Prurigo Of Pregnancy: 6 Clinical Images And Key Signs
Explore detailed images and clinical insights into prurigo of pregnancy, a common itchy rash during gestation.
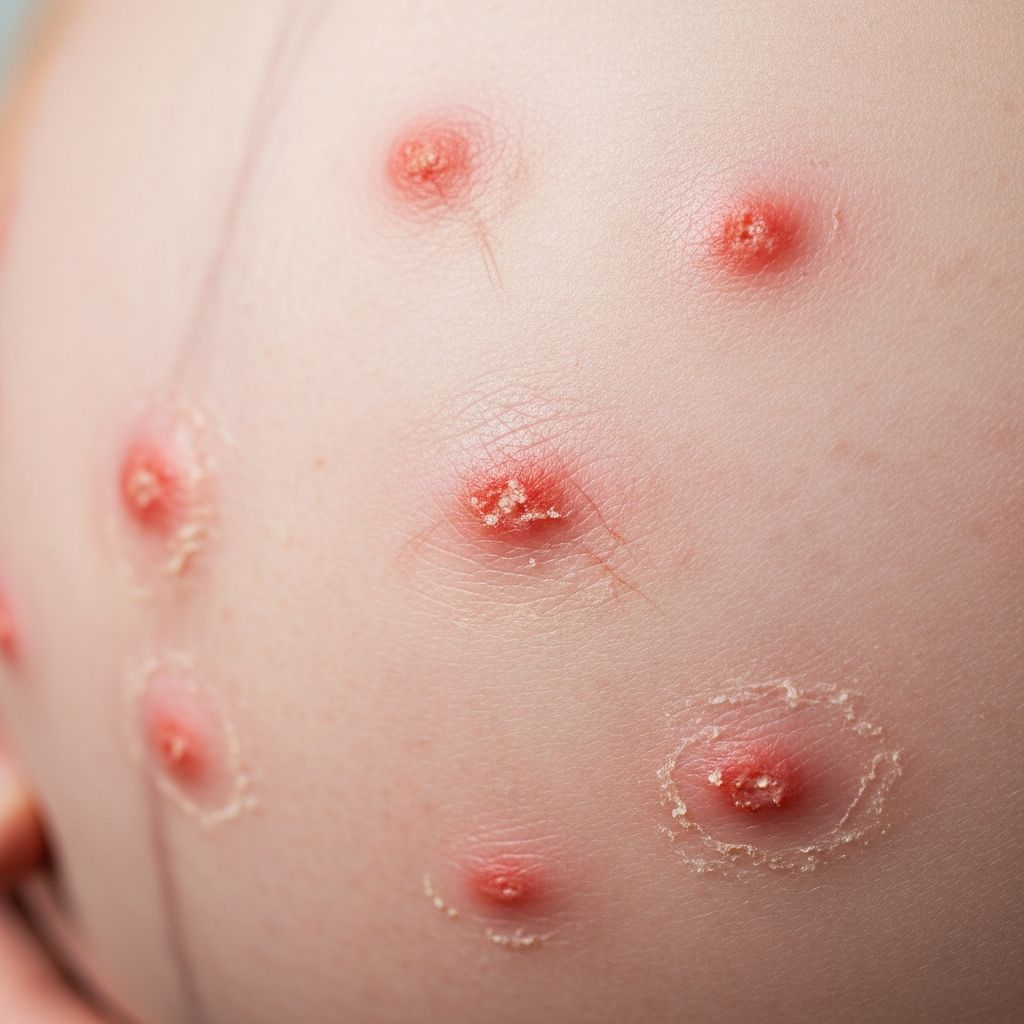
Prurigo of pregnancy — images
Prurigo of pregnancy is a benign cutaneous disorder that arises during pregnancy. It is one of the pruritic dermatoses of pregnancy, characterised by itchy papules and nodules that develop predominantly on the extensor surfaces of the limbs.
What is prurigo of pregnancy?
Prurigo of pregnancy (PP), also known as prurigo gestationis, Besnier prurigo of pregnancy or prurigo nodularis of pregnancy, typically arises during the second or third trimester of pregnancy. It may start as early as the first trimester or present immediately postpartum.
The condition is characterised by excoriated, firm papules and nodules that are intensely itchy. The lesions most commonly affect the extensor surfaces of the limbs (elbows, knees, forearms, shins), but may also involve the abdomen, upper chest and buttocks. The rash is often polymorphic, with surrounding eczematous changes and crusting due to scratching.
Prurigo of pregnancy affects approximately 1 in 300 pregnancies. It is more common in women with atopic dermatitis or a personal/family history of atopy.
Who gets prurigo of pregnancy?
Prurigo of pregnancy most commonly affects women in their second or third trimester, although it may occur at any stage of pregnancy. Risk factors include:
- Atopy: Personal or family history of atopic dermatitis, asthma or allergic rhinitis
- Previous pregnancy: Up to 20% of affected women experience recurrence in subsequent pregnancies
- Extremes of maternal age: Younger (<20 years) or older (>35 years) mothers
- Multiple pregnancy: Higher incidence in twin pregnancies
The condition is more common in women of Asian or African descent.
What causes prurigo of pregnancy?
The exact cause is unknown, but several factors contribute to the development of prurigo of pregnancy:
- Immune dysregulation: Pregnancy induces a T-helper 2 (Th2) immune shift that favours atopic conditions
- Skin barrier dysfunction: The itch-scratch cycle leads to lichenification and nodule formation
- Hormonal changes: Elevated oestrogen and progesterone may contribute
- Genetic predisposition: Familial clustering suggests genetic factors
Importantly, prurigo of pregnancy is not caused by intrahepatic cholestasis of pregnancy (ICP), although both conditions may coexist.
Clinical features
The hallmark of prurigo of pregnancy is severe pruritus preceding the development of skin lesions by days to weeks. Primary lesions include:
- Firm erythematous papules (2–5 mm)
- Domed nodules (5–20 mm)
- Excoriations and crusting from scratching
Lesions are symmetrically distributed and classically affect:
| Common sites | Less common sites |
|---|---|
| Extensor forearms | Abdomen |
| Extensor thighs | Chest |
| Anterior shins | Buttocks |
| Elbows | Scalp |
| Knees | Palmoplantar |
Chronic lesions become lichenified and hyperpigmented. The face, palms, soles and mucous membranes are typically spared.
Diagnosis
Diagnosis is primarily clinical, based on characteristic morphology and distribution during pregnancy. Key diagnostic features include:
- Onset during pregnancy (usually 2nd/3rd trimester)
- Intense pruritus preceding lesions
- Extensor limb papules/nodules with excoriations
- Absence of primary vesicles, bullae or pustules
Differential diagnosis
| Condition | Key distinguishing features |
|---|---|
| Intrahepatic cholestasis of pregnancy | Excoriations without primary lesions; elevated bile acids |
| Atopic eruption of pregnancy | More eczematous; follicular papules; earlier onset |
| Pruritic folliculitis | Sterile follicular pustules; less excoriated |
| Scabies | Burrows, interdigital webs, genitalia involved |
| Drug eruption | History of new medication; polymorphic |
Investigations
- Serum bile acids and LFTs: To exclude intrahepatic cholestasis of pregnancy
- Full blood count: Eosinophilia uncommon
- Skin biopsy: If diagnosis uncertain (shows non-specific spongiotic dermatitis)
- Scrapings: To exclude scabies
Images
Image 1: Classic extensor forearm lesions
This image shows multiple excoriated erythematous papules and nodules on the extensor forearms — the most characteristic site for prurigo of pregnancy. Note the surrounding lichenification from chronic scratching.
Image 2: Anterior shin distribution
Typical lesions on the shins demonstrating the predilection for extensor surfaces. The firm nodules show central crusting with peripheral erythema.
Image 3: Knee involvement
Symmetrical papulonodular eruption on the knees with prominent excoriations. This distribution pattern strongly supports the diagnosis.
Image 4: Abdominal extension
Less common abdominal involvement showing scattered excoriated papules amid striae gravidarum. Trunk lesions help distinguish from simple atopic dermatitis.
Image 5: Hyperpigmented chronic lesions
Advanced lesions demonstrating post-inflammatory hyperpigmentation and marked lichenification — hallmarks of chronic prurigo gestationis.
Image 6: Close-up of individual nodule
High-magnification view of a typical 1 cm dome-shaped nodule with central umbilication and peripheral scale. These lesions are pathognomonic.
Management
Treatment is symptomatic and focuses on pruritus relief and preventing new lesions. No treatment affects disease duration.
First-line therapy
- Emollients: Apply frequently (minimum 250g/week)
- Mid-potency topical corticosteroids (mometasone 0.1%, betamethasone 0.1%): BD to lesions
- Pregnancy-safe oral antihistamines:
- Loratadine 10mg daily
- Cetirizine 10mg daily
- Chlorphenamine 4–6mg QDS
Second-line therapy
- High-potency topical steroids (clobetasol 0.05%): Short courses (<2 weeks)
- Intralesional triamcinolone: 10mg/ml for persistent nodules
- Narrowband UVB phototherapy: 2–3x/week (safe in pregnancy)
Severe/refractory cases
- Oral prednisolone: 0.5–1mg/kg/day for 5–7 days then taper
- Cyclosporine: 3–5mg/kg/day (limited pregnancy safety data)
Supportive measures
- Cool oatmeal baths
- Mentholated creams (0.5–1%)
- Wet wraps with dilute steroid/emollient
- Trim nails short; cotton gloves at night
- Avoid hot showers and irritants
Complications
- Secondary bacterial infection from excoriations
- Post-inflammatory hyperpigmentation
- Sleep disturbance and anxiety
- Recurrence in 20% of subsequent pregnancies
No maternal or fetal complications from prurigo of pregnancy itself.
Prognosis
Lesions typically persist until delivery but resolve within 4–6 weeks postpartum. However:
- 15–20% of women have active lesions at delivery
- Postpartum flares occur in 10%
- Recurrence risk in future pregnancies: 20%
- Residual hyperpigmentation may last months
Frequently asked questions
Q: Is prurigo of pregnancy harmful to my baby?
A: No. Prurigo of pregnancy has no adverse effects on the fetus and does not increase risks of preterm birth or low birth weight.
Q: Will I get it again in my next pregnancy?
A: Approximately 20% of women experience recurrence, usually milder and of shorter duration.
Q: How long does it take to clear after delivery?
A: Most lesions resolve within 4–6 weeks postpartum, although pigmentation may persist longer.
Q: Can I breastfeed if I have prurigo of pregnancy?
A: Yes. Topical treatments and most antihistamines are safe during breastfeeding. Avoid high-potency steroids on the breast.
Q: Is this the same as cholestasis of pregnancy?
A: No. Cholestasis causes itching without primary rash and requires bile acid testing for diagnosis.
References
- Clinical Manifestations and Management of Prurigo in Pregnancy — PMC. 2024. https://pmc.ncbi.nlm.nih.gov/articles/PMC12754684/
- Prurigo of pregnancy (papular dermatitis and pruritic folliculitis) — Dermatology Advisor. 2023-10-15. https://www.dermatologyadvisor.com/home/decision-support-in-medicine/dermatology/prurigo-of-pregnancy-papular-dermatitis-and-pruritic-folliculitis/
- Prurigo Of Pregnancy – Causes, Symptoms, Diagnosis, and Treatment — Apollo Hospitals. 2024. https://www.apollohospitals.com/diseases-and-conditions/prurigo-of-pregnancy
- Identifying Common Pregnancy Rashes: Symptoms and Treatment — Schweiger Dermatology. 2023. https://www.schweigerderm.com/skin-care-articles/medical-dermatology/identifying-common-pregnancy-rashes/
- What Causes Rashes During Pregnancy and How to Treat Them — Healthline (citing AAFP). 2024-01-10. https://www.healthline.com/health/pregnancy/what-causes-rashes-during-pregnancy-and-how-to-treat-them
- Prurigo Of Pregnancy: Causes, Treatment & What It Looks Like — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/22642-prurigo-of-pregnancy
Read full bio of medha deb












