Skin Conditions In Newborn Babies: What Parents Need To Know
Comprehensive guide to common rashes, blisters, and skin issues in newborns, including causes, diagnosis, and management.
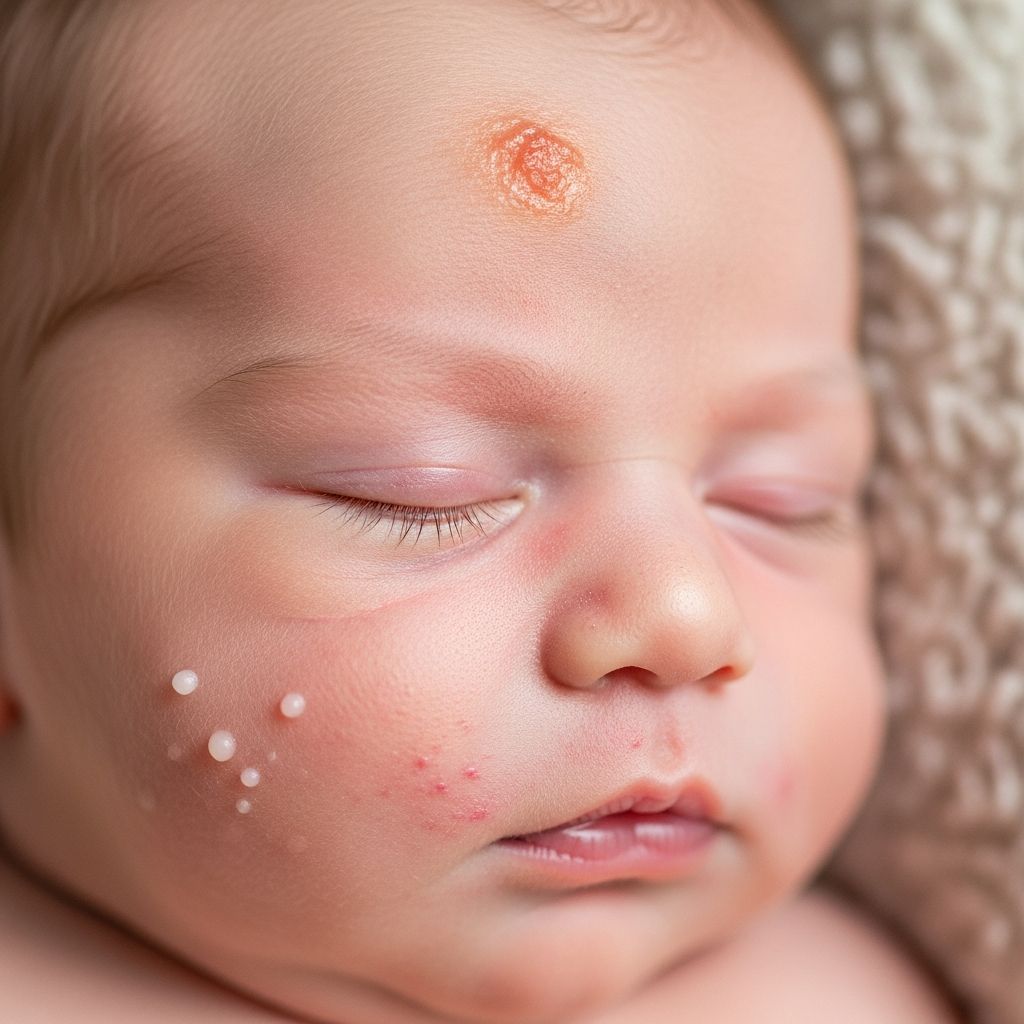
Skin Conditions in Newborn Babies
Newborn skin is delicate and undergoes rapid changes in the first weeks of life, making it prone to various transient conditions. Many rashes and blemishes are harmless and resolve spontaneously, but understanding them helps parents distinguish normal findings from those needing medical attention.
What are the most common skin conditions in newborns?
A wide array of skin issues can appear in the neonatal period, often due to the immature skin barrier, higher hydration, alkaline pH, and developing microbiome. Full-term newborns have a more developed stratum corneum by 34 weeks gestation, but preterm infants remain vulnerable to transepidermal water loss (TEWL), infections, and topical agent absorption. Common presentations include vesicles (small blisters), pustules (yellow-white spots), bullae (large blisters), erosions, and erythematous patches.
Approximately 50-70% of newborns experience some rash, most self-limiting within days to weeks. Factors like warm climates, occlusive clothing, and maternal hormones contribute. Preventive care involves gentle cleansing, fragrance-free emollients, and avoiding irritants to support barrier function.
Toxic Erythema of the Newborn
**Toxic erythema of the newborn** (also called erythema toxicum neonatorum) is the most prevalent rash, affecting up to 50% of full-term infants but rare in premies. It typically emerges on day 2-3 of life, though it can appear up to two weeks, starting on the face and spreading to trunk and limbs while sparing palms and soles.
Lesions manifest as fleeting pink or red macules, often with surrounding pale weals, papules, or small pustules in crops. The baby remains well and asymptomatic. Diagnosis is clinical; if needed, pustule microscopy reveals eosinophils, distinguishing it from bacterial or viral causes. It resolves in 1-2 days per crop, fully clearing by 2 weeks without treatment.
Transient Neonatal Pustular Melanosis
This condition presents at birth, more common in dark-skinned babies, and may represent a severe variant of toxic erythema. Hyperpigmented macules remain after fragile pustules rupture, leaving a collarette of scale. Neutrophils on microscopy confirm diagnosis; culture rules out infection. Lesions fade over weeks to months without sequelae.
Miliaria (Heat Rash)
**Miliaria** impacts 15% of newborns in warm environments due to sweat duct occlusion.
Miliaria crystallina
features clear, superficial vesicles on forehead, neck, and trunk. Deepermiliaria rubra
(prickly heat) shows red papules and pustules.Management entails cooling the infant, loose clothing, and avoiding occlusion; resolution occurs in days. Unlike adult miliaria, neonatal cases rarely scar.
Milia
Tiny 1-2 mm white keratin cysts,
milia
affect 50% of newborns on the nose, cheeks, and forehead. Oral variants include Epstein pearls (palate) and Bohn nodules (gums), all resolving by 4 weeks spontaneously. No treatment needed; avoid extraction to prevent scarring.Neonatal Acne (Milk Spots)
Triggered by maternal androgens stimulating sebaceous glands,
infantile acne
appears in the first weeks as erythematous papules and pustules on cheeks, nose, and forehead. Non-pruritic, it peaks at 2-4 weeks and clears by 3 months without intervention. Persistent cases may need topical therapy.Seborrhoeic Dermatitis (Cradle Cap)
**Cradle cap** involves greasy yellow scales on the scalp, sometimes extending to face, neck folds, and diaper area. Mildly erythematous in flexures, it’s linked to Malassezia yeast overgrowth. Apply emollients or baby oil, then gently comb scales. Persistent or inflamed cases warrant topical antifungals or low-potency steroids per pediatrician.
Atopic Dermatitis (Eczema)
Though less common neonatally, early
atopic dermatitis
presents as itchy, scaly red patches on cheeks, trunk, and extensors. Risk factors include family history and barrier defects. Daily fragrance-free moisturizers are first-line; topical steroids for flares. Emollients from birth may prevent it in high-risk infants.Other Vesicles, Pustules, Bullae, Erosions, and Ulcerations
- Herpes simplex: Grouped vesicles progressing to erosions; urgent antiviral needed.
- Candida: Moist-area pustules; topical antifungals.
- Bacterial folliculitis: Golden pustules; culture-guided antibiotics.
- Incontinentia pigmenti: Linear vesicles then hyperpigmented swirls; genetic referral.
- Epidermolysis bullosa: Trauma-induced bullae and erosions; wound care.
Always assess for systemic illness; microscopy/culture differentiates benign from infectious.
Physiology of Newborn Skin
Newborn skin differs markedly: higher TEWL initially, alkaline pH (6.34-7.5 vs adult 5-5.5), elevated hydration, and distinct microbiome favoring Staphylococci. Preterm skin lacks full barrier until 2-3 weeks, heightening risks of infection, thermoregulation failure, and percutaneous absorption. Desquamation peaks on face at 3 months. Antimicrobial proteins like lysozyme are abundant, aiding innate defense.
| Feature | Newborn | Adult |
|---|---|---|
| Stratum Corneum | Immature, high TEWL | Mature, low TEWL |
| pH | Alkaline (6.3-7.5) | Acidic (5-5.5) |
| Hydration | High | Lower |
| Permeability | High | Low |
Table 1: Key differences in skin physiology.
Skin Care for Newborns
Gentle practices preserve the barrier: use pH-neutral cleansers sparingly, pat dry, apply emollients daily (petrolatum or ceramide-based). Avoid soaps, powders, fragrances. For premies, emollients reduce TEWL but monitor infection risk. Bathe 2-3 times weekly; daily top-to-toe emollient suffices.
When to See a Doctor
- Fever, lethargy, poor feeding with rash.
- Spreading vesicles/pustules not fading in days.
- Bullae, erosions, or mucosal involvement.
- Rash in premies or persistent beyond 4 weeks.
- Signs of infection: warmth, pus, tenderness.
Frequently Asked Questions (FAQs)
Q: Is toxic erythema harmful?
A: No, it’s benign and self-resolves without treatment.
Q: How to treat cradle cap?
A: Emollients and gentle combing; see doctor if persistent.
Q: Can emollients prevent eczema?
A: Yes, in high-risk babies with daily application.
Q: Are milia normal?
A: Yes, affect 50% and vanish by 1 month.
Q: When is a newborn rash serious?
A: If accompanied by illness or not improving.
References
- Skin Physiology of the Neonate and Infant: Clinical Implications — PMC / Mancini et al. 2015-06-01. https://pmc.ncbi.nlm.nih.gov/articles/PMC4593874/
- Skin conditions affecting newborn babies — DermNet NZ. 2023-01-01. https://dermnetnz.org/topics/skin-conditions-in-newborn-babies
- Baby Blemishes: Seven Common Skin Conditions in Newborns — Children’s Wisconsin. 2025-07-01. https://childrenswi.org/at-every-turn/stories/2025/07/common-newborn-skin-conditions
- Neonatal & infant skin care — Royal Children’s Hospital. 2024-01-01. https://www.rch.org.au/rchcpg/hospital_clinical_guideline_index/neonatal___infant_skin_care/
- Newborn Skin: Part I. Common Rashes — AAFP. 2008-01-01. https://www.aafp.org/pubs/afp/issues/2008/0101/p47.html
Read full bio of medha deb