Scalp Psoriasis: Symptoms, Causes, and Treatment Options
Complete guide to understanding and managing scalp psoriasis effectively.
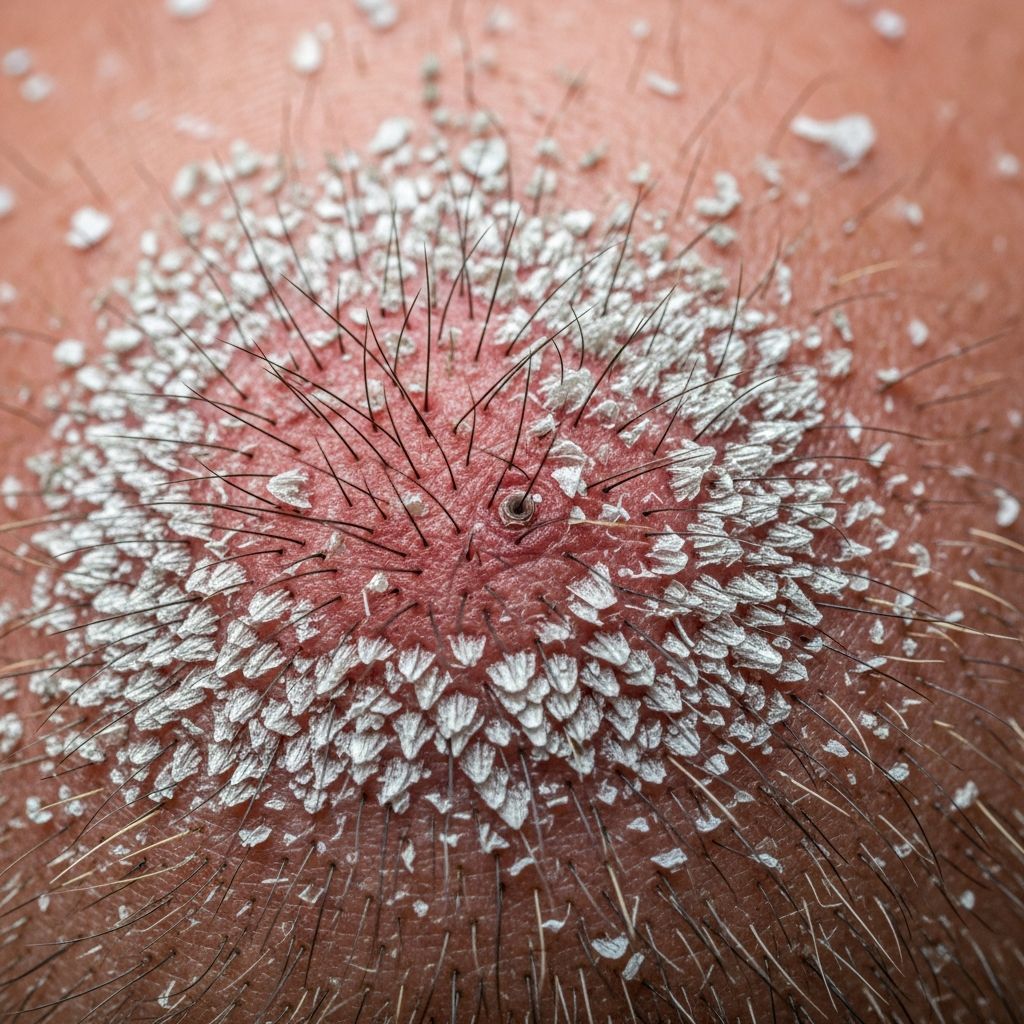
Understanding Scalp Psoriasis
Scalp psoriasis is a chronic autoimmune skin condition that specifically affects the scalp area. It occurs when the immune system mistakenly attacks healthy skin cells, causing them to build up rapidly on the scalp. This results in thick, scaly patches that can be uncomfortable, itchy, and sometimes painful. Unlike other scalp conditions like dandruff or seborrheic dermatitis, scalp psoriasis is a lifelong condition that requires ongoing management and care.
The condition affects a significant portion of the population with psoriasis. Approximately 45-56% of individuals diagnosed with psoriasis experience scalp involvement at some point in their lives. The scalp is often one of the first areas affected by psoriasis, and the frequency of lesion formation typically increases as the disease progresses over time. This makes early recognition and treatment particularly important for managing symptoms effectively.
What Are the Symptoms of Scalp Psoriasis?
Scalp psoriasis presents with several distinctive symptoms that can vary in severity from person to person. Understanding these symptoms helps individuals identify the condition and seek appropriate medical attention.
Common Symptoms Include:
- Silvery-white or gray scales on the scalp
- Intense itching that may worsen at night
- Red or inflamed patches of skin
- Dry scalp that may crack and bleed
- Soreness or tenderness in affected areas
- Hair loss due to scratching or inflammation
- Flaking and scaling visible in hair or on clothing
- Burning sensation on the scalp
The symptoms can significantly impact quality of life. Many individuals experience pain, itching, bleeding, and feelings of embarrassment about their appearance. The condition can restrict clothing choices and lead to social discomfort. Interestingly, the quality of life impact differs between demographics, with women experiencing more adverse effects than men, and individuals younger than 40 years reporting greater negative impacts compared to patients aged 60 years or older.
Causes and Risk Factors
Scalp psoriasis is an autoimmune condition, meaning the body’s immune system attacks its own healthy skin cells. While the exact trigger isn’t fully understood, several factors can increase the likelihood of developing scalp psoriasis or triggering flare-ups.
Primary Risk Factors:
- Genetic predisposition and family history
- Immune system dysfunction
- Stress and emotional tension
- Infections, particularly streptococcal infections
- Certain medications that may trigger or worsen symptoms
- Injury or trauma to the scalp (known as the Köbner phenomenon)
- Hormonal changes
- Cold, dry weather conditions
- Smoking and alcohol consumption
The condition typically begins as small, red patches that gradually become covered with silvery scales. The lesions on the scalp are usually asymmetrical and sharply demarcated, distinguishing them from other scalp disorders. Understanding these risk factors can help individuals take preventive measures and identify potential triggers for their specific condition.
Diagnosis of Scalp Psoriasis
Diagnosing scalp psoriasis can sometimes be challenging because it shares features with other scalp conditions. The most common condition causing diagnostic confusion is seborrheic dermatitis, which also causes scaling and itching. However, dermatologists use specific characteristics to differentiate scalp psoriasis from other conditions.
Diagnostic Characteristics:
- Sharply demarcated lesion boundaries
- Silvery-white scaling patterns
- Asymmetrical distribution across the scalp
- Persistent symptoms despite anti-dandruff treatments
- Associated symptoms in other body areas
- Family history of psoriasis
Your healthcare provider will typically perform a visual examination of your scalp and may ask about your medical history and any family history of psoriasis. In some cases, a small skin biopsy may be taken to confirm the diagnosis. If you notice white or gray scales on your scalp and over-the-counter anti-dandruff shampoo isn’t working, it’s important to see your healthcare provider for proper evaluation and diagnosis.
Treatment Options for Scalp Psoriasis
While there is no cure for scalp psoriasis, numerous treatment options can effectively manage symptoms and reduce the appearance of plaques. Treatment choice depends on the severity of the condition, individual patient response, and personal preferences. Many patients find success with a combination approach.
Topical Treatments
Topical therapies are typically the first line of treatment for scalp psoriasis. These treatments are applied directly to the affected areas and work locally to reduce inflammation and scale formation.
Corticosteroids
Topical corticosteroids are among the most commonly prescribed treatments for scalp psoriasis. They work by reducing inflammation and suppressing immune activity in the affected skin. Corticosteroid monotherapy has been shown to be effective, particularly for short-term management. These medications come in various strengths and formulations including creams, lotions, foams, and solutions that can be applied to the scalp.
Vitamin D Analogs
Vitamin D analogs like calcipotriol help regulate skin cell growth and reduce inflammation. When combined with hydrocortisone, vitamin D analogs show enhanced effectiveness compared to vitamin D monotherapy alone. However, research indicates that corticosteroid monotherapy may be acceptable for short-term use due to the minimal additional benefit of combination therapy.
Coal Tar and Salicylic Acid
Coal tar products have been used for decades to treat psoriasis and help soften scales on the scalp. Salicylic acid works by breaking down the scale buildup, which consists primarily of dead skin cells. These can be found in medicated shampoos and are often available over-the-counter, making them accessible treatment options for many patients.
Keratolytic and Tar-Based Shampoos
Specialized shampoos containing keratolytic agents and tar help loosen scales and reduce itching. These products soften the scale buildup, allowing it to be gently removed without forceful scratching that could worsen the condition or cause hair loss. Regular use of these shampoos, combined with other topical therapies, may be sufficient for mild to moderate scalp psoriasis.
Phototherapy
For patients who don’t respond adequately to topical treatments, phototherapy offers an effective alternative. Targeted phototherapy using an excimer laser can provide significant relief when used with a blower device that displaces hair to allow the laser to reach affected scalp areas. This treatment requires multiple sessions but can be particularly helpful for stubborn plaques.
Systemic Medications
For moderate to severe scalp psoriasis, systemic medications that work throughout the body may be prescribed. These are particularly important when scalp involvement is severe but body surface area involvement is minimal, as the patient might not otherwise qualify for systemic therapy.
Biologic Therapies
Biologic medications represent a significant advancement in psoriasis treatment. Secukinumab, a biologic therapy, demonstrated superiority over placebo in clinical trials specifically conducted in patients with moderate-to-severe scalp psoriasis. These medications work by targeting specific parts of the immune system that drive psoriasis development.
Other Systemic Options
For more difficult cases, healthcare providers may prescribe oral medications or injectable treatments that target psoriasis throughout the body, not only on the scalp but also on other affected areas, nails, and joints.
Steroid Injections
In some cases, steroid injections directly into problem areas of the scalp can provide targeted relief. This option is available for patients whose scalp psoriasis remains stubborn despite other treatments.
Management Tips and Self-Care Strategies
Effective management of scalp psoriasis involves both professional treatment and daily self-care practices. These strategies can significantly reduce symptoms and prevent worsening of the condition.
Do’s and Don’ts:
- Avoid scratching or picking at scales, as this can trigger the Köbner phenomenon and worsen symptoms
- If you must relieve itching, gently rub the area with the soft part of your fingers rather than scratching
- Use medicated shampoos as directed by your healthcare provider
- Avoid blow-drying your hair or use low heat settings to prevent additional scalp irritation
- Keep your scalp moisturized with appropriate products
- Manage stress through relaxation techniques, as stress can trigger flare-ups
- Avoid harsh hair products and treatments
- Limit hot water exposure when washing your hair
- Protect your scalp from injury whenever possible
When scratching or aggressive scale removal occurs, it can cause hair to break and worsen scalp psoriasis. This is why gentle management is crucial. As inflammation improves with proper treatment, hair typically regrows naturally.
Scalp Psoriasis and Hair Loss
One significant concern for many patients with scalp psoriasis is hair loss. The condition can cause temporary hair loss through several mechanisms, but the good news is that hair typically regrows once the psoriasis is controlled.
Hair loss occurs because the inflammation weakens hair follicles, making them brittle and prone to breakage. Additionally, the strong urge to scratch the itchy scalp can cause mechanical damage to hair. However, if scalp psoriasis is adequately treated and controlled, hair loss is usually temporary.
The only scenarios where hair might not regrow are if chronic, severe scalp psoriasis remained untreated for extended periods or if aggressive scratching caused scarring of the scalp tissue. In most cases, once the inflammatory condition is calmed down with proper treatment, hair regrowth occurs naturally.
Treatment Challenges and Solutions
Despite the availability of effective treatments, patients with scalp psoriasis often face unique challenges that can affect treatment adherence and satisfaction.
Common Challenges:
- Hair makes application of topical treatments burdensome and time-consuming
- Many patients find topical treatments cosmetically unacceptable, leaving residue or visible product
- Difficulty accessing the scalp makes thorough treatment application challenging
- Poor treatment compliance due to inconvenience or dissatisfaction
- Topical treatments can stain hair or clothing
- Some formulations have unpleasant odors
These challenges can lead to medication nonadherence, reducing treatment effectiveness. Healthcare providers work with patients to find solutions that fit their lifestyle and preferences, whether through alternative formulations, systemic medications, or combination therapies that maximize both efficacy and tolerability.
When to Seek Professional Help
Recognizing when to consult a healthcare provider is important for optimal management. You should see a dermatologist if:
- You experience a consistently itchy scalp for extended periods
- You notice white or gray scales on your scalp
- Over-the-counter anti-dandruff shampoos haven’t resolved your symptoms
- You experience pain, bleeding, or significant discomfort
- Your scalp condition is affecting your quality of life or emotional well-being
- You’re experiencing noticeable hair loss
- Your symptoms worsen despite home treatment attempts
Early intervention often leads to better outcomes and prevents progression to more severe disease.
Frequently Asked Questions About Scalp Psoriasis
Q: Is scalp psoriasis contagious?
A: No, scalp psoriasis is not contagious. It is an autoimmune condition that cannot be transmitted through contact with an affected person. However, genetic predisposition can run in families.
Q: Can scalp psoriasis spread to other parts of my body?
A: Scalp psoriasis is localized to the scalp, but individuals with scalp psoriasis may develop psoriasis in other body areas as a separate manifestation of the disease. The condition affects about 45-56% of people with psoriasis.
Q: How long does it take for treatments to work?
A: Treatment timelines vary depending on the type of therapy used. Topical treatments may show improvement within 2-4 weeks, while biologic therapies may take 8-12 weeks to demonstrate full effectiveness.
Q: Will my scalp psoriasis ever go away completely?
A: Scalp psoriasis is a chronic condition that currently has no permanent cure. However, with proper treatment and management, symptoms can be significantly controlled or even enter remission periods.
Q: Can I use regular hair products with scalp psoriasis?
A: You should avoid harsh hair products that may irritate your scalp. Consult with your healthcare provider about which products are safe to use alongside your psoriasis treatment.
Q: What should I do if my current treatment isn’t working?
A: If your treatment isn’t providing adequate relief after several weeks, contact your healthcare provider. They can adjust your current treatment plan, try alternative therapies, or recommend additional interventions like phototherapy or systemic medications.
References
- Underdiagnosed and undertreated psoriasis — National Center for Biotechnology Information (NCBI). 2019. https://pmc.ncbi.nlm.nih.gov/articles/PMC6901032/
- Psoriasis Hair Loss: How To Treat and Reduce — Cleveland Clinic. 2024. https://health.clevelandclinic.org/scalp-psoriasis-and-hair-loss
- Plaque Psoriasis: What It Looks Like, Causes & Treatment — Cleveland Clinic. 2022. https://my.clevelandclinic.org/health/diseases/22842-plaque-psoriasis
- Psoriasis: A clinical update on diagnosis and new therapies — Cleveland Clinic Journal of Medicine. https://www.ccjm.org/content/ccjom/67/2/105.full.pdf
- Psoriasis: What It Is, Symptoms, Causes, Types & Treatment — Cleveland Clinic. https://my.clevelandclinic.org/health/diseases/6866-psoriasis
Read full bio of medha deb











