Scabies: Causes, Symptoms, Treatment & Prevention Guide
Complete guide to understanding scabies: learn about symptoms, transmission, diagnosis, and effective treatment options.
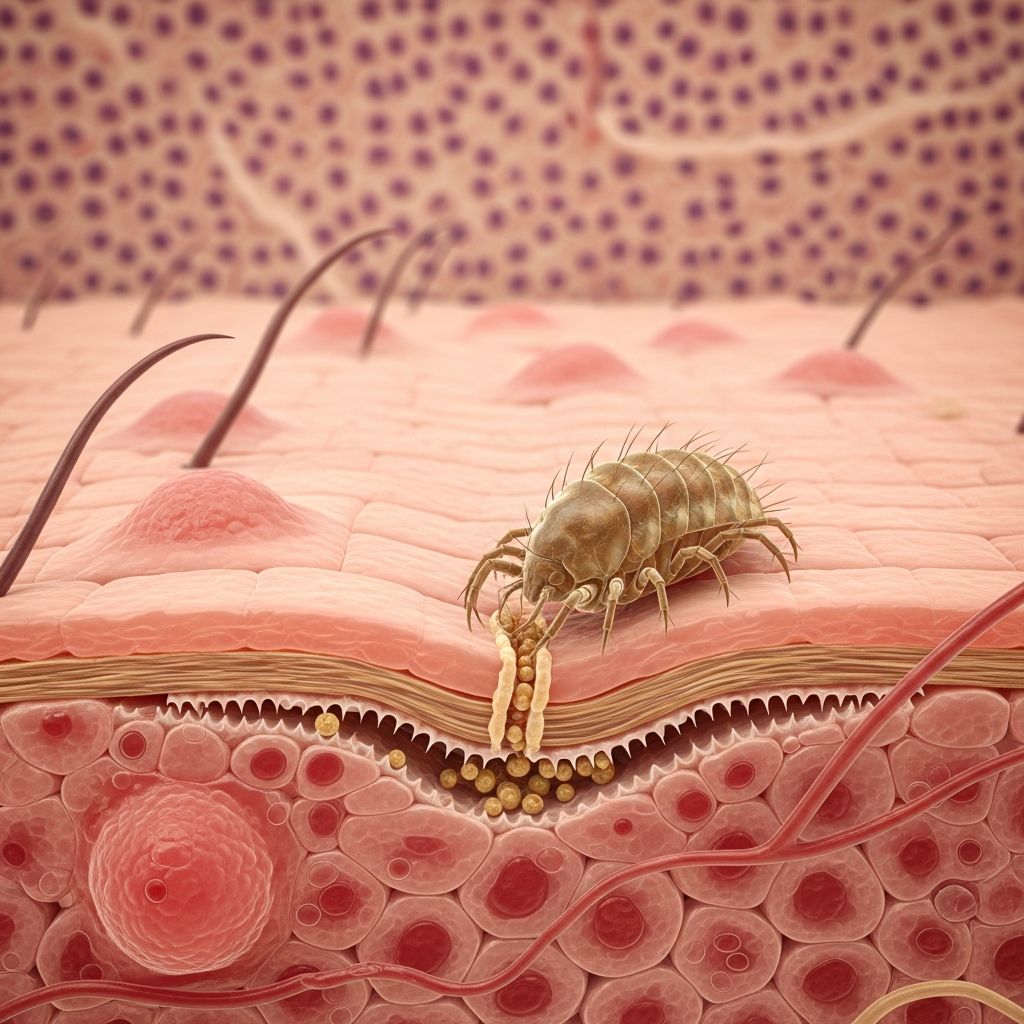
What is Scabies?
Scabies is a highly contagious skin condition caused by infestation with a parasitic mite called Sarcoptes scabiei. This microscopic mite burrows into the superficial layer of your skin (the stratum corneum) to live, feed, lay eggs, and defecate. The infestation triggers an immune response from your body, resulting in intense itching and characteristic skin rashes that can appear on various parts of your body. Scabies affects people of all ages and socioeconomic backgrounds, though certain populations are at higher risk of infection.
The condition is spread primarily through prolonged direct skin-to-skin contact with an infected person. Despite common misconceptions, scabies is not a sign of poor hygiene; rather, it is an infectious disease that requires prompt treatment to prevent spread to close contacts, family members, and others in shared living spaces.
How Do You Get Scabies?
Scabies spreads through direct contact with an infected person. The mites are transmitted when skin touches infected skin for approximately 10 to 15 minutes. This is why scabies spreads rapidly in environments with close contact, such as:
- Family homes and households
- Child care facilities and schools
- Nursing homes and residential care facilities
- Prisons and detention centers
- Hospitals and healthcare settings
In classic scabies, transmission through contaminated clothing, bedding, or furniture (fomite spread) is rare. However, in crusted scabies, a severe variant, fomite transmission is much more common due to the massive number of mites present on the skin and in the environment.
It is important to note that scabies is not spread through casual contact such as shaking hands briefly or sitting near an infected person at a distance. The mite cannot survive long away from human skin, so prolonged, intimate contact is necessary for transmission.
Symptoms of Scabies
The symptoms of scabies vary depending on whether you are experiencing a primary infection or a reinfestation, as well as your immune status.
Timeline of Symptom Development
Primary Infection: In people who have never had scabies before, symptoms typically appear 4 to 6 weeks after initial exposure to the mite. During this period, the mite burrows into the skin and begins reproducing, but the body’s immune system has not yet developed a reaction to the infestation. This delay in symptom onset can mean that infected individuals unknowingly spread the condition to others for several weeks.
Reinfestation: People who have had scabies before can develop symptoms much more quickly, sometimes within hours to days of re-exposure. This accelerated response occurs because the body has already developed sensitization to mite antigens from the previous infection.
Primary Symptoms
Intense itching, especially at night, is the hallmark symptom of scabies. This pruritus (itching) is caused by a delayed type IV hypersensitivity reaction to the mite’s presence and byproducts in the skin. The itching can be severe enough to disrupt sleep and cause significant discomfort throughout the day and night.
A pimple-like or bumpy rash commonly accompanies the itching. The rash consists of small, itchy papules (raised bumps) that may appear red, brown, or gray depending on your skin tone. The rash can look similar to hives, insect bites, or pimples and may appear in lines across the skin, representing the burrows created by the mites.
Common Locations on the Body
Scabies lesions typically appear in specific areas of the body where the mite prefers to burrow. These common sites include:
- Webbing between the fingers
- Wrists, elbows, and knees
- Armpits and axillae
- Waistline and abdomen
- Buttocks and thighs
- Genitals (penis, scrotum in males; vulva in females)
- Breasts and areolae
- Shoulder blades
- Soles of the feet
In infants and young children, the condition may also affect the scalp, face, palms, and soles of the feet, as well as areas behind the ears. The neck and facial areas are typically spared in adults with classic scabies, except in cases of crusted scabies or in elderly and immunocompromised individuals.
Burrows
One distinctive feature of scabies is the presence of burrows—thin, wavy tunnels created by the female mite as it burrows into the skin. These burrows appear as very small irregular tracks, often with a tiny papule (bump) or vesicle (fluid-filled blister) at one end. The burrow represents the path the mite takes as it tunnels through the superficial skin layer. Not all scabies cases display obvious burrows, as the rash may be generalized and eczematous features may dominate the clinical presentation.
Types of Scabies
Scabies presents in several distinct forms, each with different characteristics and treatment implications:
Classic (Ordinary) Scabies
This is the most common form of scabies, characterized by the typical presentation of intense pruritus and papular rash in the areas mentioned above. An individual with classic scabies typically harbors only 10 to 15 mites on the entire body. The symptoms are caused by the body’s immune response to the mite antigens rather than by tissue damage from the mites themselves.
Nodular Scabies
A variant of classic scabies, the nodular form is characterized by erythematous (reddish), pruritic nodules that preferentially develop in moist, thin-skinned areas such as the axillae (armpits) and groin. These nodules represent a hypersensitivity reaction to the presence of the female mite and may persist even after successful treatment of the infestation.
Crusted Scabies (Norwegian Scabies)
This is a severe and highly infectious variant that occurs primarily in elderly individuals and those who are immunosuppressed, including people with HIV/AIDS, lymphoma, or those who have undergone organ transplants. In crusted scabies, the palms and soles become covered with crusted plaques, and there is massive infestation with thousands or even hundreds of thousands of mites. This variant is much more contagious than classic scabies and can lead to heavy infestation of bedding and upholstery. Crusted scabies requires aggressive treatment with combination therapy and can be difficult to cure.
Bullous Scabies
A rare severe manifestation of scabies, bullous scabies is characterized by fluid-filled blisters and requires prompt medical attention.
Diagnosis of Scabies
Scabies diagnosis is primarily clinical, based on the characteristic presentation of symptoms and the distribution of lesions on the body. Your healthcare provider will examine your skin carefully, looking for burrows, papules, and the typical pattern of rash distribution.
While laboratory confirmation can strengthen the diagnosis, it is not always necessary. Skin scrapings from suspected burrows can be examined under a microscope to reveal mites, eggs, or fecal pellets, but this test is insensitive and may not always detect the mites even when they are present. Dermoscopy, a non-invasive technique using a specialized magnifying device, can reveal the characteristic “jetliner trail sign” pattern associated with scabies burrows.
Because scabies can present atypically in certain populations—such as elderly individuals, people with dark skin (where it may appear as granulomatous nodules), and immunocompromised patients—clinical suspicion is paramount. Your healthcare provider may recommend treatment based on clinical findings alone without waiting for laboratory confirmation.
Risk Factors and Vulnerable Populations
While anyone can develop scabies, certain populations are at higher risk of infection and may experience more severe disease:
- Young children: More susceptible to infection and often experience widespread involvement including the face, scalp, and palms.
- Elderly individuals: May develop subtle skin findings despite intense itching, making diagnosis challenging.
- People with weakened immune systems: Including those with HIV/AIDS, lymphoma, or post-organ transplant recipients, who may develop crusted scabies.
- People with developmental disabilities: Often experience rapid spread due to close living conditions.
- Hospitalized or institutionalized individuals: Including those in nursing facilities, prisons, and hospitals where close contact facilitates transmission.
- People with other skin conditions: Those with atopic dermatitis or eczema may be more susceptible to secondary bacterial infection.
Complications of Scabies
While scabies itself is not life-threatening, it can lead to significant complications if left untreated or if the intense itching leads to excessive scratching.
Skin Damage and Secondary Infection
The intense itching associated with scabies often leads to scratching, which can result in skin damage including excoriations (scratch marks), encrustation, and lichenification (thickening of the skin). More seriously, the intense itching can lead to scratching that creates skin sores, which sometimes become infected with bacteria on the skin such as Staphylococcus aureus or beta-hemolytic streptococci. This process is known as impetiginization.
Secondary bacterial infection can manifest as impetigo (characterized by honey-colored yellow crusts) or cellulitis (painful, erythematous skin infection). These bacterial superinfections may require additional antibiotic treatment beyond the scabicide used to treat the mite infestation.
Other Complications
Chronic scratching over weeks to months can result in prurigo nodularis, a condition characterized by nodular lesions caused by repetitive scratching and skin inflammation. Additionally, the psychological impact of intense itching and the social stigma associated with a parasitic infection can lead to sleep disturbance, anxiety, and depression in some individuals.
Treatment of Scabies
Scabies is treatable with prescription medications that kill the mites. Treatment options include both topical creams and oral medications, and the choice depends on the type of scabies, patient age, and other factors.
Topical Treatments
Permethrin 5% cream is the first-line treatment for scabies. This scabicide is applied to the entire body (except the head in adults; including the head in children) and left on for 8 to 14 hours before washing off. Because the mites and eggs may not all be killed with a single application, permethrin is typically applied a second time after 7 days. This two-dose approach is necessary to eliminate mites that may hatch from eggs after the first application.
Sulfur ointment is safe for use in infants younger than 2 months and can also be used in pregnant women and young children. It is applied for three consecutive nights and then washed off on the fourth day; treatment may be repeated if necessary after one week.
Oral Medications
Oral ivermectin is a systemic medication that can treat scabies when taken by mouth. The standard dose is 200 micrograms per kilogram of body weight, and it is typically repeated after 14 days. Ivermectin is particularly useful for outbreaks in institutional settings, cases of crusted scabies, or when topical treatment has failed. Oral treatment is often preferred for individuals who have difficulty applying topical creams or for those with widespread infestation.
Treatment of Crusted Scabies
Crusted scabies requires aggressive combination therapy that may include permethrin cream, oral ivermectin, and keratolytic agents (medications that soften and remove dead skin) to penetrate the thick crusted plaques and ensure adequate mite penetration. This variant often requires longer treatment courses and closer medical supervision.
Treating Contacts and the Environment
Because scabies is so contagious, healthcare providers typically recommend treating the entire family and any close contacts of an infected person, even if they do not yet show symptoms. This prevents reinfection of the primary patient and stops continued transmission in the household or facility.
Bedding, clothing, and other items that have had contact with the affected person should be washed in hot water and dried in a hot dryer. Items that cannot be washed can be sealed in a plastic bag for at least 72 hours, as the mite cannot survive long away from human skin.
Prevention of Scabies
Preventing scabies involves reducing your risk of exposure to the mite:
- Avoid prolonged skin-to-skin contact with individuals known to have scabies until they have been treated.
- Maintain good personal hygiene, though note that scabies is not caused by poor hygiene.
- Educate household members and close contacts about the signs and symptoms of scabies so they can seek prompt treatment if symptoms develop.
- In institutional settings, implement infection control measures and prompt isolation protocols for confirmed cases.
- Avoid sharing personal items such as towels, bedding, or clothing with individuals who have scabies.
- Seek prompt treatment if you develop symptoms, to reduce transmission to others.
Frequently Asked Questions
Q: How long does it take for scabies symptoms to appear after exposure?
A: In a primary infection, symptoms typically develop 4 to 6 weeks after exposure to the mite. However, if you have had scabies before, symptoms can appear within hours to days due to your body’s pre-existing sensitivity to mite antigens.
Q: Can scabies be cured?
A: Yes, scabies can be effectively cured with prescription medications such as permethrin cream or oral ivermectin. Most cases resolve completely with appropriate treatment.
Q: Is scabies contagious after treatment begins?
A: The infectiousness of scabies decreases rapidly after treatment begins. However, it is advisable to avoid close contact until at least the day after treatment is completed to minimize any remaining transmission risk.
Q: Can pets transmit scabies to humans?
A: Scabies mites are species-specific. The mite that causes scabies in humans (Sarcoptes scabiei var. hominis) does not typically infest animals. Animal scabies is caused by a different mite variant and does not spread to humans.
Q: What should I do if someone in my household has scabies?
A: If someone in your household has scabies, it is important to seek medical evaluation and treatment for all household members, even if they do not yet have symptoms. Wash all bedding, clothing, and towels in hot water and dry them on high heat. Seal items that cannot be washed in a plastic bag for at least 72 hours.
Q: Can scabies recur after successful treatment?
A: Scabies can recur if you are exposed to an infected person after successful treatment. However, your body will not develop immunity to reinfection, so you can contract scabies again at any point.
Q: Are there any long-term effects of scabies?
A: In most cases, scabies resolves completely with appropriate treatment and leaves no long-term effects. However, secondary bacterial infections from scratching can lead to scarring if severe. The itching sensation may persist for a few weeks after treatment as the immune reaction gradually subsides.
References
- Scabies — Iowa Department of Health and Human Services. 2024. https://hhs.iowa.gov/health-prevention/providers-professionals/center-acute-disease-epidemiology/epi-manual/information-other-diseases-and-conditions-fact-sheets/scabies
- Scabies Fact Sheet — Texas Department of State Health Services. 2024. https://www.dshs.texas.gov/sites/default/files/region1/documents/Scables-Fact-Sheet.pdf
- Scabies: Causes, Symptoms, Treatment & Prevention — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/4567-scabies
- Scabies — StatPearls, National Center for Biotechnology Information, U.S. National Library of Medicine. 2025. https://www.ncbi.nlm.nih.gov/books/NBK544306/
- Scabies – Dermatologic Disorders — Merck Manual Professional Edition. 2024. https://www.merckmanuals.com/professional/dermatologic-disorders/parasitic-skin-infections/scabies
- Scabies – Symptoms and Causes — Mayo Clinic. 2024. https://www.mayoclinic.org/diseases-conditions/scabies/symptoms-causes/syc-20377378
- Scabies: Diagnosis and Treatment with Images — DermNet. 2024. https://dermnetnz.org/topics/scabies
Read full bio of Sneha Tete











