Salivary Stones: Causes, Symptoms, and Treatment Options
Complete guide to understanding salivary stones, their symptoms, diagnosis, and effective treatment approaches.
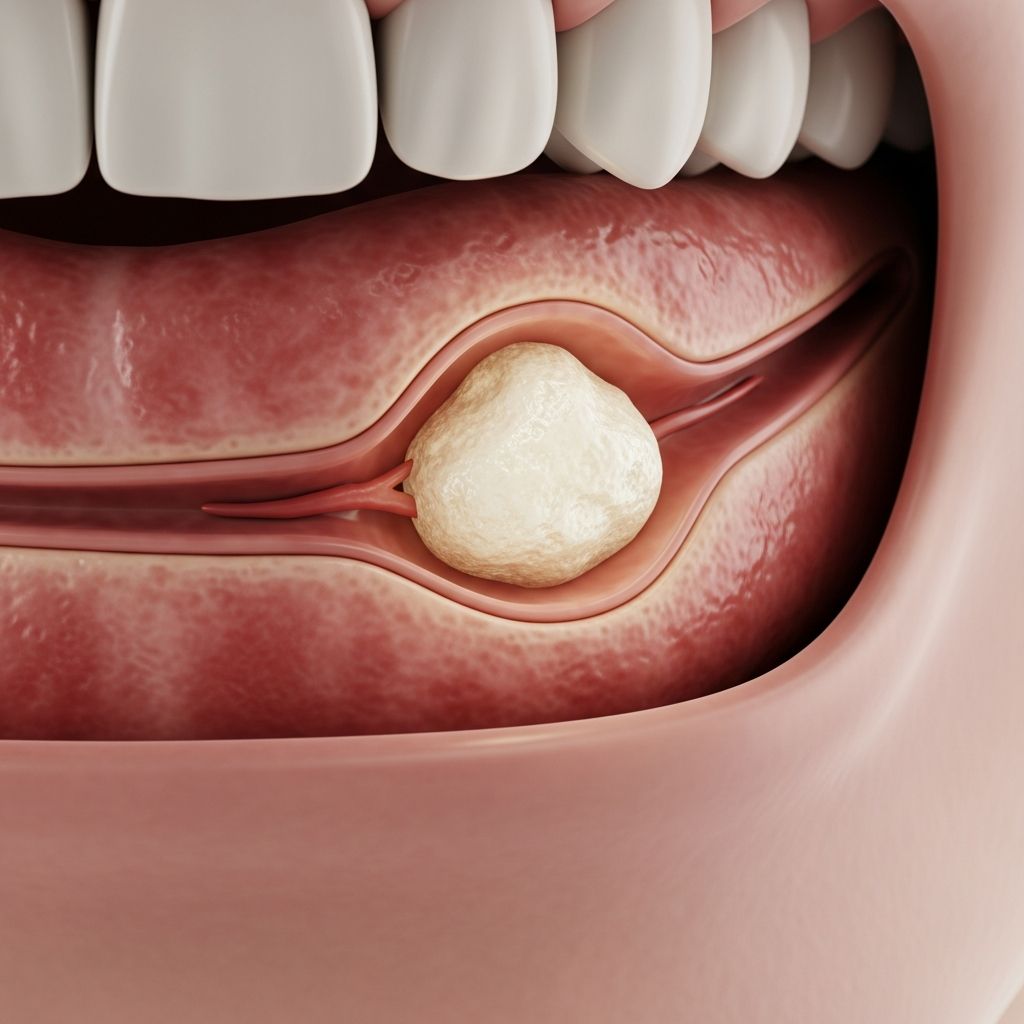
Understanding Salivary Stones
Salivary stones, medically known as sialoliths or salivary duct stones, are calcified structures that form inside salivary glands or their ducts. These mineral deposits can obstruct the normal flow of saliva into the mouth, leading to various uncomfortable symptoms and potential complications. Understanding the nature of these stones, their formation, and available treatment options is essential for anyone experiencing symptoms or concerned about their oral health.
The majority of salivary stones develop in the submandibular glands, which are located at the floor of the mouth below the jaw. These glands are responsible for producing a significant portion of the saliva that lubricates and aids in digestion. Less commonly, stones may form in the parotid glands located on the inside of the cheeks or the sublingual glands situated under the tongue. It is important to note that many individuals with this condition develop multiple stones simultaneously, complicating the clinical presentation and requiring comprehensive management strategies.
What Causes Salivary Stones
Salivary stones develop when chemicals present in saliva accumulate within the salivary duct or gland tissue. These deposits are predominantly composed of calcium and other minerals. While the exact mechanism of stone formation is not completely understood, research has identified several contributing factors that increase the risk of sialolith development.
Decreased salivary flow, or salivary stasis, represents one of the primary risk factors for stone formation. When saliva production is reduced, minerals and other substances that are normally diluted and washed away can precipitate and accumulate. Several factors contribute to reduced saliva production or thickened saliva consistency:
– Chronic dehydration and inadequate fluid intake- Poor nutritional habits and decreased food intake- Medications that suppress salivary gland function, including certain antihistamines used for allergies, blood pressure medications, psychiatric drugs, and bladder control medications- Systemic conditions affecting saliva composition- Trauma to the salivary glands from injury or previous dental procedures- Anatomical variations in salivary duct structure that predispose to stasis
The biochemical composition of saliva can also play a role in stone formation. Individuals with altered saliva composition, particularly those with elevated calcium levels, may have a higher predisposition to developing sialoliths. Understanding these risk factors allows individuals to implement preventive measures and seek timely medical attention when symptoms develop.
Recognizing Symptoms and Complications
The presentation of salivary stones varies significantly depending on whether the stone is completely occluding the duct or only partially blocking it. Many stones may form silently without causing any noticeable symptoms. However, as stones grow larger or shift position within the duct system, they can trigger distinctive symptoms that warrant medical evaluation.
During the initial formation phase, stones typically cause no symptoms. However, if a stone reaches a size sufficient to block the salivary duct, saliva backs up into the affected gland, causing characteristic pain and swelling. This obstruction increases intra-glandular pressure, leading to progressive discomfort. The pain may be intermittent at first but tends to worsen over time, particularly during meals when salivary gland activity increases.
Common symptoms of salivary stones include:
– Dull, aching pain in the mouth that fluctuates in intensity- Swelling in the affected area, including the cheek, jaw, or under the tongue- Increased pain and swelling during or after eating, when the glands are stimulated to produce more saliva- Difficulty opening the mouth or swallowing- Dry mouth sensation- Redness and inflammation around the affected gland- In cases of infection, fever and systemic symptoms
The periodic painful attacks caused by salivary stones are often referred to as salivary colic, and intense pain during meals may indicate complete ductal obstruction, typically lasting one to two hours. Approximately 90% of patients with salivary stones develop infection of the affected gland, and 12-18% experience purulent discharge from the gland opening. This infection, known as sialadenitis, can be caused by bacterial overgrowth resulting from the stagnant saliva environment created by the stone obstruction.
Diagnostic Approaches
Accurate diagnosis of salivary stones requires a systematic approach combining clinical assessment and imaging studies. The diagnostic process typically begins during a patient consultation when symptoms are reported and medical history is obtained.
During the physical examination, a healthcare provider will assess the affected area for signs of swelling, palpate the region to detect masses, and evaluate the patient’s ability to open the mouth and swallow. In some cases, the stone can be felt by bimanual examination, where the examiner places fingers both inside and outside the mouth to locate the calcified deposit.
If physical examination suggests a salivary stone, imaging studies may be ordered to confirm the diagnosis and determine the stone’s exact location and size:
– Ultrasound imaging: Often used as a first-line imaging modality due to its safety, accessibility, and effectiveness in visualizing stones within the duct system- Computed tomography (CT) scans: Provide detailed cross-sectional images that help identify the stone and exclude other potential diagnoses such as tumors, dental abscesses, swollen lymph glands, lymphoma, or sarcoidosis- X-ray imaging: May be utilized, though some salivary stones have limited radiopacity and may not be visible on conventional radiographs- Sialography: A specialized radiographic technique where contrast dye is injected into the salivary duct to visualize the duct system and confirm stone presence- Panoramic dental radiographs: Routine dental imaging that may incidentally reveal asymptomatic stones
Blood tests may also be ordered to assess for signs of infection or systemic conditions contributing to stone formation. These diagnostic tools work together to provide a comprehensive picture of the patient’s condition and guide treatment planning.
Treatment Options
The primary objective in treating salivary stones is to remove the obstruction while preserving salivary gland function and minimizing patient discomfort and complications. Treatment approaches are individualized based on stone size, location within the duct system, presence of infection, and the patient’s overall health status.
Conservative Management
For small stones or those in early stages, conservative non-invasive approaches may be attempted first. These methods focus on stimulating saliva flow to facilitate natural stone passage and reducing associated symptoms.
Conservative management strategies include:
– Salivary gland massage: Gentle massage of the affected gland can help encourage stone movement and saliva flow- Sialogogues: Substances that stimulate saliva production, such as lemon juice or sour candies, can increase saliva flow and potentially promote spontaneous stone passage- Heat therapy: Warm compresses or soaks applied to the affected area help reduce pain and promote relaxation of gland tissues- Increased fluid intake: Maintaining proper hydration supports optimal saliva production- Sour diet: Consuming acidic foods and beverages stimulates saliva secretion- Antibiotic therapy: If infection is suspected, antibiotics are prescribed to treat bacterial infection and prevent abscess formation
This conservative approach has the highest success rate when stones are small and located in the duct rather than within the gland tissue itself. Patients should maintain consistent application of these measures and report any worsening symptoms to their healthcare provider.
Minimally-Invasive Sialendoscopy
Sialendoscopy represents a significant advancement in salivary stone treatment, offering a minimally-invasive alternative to traditional surgical gland removal. This technique was developed and successfully utilized in Europe for over a decade before gaining widespread adoption in North American medical centers.
During sialendoscopy, a tiny lighted scope (endoscope) is carefully inserted into the salivary gland’s opening in the mouth. This allows the surgeon to visualize the entire salivary duct system in real-time detail. Once the stone is located using this visualization, micro-instruments are introduced through the scope to carefully extract the stone and relieve the blockage. The procedure is typically performed under local anesthesia or light general anesthesia, allowing patients to return home the same day.
Advantages of sialendoscopy include:
– Preservation of salivary gland function- Elimination of surgical scars and stitches- Minimal recovery time with almost instantaneous functional recovery- Reduced postoperative pain and discomfort- Outpatient procedure reducing hospitalization requirements- Lower complication rates compared to traditional surgery
This procedure is particularly effective for stones that can be palpated during physical examination or those localized by ultrasound within the prehilar region of the gland. Penn Medicine and similar academic medical centers are recognized as national leaders in this cutting-edge treatment approach.
Surgical Removal
In cases where stones cannot be removed through conservative measures or sialendoscopy, or when the salivary gland has sustained irreversible damage, surgical removal of the affected gland may become necessary. This approach is typically reserved for patients with:
– Recurrent salivary stones despite previous treatment attempts- Significant, irreversible damage to gland tissue- Chronic, refractory infections- Failed minimally-invasive procedures
While salivary gland removal is sometimes necessary, modern practice emphasizes gland preservation whenever possible. This is because removal eliminates the gland’s contribution to overall saliva production, which can lead to dry mouth (xerostomia) and related complications. Surgical gland removal is only performed in rare cases where minimally-invasive procedures cannot effectively remove the stone.
Post-Treatment Care and Prevention
Following successful stone removal, patients should implement measures to prevent recurrence and support gland healing. After stone extraction, it is recommended that patients perform salivary gland massage several times daily, combined with a sour diet and continued use of sialogogues to stimulate saliva flow and prevent new stone formation.
Long-term prevention strategies include:
– Maintaining adequate hydration throughout the day- Consuming a balanced diet with sufficient nutritional content- Reviewing medications with healthcare providers to identify those that may suppress saliva production- Chewing sugar-free gum to stimulate saliva flow- Practicing good oral hygiene- Avoiding prolonged periods without food or drink- Managing underlying systemic conditions that may affect saliva composition
Frequently Asked Questions
Q: Can salivary stones disappear on their own?
A: Small salivary stones may pass spontaneously with conservative management, including increased fluid intake, gland massage, and stimulation of saliva flow through sour candies or lemon juice. However, larger stones typically require professional intervention.
Q: How long does sialendoscopy take, and when can I return to normal activities?
A: Sialendoscopy is an outpatient procedure typically performed in 30-60 minutes. Recovery is almost instantaneous, and most patients can return to normal activities within a few days, though vigorous activity should be limited initially.
Q: What happens if I leave salivary stones untreated?
A: Untreated stones can lead to chronic pain, recurrent infections, permanent gland damage, and abscess formation. Progressive damage may eventually necessitate gland removal, making early treatment preferable.
Q: Are salivary stones common in children?
A: While more common in older adults, salivary stones can occur in children and even infants, sometimes causing serious infections requiring prompt medical attention.
Q: How can I prevent salivary stones?
A: Prevention focuses on maintaining adequate hydration, ensuring proper nutrition, minimizing medications that suppress saliva, and managing underlying health conditions that affect saliva composition and flow.
References
- Salivary Gland Stones: Symptoms, Causes, and Treatment — WebMD. 2024. https://www.webmd.com/oral-health/salivary-gland-stones-symptoms-causes-treatments
- Salivary stones: symptoms, aetiology, biochemical composition and management — Nature, British Dental Journal. 2015. https://www.nature.com/articles/sj.bdj.2014.1054
- Salivary Gland Stone (Sialolithiasis) — Penn Medicine. 2024. https://www.pennmedicine.org/conditions/salivary-gland-stone
- Salivary gland stones – Symptoms and management — NHS. 2024. https://www.nhs.uk/conditions/salivary-gland-stones/
- Salivary Duct Stones — Children’s Hospital of Philadelphia. 2024. https://www.chop.edu/conditions-diseases/salivary-duct-stones
- Managing Your Salivary Gland Stones – Symptoms & Treatment — Carle Foundation Hospital. 2024. https://carle.org/conditions/salivary-gland-stone
- Salivary Gland Stone: Care Instructions — MyHealth Alberta. 2024. https://myhealth.alberta.ca/Health/aftercareinformation/pages/conditions.aspx?hwid=abq9474
Read full bio of Sneha Tete











