Stomach Ulcer: Signs, Symptoms, Causes & Treatment
Comprehensive guide to understanding stomach ulcers, their causes, symptoms, and effective treatment options.
What Is a Stomach Ulcer?
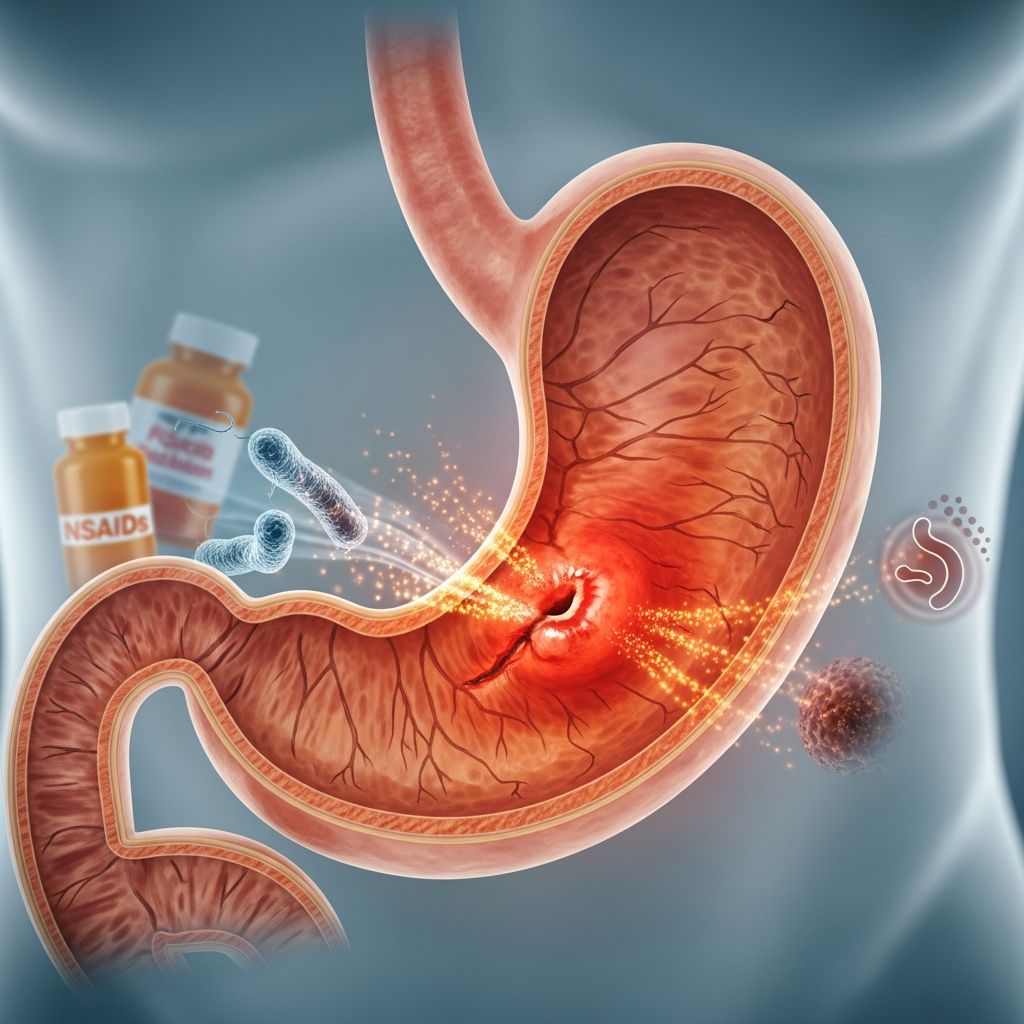
A stomach ulcer, also known as a gastric ulcer, is an open sore that develops in the lining of your stomach. This occurs when stomach acid erodes through the protective mucosa layer that lines your stomach wall. When this protective barrier breaks down, the acidic environment of your stomach can create painful sores that cause significant discomfort and digestive issues.
The stomach naturally produces acid to help digest food, but this acid is kept in check by a protective mucus layer. When this balance is disrupted, ulcers can form. While many people experience occasional heartburn, a true stomach ulcer represents a more serious condition that requires medical attention and proper treatment to heal effectively.
Common Causes of Stomach Ulcers
Understanding what causes stomach ulcers is essential for both treatment and prevention. The two most common culprits behind stomach ulcer development are:
Helicobacter pylori (H. pylori) Infection
H. pylori is a bacterium that infects the stomach lining and is one of the leading causes of peptic ulcers worldwide. This infection can persist for years without symptoms and may be passed from person to person through contaminated food or water. When present in your stomach, H. pylori damages the protective mucus layer, allowing acid to create ulcers. Healthcare providers now recommend testing for H. pylori in all patients suspected of having peptic ulcer disease, as identifying and treating this infection is crucial for ulcer healing and prevention of recurrence.
Nonsteroidal Anti-Inflammatory Drugs (NSAIDs)
Regular use of NSAIDs such as ibuprofen, naproxen, and aspirin represents another major cause of stomach ulcers. These medications can erode the protective lining of your stomach and increase acid production, making ulcer formation more likely. People who use these pain relievers frequently, particularly older adults and those with chronic pain conditions, face a higher risk of developing ulcers.
Other Contributing Factors
While H. pylori and NSAIDs account for most stomach ulcers, other factors can contribute to their development. Excessive alcohol consumption can irritate the stomach lining and increase acid production. Severe stress may also play a role in some cases. Certain medical conditions, such as Zollinger-Ellison syndrome, which causes your stomach to produce excessive amounts of acid, can lead to chronic ulcers. Additionally, smoking has been linked to increased ulcer risk and slower healing.
Recognizing Stomach Ulcer Symptoms
Stomach ulcer symptoms can vary widely among individuals, ranging from mild discomfort to severe pain. The most common symptom is a burning sensation in your stomach, often described as gnawing or aching pain. This burning pain typically occurs between meals when your stomach is empty, as acid contacts the ulcer directly. Some people experience this discomfort at night, which can interrupt sleep patterns.
Beyond burning pain, stomach ulcers can cause indigestion, bloating, heartburn, and loss of appetite. Some individuals report feeling uncomfortably full after eating only small amounts of food. Nausea may accompany these symptoms, and some people experience vomiting. In more severe cases, you might notice dark or bloody stools, or vomit that contains blood, which indicates internal bleeding and requires immediate medical attention.
It’s important to note that symptom timing differs based on ulcer location. Epigastric pain from gastric ulcers usually occurs within 15-30 minutes following a meal, while pain from duodenal ulcers (in the upper small intestine) typically develops 2-3 hours after eating.
Diagnosis of Stomach Ulcers
If you suspect you have a stomach ulcer, your healthcare provider will begin with a thorough evaluation. This typically starts with a detailed medical history and physical examination. During this consultation, your provider will ask about your symptoms, when they began, and whether they worsen when your stomach is empty. They’ll also inquire about your current medications, particularly pain relievers and anti-inflammatory drugs.
Your provider will review your personal medical history, including any family history of ulcers or H. pylori infection, major stresses, and recent life changes. All medications, vitamins, and supplements you take will be documented, as these can influence ulcer development and treatment options.
Diagnostic Tests
Several tests can confirm an ulcer diagnosis:
- Upper Endoscopy: This is the most definitive test for stomach ulcers. A long, flexible tube called an endoscope, equipped with a tiny camera, is passed down your throat into your esophagus and stomach. This allows your healthcare provider to visualize the ulcer directly and assess its severity. During endoscopy, tissue samples may be taken to test for H. pylori.
- H. pylori Testing: If H. pylori infection is suspected, your provider may perform a breath test, stool test, or blood test to detect the bacteria.
- Additional Imaging: X-rays or other imaging studies may be ordered in certain cases to evaluate the extent of the ulcer or check for complications.
Treatment Options for Stomach Ulcers
Healthcare providers treat most stomach ulcers with a combination of medications designed to reduce stomach acid, protect the ulcer during healing, and eliminate any bacterial infection. The specific treatment plan depends on the underlying cause of your ulcer.
Medications for Acid Reduction
Two main classes of medications are used to reduce stomach acid:
Proton Pump Inhibitors (PPIs)
PPIs are among the most effective medications for treating ulcers. These drugs work by blocking the production of stomach acid at its source, the proton pumps in stomach cells. By significantly reducing acid production, PPIs allow the ulcer to heal while also coating and protecting the stomach lining. Common PPIs include omeprazole (Prilosec), lansoprazole (Prevacid), and esomeprazole (Nexium). You typically take PPIs for several weeks as part of your treatment regimen.
Histamine Receptor Blockers (H2 Blockers)
H2 blockers reduce stomach acid by blocking the chemical signals that tell your body to produce it. These medications include famotidine (Pepcid) and ranitidine. While slightly less potent than PPIs, H2 blockers remain effective treatment options, particularly for milder ulcers or as maintenance therapy.
Protective Coating Agents
Sucralfate forms a protective barrier directly over the ulcer, shielding it from stomach acid while it heals. This medication is particularly useful for protecting the ulcer during the healing process and is often used in combination with acid-reducing drugs.
Antibiotic Therapy
If H. pylori infection is confirmed, antibiotics are essential for successful treatment. The most common approach involves triple-drug therapy combining a proton pump inhibitor with two different antibiotics. This combination effectively eliminates the H. pylori bacteria and prevents ulcer recurrence. Typical antibiotic combinations may include clarithromycin, amoxicillin, or metronidazole, taken for 10-14 days.
Over-the-Counter Options
While over-the-counter medications like antacids (calcium carbonate, magnesium hydroxide) and bismuth subsalicylate can provide temporary symptom relief, they won’t heal your ulcer. These should only be used as temporary measures while you seek proper medical care. Relying solely on OTC medications without addressing the underlying cause allows the ulcer to persist and potentially worsen.
Lifestyle Modifications to Support Healing
Your healthcare provider may recommend specific lifestyle changes to help your stomach heal and prevent future ulcers:
- Avoid NSAIDs or reduce their usage under medical supervision
- Limit or eliminate alcohol consumption
- Stop smoking, as it delays ulcer healing
- Manage stress through relaxation techniques, exercise, or counseling
- Eat smaller, more frequent meals rather than large meals
- Avoid foods that trigger symptoms, such as spicy or acidic foods
- Maintain a consistent sleep schedule
- Stay hydrated by drinking adequate water
Treating Complicated Ulcers
Most people respond well to medical treatment, but some ulcers develop complications requiring additional intervention. If your ulcer causes internal bleeding, your provider can treat this during endoscopy by cauterizing the blood vessel or injecting medication directly into the wound to stop the bleeding.
In rare cases where an ulcer creates a hole (perforation) in your stomach or intestine, emergency surgery may be necessary. A colorectal surgeon can repair this perforation to prevent life-threatening complications like peritonitis or sepsis. While surgical treatment is uncommon, it may be essential for severe, untreated ulcers.
Long-Term Management and Prevention
Most people require only short-term ulcer treatment before achieving complete healing. However, some individuals have chronic conditions that lead to recurrent ulcers. Zollinger-Ellison syndrome, which causes excessive stomach acid production, may require long-term PPI therapy to prevent ulcer recurrence.
After completing your initial treatment course, your healthcare provider will follow up within a few weeks to ensure your symptoms are improving. If symptoms persist or worsen, additional evaluation may be necessary. Regular check-ins help your provider monitor your recovery and adjust treatment if needed.
To prevent future ulcers, take these preventive steps:
- If you must use NSAIDs, take the lowest effective dose for the shortest time possible, and discuss protective measures with your provider
- If H. pylori is detected in household members, consider family screening and treatment
- Maintain a healthy diet rich in fruits, vegetables, and lean proteins
- Manage stress through regular exercise and relaxation techniques
- Seek prompt treatment for any H. pylori infections
- Avoid smoking and excessive alcohol
Frequently Asked Questions About Stomach Ulcers
Q: Can stress cause stomach ulcers?
A: While stress alone doesn’t directly cause ulcers, it can increase stomach acid production and worsen existing ulcers. The primary causes remain H. pylori infection and NSAID use. However, managing stress is an important part of ulcer treatment and prevention.
Q: How long does it take for a stomach ulcer to heal?
A: With proper treatment, most stomach ulcers heal within 4-8 weeks. The exact timeline depends on the ulcer’s size, severity, and your adherence to treatment. Continuing medications as prescribed is essential for complete healing.
Q: Are stomach ulcers contagious?
A: The ulcer itself is not contagious, but H. pylori infection, which causes many ulcers, can be transmitted from person to person through contaminated food or water. If you have H. pylori, practicing good hygiene helps prevent spreading the infection to others.
Q: Can I eat normally with a stomach ulcer?
A: You should modify your diet while healing. Eat smaller meals more frequently, avoid spicy or highly acidic foods, limit caffeine and alcohol, and avoid foods that trigger your symptoms. Once healed, you can gradually return to a normal diet.
Q: Do I need surgery for my stomach ulcer?
A: Most stomach ulcers heal with medication alone. Surgery is rarely needed unless your ulcer causes serious complications like perforation or severe bleeding that cannot be controlled endoscopically.
Q: What should I do if my symptoms return after treatment?
A: Contact your healthcare provider immediately if symptoms return or worsen. This may indicate treatment failure, reinfection with H. pylori, or continued NSAID use. Your provider can adjust your treatment plan accordingly.
References
- Peptic Ulcer Disease — National Center for Biotechnology Information (NCBI) Bookshelf. 2024. https://www.ncbi.nlm.nih.gov/books/NBK534792/
- Stomach Ulcer: Signs, Symptoms, Causes & Treatment — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/22314-stomach-ulcer
- Peptic Ulcer – Diagnosis and Treatment — Mayo Clinic. 2023. https://www.mayoclinic.org/diseases-conditions/peptic-ulcer/diagnosis-treatment/drc-20354229
- Proton Pump Inhibitors (PPIs): What They Are & Side Effects — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/articles/proton-pump-inhibitors
- Sucralfate (Carafate): Uses & Side Effects — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/drugs/20284-sucralfate-tablets
- A Clinician’s Guide to Managing Helicobacter pylori Infection — Cleveland Clinic Journal of Medicine. 2005. https://www.ccjm.org/content/72/2/109
Read full bio of medha deb











