Stereotactic Breast Biopsy: 6 Steps And What To Expect
Learn what to expect from a stereotactic breast biopsy, a minimally invasive procedure to diagnose breast abnormalities detected on mammograms.
A
stereotactic breast biopsy
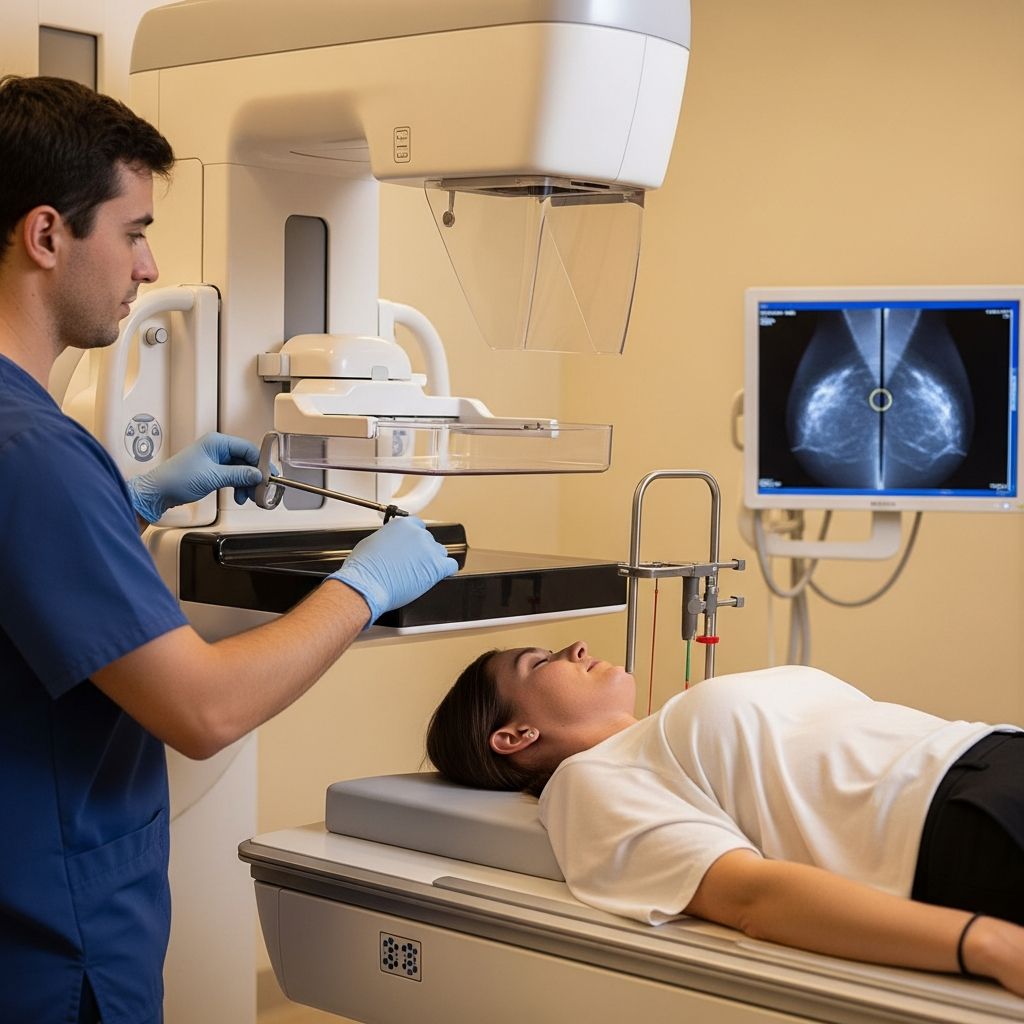
is a minimally invasive diagnostic procedure that uses advanced mammography imaging to precisely locate and sample suspicious areas in the breast detected during routine screening. This technique, also known as a tomosynthesis-guided or mammography-guided biopsy, allows doctors to obtain tissue samples for pathological examination without the need for open surgery, confirming whether abnormalities like calcifications or masses are cancerous or benign.What Is a Stereotactic Breast Biopsy?
A stereotactic breast biopsy combines digital mammography with computer-guided technology to target non-palpable lesions invisible on ultrasound. During the procedure, the breast is compressed between plates while X-rays are taken from multiple angles (typically 0°, +15°, and -15°) to create a three-dimensional map of the abnormality. A computer calculates the exact coordinates, guiding a biopsy needle to the precise location for tissue extraction.
This method is particularly useful for microcalcifications or architectural distortions seen on mammograms but not detectable by physical exam or ultrasound. Unlike surgical biopsies, it requires only a tiny skin incision and local anesthesia, making it outpatient-friendly with quick recovery.
- Key Technology: Stereotactic mammography unit with vacuum-assisted or core needle biopsy devices.
- Sample Collection: 6-12 tissue cores per session to ensure adequacy.
- Marker Placement: A small titanium clip is often deployed post-biopsy to mark the site for future imaging or surgery.
Purpose of Stereotactic Breast Biopsy
The primary goal is to diagnose breast cancer or other conditions by analyzing tissue from mammogram-detected abnormalities. Imaging like mammography reveals suspicious findings such as calcifications, masses, or asymmetries, but only biopsy provides definitive histology.
Indications include:
- Clusters of microcalcifications.
- Asymmetrical densities or distortions.
- Non-mass enhancements not visible on ultrasound.
- Lesions requiring pathological correlation after imaging.
If results are malignant, it aids in staging and treatment planning; benign results often avoid unnecessary surgery. Studies show less than 30% of stereotactic biopsies confirm cancer, highlighting its role in ruling out malignancy.
How Is a Stereotactic Breast Biopsy Performed?
The procedure typically lasts 30-60 minutes and is performed by a breast radiologist in an outpatient imaging center. Patients are awake but numbed locally.
Step-by-Step Process:
- Positioning: Patient lies prone on a specialized table with the breast protruding through a hole, or sits upright in some systems. The breast is compressed for stability.
- Imaging: Scout mammogram at 0° followed by angled views (±15°) localizes the target. Computer software computes depth and coordinates.
- Anesthesia: Lidocaine injection numbs the skin and deeper tissues; a slight pinch is felt.
- Incision and Needle Insertion: Tiny nick in skin; needle (core, vacuum-assisted, or spring-loaded) advances under stereotactic guidance. Post-positioning images confirm accuracy.
- Sampling: Multiple passes yield 6-12 samples. Specimen radiography verifies target inclusion.
- Completion: Clip placement, compression bandage, and post-procedure mammogram.
For MRI-guided variants (if mammogram-invisible), patients lie prone in an MRI scanner with similar sampling under intermittent imaging.
Preparation for Stereotactic Breast Biopsy
Minimal preparation is needed, but patients should:
- Discuss medications (e.g., blood thinners like aspirin, warfarin) with providers; may need to pause 3-7 days prior.
- Avoid caffeine and blood-thinning supplements (fish oil, vitamin E) for 3-5 days.
- Inform about allergies, implants, pregnancy, or deodorant (which can interfere with imaging).
- Arrange a ride home due to sedation or emotional stress, though driving is often possible.
- Wear comfortable, two-piece clothing; no lotions or perfumes on the breast.
No fasting required unless sedation is used. Screening questions ensure safety.
During the Procedure: What to Expect
Pressure from breast compression is the most common sensation, similar to a mammogram but prolonged (10-20 minutes). Anesthesia minimizes pain; brief pressure or tugging occurs during sampling.
| Sensation | Description |
|---|---|
| Anesthesia Injection | Slight pinch or sting. |
| Compression | Firm pressure; hold still. |
| Needle Insertion/Sampling | Pressure, no sharp pain. |
| Post-Procedure | Mild soreness relieved by ice/OTC pain relievers. |
Recovery After Stereotactic Breast Biopsy
Patients resume normal activities immediately, with a bandage over the site. Mild bruising, swelling, or soreness lasts 1-2 days; apply ice and take ibuprofen as needed.
Care Instructions:
- Keep bandage dry for 24-48 hours.
- Avoid heavy lifting or strenuous exercise for 24 hours.
- Monitor for infection (redness, fever) or hematoma; rare.
- Results in 2-7 days via phone or portal.
A follow-up mammogram confirms clip placement.
Risks and Complications
Safe with low complication rates (<1% serious):
- Bleeding/hematoma (most common, self-resolves).
- Infection.
- Pain or vasovagal reaction.
- False negatives (rare with multiple samples).
- Allergic reaction to anesthesia.
Vacuum-assisted devices reduce these risks compared to older methods.
Results and Next Steps
A pathologist examines samples under microscope:
- Benign: No cancer; routine screening resumes.
- Malignant: Discuss surgery, chemo, radiation.
- Discordant: Surgical biopsy if pathology mismatches imaging.
Early detection via stereotactic biopsy improves outcomes.
Benefits of Stereotactic Breast Biopsy
- Minimally invasive alternative to surgery.
- High accuracy (95%+).
- Cost-effective, outpatient.
- Reduces anxiety with quick diagnosis.
- Preserves breast aesthetics.
Frequently Asked Questions (FAQs)
Is stereotactic breast biopsy painful?
Local anesthesia ensures minimal pain; most feel only pressure.
How long does it take?
30-60 minutes total.
Can I drive home after?
Usually yes, but arrange support for emotional reasons.
What if results show cancer?
Treatment options like lumpectomy follow.
Is it safe for all breast types?
Best for posterior/superior lesions; MRI alternative if ineligible.
References
- Stereotactic Breast Biopsy — Cleveland Clinic. 2023-10-15. https://my.clevelandclinic.org/health/diagnostics/24256-stereotactic-breast-biopsy
- Stereotactic and Needle Breast Biopsy — StatPearls, NCBI Bookshelf. 2023-07-17. https://www.ncbi.nlm.nih.gov/books/NBK559147/
- Breast biopsy – stereotactic — Health Encyclopedia, Florida Health Finder. 2024-01-10. https://quality.healthfinder.fl.gov/health-encyclopedia/HIE/1/007433
Read full bio of Sneha Tete