Skin Infections: Types, Causes, and Treatment Options
Comprehensive guide to bacterial, fungal, and viral skin infections with prevention and treatment strategies.
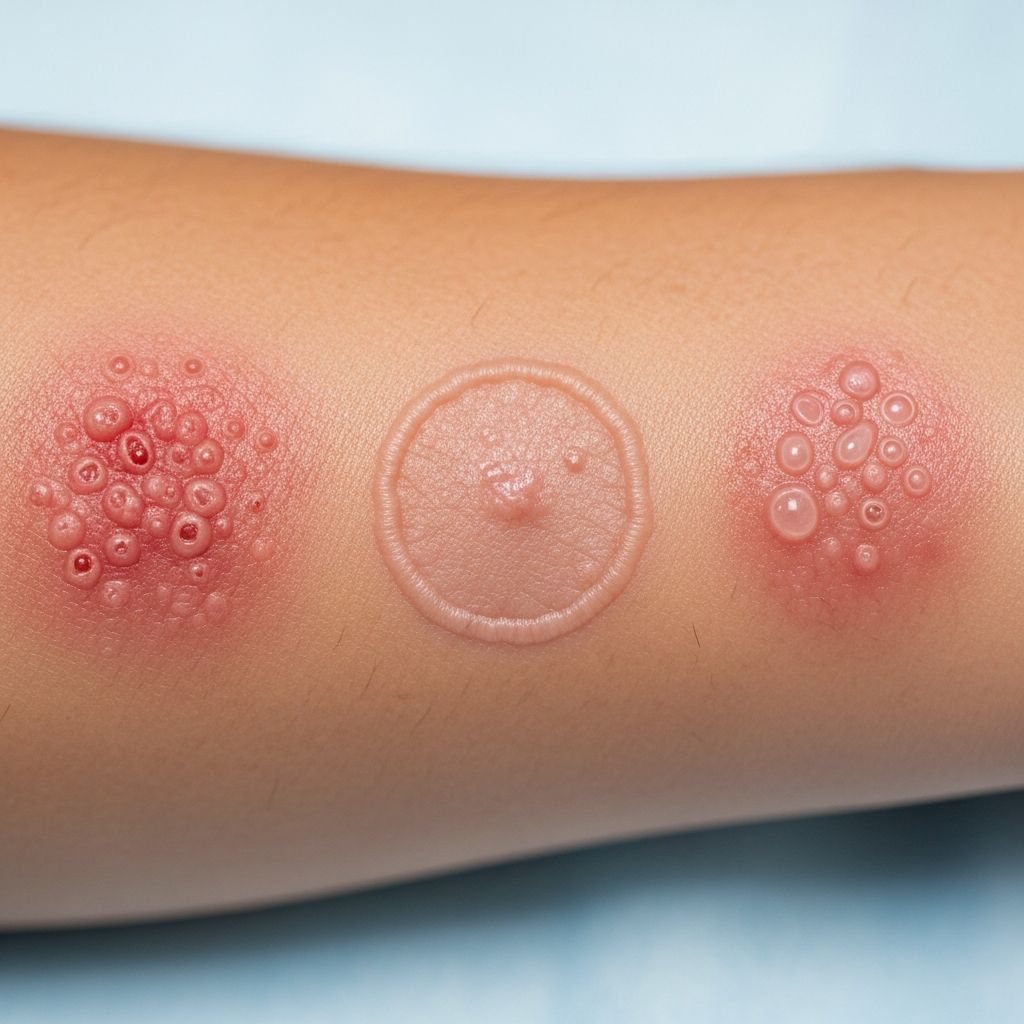
Introduction to Skin Infections
Skin infections are diseases and conditions caused by or related to external organisms that can significantly impact skin health and comfort. These infections can arise from various microorganisms and may result from direct invasion of normal skin or involvement of compromised skin barriers. Understanding the different types of skin infections, their causes, and appropriate treatment options is essential for effective management and prevention of complications.
Infections can be classified based on the type of organism responsible, including bacteria, fungi, viruses, and parasitic organisms. The human skin is naturally colonized by numerous microorganisms—collectively known as the skin microbiota—which typically coexist harmlessly with healthy skin. However, when the skin barrier is compromised or immune function is impaired, these organisms may cause infection.
Classification of Infectious Organisms
Skin infections are caused by various classes of microorganisms, each requiring different diagnostic approaches and treatment strategies:
- Bacteria: Commonly Staphylococcal or Streptococcal species that invade normal skin or affect compromised skin barriers
- Fungi: Including yeasts and dermatophytes that thrive in warm, moist environments
- Viruses: Such as herpes simplex virus and other viral pathogens affecting the skin
- Parasites and Mites: Organisms causing infestations and inflammatory skin responses
Risk Factors and Predisposing Conditions
Skin infection is more likely to occur under specific circumstances. Several factors increase susceptibility to infection:
- Lacerations, abrasions, thermal burns, chemical burns, animal bites, and insect bites that compromise skin integrity
- Immunosuppression or weakened immune system function
- Existing skin conditions such as atopic dermatitis or eczema with damaged skin barriers
- Surgical wound sites vulnerable to bacterial colonization
- Warm, moist skin environments conducive to fungal growth
- Poor hygiene practices or inadequate wound care
Optimal health and skin barrier function are essential for preventing and treating infections effectively. Minimizing the risk of skin damage through appropriate protective measures is fundamental to infection prevention.
Opportunistic Infections
Opportunistic infections occur in immunosuppressed patients and are more frequent or severe because of compromised immune function. These infections may be caused by common infectious organisms such as Staphylococcus aureus, Candida albicans, or Herpes simplex, or by organisms that rarely affect healthy individuals. Organisms that primarily affect immunocompromised individuals include nocardia, bartonella, atypical mycobacteria, cytomegalovirus, cryptococcus, and various systemic mycoses (deep fungal infections).
Bacterial Skin Infections
Overview and Common Causative Organisms
Bacterial skin infections represent a significant portion of dermatological conditions. The most common bacteria responsible for skin infections are Staphylococcus and Streptococcus species. These bacteria can invade normal, intact skin or colonize compromised skin barriers, leading to various clinical presentations.
Clinical Features of Bacterial Skin Infections
Bacterial skin infections typically present with characteristic signs and symptoms:
- Erythema (redness) of affected areas
- Pain and tenderness
- Warmth at the infection site
- Swelling (edema)
- Functional impairment depending on severity
- Purulent discharge (pus) in moderate to severe infections
- Lymphadenopathy (enlarged lymph nodes)
In severe infections, systemic signs may develop, including fever and malaise. It is important to note that erythema may be less evident in darker skin tones, and postinflammatory hyperpigmentation is more commonly observed in individuals with increased skin pigmentation.
Diagnosis of Bacterial Infections
Bacterial skin infection is commonly diagnosed through clinical assessment, although laboratory studies enhance diagnostic accuracy. Useful diagnostic methods include:
- Culture and sensitivity testing to identify the specific organism and antibiotic susceptibility
- Gram staining of samples
- Blood cultures in severe infections
- Skin swabs for microbiological analysis
It is best practice to obtain samples before commencing antibiotic therapy to allow proper identification and targeted treatment. However, in serious infections such as suspected meningococcal disease, treatment with broad-spectrum antibiotics should not be delayed pending culture results.
Treatment of Bacterial Skin Infections
Treatment approaches depend on infection severity and organism sensitivity:
- Minor infections: Often resolve without treatment; topical antiseptics are preferred over topical antibiotics due to rising antibiotic resistance concerns
- Moderate infections: Oral antibiotics targeting the identified organism
- Severe infections: Intravenous or intramuscular antibiotics, sometimes requiring hospitalization
As culture and sensitivity results become available, treatment should be adjusted from broad-spectrum to appropriate narrow-spectrum antibiotics to minimize resistance development and reduce unnecessary antibiotic exposure.
Fungal Skin Infections
Types of Fungal Infections
Fungal infections of the skin are caused by organisms naturally present on everyone’s skin. Two main categories of fungal infections affect the skin:
- Candida infections: A yeast that thrives in warm, moist areas such as under the arms, groin region, and neck area (particularly in children)
- Dermatophyte infections: Molds causing tinea (ringworm), named descriptively for the shape of lesions rather than the presence of actual worms
Tinea Infections Classification
Tinea infections are named according to their anatomical location:
- Tinea corporis: Fungal infection of body surfaces
- Tinea capitis: Fungal infection of the scalp
- Tinea pedis: Fungal infection of the feet (athlete’s foot)
- Tinea unguium: Fungal infection of the nails
Tinea infections can be difficult to distinguish from discoid eczema based on clinical appearance alone, sometimes requiring mycological analysis for definitive diagnosis.
Diagnosis and Treatment of Fungal Infections
Initial treatment typically involves topical antifungal agents such as miconazole cream, which is available both by prescription and over-the-counter at pharmacies. The healthcare provider may prescribe topical treatment to assess skin response and lesion clearance.
For scalp and nail infections, oral antifungal agents are necessary and require prescription from a healthcare provider. A skin scraping can be obtained for mycological analysis when diagnostic uncertainty exists or lesions prove difficult to resolve.
Unlike antibiotic creams, antifungal creams do not carry the same resistance concerns. Consistent application is required for optimal results, typically three times daily or as directed by healthcare providers, continuing until lesions completely clear.
Viral Skin Infections
Herpes Simplex Virus Infections
The herpes simplex virus typically causes cold sores in the general population, but in individuals with compromised skin barriers or specific conditions, it can develop into more serious manifestations. The virus spreads through direct contact, both skin-to-skin and through contact with contaminated surfaces, where the virus can survive for several hours.
Eczema Herpeticum
A particularly serious viral infection that can develop is eczema herpeticum, where herpes simplex virus spreads rapidly through the skin. Symptoms of this condition include:
- Areas of painful eczema that rapidly deteriorate
- Groups of fluid-filled blisters that rupture, leaving small shallow sores
- High fever and general malaise (in some cases)
- Rapid spread of infection across affected skin areas
Prevention and Treatment of Viral Infections
To prevent transmission of eczema herpeticum, patients should immediately notify healthcare providers upon arrival at medical facilities of suspected infection, allowing for assessment in a private area to prevent further spread.
Treatment for eczema herpeticum involves antiviral medication called aciclovir. Many patients require hospitalization for intravenous administration of therapy, typically for several days to ensure adequate treatment and monitoring of recovery.
Diagnostic Approach to Skin Infections
Accurate diagnosis is fundamental to appropriate treatment selection. Diagnostic methods vary based on suspected organism type:
- Clinical examination and history taking
- Culture and sensitivity testing
- Gram staining procedures
- Mycological analysis for fungal infections
- Viral cultures or PCR testing when indicated
- Imaging studies in complicated infections
Proper sample collection before commencing treatment ensures accurate identification and targeted therapy, improving treatment outcomes and minimizing resistance development.
Treatment Principles and Considerations
Treatment of skin infection depends on multiple factors:
- The causative organism (bacterial, fungal, or viral)
- Severity of infection (minor, moderate, or severe)
- Sensitivity of the organism to proposed treatment agents
- Location and extent of infection
- Patient immune status and overall health
- Potential for resistance development
Minor skin infections may settle on their own in healthy individuals without active treatment, as tackling infection can enhance natural immunity development. However, some infections require treatment to prevent serious complications or systemic spread.
Prevention of Skin Infections
Effective prevention strategies significantly reduce infection risk:
- Minimize skin trauma through careful handling and appropriate protective measures
- Maintain proper hygiene without excessive measures that may disrupt skin microbiota
- Keep wounds clean and properly dressed with non-adherent materials
- Avoid sharing personal items such as towels or razors
- Maintain healthy skin barrier function through appropriate moisturization
- Address underlying skin conditions promptly
- Practice good hand hygiene, especially before applying treatments
Importantly, excessive hygienic measures can be counterproductive if they excessively disrupt normal skin microbiota or cause unnecessary skin irritation.
When to Seek Medical Attention
Professional evaluation is warranted for:
- Infections showing signs of spreading or systemic involvement
- Infections not responding to home care within a few days
- Signs of systemic infection (fever, malaise, enlarged lymph nodes)
- Infections in high-risk individuals (immunocompromised, very young, elderly)
- Suspected resistant bacterial strains (MRSA)
- Potential serious viral infections like eczema herpeticum
Frequently Asked Questions
Q: Can minor skin infections resolve without treatment?
A: Yes, minor bacterial infections often resolve without active treatment in healthy individuals, though some infections require treatment to prevent complications or serious disease spread.
Q: Why is antibiotic resistance a concern in skin infection treatment?
A: Overuse of topical and oral antibiotics promotes the development of resistant bacterial strains, making future infections harder to treat. Therefore, first-line use of topical antibiotics is discouraged, with topical antiseptics preferred for minor infections.
Q: How can I prevent fungal skin infections?
A: Keep skin dry, especially in warm moist areas; avoid sharing personal items; maintain proper hygiene; and treat any breaks in the skin barrier promptly to prevent fungal colonization.
Q: What is the difference between tinea and ringworm?
A: Tinea and ringworm refer to the same fungal infection caused by dermatophytes. The term “ringworm” describes the characteristic ring-shaped lesion appearance, though the infection involves no actual worms.
Q: When should samples be taken for testing?
A: Samples should ideally be obtained before commencing antibiotic therapy to allow proper organism identification and sensitivity testing, enabling targeted treatment that minimizes resistance development.
References
- Skin Infections — DermNet NZ. 2024. https://dermnetnz.org/topics/skin-infections
- Bacterial Skin Infections — DermNet NZ. 2024. https://dermnetnz.org/topics/bacterial-skin-infections
- Skin Infections and Eczema — National Eczema Association. 2024. https://eczema.org/information-and-advice/living-with-eczema/skin-infections-and-eczema/
- Do Not Be Rash With Rashes: A Guide to Dermatological Description — Royal College of Emergency Medicine. 2024. https://www.rcemlearning.co.uk/foamed/do-not-be-rash-with-rashes-a-guide-to-dermatological-description/
- Looking After and Treating Skin Infections — Ministry of Health, New Zealand. 2013. https://www.health.govt.nz/system/files/2013-11/skin-infections-booklet-nov13v2.pdf
Read full bio of Sneha Tete












