Skin Signs Of Non-Accidental Injury: Expert Guide For Clinicians
Recognizing cutaneous indicators of child abuse and distinguishing them from accidental trauma or medical conditions.
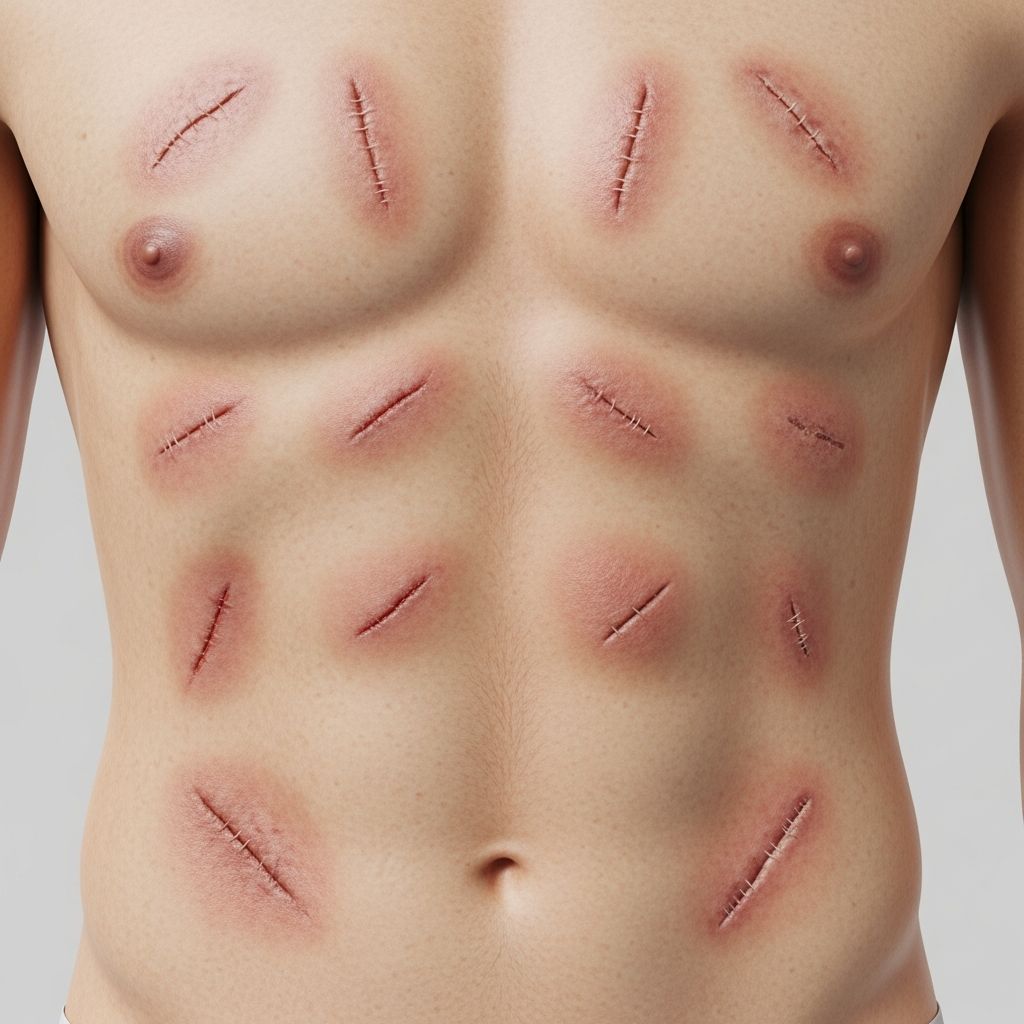
Skin Signs of Non-Accidental Injury
Non-accidental injury (NAI), often termed child physical abuse, frequently presents with characteristic skin findings. Dermatologists and clinicians must recognize these to protect vulnerable children, distinguishing intentional harm from accidental trauma or dermatological conditions.
What is non-accidental injury?
Non-accidental injury refers to deliberate physical harm inflicted on a child by a caregiver or authority figure. Skin lesions are the most common physical evidence, appearing in over 80% of confirmed abuse cases. These signs require urgent reporting to child protection services.
Who gets non-accidental injury?
NAI affects children under 3 years most frequently, with infants under 1 year at highest risk due to dependency and inability to disclose abuse. Pre-existing conditions like osteogenesis imperfecta or bleeding disorders can mimic findings, necessitating thorough evaluation.
Clinical features of skin signs in non-accidental injury
Skin manifestations vary by injury mechanism but share patterns inconsistent with accident explanations. Key features include lesion distribution, morphology, age discrepancy, and multiplicity.
Bruising
Bruises from abuse often appear on non-prominent sites like buttocks, thighs, or torso, unlike accidental bruises on shins or foreheads. Patterns include loop marks from belts/cords, handprints, or grab marks. Fresh bruises evolve from red to purple, green, then yellow over 10-14 days.
- Site: Central body, back, face (under 4 months suspicious)
- Pattern: Linear, tram-track, petechiae from strangulation
- Number: Multiple in clusters, varying ages
Burns
Abuse burns show sharp demarcation, sparing creases (immersion not accidental). Cigarette burns are circular (0.5-2 cm) with central necrosis; rope burns linear. Splash/spill burns irregular.
| Burn Type | Characteristics | Abuse Indicators |
|---|---|---|
| Immersion | Glove/stockings, tidy edges | Spares flexion creases, uniform depth |
| Contact | Cigarette, iron | Volckmann’s ischemic lines absent |
| Chemical | Irregular, deep | History mismatch |
Bite marks
Human bites show double arc (upper/lower teeth), 3-5 cm wide, often on face/genitals. Animal bites have single arc or punctures. Measure intercanine distance (>3 cm adult human).
Lacerations and scars
Parallel lines from whips/belts; jagged from teeth/tools. Healed scars parallel or geometric suggest repetition.
Ligature marks
Neck, wrists, ankles from binding; linear with abrasion.
Other signs
- Head banging: Alopecia patches
- Factitial: Self-inflicted, but in NAI may be forced
- Neglect: Pressure ulcers, impetigo
Complications
Untreated NAI leads to chronic trauma, infection, scarring, psychological harm. Missed diagnosis risks fatality (shaken baby syndrome).
Differential diagnosis of skin signs of non-accidental injury
| Condition | Distinguishing Features |
|---|---|
| Mongolian blue spots | Present at birth, non-tender, buttocks/lower back |
| Phytophotodermatitis | Drip/streak pattern, hyperpigmented |
| Haemophilia/bleeding disorders | Spontaneous, joints/muscles, family history |
| Infections (impetigo) | Honey-crusted, contagious |
| Lichen sclerosus | Genital, ivory plaques |
Normal bruising peaks at toddler stage from activity; abuse shows atypical sites/patterns.
Diagnosis of skin signs of non-accidental injury
Diagnosis combines history (inconsistent), exam (patterns), and investigations. Document with photos (ruler reference), measurements, diagrams. Skeletal survey for occult fractures; ophthalmology for retinal hemorrhages.
- Photo all lesions in natural light
- UV light for occult bruises
- Biopsy if unclear (e.g., rule vasculitis)
Management
Immediate child protection notification mandatory. Admit if risk high; multidisciplinary team (paediatrics, social services, police). Supportive wound care; psychological assessment.
Prevention of skin signs of non-accidental injury
Education for parents, early intervention for at-risk families (domestic violence, substance abuse). Clinician vigilance: screen high-risk presentations (recurrent ER visits, vague histories).
Evidence-based studies on skin signs of non-accidental injury
Studies confirm patterned bruising specificity (loop marks 95% abuse). Forensic analysis distinguishes human vs. animal bites via microscopy.
Guidelines on skin signs of non-accidental injury
- WHO: Mandatory reporting
- American Academy of Pediatrics: Skeletal surveys <2 years
- Royal College of Paediatrics: Pattern recognition training
Frequently Asked Questions
Can normal activity cause patterned bruises?
No, geometric/linear patterns indicate implements, not accidents.
How to document suspected NAI?
Use body maps, calibrated photos, detailed descriptions without interpretation.
Are facial bruises always abuse?
In infants <4 months, yes highly suspicious; toddlers may fall.
What if parents refuse evaluation?
Court order for protection; safety first.
Role of dermatologist in NAI?
Expert consultation for mimics, biopsy, forensic opinion.
Related topics
- Forensic dermatology
- Child abuse syndromes
- Pressure injuries
References
- Forensic Dermatology — DermNet NZ. 2023-05-15. https://dermnetnz.org/topics/forensic-dermatology
- Skin Signs of Coma — DermNet NZ. 2023-08-20. https://dermnetnz.org/topics/skin-signs-of-coma
- Child Physical Abuse — American Academy of Pediatrics. 2024-01-10. https://publications.aap.org/pediatrics/article/153/3/e2023062951/196198
- Guidelines for the Investigation of Child Physical Abuse — Royal College of Paediatrics and Child Health. 2023-11-05. https://www.rcpch.ac.uk/resources/child-protection-evidence-systematic-review-cpesr-physical-abuse
- WHO Child Maltreatment Prevention — World Health Organization. 2024-06-12. https://www.who.int/teams/social-determinants-of-health/violence-prevention/child-maltreatment
Read full bio of Sneha Tete