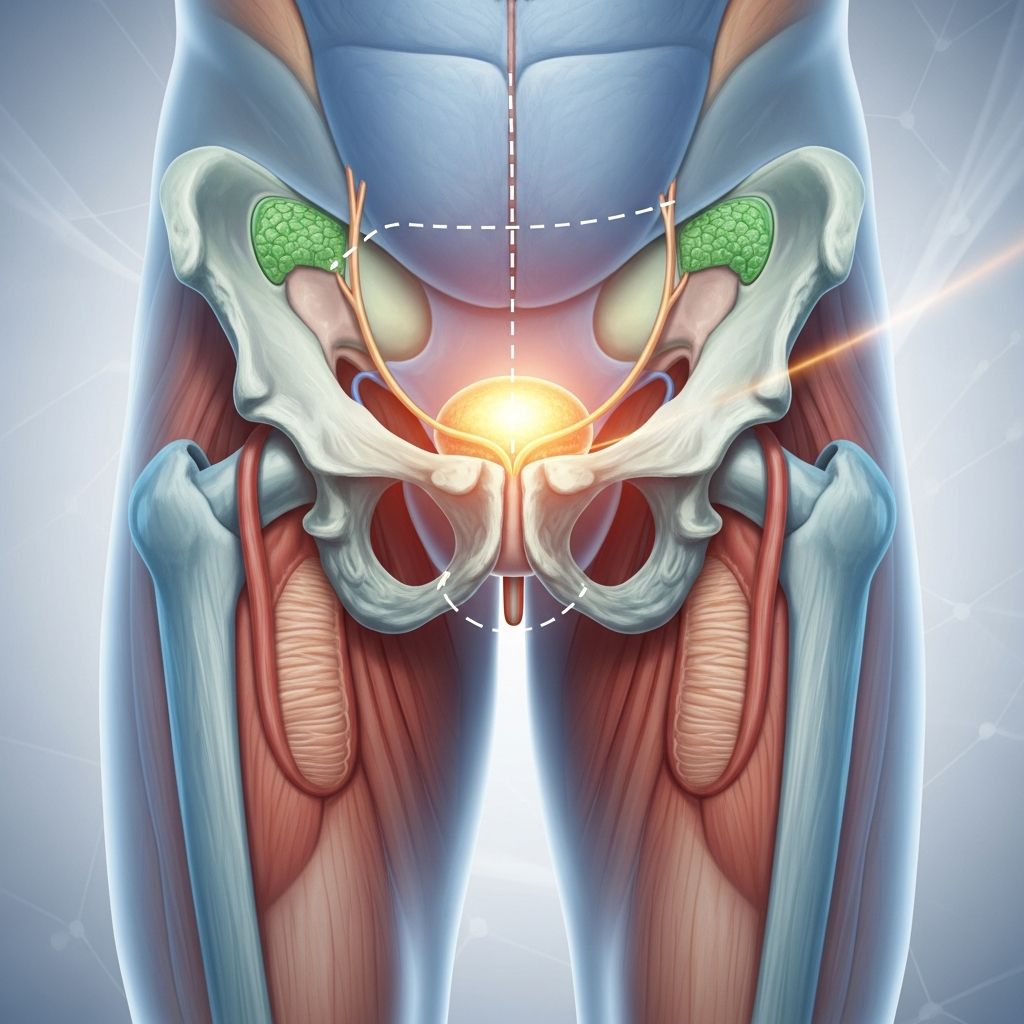
A prostatectomy is a surgical procedure to remove part or all of the prostate gland, often recommended for treating prostate cancer, benign prostatic hyperplasia (BPH), or other prostate conditions. Understanding what to expect before, during, and after this significant surgery can help patients prepare mentally and physically for the procedure and recovery period. This comprehensive guide covers the different types of prostatectomy, what happens during surgery, and the recovery process.
Types of Prostatectomy Procedures
There are several surgical approaches to prostatectomy, each with distinct advantages and considerations. The choice of procedure depends on factors such as the extent of the condition, the surgeon’s experience, patient preference, and overall health status.
Simple Prostatectomy
A simple prostatectomy, also called a transurethral resection of the prostate (TURP) or open simple prostatectomy, involves removing only the inner portion of the prostate gland while leaving the outer shell intact. The surgeon makes a surgical cut in the lower abdomen, typically from below the belly button to just above the pubic bone, or occasionally horizontally above the pubic bone. The surgeon then opens the bladder and removes the inner prostate tissue through this incision, similar to scooping out the inside of an orange while leaving the peel intact. This procedure is commonly used for benign prostatic hyperplasia rather than cancer treatment.
Radical Prostatectomy
During a radical prostatectomy, the surgeon removes the entire prostate gland along with surrounding tissues. This procedure typically includes removal of the seminal vesicles (glands that produce ejaculate) and may involve removal of lymph nodes for cancer staging. The surgeon then reattaches the urethra to the bladder using sutures and cuts the vas deferens, which transports semen from the testicles to the urethra. Radical prostatectomy is the standard surgical treatment for localized prostate cancer.
Robot-Assisted Laparoscopic Prostatectomy
Robot-assisted prostatectomy uses the da Vinci Surgical System to perform minimally invasive surgery. Unlike traditional open surgery, this approach involves several small incisions where surgical instruments and a camera are inserted. The surgeon controls the robotic arms from a computer console, translating hand movements into precise motions of the instruments inside the body. This technique offers potential benefits including reduced blood loss, smaller incisions, and potentially faster recovery compared to open surgery.
Open Retropubic Prostatectomy
In an open retropubic approach, the prostate is removed through an incision in the lower part of the abdomen. This remains a common approach for radical prostatectomy and allows the surgeon direct visualization and access to the prostate gland and surrounding structures.
Open Perineal Prostatectomy
This approach involves removal of the prostate through an incision in the perineum, the area between the scrotum and anus. While less commonly used than the retropubic approach, this technique may be selected in certain clinical situations.
Before Your Surgery
Proper preparation before prostatectomy is essential for a successful procedure and smooth recovery. Your surgical team will provide specific pre-operative instructions tailored to your medical history and the type of procedure you’re having.
Pre-Operative Evaluation
Before surgery, you’ll undergo comprehensive medical evaluation including blood tests, imaging studies, and cardiac assessment if needed. Your surgeon will review your medical history, current medications, and any allergies. It’s important to inform your healthcare team about all medications and supplements you’re taking, as some may need to be discontinued before surgery.
Anesthesia Consultation
You’ll meet with an anesthesiologist who will discuss anesthesia options and answer your questions about the anesthetic plan. Most prostatectomies are performed under general anesthesia, meaning you’ll be completely asleep and pain-free throughout the procedure. Some simpler procedures may use spinal anesthesia.
Fasting Requirements
You’ll typically be instructed to fast (nothing to eat or drink) for several hours before surgery. Follow your surgical team’s specific fasting guidelines, as eating or drinking before surgery can increase risks during anesthesia.
During Your Surgery
Understanding what happens during your prostatectomy can help reduce anxiety and prepare you for the experience. The specific details vary depending on which surgical approach your surgeon uses.
General Surgical Setup
After arriving at the operating room, an anesthesiologist will administer anesthesia to ensure you’re comfortable, asleep, and pain-free. A urinary catheter will be inserted to drain urine during and immediately after surgery. The surgical team performs a standard “time-out” to verify patient identity, surgical site, and procedure details.
Incision and Surgical Approach
For open prostatectomy, the surgeon makes an incision typically between 6 and 12 inches long in the lower abdomen. This large incision gives the surgeon clear visualization of the prostate and surrounding tissues. For robot-assisted procedures, several small incisions are made instead, through which instruments and a camera are inserted.
Prostate Removal and Tissue Handling
The surgeon carefully separates the prostate gland from surrounding tissues, including blood vessels and nerves when applicable. During radical prostatectomy, the seminal vesicles and surrounding fat tissues are also removed. In robot-assisted procedures, the surgeon controls the robotic instruments from a computer console to perform precise movements. For radical prostatectomy, lymph nodes may be removed and examined for cancer spread.
Urethral Reconnection
After removing the prostate, the surgeon reattaches the urethra to the bladder using small sutures. This reconnection is critical for normal urination after recovery. Careful attention to this step helps minimize urinary complications during healing.
Surgical Duration
Prostatectomy typically takes between 2 to 4 hours in the operating room. This timeframe doesn’t include preparation time or recovery room monitoring. The entire surgical experience from arrival to discharge from the recovery area may span several hours.
Immediately After Surgery
Once the procedure is complete, you’ll be moved to a recovery area for careful monitoring as you regain consciousness from anesthesia. Healthcare providers will closely observe your vital signs and manage pain with appropriate medications.
Incision Closure and Drainage
The surgical incision is closed with sutures (stitches) or small metal staples. Your surgeon may also place one or two surgical drain tubes near the surgery site to remove blood or excess fluid as your body heals. These drains typically remain in place for a few days and are usually removed before you leave the hospital or shortly after discharge without requiring additional anesthesia or pain medication.
Catheter Placement
A urinary catheter remains in place after surgery to allow your bladder to rest and heal properly. The catheter may be placed in the urethra or lower abdomen, and sometimes both catheters are used. This catheter drains urine into a collection bag and typically remains for 1 to 3 weeks depending on your surgeon’s preference and the type of prostatectomy performed.
Recovery Timeline and What to Expect
Recovery from prostatectomy is a gradual process that extends well beyond your initial discharge from the hospital. Understanding the typical recovery timeline helps set realistic expectations.
Hospital Stay
Most patients spend 1 to 3 days in the hospital following open prostatectomy, while robot-assisted procedures may result in shorter hospital stays due to the minimally invasive nature. During your hospital stay, nurses will monitor your incision, manage pain, encourage movement, and ensure you’re eating and drinking appropriately.
First Two Weeks at Home
During the first two weeks after surgery, focus on rest and avoiding strenuous activities. You may experience some discomfort, swelling, and bruising around the incision site, which is normal. Keep your incision clean and dry as instructed. Most patients can resume light activities like short walks around the house. Avoid heavy lifting, strenuous exercise, and sexual activity during this period.
Two to Six Weeks Post-Surgery
Gradually increase your activity level as tolerated, but avoid heavy lifting (more than 10 pounds) and strenuous exercise. Many patients can return to light desk work during this period. Most surgical drains are removed within the first two weeks. Your catheter is typically removed after 2 to 3 weeks, though your surgeon will determine the exact timing. After catheter removal, you may experience temporary urinary urgency or frequency as your bladder readjusts.
Six Weeks to Three Months
Most patients can gradually return to normal activities and exercise routines. However, avoid high-impact activities and strenuous exercise until cleared by your surgeon. Sexual activity can typically resume as comfort allows, though erectile dysfunction may occur temporarily or permanently depending on surgical technique and nerve preservation.
Three Months and Beyond
By three months post-surgery, most patients have returned to their normal activities. However, complete healing continues for up to six months to one year. Continued improvement in urinary and sexual function may occur gradually during this extended recovery period.
Managing Common Post-Operative Symptoms
Certain symptoms and challenges are common after prostatectomy and typically resolve with time and appropriate management.
Pain and Discomfort
Mild to moderate pain at the incision site is expected and manageable with prescribed pain medications. Pain typically improves significantly within the first two weeks and continues to diminish over subsequent weeks. Report severe or worsening pain to your healthcare provider.
Urinary Urgency and Frequency
After catheter removal, many patients experience urinary urgency and frequency as the bladder heals and readjusts. This typically improves over weeks to months. Performing pelvic floor exercises (Kegel exercises) can strengthen urinary control muscles and accelerate improvement.
Urinary Incontinence
Some degree of temporary urinary incontinence is common after prostatectomy and usually improves with time and pelvic floor exercises. Most patients achieve continence within 3 to 12 months, though individual recovery varies. Discuss incontinence management strategies with your healthcare provider if symptoms persist.
Erectile Dysfunction
Erectile dysfunction may occur temporarily or permanently depending on surgical technique, nerve preservation, and individual factors. Discuss concerns with your surgeon, as various treatment options are available to help restore sexual function.
When to Contact Your Healthcare Provider
Certain symptoms warrant prompt medical attention during your recovery. Contact your healthcare provider immediately if you experience fever (over 101°F), excessive bleeding or blood clots in urine, signs of infection at the incision site (increased redness, warmth, swelling, or discharge), severe pain unrelieved by medication, inability to urinate after catheter removal, or persistent nausea and vomiting.
Follow-Up Care and Monitoring
Regular follow-up appointments with your urologist are essential after prostatectomy. Your surgeon will monitor your incision healing, assess urinary and sexual function, and in cases of cancer treatment, monitor PSA levels and screen for recurrence. Attend all scheduled appointments and communicate any concerns about your recovery.
Frequently Asked Questions
Q: How long does it take to recover from a prostatectomy?
A: Most patients return to normal activities within 6 to 8 weeks, though complete healing may take 3 to 6 months. Recovery timelines vary based on surgical approach, age, and overall health.
Q: Will I need a blood transfusion during prostatectomy?
A: Blood transfusions are rarely needed during prostatectomy. Modern surgical techniques and careful hemostasis minimize blood loss. Your surgical team will discuss transfusion risks during your pre-operative consultation.
Q: How long will the catheter remain in place?
A: Typically, the catheter remains for 2 to 3 weeks, though this varies by surgeon preference and surgical technique. Your surgeon will provide specific timing instructions.
Q: Is robot-assisted prostatectomy better than open surgery?
A: Both approaches are effective. Robot-assisted surgery offers potential benefits including smaller incisions, reduced blood loss, and potentially faster recovery. Discuss which approach is best for your specific situation with your surgeon.
Q: When can I resume sexual activity after prostatectomy?
A: Most surgeons recommend waiting 4 to 6 weeks after surgery before resuming sexual activity. Discuss specific timing with your surgeon, as individual recovery varies.
Q: Will prostatectomy cure my prostate cancer?
A: Prostatectomy can cure prostate cancer when caught early and localized to the gland. Your surgeon and oncologist will discuss your specific prognosis based on cancer staging and pathology findings.
References
- Robot-Assisted Radical Prostatectomy: A Step-by-Step Guide — National Center for Biotechnology Information (NCBI/PMC). 2018. https://pmc.ncbi.nlm.nih.gov/articles/PMC6071518/
- Simple Prostatectomy — MedlinePlus Medical Encyclopedia, U.S. National Library of Medicine. 2024. https://medlineplus.gov/ency/article/007416.htm
- Prostatectomy: Purpose, Types, Procedure, Risks & Recovery — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/treatments/24294-prostatectomy
- Prostatectomy (Prostate Removal Surgery) — Mayo Clinic. 2024. https://www.mayoclinic.org/tests-procedures/prostatectomy/about/pac-20385198
- Robotic Prostatectomy — Penn Medicine, University of Pennsylvania Health System. 2024. https://www.pennmedicine.org/treatments/robotic-prostatectomy
Read full bio of Sneha Tete