Radiculopathy: Causes, Symptoms, and Treatment
Complete guide to understanding radiculopathy: nerve compression, symptoms, diagnosis, and effective treatment options.
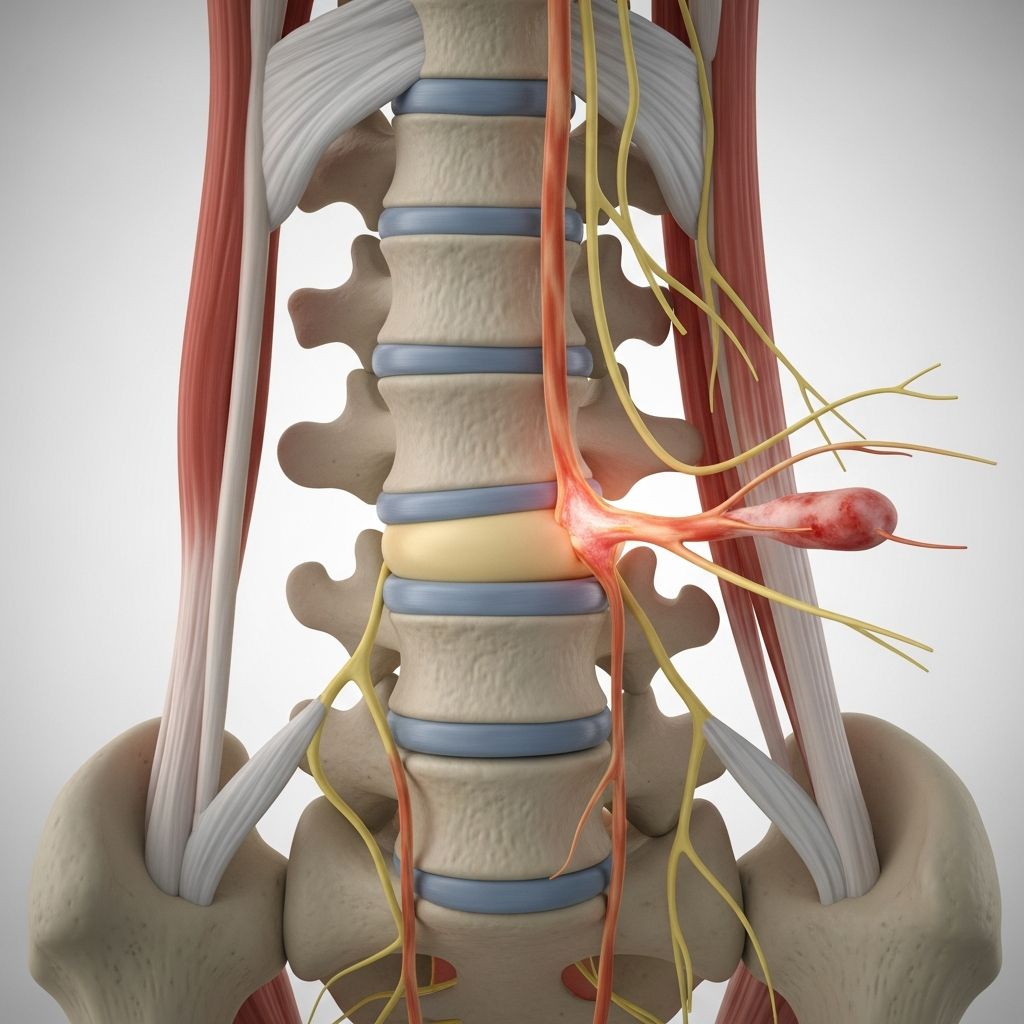
Understanding Radiculopathy
Radiculopathy is a medical condition that occurs when nerve roots in the spine become compressed, irritated, or inflamed. This compression can result from various spinal conditions and typically causes pain, weakness, numbness, and tingling sensations that radiate along the path of the affected nerve. The condition is sometimes referred to as a “pinched nerve” and can affect different regions of the spine, causing symptoms that vary depending on the location of the nerve compression.
When nerve roots are compressed or irritated, they send abnormal signals to the brain, resulting in the characteristic symptoms experienced by those with radiculopathy. Understanding this condition is essential for proper diagnosis and treatment, as early intervention can prevent long-term complications and help restore normal function.
Types of Radiculopathy by Location
Radiculopathy can develop in different regions of the spine, and the location determines which parts of the body are affected. Each type presents distinct symptoms and may require different management approaches.
Cervical Radiculopathy
Cervical radiculopathy involves compression of nerve roots in the neck region of the spine. This type affects the nerves that control movement and sensation in the upper limbs and typically causes pain, tingling, or weakness in the shoulders, arms, or hands. The symptoms often worsen with certain neck movements, such as turning the head or lifting heavy objects. In severe cases, patients may experience loss of coordination or difficulty with fine motor skills.
Thoracic Radiculopathy
Thoracic radiculopathy affects the nerve roots in the upper back region. This type is less common than cervical or lumbar radiculopathy but can cause pain, numbness, or tingling in the chest, ribs, or abdominal area. Symptoms may extend to the front of the body and can significantly impact quality of life if left untreated.
Lumbar Radiculopathy
Lumbar radiculopathy involves compression of nerve roots in the lower back and is the most common type. This condition frequently leads to sciatica, characterized by sharp, burning pain that radiates down the legs. Patients often experience numbness and weakness in the legs, which may worsen with physical activity or prolonged sitting.
Symptoms and Signs of Radiculopathy
The symptoms of radiculopathy vary depending on which nerve roots are affected and the severity of the compression. Common symptoms include:
General Symptoms
The hallmark symptom of radiculopathy is nerve root pain that radiates along the distribution of the affected nerve. Patients commonly experience sharp or burning pain that travels from the site of compression to distant body areas. Other general symptoms include:
- Sharp or burning pain in the back, arms, legs, or shoulders
- Tingling or “pins and needles” sensations
- Numbness in the skin of the arms or legs
- Muscle weakness or loss of reflexes
- Hypersensitivity to light touch
- Loss of coordination in severe cases
Cervical Radiculopathy Specific Symptoms
When cervical nerve roots are compressed, symptoms typically manifest in the upper body. These may include sharp or burning pain that radiates down the shoulder or arm, which often worsens with specific neck movements and improves when resting the hands on the head. Tingling and abnormal sensations such as pins and needles commonly occur in the hands or fingers, and patients may experience weakness, numbness, or loss of reflexes in the shoulder, arm, or hand.
Lumbar Radiculopathy Specific Symptoms
Lumbar radiculopathy typically affects the lower extremities. Patients often experience pain radiating down one or both legs, a condition known as sciatica. This pain may be accompanied by numbness, weakness, or tingling in the legs and feet. Symptoms frequently worsen with physical activity, prolonged sitting, or certain movements that place additional pressure on the affected nerve roots.
Causes and Risk Factors
Radiculopathy develops when conditions narrow the spaces where nerve roots exit the spine. The most common causes include:
Primary Causes
- Herniated Discs: One of the most common causes, occurring when the soft inner material of a spinal disc protrudes and compresses adjacent nerve roots.
- Spinal Stenosis: A condition characterized by the narrowing of the spinal canal, which reduces space available for nerve roots.
- Bone Spurs: Bony growths that develop along the spine, often due to arthritis or degenerative disc disease, can compress nerve roots.
- Degenerative Disc Disease: Age-related wear and tear of the spinal discs, leading to loss of disc height and nerve compression.
- Thickening of Spinal Ligaments: Ligament hypertrophy can reduce space available for nerve roots.
Risk Factors
Certain factors increase the likelihood of developing radiculopathy. These include age-related degenerative changes, obesity, repetitive lifting or pushing activities, poor posture, previous spinal injuries or surgeries, and conditions such as degenerative joint disease. Additionally, activities that place strain on the spine or individuals with a sedentary lifestyle combined with poor core strength are at higher risk.
Diagnosis of Radiculopathy
Accurate diagnosis is essential for developing an appropriate treatment plan. The diagnostic process typically involves multiple steps and assessment techniques.
Clinical Evaluation
The initial step in diagnosing radiculopathy begins with a thorough physical examination and comprehensive medical history review. During the physical exam, your healthcare provider will assess your range of motion, posture, muscle function, and reflexes. They may perform specific movement tests to identify pain patterns and determine which nerves are affected. Sensory testing helps detect numbness or tingling in specific distributions.
Your medical history provides crucial information about the onset and duration of symptoms, any past injuries or surgeries, and conditions that may contribute to nerve compression. This information helps differentiate between acute injuries, chronic conditions, and age-related changes.
Imaging and Diagnostic Tests
Several imaging and diagnostic tests help confirm radiculopathy and identify the underlying cause:
- Magnetic Resonance Imaging (MRI): Provides detailed images of the spine, discs, and nerves to identify compression sources.
- Computed Tomography (CT) Scan: Offers detailed bone imaging and can reveal bone spurs or stenosis.
- X-rays: Help identify structural changes and degenerative conditions.
- Electromyography (EMG): Measures electrical activity in muscles to assess nerve function.
- Nerve Conduction Studies: Evaluate how well nerves transmit electrical signals.
- Nerve Ultrasound: Uses sound waves to visualize nerves and identify compression.
These diagnostic tools help determine the location and severity of nerve compression, which guides appropriate treatment selection.
Treatment Options for Radiculopathy
Treatment for radiculopathy depends on the severity of symptoms and the underlying cause. Most cases improve within 6 to 12 weeks with appropriate conservative management, though some may require more advanced interventions.
Conservative Treatment Approaches
The majority of radiculopathy cases respond well to non-surgical treatment strategies:
Lifestyle Modifications
Initial management often focuses on lifestyle changes that reduce nerve irritation. Gentle movements and exercises help minimize pain and speed recovery by allowing the nerve to calm down. Continuing to move teaches your body that activity is safe while building support and strength along the spine. This may include activity modification, proper ergonomics, and avoiding positions that worsen symptoms.
Physical Therapy
Customized physical therapy programs are highly effective for managing radiculopathy. These programs typically include stretching exercises to improve flexibility, strengthening exercises to support the spine, postural training, and therapeutic modalities such as heat, cold, ultrasound, or electrical stimulation. Physical therapy strengthens the muscles surrounding the spine, improves posture, and alleviates nerve pressure, promoting long-term recovery.
Medications
Various medications can help manage radiculopathy symptoms:
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): Over-the-counter options like ibuprofen or naproxen reduce pain and inflammation.
- Muscle Relaxants: Help reduce muscle spasms that may contribute to nerve compression.
- Anticonvulsants: Medications like gabapentin or pregabalin can help manage nerve pain.
- Corticosteroids: More potent anti-inflammatory agents for severe cases.
Always consult with a healthcare provider before starting any medication regimen to avoid potential side effects, especially with long-term use.
Thermal Therapy
Ice and heat therapy can provide symptom relief. Ice therapy may reduce inflammation and numb pain in acute phases, while heat therapy can relax muscles and improve blood flow during chronic phases. These modalities are often used in conjunction with other treatments.
Steroid Injections
Epidural steroid injections deliver anti-inflammatory medication directly to the affected area around the nerve root. These injections can provide significant relief for patients with moderate to severe pain who have not responded adequately to conservative measures.
Advanced and Surgical Treatment Options
When conservative treatments fail to provide relief or symptoms worsen, more advanced interventions may be necessary:
Advanced Treatments
- Spinal Decompression Therapy: Non-surgical technique that gently stretches the spine to reduce pressure on nerve roots.
- Acupuncture and Chiropractic Care: Alternative approaches that may provide symptom relief for some patients.
- Massage Therapy: Can help reduce muscle tension and improve circulation.
Surgical Interventions
Surgery becomes an option when conservative treatments fail or neurological deficits worsen. Surgical procedures include:
- Microdiscectomy: Removal of a portion of a herniated disc to relieve nerve compression.
- Laminectomy: Removal of part of the lamina (spinal bone) to enlarge the spinal canal.
- Foraminotomy: Enlargement of the foramen (opening where nerve roots exit) to increase space for nerves.
- Artificial Disc Replacement: Replacement of a degenerated disc with an artificial one to maintain spine mobility.
These minimally invasive techniques often result in less postoperative pain and faster recovery times compared to traditional open surgery.
Prognosis and Outcomes
The prognosis for radiculopathy depends on early diagnosis and appropriate treatment. When diagnosed and treated early, healthcare providers can often reduce or eliminate painful symptoms through minimally invasive techniques or conservative management. In general, radicular symptoms improve within 6 to 12 weeks with proper care.
Without proper treatment, patients face a higher risk of developing more severe symptoms that can potentially cause permanent nerve damage. While rare, untreated radiculopathy can lead to serious long-term complications including paralysis, bowel or bladder dysfunction, or permanent numbness. This underscores the importance of early consultation with a healthcare provider when symptoms develop.
Prevention and Management Strategies
While some risk factors for radiculopathy cannot be controlled, several preventive strategies may reduce your risk:
- Maintain proper posture during daily activities and at work
- Engage in regular exercise to strengthen core muscles
- Practice proper lifting techniques when handling heavy objects
- Maintain a healthy weight to reduce spinal stress
- Take regular breaks during prolonged sitting or repetitive activities
- Avoid smoking, which can degenerate spinal discs
- Sleep on a supportive mattress and use proper pillow positioning
- Stay hydrated and maintain good nutrition for spinal health
Frequently Asked Questions
Q: Is radiculopathy permanent?
A: When diagnosed and treated early, most cases of radiculopathy are not permanent. Symptoms typically improve within 6 to 12 weeks with conservative treatment. However, without proper treatment, there is a risk of developing permanent nerve damage, including paralysis or permanent numbness, though this is rare.
Q: Can radiculopathy go away on its own?
A: Many cases of radiculopathy do improve over time without invasive treatment. Most people experience symptom improvement within 6 to 12 weeks. However, conservative treatments like physical therapy, medications, and lifestyle modifications can significantly accelerate recovery.
Q: What is the difference between radiculopathy and myelopathy?
A: Radiculopathy refers to compression of nerve roots exiting the spine, causing pain and weakness in specific areas. Myelopathy refers to compression of the spinal cord itself, which can cause more widespread symptoms affecting multiple limbs and bodily functions.
Q: When should I see a doctor for suspected radiculopathy?
A: You should schedule an appointment with a healthcare provider if you experience persistent sharp pain, numbness, tingling, or weakness that radiates along one side of your body, especially if symptoms worsen or interfere with daily activities.
Q: Can physical therapy alone treat radiculopathy?
A: Physical therapy is often effective as part of a comprehensive treatment approach. Many patients experience significant improvement with physical therapy combined with lifestyle modifications, medications, and proper rest. However, the effectiveness depends on the severity of nerve compression.
Q: What imaging test is best for diagnosing radiculopathy?
A: MRI is typically the most useful imaging test for diagnosing radiculopathy, as it provides detailed images of the spine, discs, and nerves. However, a combination of tests including X-rays, CT scans, and nerve studies may be used depending on the clinical situation.
References
- The Complete Radiculopathy Guide: From Diagnosis to Recovery — Rupa Health. Accessed December 2025. https://www.rupahealth.com/post/the-complete-radiculopathy-guide-from-diagnosis-to-recovery
- A Patient’s Guide to Radiculopathy — New Jersey Spine Specialists. Accessed December 2025. https://njspinespecialists.net/blog/radiculopathy-guide/
- Radiculopathy: Definition, Types, Symptoms, Causes & More — Hinge Health. Accessed December 2025. https://www.hingehealth.com/resources/glossary/radiculopathy/
- Radiculopathy: Symptoms, Causes & Treatment — Healthgrades. Accessed December 2025. https://resources.healthgrades.com/right-care/spine-conditions/radiculopathy
- The Complete Guide to Pinched Nerves and Radiculopathy — Achilles Neurology. Accessed December 2025. https://achillesneurology.com/conditions/pinched-nerves
Read full bio of medha deb











