Shin Splints: Causes, Symptoms, and Treatment
Complete guide to understanding shin splints, their causes, symptoms, and effective treatment options.
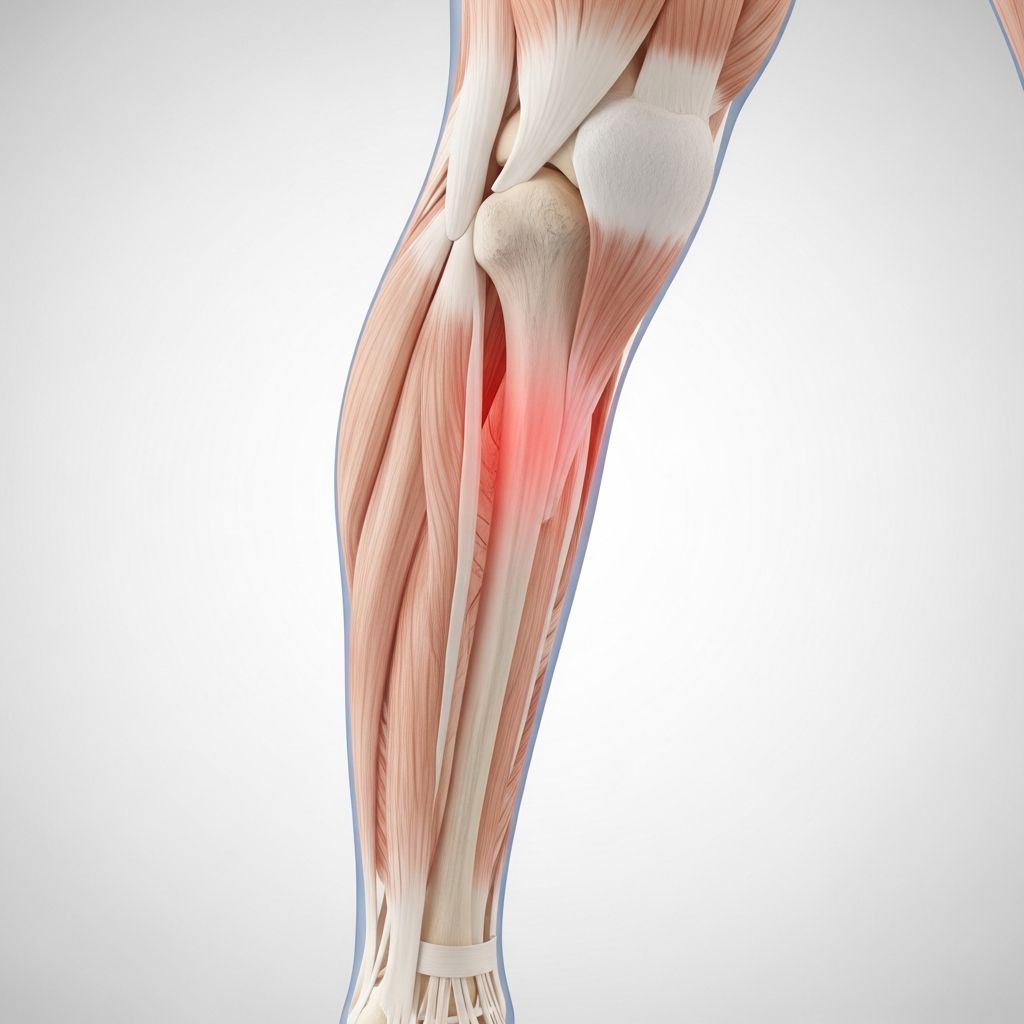
What Are Shin Splints?
Shin splints, medically known as medial tibial stress syndrome (MTSS), are a common exercise-related condition that causes pain and inflammation in the lower leg. The condition involves stress and inflammation affecting the shin bone (tibia), the muscles surrounding it, and the connective tissues in the lower leg. This painful condition typically develops along the inner edge of the shinbone and is one of the most prevalent causes of lower leg pain related to physical activity.
The tibia, or shinbone, is the long bone located at the front of your lower leg that extends from your knee to your ankle. When repetitive stress and strain are placed on this bone and the surrounding muscle and tendon tissues, inflammation can develop, leading to the characteristic pain associated with shin splints. The condition is particularly common among athletes, runners, dancers, and military recruits who engage in repetitive impact activities.
Understanding the Different Types of Shin Splints
Shin splints are classified into two main types depending on which area and muscles of the shin are affected:
Medial Tibial Stress Syndrome (MTSS)
MTSS is the most common type of shin splints, accounting for the majority of cases. This type causes pain specifically along the inner edge of the shinbone. The pain results from inflammation in the muscles, tendons, and bone tissue around the tibia. The inflammation occurs in the tissues that run along the medial, or inner, border of the shin bone.
Anterior Tibial Stress Syndrome
This less common type of shin splints causes pain along the front of the lower leg. Anterior tibial stress syndrome is often related to the muscles attached to the front of the tibia and typically results from overuse of these specific muscle groups during repetitive activities.
Causes and Risk Factors of Shin Splints
Shin splints develop when the muscle and bone tissue in the leg become overworked by repetitive activity. Understanding the causes and risk factors is essential for both prevention and management of this condition.
Common Causes
The primary cause of shin splints is repetitive stress and strain on the muscles, tendons, and bone tissue around the shinbone. This stress typically occurs due to:
- Sudden increases in the amount or intensity of exercise
- Repeated impact, particularly in high-impact activities such as running, jumping, or sports involving sudden starts and stops
- Biomechanical issues including flat feet, excessive pronation (inward rolling of the foot), and differences in leg length
- Weak or tight muscles in the calves, hips, or core
- Running on uneven or hard surfaces without proper support
- Using unsupportive, improperly fitting, or worn-out shoes during exercise
Risk Factors
Certain individuals are at higher risk for developing shin splints. Runners have the highest risk of developing the condition, though dancers and military recruits are also frequently diagnosed. Additional risk factors include having flat feet or abnormally rigid arches, exercising with improper footwear, and rapidly increasing exercise intensity or duration.
Recognizing the Symptoms of Shin Splints
The primary symptom of shin splints is pain along the inner edge of the tibia, though the specific characteristics of this pain can vary among individuals. Recognizing these symptoms early allows for prompt intervention and treatment.
Primary Symptoms
- Pain along the border of the tibia that may be sharp and razor-like or dull and throbbing
- Pain that occurs during and after exercise
- Mild swelling in the lower leg area
- Discomfort that is aggravated by touching the affected area
- Possible weakness or numbness in the lower leg
The pain may start gradually and worsen over time if the condition remains untreated. Some individuals experience pain only after exercise, while others may feel discomfort during physical activity as well. The severity of symptoms can range from mild to debilitating, depending on the extent of the inflammation and stress on the bone and surrounding tissues.
Diagnosis of Shin Splints
Diagnosing shin splints typically involves a combination of clinical evaluation and imaging studies. Healthcare providers will take a detailed medical history, perform a physical examination of the affected area, and may order imaging tests if necessary. The diagnosis is usually straightforward based on the location of pain and the patient’s activity history, particularly when pain occurs along the inner edge of the shinbone after repetitive impact activities.
During the physical examination, a healthcare provider will assess the painful area, check for swelling, and evaluate your gait and leg alignment. In some cases, X-rays or other imaging may be used to rule out stress fractures or other conditions that cause similar symptoms. MRI or ultrasound imaging may be recommended to evaluate the soft tissues and assess the degree of inflammation.
Treatment Options for Shin Splints
Treatment for shin splints typically includes self-care methods, medicines, and physical therapy. Most cases of shin splints can be effectively managed with conservative treatment approaches.
Self-Care Management
Self-care is often the first and most important step in treating shin splints. These measures can usually ease pain effectively:
- Rest from activities that cause pain, swelling, or discomfort, though you should continue engaging in low-impact movement
- Apply ice packs to the affected area for 15 to 20 minutes, several times a day to reduce inflammation
- Perform stretching exercises specifically targeting the calves and lower leg muscles
- Wear supportive footwear with shock-absorbing insoles to relieve stress on the shins
- Avoid activities that cause pain until healing has progressed
- Gradually return to exercise at a slow pace after pain has improved
Physical Therapy and Advanced Treatments
When self-care measures are insufficient, physical therapy and other advanced treatments may be recommended:
- Professional physical therapy to strengthen muscles and improve flexibility
- Ice massage along the affected area
- Ultrasound therapy to promote healing
- Iontophoresis, which uses a small electric charge to deliver medication through the skin
- Phonophoresis, which uses ultrasound to help deliver medication
- Periosteal pecking, a type of needling technique performed by specialists
- Shockwave therapy for cases resistant to conservative treatment
Footwear and Orthotics
Proper footwear is crucial in treating and preventing shin splints. It is recommended to change shoes every 300 to 400 miles and ensure they provide adequate support and cushioning. Shoe inserts with shock-absorbing properties can significantly help relieve stress on the shins. Custom orthotics may be prescribed if biomechanical issues like flat feet or excessive pronation are contributing to the condition.
Activity Modification
While treating shin splints, substituting lower-impact activities for high-impact exercise can maintain fitness while allowing the injury to heal. Swimming, cycling, and water running place significantly less stress on the lower leg compared to running or jumping sports.
Complications of Untreated Shin Splints
While shin splints are not immediately life-threatening, untreated or inadequately managed cases can lead to serious complications. The pain from shin splints can hinder movement and prevent participation in physical activities. More significantly, if shin splints are not properly treated, they may progress and lead to stress fractures in the shin bone. Stress fractures are small, hairline breaks in the bone that can become severe if activity is not reduced and appropriate treatment is not pursued.
Other potential complications include chronic exertional compartment syndrome, where swelling of muscles due to exertion causes increased pressure within the muscle compartment, potentially compromising blood supply to the muscle. Tendonitis, involving partial tears in tendons, can also develop if repetitive stress continues unchecked.
Prevention Strategies
Preventing shin splints involves careful attention to exercise habits, footwear, and physical conditioning. Gradually increasing exercise intensity and duration, rather than making sudden large increases, significantly reduces risk. Proper warm-up before exercise and cool-down afterward help prepare the muscles and bones for activity. Ensuring adequate core and calf muscle strength through targeted exercises helps support proper leg alignment and reduces stress on the shinbone.
Wearing appropriate, well-fitted footwear with adequate shock absorption is essential for prevention. Regular replacement of worn-out shoes maintains proper support during activities. Varying exercise routines to include different surfaces and activities helps prevent overuse of the same muscle groups. Additionally, allowing adequate recovery time between intense workouts gives bones and muscles time to repair and strengthen.
When to Seek Medical Attention
While many cases of shin splints can be self-managed, certain situations warrant professional medical evaluation. Seek medical attention if pain is severe, persists despite conservative treatment efforts, is accompanied by significant swelling or warmth in the leg, or if you suspect a stress fracture. Healthcare providers can perform advanced diagnostics and recommend specialized treatment options when conservative measures are ineffective.
Frequently Asked Questions
Q: How long does it take for shin splints to heal?
A: Recovery time varies depending on severity, but most cases of shin splints improve within a few weeks to several months with appropriate rest and treatment. Mild cases may resolve in 2-4 weeks, while more severe cases may require 3-6 months of conservative management.
Q: Can shin splints recur after treatment?
A: Yes, shin splints can recur if the underlying causes are not addressed. To prevent recurrence, continue wearing appropriate footwear, maintain proper conditioning, and gradually increase exercise intensity rather than making sudden changes.
Q: Are shin splints a permanent condition?
A: No, shin splints are not permanent. With appropriate treatment and prevention strategies, most people fully recover from shin splints and can return to their previous level of activity without ongoing problems.
Q: Can I exercise while treating shin splints?
A: You can engage in low-impact exercises such as swimming, cycling, or water running while treating shin splints. However, avoid activities that cause pain or stress to the affected shin, as these can worsen the condition and delay healing.
Q: What is the difference between shin splints and a stress fracture?
A: Shin splints involve inflammation of muscles and tissues around the shinbone, while stress fractures are small breaks in the bone itself. Stress fractures cause more localized, sharper pain and typically require imaging to diagnose. Untreated shin splints can progress to stress fractures.
References
- Shin splints – symptoms, causes, treatment and diagnosis — Healthdirect Australia. 2024. https://www.healthdirect.gov.au/shin-splints
- Shin Splints: Symptoms, Causes & Treatments — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/17467-shin-splints
- Shin Splints — American Academy of Orthopaedic Surgeons (AAOS). 2024. https://orthoinfo.aaos.org/en/diseases–conditions/shin-splints/
- Shin Splints Causes, Symptoms, & Treatment — UPMC. 2024. https://www.upmc.com/services/orthopaedics/conditions/shin-splints
- Shin splints – Diagnosis & treatment — Mayo Clinic. 2024. https://www.mayoclinic.org/diseases-conditions/shin-splints/diagnosis-treatment/drc-20354110
- Shin Splints — St. Louis Children’s Hospital. 2024. https://www.stlouischildrens.org/conditions-treatments/shin-splints
- Shin Splints: Causes, Symptoms, and Treatment — WebMD. 2024. https://www.webmd.com/fitness-exercise/shin-splints
Read full bio of medha deb











