Segmental Pigmentation Disorder: What You Need To Know
Understanding segmental pigmentation disorder: unilateral hypo- or hyperpigmented patches on the torso without systemic issues.
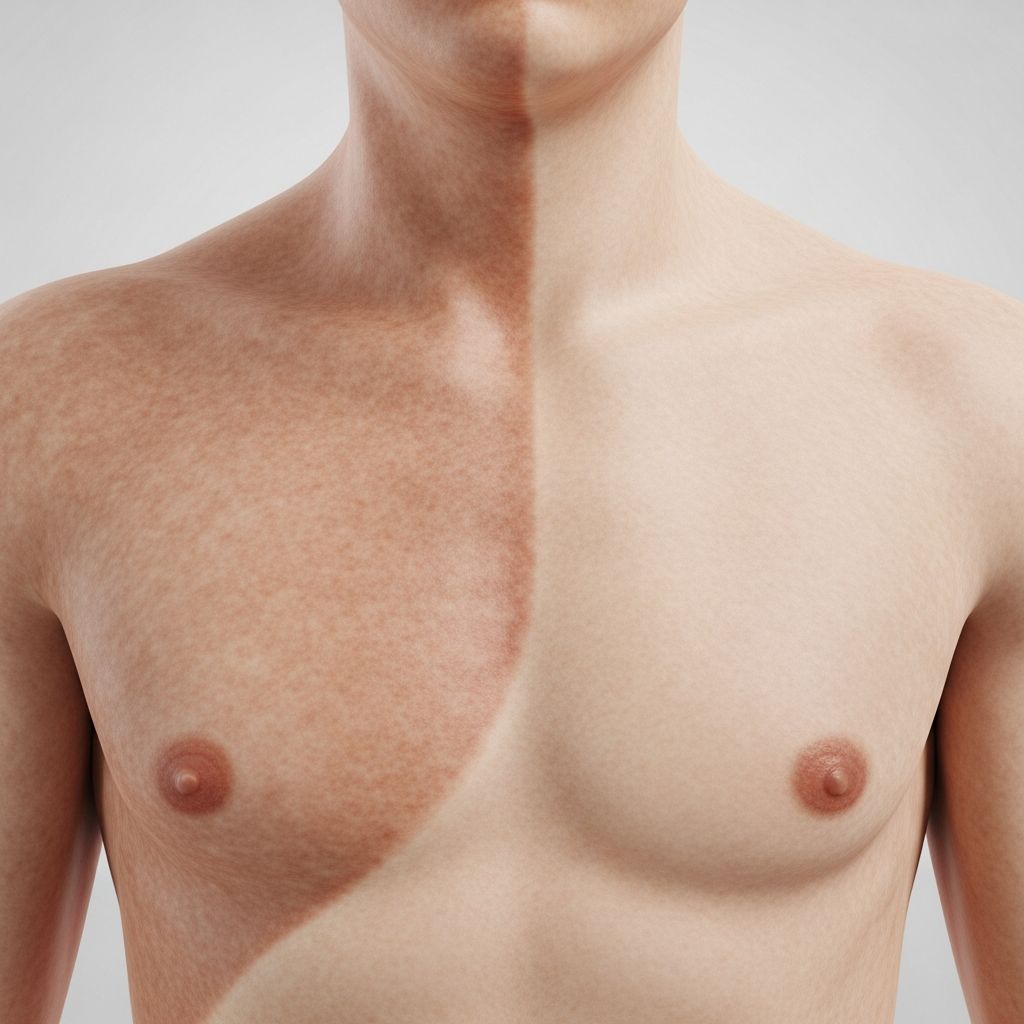
Segmental Pigmentation Disorder
Segmental pigmentation disorder (SegPD) refers to a subset of localised cutaneous pigmentary anomalies without systemic manifestations. It is characterised by unilateral hypo- or hyperpigmented patches, predominantly on the frontal torso with a sharp midline delineation.
Introduction
Segmental pigmentation disorder, often abbreviated as SegPD, represents a distinct pigmentary condition observed primarily in infants and young children. First proposed as a specific entity in 1983, it has been documented under various names including segmental pigmentation anomaly, patterned dyspigmentation, and pigmentary mosaicism. The revival of the term ‘segmental pigmentation disorder’ in 2010 aimed to clarify its nosological position, distinguishing it from other mosaic-patterned pigmentation disorders associated with neural, ocular, or cardiac issues, thereby reducing parental anxiety.
SegPD typically manifests as hypo- or hyperpigmented patches following a segmental distribution, most commonly on the torso. These lesions are usually evident from birth or early infancy, with a sharp border along the ventral midline. Unlike more complex pigmentary disorders, SegPD lacks extracutaneous abnormalities, making it a benign condition.
Demographics
SegPD affects both genders equally, with studies reporting similar numbers of males and females. In one cohort of 39 patients, there were 20 females and 19 males. Another larger series from Israel involving paediatric dermatology centres confirmed no significant gender bias.
The condition is more prominent in darker-skinned individuals. Research indicates that cutaneous findings are especially noticeable in children with Fitzpatrick skin types IV-VI, where contrast between normal and affected skin is heightened. Age of onset is typically very early; the mean age is around 3.4 months, with a median of 0.25 months, often present at birth.
Family history is rare, positive in only about 5% of cases, such as siblings or parents affected. Prevalence data suggest it is relatively common in paediatric dermatology clinics, though exact population figures are lacking due to underreporting of benign lesions.
Causes
The precise aetiology of SegPD remains unknown. Several mechanisms have been proposed, including neural and hormonal factors influencing melanocytes (pigment-producing cells), postzygotic somatic mosaicism, and cellular chimerism.
Somatic mosaicism, where genetic mutations occur after zygote formation, leads to clones of cells with altered pigmentation potential, explaining the segmental pattern. Both melanocytes and neural crest cells derive from the ectoderm, but SegPD shows no neurological links, suggesting an embryological disruption in pigment migration postnatally without broader congenital defects.
Skin pigmentation develops mediolaterally and respects the linea alba (ventral midline), accounting for the sharp midline demarcation. Lesions rarely cross this line by more than a few centimetres. Hyperpigmented lesions exhibit increased melanin in the basal layer due to heightened production, akin to café-au-lait macules, while hypopigmented ones have reduced melanin with normal or decreased melanocyte numbers.
Clinical Features
Clinically, SegPD presents as unilateral patches of hypo- or hyperpigmentation in a segmental, dermatomal, or chequerboard pattern. The torso is most affected (77-86% of cases), particularly the frontal aspect (chest and abdomen), with extension to face, neck, arms, or legs in some instances.
- Distribution: Frontal torso predominant (61-77%), dorsal less common; face-only in ~15%.
- Type: Hyperpigmentation in 77% in one study, hypopigmentation in 23%; another found 52% hypopigmented.
- Borders: Sharp ventral midline (82%), blurred lateral; well- or ill-defined edges nearly equal.
- Number: Usually few patches, stable in size (41-55%) and intensity (55%).
Lesions are often noticed at birth or infancy, with hyperpigmented patches tending to fade over time, though some persist into adulthood. Additional cutaneous findings occur in 95% of cases, but none are specific.
Variation in Skin Types
SegPD manifestations vary by skin phototype. In lighter skin (Fitzpatrick I-III), hyperpigmented lesions may be subtle, while hypopigmentation stands out less. Conversely, in darker skin (IV-VI), both types are strikingly visible due to high contrast, leading to more frequent referrals.
Studies confirm prominence in darker-skinned children, aligning with initial descriptions. This variation underscores the importance of considering ethnicity in clinical recognition; for instance, what appears as a faint patch in pale skin may be diagnostic in olive or brown tones.
Complications
SegPD is primarily cosmetic with no functional complications. Unlike associated mosaic disorders, it lacks systemic issues; only rare, uncertain extracutaneous findings like atrial septal defect, strabismus, or cysts reported in <8%.
No neurological abnormalities are linked, distinguishing it from conditions like hypomelanosis of Ito. Psychosocial impact may arise from visible lesions, especially in darker skin, but reassurance of benignity alleviates concerns.
Diagnosis
Diagnosis is clinical, based on history (early onset, segmental pattern, sharp midline) and examination. No routine investigations needed; Wood’s lamp may highlight hypopigmentation.
Biopsy, if performed, shows non-specific changes: reduced melanin/melanocytes in hypopigmented areas, increased basal melanin in hyperpigmented. Genetic testing unnecessary absent systemic signs.
Differential Diagnoses
Accurate differentiation prevents unnecessary workup.
Segmental Hypopigmentation
- Naevus depigmentosus: Present at birth, stable, feather-like borders.
- Postinflammatory hypopigmentation: History of inflammation, evolves.
- Piebaldism: Leukoderma with poliosis, family history.
- Vitiligo: Progressive, depigmented, autoimmune markers.
- Hypomelanosis of Ito: Widespread, systemic associations.
Segmental Hyperpigmentation
- Café-au-lait macule: Uniform, smooth borders, multiple may suggest NF1.
- McCune-Albright syndrome: Fibrous dysplasia, endocrine issues.
- Linear and whorled nevoid hypermelanosis: Velvety, follows Blaschko lines.
- Postinflammatory hyperpigmentation: Trauma history.
- Pigmentary mosaicism types: With potential systemic risks.
| Condition | Pattern | Onset | Systemic? |
|---|---|---|---|
| SegPD | Segmental, midline sharp | Infancy | No |
| Naevus depigmentosus | Feathered | Birth | No |
| Café-au-lait | Oval | Early | Possible (NF1) |
| Vitiligo | Confetti-like | Any | Autoimmune |
Treatment
SegPD requires no treatment as it is asymptomatic and stable. Cosmetic camouflage for visible lesions if distressing. Sun protection advised to prevent contrast accentuation.
Unlike other pigment disorders, topicals (hydroquinone, retinoids) or lasers unnecessary and potentially risky. Reassurance key.
Outcome
Lesions remain stable, hyperpigmented ones often fade. No progression or malignant risk. Long-term follow-up unneeded absent new symptoms, easing family burden.
Frequently Asked Questions (FAQs)
Q: Is segmental pigmentation disorder dangerous?
A: No, it is a benign skin condition without systemic associations.
Q: Does it go away?
A: Hyperpigmented patches may fade; hypopigmented stable or subtle over time.
Q: Is treatment needed?
A: Generally no; cosmetic options if desired.
Q: Can it affect my child neurologically?
A: No evidence links SegPD to neurological issues.
Q: Is it hereditary?
A: Rarely familial; mostly sporadic.
References
- Segmental pigmentation disorder — British Journal of Dermatology. 2010-06-01. https://academic.oup.com/bjd/article-abstract/162/6/1337/6642868
- Segmental Pigmentation Disorder: Clinical Manifestations and … — PMC / NCBI. 2022-10-19. https://pmc.ncbi.nlm.nih.gov/articles/PMC9631269/
- Segmental Pigmentation Disorder – DermNet — DermNet NZ. 2023. https://dermnetnz.org/topics/segmental-pigmentation-disorder
- Pigmentation Disorders: Diagnosis and Management – AAFP — American Academy of Family Physicians. 2017-12-15. https://www.aafp.org/pubs/afp/issues/2017/1215/p797.html
- Segmental pigmentation disorder image – DermNet — DermNet NZ. 2023. https://dermnetnz.org/imagedetail/2811-segmental-pigmentation-disorder
Read full bio of Sneha Tete