Shingles (Herpes Zoster): Causes, Symptoms & Treatment
Complete guide to understanding shingles: causes, symptoms, treatment options, and prevention strategies.
Understanding Shingles: What You Need to Know
Shingles, medically known as herpes zoster, is a painful viral infection characterized by a rash and nerve pain caused by the varicella-zoster virus (VZV). If you’ve ever had chickenpox, you’re at risk for developing shingles later in life. The condition affects thousands of people annually and can cause significant discomfort, but understanding its causes, symptoms, and treatment options can help you manage it effectively.
The relationship between chickenpox and shingles is direct: the same virus that causes chickenpox in childhood remains dormant in your body’s nerve cells for decades and may reactivate as shingles in adulthood. This reactivation typically occurs when your immune system weakens due to aging or other health factors.
What Causes Shingles?
Shingles is caused by the varicella-zoster virus, the same pathogen responsible for chickenpox. After you recover from chickenpox, the virus doesn’t leave your body entirely. Instead, it remains inactive (dormant) within your nerve cells, where it can stay for decades without causing any symptoms.
The exact reason why the virus reactivates later in life isn’t completely understood, but researchers believe it occurs when your immune system weakens. This weakening can happen naturally as you age, or it can result from various medical conditions and medications that compromise immune function.
Several factors increase your risk of developing shingles:
– Age: Risk increases significantly as you get older, particularly after age 50- Previous chickenpox infection: Essential requirement for developing shingles- Weakened immune system: Due to HIV, cancer treatment, or immunosuppressive medications- Stress: Physical or emotional stress can trigger reactivation- Certain medications: Corticosteroids and immunosuppressants increase susceptibility
Recognizing Shingles Symptoms
Shingles typically begins with early warning signs before the characteristic rash appears. Recognizing these initial symptoms can help you seek treatment quickly, which may reduce severity and duration.
Early Warning Signs
Before the rash develops, you may experience:
– Burning pain or burning sensation in the affected area- Tingling sensations– Itching– Discoloration of the skin– Headache– Fever– Extreme sensitivity to touch– Sensitivity to light
The Characteristic Rash
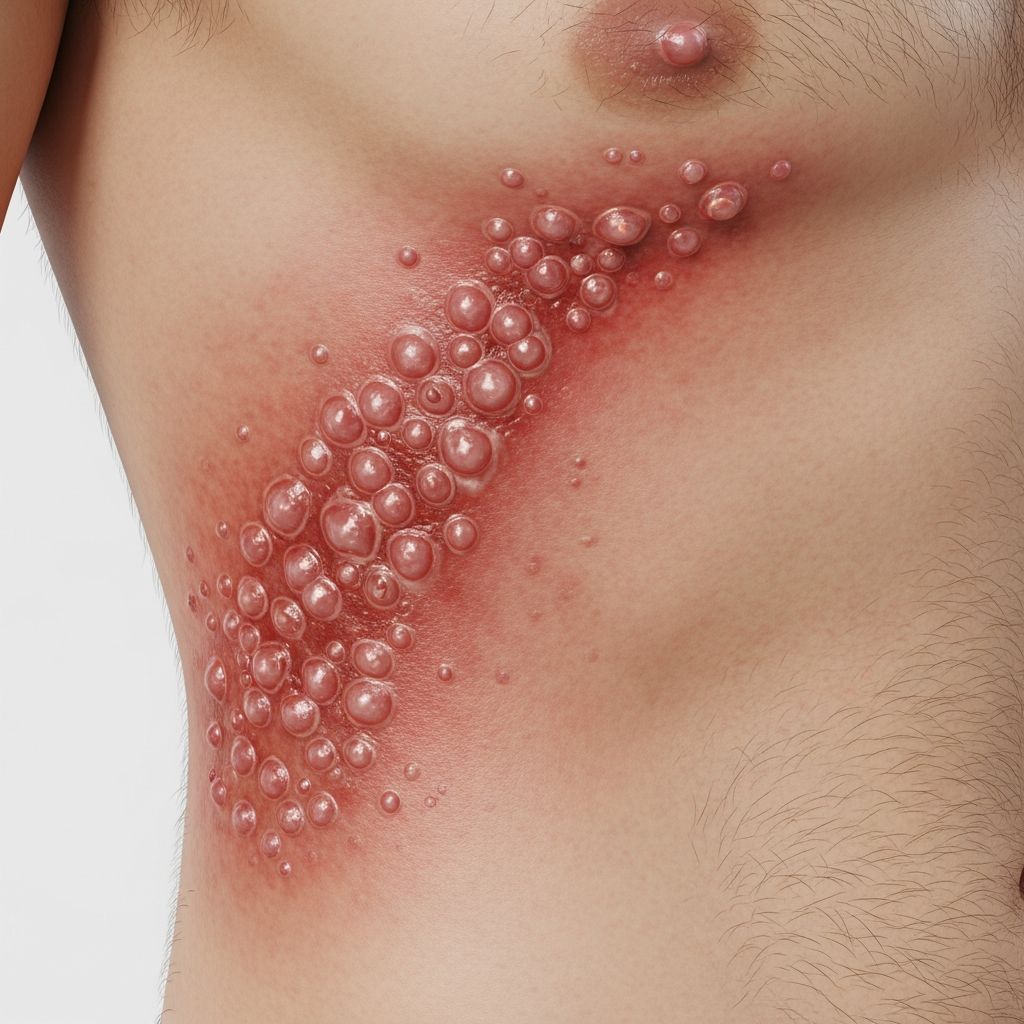
The most recognizable symptom of shingles is the rash itself. The rash typically appears within a few days of the initial pain and follows a specific pattern:
Initial appearance: The rash starts as small, raised red bumps or red dots. Within 7 to 10 days, these bumps develop into fluid-filled blisters. These blisters then break open and crust over within a matter of days. The rash usually clears up and scabs over, typically healing within 2 to 4 weeks.
Location pattern: Shingles typically appears in a band-like pattern on only one side of your body. Common locations include:
– Near the waist or torso– Chest– Back– Neck– One side of the face– Belly– Other parts of the body
The rash follows dermatomes, which are areas of skin connected to a single nerve. Importantly, the rash typically does not cross the midline of your body, which helps healthcare providers distinguish shingles from other skin conditions.
Atypical Presentations
It’s important to note that some people don’t develop a rash with shingles at all. Additionally, symptoms vary significantly from person to person. If you experience symptoms of shingles even without a visible rash, you should consult a healthcare provider for evaluation.
How Shingles Is Diagnosed
Healthcare providers typically diagnose shingles through clinical evaluation. The diagnostic process includes:
– Symptom assessment: Your doctor will ask about your symptoms and their progression- Visual examination: The provider will examine the rash carefully- Pattern recognition: A rash that follows dermatomes and doesn’t cross the body’s midline strongly suggests shingles- Laboratory confirmation: Your healthcare provider may send scrapings or swabs from blister fluid to a laboratory for confirmation, particularly in immunocompromised individuals where the rash appearance may be atypical
Treatment Options for Shingles
While there’s no cure for shingles, various treatments can reduce pain, speed healing, and prevent complications. Treatment is most effective when started early, ideally within 72 hours of rash onset.
Antiviral Medications
Antiviral medications form the cornerstone of shingles treatment:
– Acyclovir: A traditional antiviral medication- Valacyclovir: Often preferred due to better absorption- Famciclovir: Another effective antiviral option
These medications work by suppressing virus replication and are typically taken until symptoms subside, usually within 3 to 5 weeks.
Pain Management
During treatment, several approaches can relieve pain and reduce symptom severity:
– Over-the-counter pain relievers such as acetaminophen or ibuprofen- Topical treatments including numbing creams or calamine lotion- Corticosteroids which may reduce inflammation and pain- Cool compresses applied to the affected area- Prescription pain medications if needed for severe pain
Self-Care During Treatment
During your shingles episode, following these guidelines helps promote healing and prevent complications:
– Keep the rash clean and dry- Avoid scratching the affected area- Wear loose, comfortable clothing- Use cool, wet compresses on the rash- Avoid touching your eyes if the rash is on your face- Maintain good hygiene to prevent secondary bacterial infections
Complications and Long-Term Effects
While most people recover fully from shingles, complications can occur, particularly if treatment is delayed or the immune system is severely compromised.
Postherpetic Neuralgia (PHN)
The most common complication is postherpetic neuralgia, chronic nerve pain that persists after the rash has healed. This chronic pain can last for months or even years and may be debilitating. Over time, especially if you’ve experienced shingles more than once, the risk of developing PHN increases.
Other Complications
Other potential complications include:
– Secondary bacterial infections of the rash- Vision problems or blindness if shingles affects the eye area- Hearing loss or balance disorders- Weakness or paralysis in affected areas- Meningitis or encephalitis in rare cases- In rare instances, shingles can be fatal
Contagiousness and Prevention of Transmission
Understanding shingles transmission is crucial for protecting vulnerable individuals. You cannot directly transmit shingles to another person. However, the virus in your blisters can cause chickenpox in people who haven’t had chickenpox before and aren’t vaccinated.
You are contagious until the rash completely dries and crusts over. During this period, you should cover the rash and avoid contact with:
– Individuals with weakened immune systems- Infants and young children- Pregnant women who haven’t had chickenpox- People in schools or daycares
Can You Get Shingles More Than Once?
While most people experience shingles only once in their lifetime, recurrence is possible. Approximately 1.2% to 9.6% of people may develop shingles more than once.
Recurrent shingles typically occurs in individuals with weakened immune systems. Having shingles once increases your chance of future outbreaks, though not everyone experiences a second occurrence. When shingles does recur, many people report that subsequent episodes are less severe than the first experience, though this varies based on individual immune system health, current medications, and overall health status.
Several conditions can compromise immune function and increase recurrence risk:
– HIV/AIDS- Cancer and cancer treatments- Organ transplantation- Chronic corticosteroid use- Autoimmune diseases
Prevention Strategies
While you cannot entirely prevent a shingles outbreak if you’ve had chickenpox, several strategies can significantly reduce your risk:
Vaccination
The most effective prevention method is receiving the shingles vaccine. Modern vaccines like Shingrix can reduce shingles likelihood even in people with weakened immune systems. Vaccination is recommended for adults aged 50 and older and for certain immunocompromised individuals.
Immune System Support
Maintaining a strong immune system helps prevent shingles reactivation:
– Exercise regularly- Eat a balanced, nutritious diet- Get adequate sleep- Manage stress effectively- Maintain healthy weight- Avoid smoking and excessive alcohol consumption- Stay current with recommended vaccinations
Frequently Asked Questions About Shingles
Q: Can you get shingles without ever having chickenpox?
A: No, shingles only develops in people who have previously had chickenpox or received the varicella vaccine. The virus must be dormant in your nerve cells first.
Q: How long does shingles typically last?
A: With treatment, shingles typically resolves within 3 to 5 weeks. The rash usually scabs over and heals within 2 to 4 weeks. However, nerve pain may persist longer.
Q: Is shingles contagious to people who’ve had chickenpox?
A: No, shingles is not contagious to people who have had chickenpox or are vaccinated. However, the virus can cause chickenpox in unvaccinated, unexposed individuals.
Q: What age group is most affected by shingles?
A: While anyone who’s had chickenpox can develop shingles, risk increases significantly with age, particularly after age 50. However, children and younger adults can also develop the condition.
Q: Is shingles serious?
A: For most people, shingles is painful and uncomfortable but not dangerous. However, complications like postherpetic neuralgia can cause long-term pain, and in rare cases, shingles can affect vision, hearing, or neurological function.
Q: Can I go to work or school with shingles?
A: You can return to work or school once the rash is dried and crusted over, as long as you can keep it covered. Avoid contact with vulnerable individuals until this point.
When to Seek Medical Attention
Contact a healthcare provider if you experience:
– Severe pain not controlled by over-the-counter medications- Rash near your eye- Signs of bacterial infection (increasing redness, warmth, drainage)- Symptoms of neurological complications- Rash spreading extensively- Immunocompromising conditions combined with shingles symptoms
References
- Can You Get Shingles More Than Once? — Cleveland Clinic. 2025. https://health.clevelandclinic.org/can-you-get-shingles-more-than-once
- Shingles (Herpes Zoster): Causes, Symptoms & Treatment — Cleveland Clinic. 2025. https://my.clevelandclinic.org/health/diseases/11036-shingles
- Preventing herpes zoster in immunocompromised patients: Current perspectives — Cleveland Clinic Journal of Medicine, 2022. https://www.ccjm.org/content/91/7/437
- Varicella Zoster Virus (VZV): Infection & Diseases — Cleveland Clinic. 2025. https://my.clevelandclinic.org/health/diseases/varicella-zoster-virus
- All About Shingles: Symptoms, Causes and Treatment — Cleveland Clinic Abu Dhabi. 2025. https://www.clevelandclinicabudhabi.ae/en/health-byte/health/all-about-shingles
- Shingles: What You Should Know About the Sequel to Chickenpox — Cleveland Clinic Health Essentials Podcast. 2025. https://my.clevelandclinic.org/podcasts/health-essentials/shingles-what-you-should-know-about-the-sequel-to-chickenpox-with-dr-jeffrey-brown
- Postherpetic Neuralgia: What It Is, Symptoms & Treatment — Cleveland Clinic. 2025. https://my.clevelandclinic.org/health/diseases/12093-postherpetic-neuralgia
Read full bio of medha deb











