School Sores (Impetigo): Symptoms, Treatment, Prevention Guide
Comprehensive insights into preventing, recognizing, and treating school sores in children and adults.
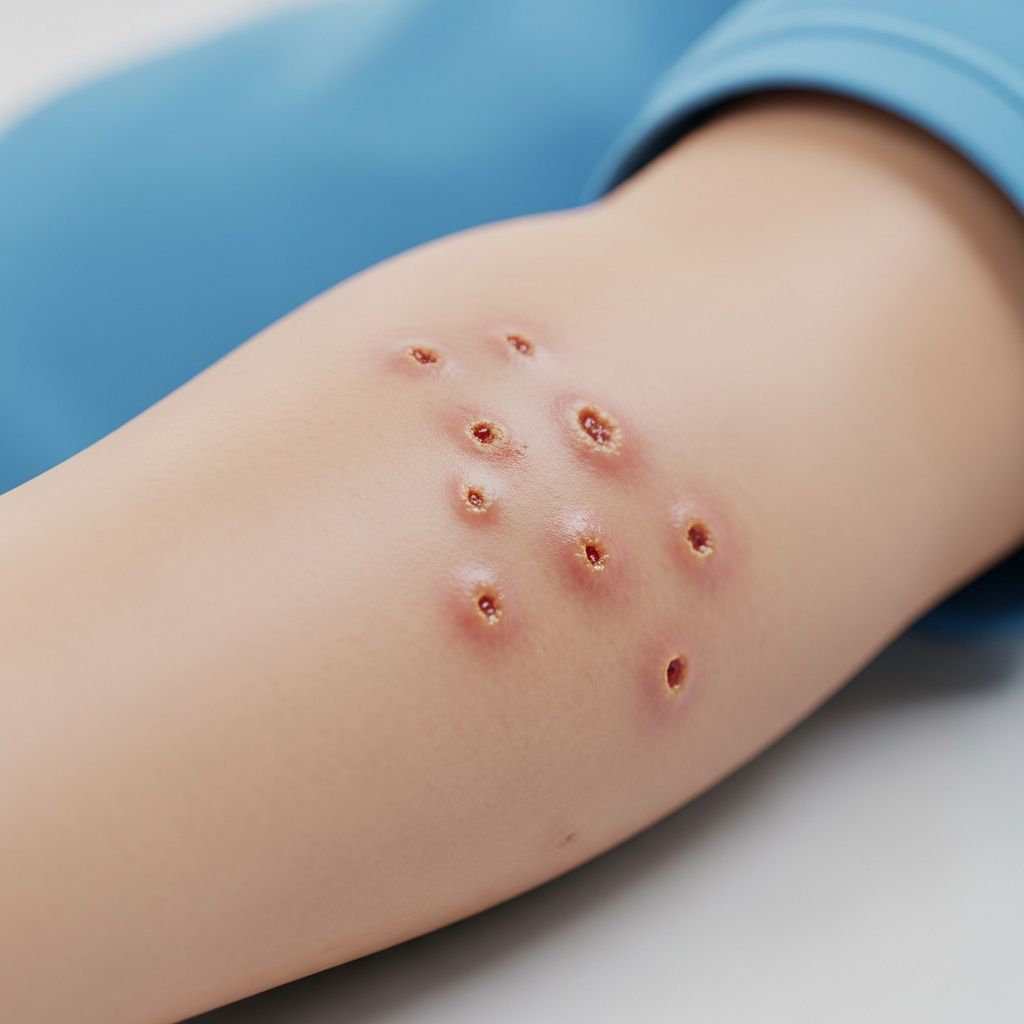
School sores, commonly referred to as impetigo, represent one of the most frequent bacterial skin infections, particularly among young children. This highly contagious condition manifests as itchy, crusty lesions on the skin, often thriving in environments like schools and playgrounds where close contact is inevitable. Prompt recognition and intervention are crucial to curb its spread and ensure quick recovery.
Recognizing the Signs of School Sores
Early identification of school sores can prevent widespread transmission. The infection typically begins with small red spots or pimples that evolve into fluid-filled blisters. These blisters rupture easily, releasing a clear or yellowish fluid that dries into distinctive honey-colored crusts. Common locations include the face, particularly around the nose and mouth, as well as the arms and legs—areas prone to minor injuries or exposure.
- Initial red pimples or bumps on the skin
- Blisters containing fluid that burst open
- Itchy, oozing rash forming yellow or golden scabs
- Larger patches greater than 1 cm in some cases
Symptoms usually appear 4 to 10 days after exposure to the bacteria. While generally mild, the sores can cause discomfort and itchiness, leading children to scratch and inadvertently spread the infection further.
Root Causes Behind This Common Infection
At its core, school sores stem from bacteria such as Staphylococcus aureus (staph) or Streptococcus pyogenes (strep), which are normal residents on the skin or in the nose but become problematic when they invade through breaks in the skin barrier. Minor cuts, scrapes, insect bites, or conditions like eczema provide entry points. In warmer months, the risk heightens due to increased sweating and skin abrasions from outdoor play.
These bacteria flourish in crowded settings, explaining the nickname “school sores.” Transmission occurs directly via touch or indirectly through shared items like towels, toys, or clothing contaminated with sore fluid. Healthy skin can sometimes be affected, but vulnerability rises with dry, cracked, or irritated surfaces.
Effective Treatment Strategies for Quick Relief
Treatment focuses on eliminating the bacteria and promoting healing while minimizing contagion. For mild cases with few sores, topical antibiotic ointments applied directly to the lesions suffice. More extensive or persistent infections require oral antibiotics in tablet, liquid, or syrup form, prescribed by a healthcare provider.
Healthcare professionals diagnose impetigo through visual examination, rarely needing lab swabs unless complications arise. Complete the full antibiotic course, even if sores improve, to prevent recurrence or resistance.
Home Care Routine
Support medical treatment with diligent daily care:
- Gently wash sores with soap and warm water every 8-12 hours to remove crusts.
- Soak crusts with a warm, soapy compress until soft, then wipe away gently.
- Pat dry with a clean towel and apply prescribed antibiotic ointment.
- Cover with loose, breathable bandages or waterproof dressings, especially on exposed areas.
- Wash hands thoroughly after care and avoid sharing towels.
Monitor progress; sores should begin healing within 3 days. Seek further advice if they worsen, spread, or if fever develops.
Prevention Tactics for Families and Schools
Proactive measures significantly reduce impetigo incidence. Encourage good hygiene: regular handwashing with soap, keeping nails short to deter scratching, and promptly cleaning minor wounds with antiseptic. In schools, exclude affected children until 24-48 hours after starting antibiotics or until sores dry and crusts heal.
| Prevention Step | Why It Works | Best For |
|---|---|---|
| Frequent handwashing | Removes bacteria before entry | Children and caregivers |
| Cover cuts promptly | Blocks bacterial invasion | Playgrounds and sports |
| Don’t share personal items | Prevents indirect spread | Schools and homes |
| Daily showers | Cleans skin of sweat/bacteria | Warm weather months |
| Moisturize dry skin | Maintains skin barrier | Eczema-prone kids |
These habits, combined with awareness, form a robust defense.
Potential Complications and When to Worry
Though rarely severe, untreated impetigo can lead to cellulitis (deeper skin infection), abscesses, or post-streptococcal glomerulonephritis affecting kidneys. Newborns and immunocompromised individuals face higher risks, making isolation from infants essential. Watch for spreading redness, pus, pain, or systemic symptoms like fever.
Adults in close quarters, such as military barracks, may also contract it, often linked to weakened immunity or skin trauma.
School and Childcare Policies
Educational settings play a pivotal role. Policies typically mandate staying home until non-contagious: 24 hours post-antibiotic initiation or when sores are crusted and dry. Notify parents, disinfect surfaces, and educate on hygiene to contain outbreaks.
FAQs on School Sores
Q: How long is someone contagious with school sores?
A: As long as sores ooze fluid; usually until 24-48 hours after antibiotics start.
Q: Can adults get impetigo?
A: Yes, though less common, especially in crowded or immune-suppressed conditions.
Q: Is over-the-counter ointment enough?
A: For very mild cases, but consult a doctor for prescription strength to ensure effectiveness.
Q: Does impetigo leave scars?
A: Rarely, if properly treated; keep children from picking scabs.
Q: What’s the difference between impetigo types?
A: Non-bullous (crusty sores) is most common; bullous features larger blisters from staph toxins.
Long-Term Skin Health Tips
Beyond acute management, foster resilient skin through moisturizing, sun protection, and treating underlying issues like allergies. Nutrition rich in vitamins A and C supports immunity and healing. Regular pediatric check-ups catch vulnerabilities early.
Empowering parents with knowledge transforms school sores from a dreaded outbreak into a manageable blip. Vigilance in hygiene and swift treatment keep communities healthy.
References
- Find Treatment for School Sores or Impetigo — Goshen Health. 2023. https://goshenhealth.com/services-conditions/impetigo
- School sores (impetigo) – Symptoms, treatment, prevention — SA Health (Government of South Australia). 2024-01-15. https://www.sahealth.sa.gov.au/wps/wcm/connect/public+content/sa+health+internet/conditions/infectious+diseases/school+sores/school+sores+impetigo+-+including+symptoms+treatment+and+prevention
- Impetigo – treatments, symptoms and causes — healthdirect (Australian Government). 2024. https://www.healthdirect.gov.au/impetigo
- Impetigo – school sores — Better Health Channel (State of Victoria). 2023-06-20. https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/impetigo-school-sores
- Kids Health Info: Impetigo (school sores) — Royal Children’s Hospital Melbourne. 2024. https://www.rch.org.au/kidsinfo/fact_sheets/impetigo_school_sores/
- Impetigo: Symptoms, Complications, Treatment — Centers for Disease Control and Prevention (CDC). 2024-10-01. https://www.cdc.gov/group-a-strep/about/impetigo.html
- Impetigo — Texas Department of State Health Services. 2023. https://www.dshs.texas.gov/impetigo
Read full bio of medha deb













