Runner’s Knee: Symptoms, Causes, and Treatment
Learn about runner's knee (patellofemoral pain syndrome), its symptoms, causes, treatments, and prevention strategies for lasting knee health.
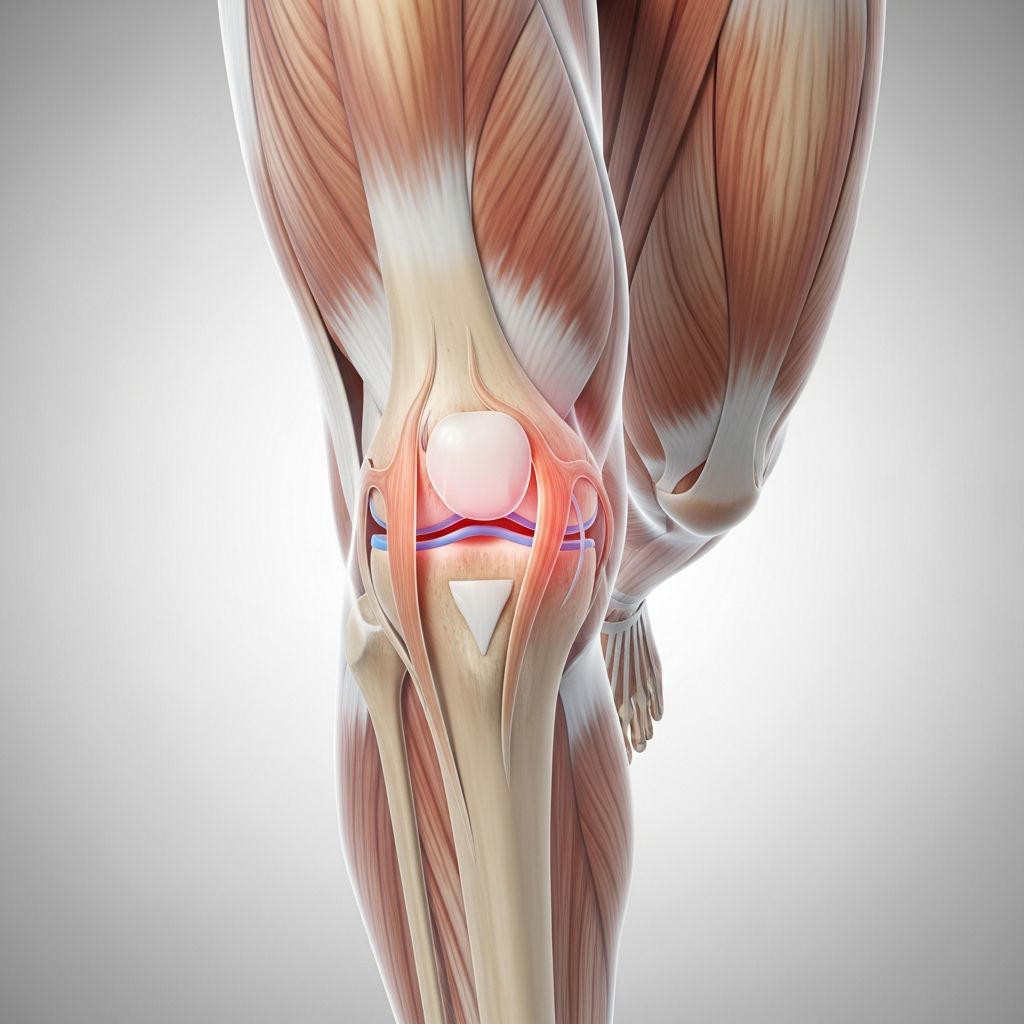
Runner’s knee, medically known as
patellofemoral pain syndrome (PFPS)
, is a prevalent overuse injury characterized by pain around or behind the kneecap (patella). It commonly affects runners, jumpers, skiers, cyclists, and soccer players due to repetitive knee stress, but can occur in non-athletes from daily activities.What Is Runner’s Knee?
Runner’s knee refers to pain originating from irritation or breakdown of cartilage under the kneecap, improper patella tracking in the femoral groove, or surrounding soft tissue strain. The patella fails to glide smoothly, leading to friction, inflammation, and discomfort. This condition encompasses anterior knee pain syndrome, patellofemoral malalignment, and chondromalacia patella.
It arises when repetitive bending stresses the knee joint, particularly in sports involving running, jumping, or squatting. Even walking or cycling can trigger it in susceptible individuals. Pain typically manifests as a dull ache that intensifies with activity.
Symptoms of Runner’s Knee
Symptoms often emerge during or post-exercise and worsen with specific movements. Key signs include:
- Pain at the front of the knee, especially around, under, or along the inner edge of the kneecap.
- Tenderness when pressing the kneecap.
- Swelling after activity.
- Stiffness or pain after prolonged sitting (“movie sign”), walking hills, stairs, or squatting.
- Clicking, popping, or grinding sensations (crepitus) during knee motion.
Pain may start mildly and progress to sharp discomfort, particularly during downhill running or kneeling. It often feels worse after inactivity.
Causes of Runner’s Knee
Runner’s knee stems from multiple factors, primarily
overuse
where knees endure excessive repetitive stress without adequate recovery. Common triggers include:- Overuse from high-impact activities: Repeated knee bending in running, lunges, plyometrics, squats, or stair climbing.
- Malalignment: Kneecap tracking issues due to hip-to-ankle bone misalignment, increasing pressure on cartilage.
- Muscle imbalances: Weak or tight quadriceps, hips, or hamstrings fail to stabilize the patella.
- Foot problems: Flat feet, high arches, or overpronation alter gait, stressing the knee.
- Direct trauma: Falls or blows to the knee.
- Anatomical variations: Leg length discrepancy, knock-knees, or bowlegs.
Risk amplifies with sudden training increases, poor biomechanics, or inadequate warm-ups.
Risk Factors for Developing Runner’s Knee
Certain groups face higher susceptibility:
- Athletes in running, jumping, or cycling sports.
- Novice runners or those ramping up intensity/duration rapidly.
- Individuals with weak thigh/hip muscles or tight iliotibial bands.
- Those with foot deformities or wearing unsupportive shoes.
- Females, due to wider pelvis potentially increasing Q-angle (though evidence is mixed).
- Workers involving prolonged squatting or heavy lifting.
Combining factors like overuse with muscle weakness heightens risk.
How Runner’s Knee Is Diagnosed
Diagnosis relies on clinical history and physical exam, confirming pain around the kneecap during stress activities like squatting or stair climbing, absent other pathologies.
Doctors assess:
- Pain location and triggers.
- Kneecap mobility and tenderness.
- Leg alignment, muscle strength, and gait.
- Foot structure.
Imaging (X-rays, MRI) rules out fractures, meniscus tears, or osteoarthritis, rare in younger patients. No specific test confirms PFPS; it’s exclusion-based.
Treatment Options for Runner’s Knee
Conservative management resolves most cases within weeks to months. Strategies include:
- RICE protocol: Rest, Ice (20 mins every 2-3 hours), Compression, Elevation.
- Pain relief: NSAIDs like ibuprofen (short-term; avoid masking pain for intense activity).
- Activity modification: Avoid painful motions; switch to low-impact like swimming.
- Bracing/taping: Patellar straps or McConnell taping realign the kneecap.
- Physical therapy: Core for strengthening and stretching.
Surgery is rare, reserved for persistent cases with maltracking.
Physical Therapy and Rehabilitation Exercises
PT focuses on addressing root causes via targeted exercises. Perform 2-3 sets of 10-15 reps, 3-5x/week, progressing gradually.
| Exercise | Target | How to Do It |
|---|---|---|
| Straight Leg Raises | Quadriceps | Lie on back, one knee bent. Tighten quad, lift straight leg 12 inches, hold 5 secs. Lower slowly. |
| Clamshells | Hip abductors | Lie on side, knees bent. Keep feet together, lift top knee like clamshell. Hold 3-5 secs. |
| Wall Sits | Quads, glutes | Back against wall, slide to 90-degree knee bend. Hold 20-60 secs. |
| Hip Bridges | Glutes, hamstrings | Lie on back, feet flat. Lift hips to form straight line from knees to shoulders. |
| Calf Stretches | Achilles, calves | Step one foot back, heel down, lean forward. Hold 30 secs per side. |
Include balance work on foam pads and gait retraining. Foam rolling IT band aids flexibility.
Preventing Runner’s Knee
Proactive steps reduce recurrence:
- Gradual progression: Follow 10% rule—increase mileage/intensity by no more than 10% weekly.
- Strength training: Maintain balanced quads, hips, core 2-3x/week.
- Proper footwear: Replace shoes every 300-500 miles; consider orthotics for flat feet.
- Warm-up/cool-down: Dynamic stretches pre-run, static post.
- Cross-training: Mix running with biking, yoga to avoid overuse.
- Biomechanics check: Video gait analysis or PT consult.
Listen to body signals; rest at early pain signs.
When to See a Doctor for Runner’s Knee
Seek medical advice if:
- Pain persists >2 weeks despite rest.
- Swelling, locking, or giving way occurs.
- Inability to bear weight or straighten knee.
- Associated fever or redness (infection sign).
Early intervention prevents chronic issues.
Frequently Asked Questions (FAQs)
Why do my knees hurt after running?
Knee pain post-run often stems from overuse like runner’s knee, stress fractures, or arthritis. Repetitive impact irritates tissues; PFPS specifically targets the kneecap.
Can runner’s knee heal on its own?
Yes, with rest, ice, and activity modification, most cases resolve in 4-6 weeks. Consistent rehab accelerates recovery.
Is runner’s knee the same as chondromalacia?
Chondromalacia patella (cartilage softening) is one cause of runner’s knee; PFPS is the broader syndrome including maltracking and tendon strain.
How long does recovery from runner’s knee take?
Typically 6-12 weeks with proper treatment; full return to sport may take 3-6 months.
Can I still run with runner’s knee?
Avoid running until pain-free; opt for alternatives. Gradual return under guidance prevents re-injury.
References
- Runner’s Knee: Symptoms, Pain, Causes, and Treatment — WebMD. 2023-10-15. https://www.webmd.com/pain-management/knee-pain/runners-knee
- Runner’s Knee – Patellofemoral Pain — Joshua Frank MD. 2024-05-20. https://www.joshuafrankmd.com/runners-knee/
- Overview: Patellofemoral pain syndrome (runner’s knee) — NCBI/NIH. 2023-08-01. https://www.ncbi.nlm.nih.gov/books/NBK561507/
- Patellofemoral Pain Syndrome (PFPS): Symptoms & Treatment — Cleveland Clinic. 2024-02-12. https://my.clevelandclinic.org/health/diseases/17914-patellofemoral-pain-syndrome-pfps
- Knee pain and other running injuries — NHS. 2024-11-05. https://www.nhs.uk/live-well/exercise/knee-pain-and-other-running-injuries/
Read full bio of Sneha Tete











