Prostatic Artery Embolization: Minimally Invasive BPH Treatment
Discover how PAE offers a minimally invasive solution for enlarged prostate and urinary symptoms.
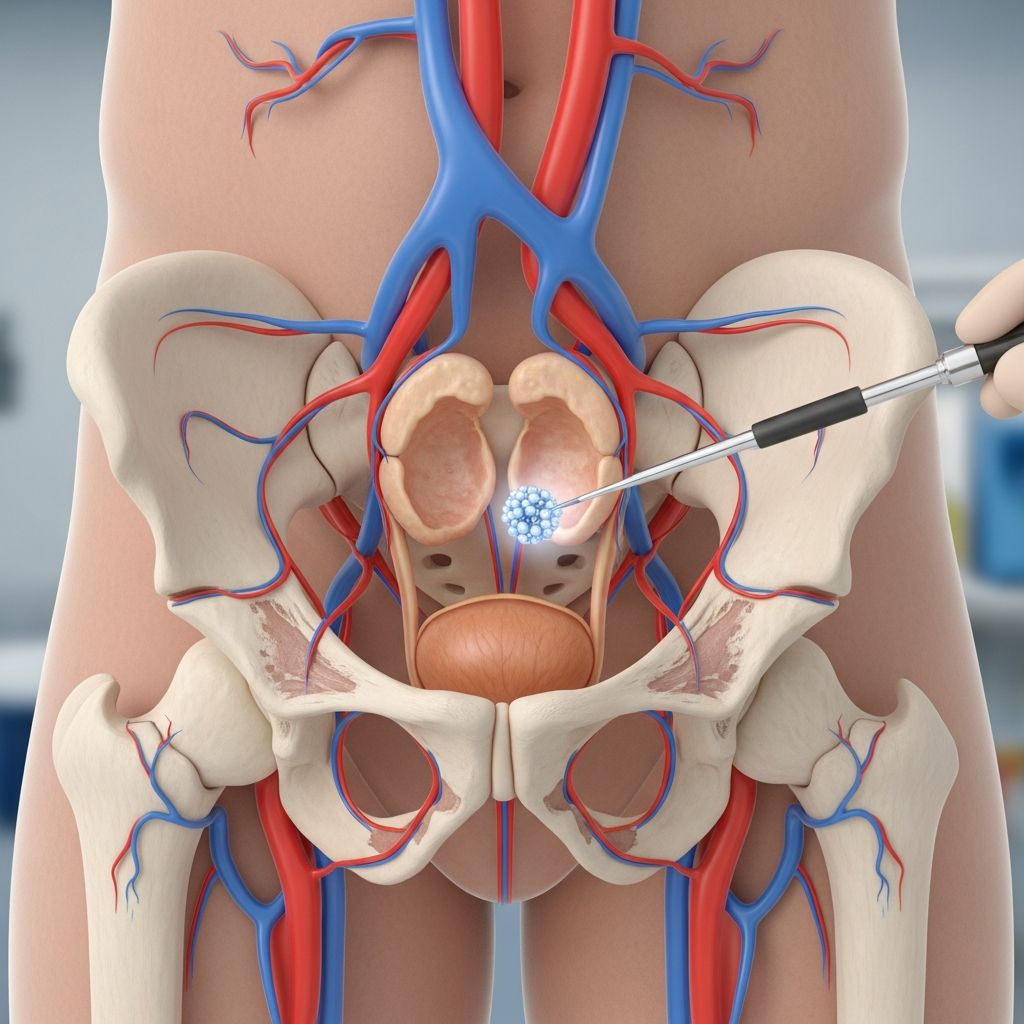
What is Prostatic Artery Embolization?
Prostatic artery embolization (PAE) is a minimally invasive interventional radiology procedure designed to treat benign prostatic hyperplasia (BPH), commonly known as an enlarged prostate. The procedure works by strategically blocking the blood vessels that supply the prostate gland, reducing blood flow and causing the enlarged tissue to shrink over time. Unlike traditional surgical approaches that require general anesthesia and significant recovery time, PAE offers patients a less invasive alternative with minimal downtime and a rapid return to normal activities.
The procedure has emerged as a promising treatment option for men experiencing moderate to severe lower urinary tract symptoms (LUTS) associated with BPH. By reducing the size of the prostate and improving urinary function, PAE provides symptom relief while maintaining sexual function and minimizing complications. This innovative approach has gained increasing recognition in tertiary medical centers across the United States and internationally.
Understanding Benign Prostatic Hyperplasia
Benign prostatic hyperplasia is a common condition affecting aging men. As men get older, the prostate gland naturally enlarges, which can obstruct the urethra and restrict normal urine flow. This enlargement often leads to bothersome urinary symptoms including frequent urination, urgency, weak urine stream, incomplete emptying of the bladder, and nocturia (waking multiple times during the night to urinate).
BPH is not cancer and is not contagious, but it can significantly impact quality of life. While some men manage symptoms with medications, others may require more interventional treatment options. PAE represents an attractive middle ground between medical management and invasive surgical procedures like transurethral resection of the prostate (TURP).
How Prostatic Artery Embolization Works
Prostatic artery embolization operates on a straightforward principle: by reducing blood supply to the prostate, the gland shrinks and urinary symptoms improve. The procedure involves several key steps that are performed by an interventional radiologist using advanced imaging technology.
The PAE Procedure Step-by-Step
Step 1: Access and Preparation
The procedure begins with local anesthesia and intravenous twilight sedation, ensuring patient comfort without requiring general anesthesia. An interventional radiologist makes a small needle puncture, typically in the groin or wrist, to access a major blood vessel. This access point is minimally traumatic and requires only a small bandage after the procedure.
Step 2: Catheter Navigation
A thin, flexible tube called a catheter is inserted through the puncture site and carefully advanced through the blood vessels using real-time X-ray imaging, known as fluoroscopy. This imaging guidance allows the radiologist to precisely navigate the catheter to the prostatic arteries that supply blood to the prostate gland.
Step 3: Artery Identification
Once the catheter reaches the prostatic arteries, the radiologist injects a special contrast dye to visualize the blood vessels more clearly. This detailed imaging confirms the location of the prostatic arterial branches and helps identify any collateral blood vessels that need to be protected during embolization.
Step 4: Micro-Catheter Positioning
A specialized micro-catheter, measuring less than one millimeter in diameter, is then advanced through the main catheter into the prostatic arterial branches. The radiologist may perform a three-dimensional cone-beam CT scan at this stage to obtain detailed volumetric imaging, confirming safe catheter positioning within the target arteries.
Step 5: Embolic Agent Delivery
Microscopic beads called embolic agents—typically microspheres measuring 100 to 500 microns—are slowly injected through the micro-catheter into the prostatic arteries. These particles gradually fill the blood vessels, progressively reducing blood flow to the prostate. The slow injection technique is critical to ensure diffuse distribution throughout the prostate tissue and prevent early vessel occlusion.
Step 6: Bilateral Treatment
Because the prostate typically receives blood supply from both sides of the pelvis, the procedure must be performed on both the right and left prostatic arteries. Once embolization is complete on one side, the catheter is withdrawn and carefully navigated to the opposite pelvic artery, where the embolization process is repeated.
Step 7: Final Verification
After completing embolization on both sides, the radiologist performs final angiography to confirm that blood flow to the prostate has been successfully blocked. The catheter is then carefully removed, and the small arterial puncture closes naturally within a few minutes. A simple bandage is applied to the access site.
The PERFECTED Technique
A refinement in PAE methodology called the PERFECTED technique (Proximal Embolization First, Then Embolize Distal) has demonstrated superior clinical outcomes compared to conventional approaches. This technique involves first embolizing the proximal portions of the prostatic arteries before advancing the micro-catheter distally into the intraprostatic branches. This staged approach produces greater prostate ischemia and infarction, resulting in better symptom improvement and lower recurrence rates.
Clinical Indications for PAE
Prostatic artery embolization is an appropriate treatment option for carefully selected patients meeting specific clinical criteria:
- Men with severe lower urinary tract symptoms secondary to benign prostatic hyperplasia
- Patients who are candidates for TURP or similar surgical procedures but prefer a minimally invasive alternative
- Men with prostate enlargement too extensive for conventional surgical approaches
- Patients who have undergone previous prostate surgery without adequate symptom improvement
- Individuals with medical comorbidities making them poor candidates for general anesthesia
- Men seeking to avoid the sexual dysfunction risks associated with traditional prostate surgery
Benefits of Prostatic Artery Embolization
PAE offers numerous advantages compared to traditional surgical interventions and medical management alone:
Minimally Invasive Approach
Unlike TURP and other surgical procedures, PAE requires only a small needle puncture rather than transurethral instrumentation or open surgery. This minimal tissue trauma translates to reduced pain, faster healing, and minimal blood loss.
Rapid Recovery and Discharge
The entire procedure typically takes two to three hours, followed by a brief recovery period of two to three hours. Most patients are discharged home the same day and can resume normal activities within days, compared to weeks or months required for surgical recovery.
Preservation of Sexual Function
A significant advantage of PAE is its very low rate of sexual dysfunction and ejaculatory complications. Unlike transurethral resection of the prostate, which commonly causes retrograde ejaculation and erectile dysfunction, PAE preserves sexual function in the vast majority of patients. Some men even experience improvement in sexual function following the procedure.
No Tissue Removal
PAE does not require removal of prostate tissue. Instead, it works through controlled ischemia to shrink the existing tissue. This biological approach may result in more durable symptom relief compared to procedures involving tissue resection.
Excellent Safety Profile
Clinical studies have demonstrated that PAE is a safe procedure with low complication rates. The procedure avoids the urethral trauma associated with transurethral approaches and provides an alternative for men who cannot tolerate or are ineligible for general anesthesia.
Symptom Improvement and Outcomes
Following prostatic artery embolization, patients experience gradual but progressive symptom improvement over several weeks to months. As the prostate gland shrinks due to reduced blood supply, the urethra gradually opens, allowing urine to flow more freely and naturally. Most patients report meaningful improvement in lower urinary tract symptoms, including increased urinary flow rates, reduced frequency of urination, decreased nocturia, and improved quality of life scores.
Clinical research has demonstrated that PAE effectively reduces prostate volume and improves urodynamic parameters in the majority of treated patients. The symptom improvement continues to progress over the months following the procedure as the prostate tissue gradually undergoes ischemic involution.
Preparation for Prostatic Artery Embolization
Proper patient preparation is essential for successful PAE outcomes. Pre-procedural evaluations typically include comprehensive clinical examinations, symptom questionnaires to assess baseline urinary function, laboratory tests to evaluate general health and renal function, imaging studies including ultrasound or MRI to assess prostate volume and anatomy, and urodynamic testing in selected cases.
Patients should discuss all current medications with their medical team, as certain blood thinners may need to be adjusted. Fasting requirements are typically similar to those for other procedures requiring anesthesia. Clear communication with the interventional radiology team regarding patient expectations and medical history ensures optimal preparation.
Recovery and Post-Procedure Care
Recovery from prostatic artery embolization is remarkably straightforward. Most patients experience minimal pain at the puncture site, managed easily with over-the-counter analgesics. The small bandage can typically be removed after 24 hours. Patients should avoid strenuous activity and heavy lifting for approximately one week but can resume light activities and work within days.
Initial urinary symptoms may actually worsen slightly in the first few days as inflammation develops; however, this typically resolves within one to two weeks. Progressive symptom improvement continues over the following weeks and months as the prostate gradually shrinks.
Comparing PAE to Alternative Treatments
| Treatment Option | Invasiveness | Recovery Time | Sexual Function Impact | Anesthesia Required |
|---|---|---|---|---|
| Prostatic Artery Embolization | Minimally invasive | Days to weeks | Preserved/improved | Twilight sedation only |
| TURP (Transurethral Resection) | Moderately invasive | Several weeks | Often compromised | General or spinal anesthesia |
| Open Prostatectomy | Highly invasive | Several months | Often compromised | General anesthesia required |
| Medical Management (Medications) | Non-invasive | N/A | May be affected by medications | None required |
Potential Risks and Complications
While prostatic artery embolization has an excellent safety profile, as with any medical procedure, certain risks exist. Potential complications are relatively uncommon and typically minor. These may include temporary urinary urgency or frequency, mild hematuria (blood in urine), transient pelvic pain, rare infections, and very uncommonly, damage to surrounding tissues if the embolic material migrates to unintended locations.
The radiation exposure associated with fluoroscopy is minimized through careful technique and collimation. Serious complications are rare when the procedure is performed by experienced interventional radiologists at qualified medical centers.
Frequently Asked Questions
Q: Is general anesthesia required for PAE?
A: No. The procedure is performed under local anesthesia with intravenous twilight sedation, allowing patients to remain comfortable without the risks associated with general anesthesia.
Q: How long does the PAE procedure take?
A: The procedure typically requires two to three hours to complete, including embolization on both sides of the prostate.
Q: When can I return to normal activities?
A: Most patients can resume light activities within days and return to work within one week. Strenuous activity should be avoided for approximately one week.
Q: Will PAE affect my sexual function?
A: Unlike surgical procedures like TURP, PAE has a very low rate of sexual dysfunction. Most men maintain or improve their sexual function following the procedure.
Q: How long does it take to see symptom improvement?
A: Progressive symptom improvement typically occurs over weeks to months as the prostate gradually shrinks. Significant improvement is usually noted within three to six months.
Q: Is PAE suitable for all men with enlarged prostate?
A: No. PAE is most appropriate for men with moderate to severe LUTS from BPH who have failed medical management or prefer a minimally invasive approach. Individual suitability must be determined through consultation with an interventional radiologist.
Q: What is the success rate of PAE?
A: Clinical studies demonstrate that PAE successfully improves urinary symptoms in the majority of treated patients, with low recurrence rates and excellent safety profiles.
References
- Prostatic Artery Embolization: Indications, Preparation, Techniques, and Imaging Features — Radiological Society of North America (RSNA). 2021. https://pubs.rsna.org/doi/abs/10.1148/rg.2021200144
- Prostate Artery Embolization (PAE) — Penn Medicine, University of Pennsylvania. 2024. https://www.pennmedicine.org/treatments/prostate-artery-embolization
- Prostate Artery Embolization: Challenges, Tips, Tricks, and Controversies — National Center for Biotechnology Information (NCBI), U.S. National Library of Medicine. 2023. https://pmc.ncbi.nlm.nih.gov/articles/PMC9865478/
- Prostate Artery Embolization (PAE) — University of California San Francisco (UCSF) Radiology. 2024. https://radiology.ucsf.edu/patient-care/services/prostate-artery-embolization
- Prostatic Artery Embolization | Fact Sheets — Yale Medicine. 2024. https://www.yalemedicine.org/conditions/prostatic-artery-embolization
- Preparing for Your Prostate Artery Embolization (PAE) — UW Health, University of Wisconsin. 2024. https://patient.uwhealth.org/healthfacts/8058
Read full bio of medha deb













