Subcutaneous Fat Necrosis of the Newborn
Rare self-limiting panniculitis in newborns: firm nodules, hypercalcemia risks, and vigilant monitoring essential for complications.
Author: Dermatological Society Revised: January 2026
What is subcutaneous fat necrosis of the newborn?
Subcutaneous fat necrosis of the newborn (SCFN), also known as adiponecrosis subcutanea neonatorum or subcutaneous fat necrosis, is a rare, self-limiting form of lobar panniculitis that occurs in the adipose (fat) tissue of full-term or post-term newborns, typically within the first six weeks of life. It manifests as firm, indurated plaques or erythematous to violaceous nodules, primarily on the cheeks, back, buttocks, thighs, and proximal extremities, sparing the abdomen and chest in most cases. SCFN is usually benign and resolves spontaneously without scarring over weeks to months, but it carries significant risks of metabolic complications, particularly hypercalcemia, which affects up to 50-100% of monitored cases and can be life-threatening if untreated.
The condition arises from necrosis (death) of subcutaneous adipocytes due to ischemic injury, often triggered by perinatal stressors. Brown fat in newborns, more sensitive to hypoxia than adult white fat, contributes to vulnerability. While the exact pathogenesis remains unclear, SCFN does not recur and is distinct from other neonatal panniculitides like sclerema neonatorum.
Who gets subcutaneous fat necrosis of the newborn?
SCFN predominantly affects full-term or post-term infants (gestational age ≥37 weeks), with 84% born at term in one retrospective study of 32 cases. It is more common in males (slight predominance) and infants of normal weight for gestational age (69%). Risk is elevated in complicated deliveries: 53% had obstetric complications, including 58% born via cesarean section. Maternal factors like preeclampsia or diabetes may precipitate it, alongside neonatal stressors.
In a cohort analysis, 91% of infants undergoing therapeutic hypothermia for hypoxic-ischemic encephalopathy (HIE) developed SCFN, highlighting cooling therapy as a modern risk factor. Incidence is rare, estimated at <1% of newborns, but likely underdiagnosed due to mild cases resolving unnoticed.
What causes subcutaneous fat necrosis of the newborn?
The precise etiology is unknown, but multifactorial perinatal insults to subcutaneous fat are implicated. Key triggers include:
- Birth trauma and hypoxia: Asphyxia, meconium aspiration, umbilical cord prolapse.
- Thermoregulatory stress: Hypothermia or therapeutic hypothermia for HIE (91% association).
- Maternal conditions: Preeclampsia, gestational diabetes.
- Obstetric interventions: Forceps/vacuum delivery, cesarean sections.
These factors cause local ischemia in fat lobules, leading to inflammation, saponification (fatty acid soap formation), and foreign body giant cell reaction. Crystal formation (e.g., sodium, calcium) within adipocytes exacerbates necrosis.
What are the clinical features of subcutaneous fat necrosis of the newborn?
Lesions typically emerge 6-10 days post-birth (92% within 28 days; 56% in first week), evolving over 2-4 weeks before regressing. Characteristics include:
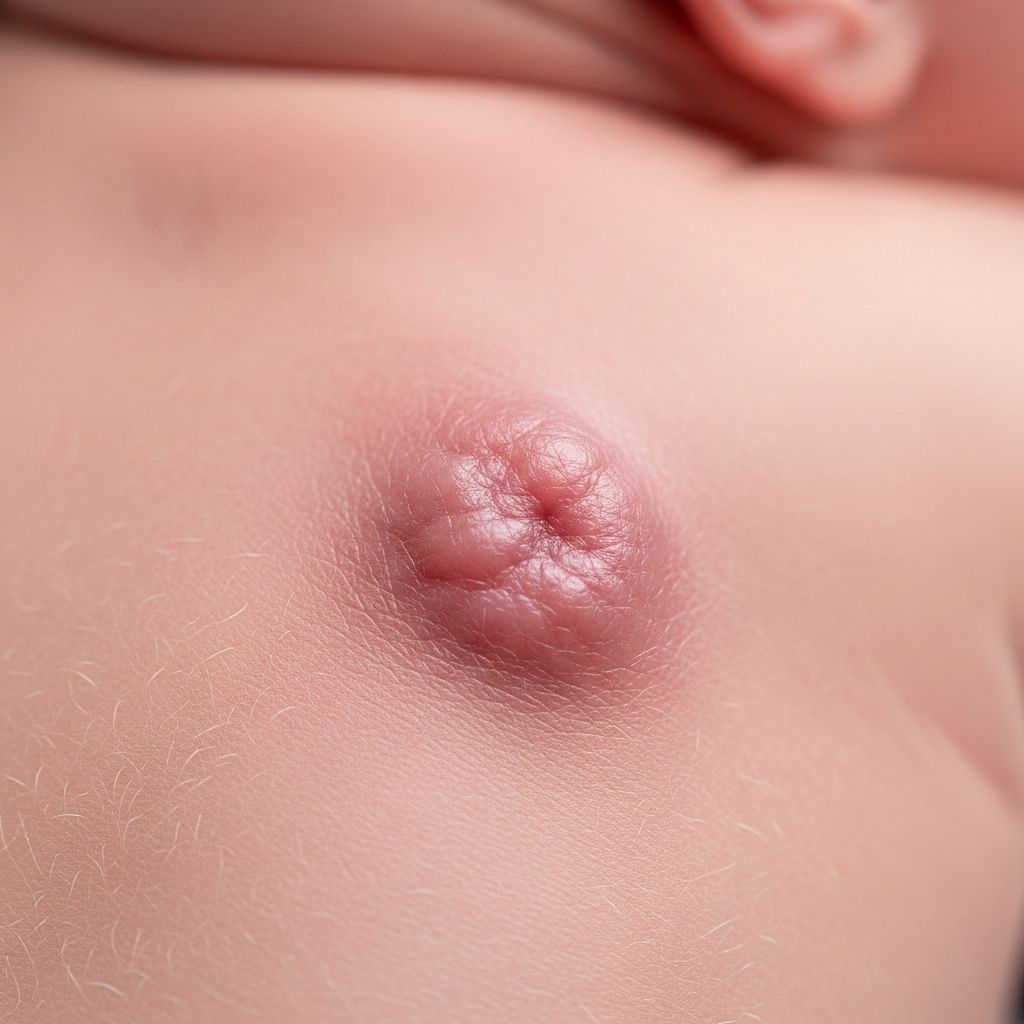
- Morphology: Firm, mobile subcutaneous nodules (100%) or plaques; 0.5-8 cm diameter; red, purple, or bruised hue (73%).
- Sites: Back/buttocks (most common), cheeks, arms/shoulders (57%), thighs, calves; rare scalp involvement with alopecia.
- Symptoms: Tender/painful (23%); indurated; may soften, ulcerate, drain chalky white-brown oily fluid.
No fever or systemic illness at onset in healthy vigorous infants. Complications manifest later: hypercalcemia (50-100%), hypertriglyceridemia, thrombocytopenia, hypoglycemia, anemia.
| Feature | Frequency | Description |
|---|---|---|
| Subcutaneous nodules | 100% | Firm, mobile lumps |
| Erythema | 73% | Red-purple discoloration |
| Pain/Tenderness | 23% | Lesion-specific |
| Swelling | 13% | Localized edema |
How is subcutaneous fat necrosis of the newborn diagnosed?
Diagnosis combines clinical presentation, history of perinatal stress, and imaging; biopsy is rarely needed. Key diagnostics:
- Clinical: Characteristic sites, full-term healthy infant.
- Ultrasound: Hyperechoic subcutaneous masses ± calcifications; Doppler shows preserved vascularity.
- Biopsy (if atypical): Lobar panniculitis with fat necrosis, needle-shaped clefts (cholesterol), multinucleated giant cells, inflammatory infiltrate; no vasculitis.
Differential includes sclerema neonatorum (diffuse, ill infants), neonatal cold injury, erythema nodosum, metastatic neuroblastoma, juvenile xanthogranuloma.
What is the treatment for subcutaneous fat necrosis of the newborn?
Supportive care is mainstay, as SCFN self-resolves in 1-6 months without intervention. Lesions require no specific therapy unless ulcerated (wound care). Focus on complication surveillance:
- Hypercalcemia management: Monitor ionized calcium weekly x4, then monthly x3 months. Treat if >1.6 mmol/L symptomatic or persistent: hydration, low-calcium formula, furosemide, corticosteroids, bisphosphonates (pamidronate); endocrinology consult.
- Symptomatic relief: Analgesics for pain.
- Follow-up: Renal ultrasound for nephrocalcinosis (seen in some).
No role for antibiotics unless secondary infection. Hypercalcemia peaks at 1-3 months, resolves by 6 months.
What is the outcome for subcutaneous fat necrosis of the newborn?
Excellent prognosis: skin lesions resolve completely without atrophy or scarring. Complications like hypercalcemia (100% in monitored cohorts) are transient but mandate vigilance—3/32 cases symptomatic, 2 nephrocalcinosis, 1 AKI. Rare fatalities from untreated severe hypercalcemia (seizures, cardiac arrhythmias). Early detection prevents morbidity; no long-term sequelae post-resolution.
Peak ionized calcium <1.5 mmol/L predicts low complication risk.
Frequently asked questions about subcutaneous fat necrosis of the newborn
Q: Is subcutaneous fat necrosis dangerous?
A: Primarily benign, but hypercalcemia (up to 100% in tested infants) can cause serious issues like seizures if unmanaged. Routine monitoring essential.
Q: When does hypercalcemia occur with SCFN?
A: 86% diagnosed within 28 days; peaks early neonatal period to 3 months. Monitor first 3 months.
Q: Can SCFN be prevented?
A: Not reliably, but minimizing birth trauma/hypoxia helps. High-risk infants (HIE cooling) need skin checks.
Q: Does SCFN leave scars?
A: No, resolves without scarring.
Q: How common is SCFN after therapeutic hypothermia?
A: Up to 91% in HIE-treated infants.
Related topics
- Sclerema neonatorum
- Neonatal lupus erythematosus
- Panniculitis
- Hypercalcaemia of infancy
References
- Subcutaneous fat necrosis of the newborn — Wikipedia. 2023. https://en.wikipedia.org/wiki/Subcutaneous_fat_necrosis_of_the_newborn
- Subcutaneous Fat Necrosis of the Newborn — MD Searchlight. 2023. https://mdsearchlight.com/child-health/subcutaneous-fat-necrosis-of-the-newborn/
- Subcutaneous fat necrosis of the newborn: A retrospective study — Wiley Online Library (Pediatric Dermatology). 2022-12-21. https://onlinelibrary.wiley.com/doi/full/10.1111/pde.15219
- Subcutaneous Fat Necrosis of the Newborn — NCBI StatPearls. 2023. https://www.ncbi.nlm.nih.gov/books/NBK557745/
- Fat Necrosis — Cleveland Clinic. 2023. https://my.clevelandclinic.org/health/diseases/24187-fat-necrosis
Read full bio of medha deb