Tetralogy of Fallot: Causes, Symptoms, and Treatment
Understanding TOF: A comprehensive guide to this common congenital heart defect.
What is Tetralogy of Fallot?
Tetralogy of Fallot (TOF) is the most common cyanotic congenital heart defect, representing a complex condition that affects the structure of the heart and how blood flows through it. This condition is named after French physician Étienne-Louis Fallot, who first described the anatomical features in the late 19th century, though the defect was initially documented by Danish monk Niels Stenson in 1671. TOF is characterized by four distinct heart abnormalities that occur together, disrupting the normal circulation of blood between the heart and lungs.
The condition results from improper development of the fetal heart during pregnancy, creating structural problems that persist after birth. While TOF is a serious cardiac condition, remarkable advances in surgical techniques and medical management over the past several decades have dramatically improved outcomes for affected individuals.
The Four Defects of Tetralogy of Fallot
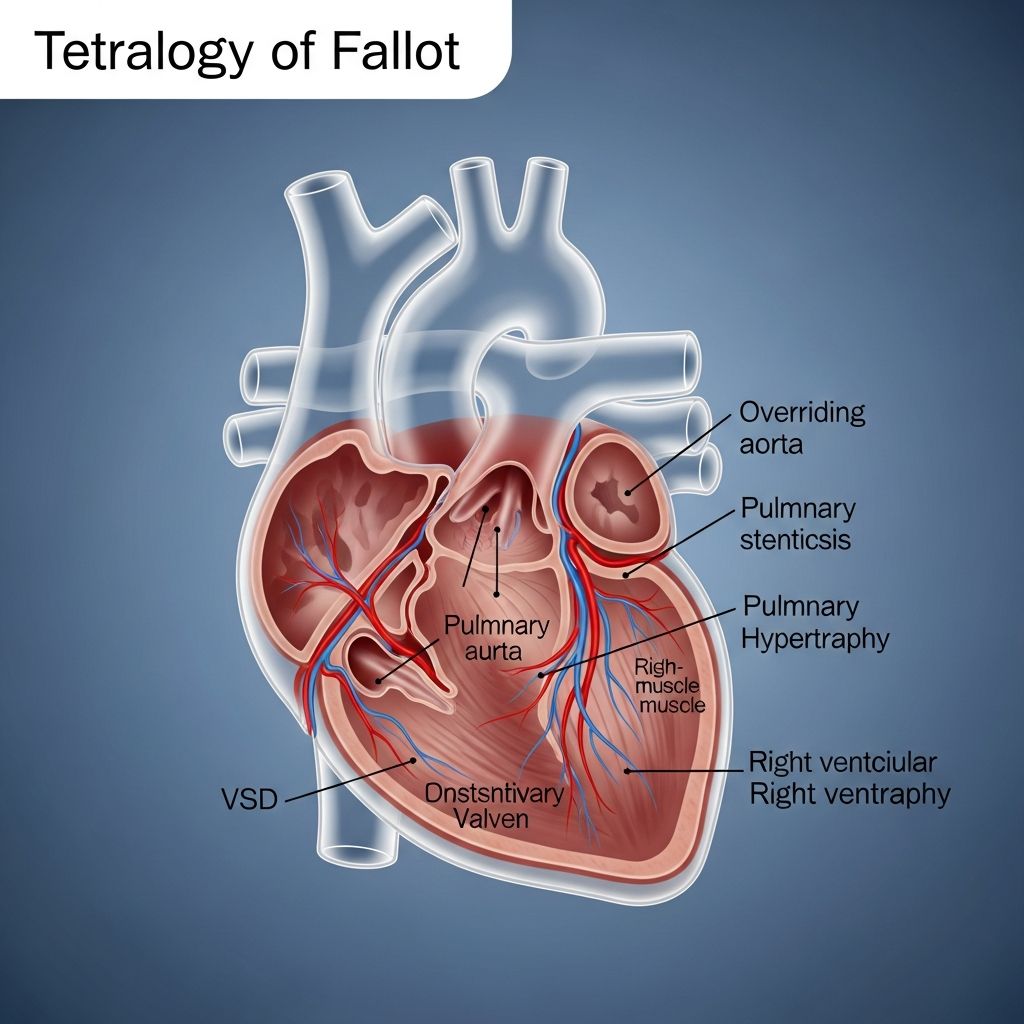
Tetralogy of Fallot consists of four interconnected heart abnormalities that work together to disrupt normal blood circulation:
1. Ventricular Septal Defect (VSD)
A hole exists in the wall (septum) that separates the two lower chambers (ventricles) of the heart. This opening allows oxygen-poor blood from the right ventricle to mix with oxygen-rich blood from the left ventricle, reducing the oxygen content of blood pumped to the body.
2. Pulmonary Stenosis
The pulmonary valve, which controls blood flow from the right ventricle to the lungs, is narrowed and thickened. This stenosis restricts the amount of blood that can reach the lungs to pick up oxygen.
3. Right Ventricular Hypertrophy
Due to the increased workload required to pump blood through the narrowed pulmonary valve, the right ventricle becomes thickened and enlarged over time, reducing its efficiency.
4. Overriding Aorta
The aorta, which normally arises from the left ventricle, is positioned over the ventricular septal defect. This allows it to receive blood from both the right and left ventricles, further mixing oxygenated and deoxygenated blood.
Causes and Risk Factors
Tetralogy of Fallot develops during fetal heart development, typically between weeks 2 and 8 of pregnancy when the heart is forming. The exact cause of TOF remains incompletely understood, though several factors may increase the risk of development:
- Genetic factors: Certain genetic mutations and chromosomal abnormalities increase TOF risk. Children with Down syndrome (trisomy 21) have an elevated incidence of TOF.
- Maternal factors: Maternal diabetes, rubella infection during pregnancy, or use of certain medications like retinoids may increase risk.
- Environmental exposures: Maternal exposure to certain chemicals or toxins during early pregnancy may contribute to heart defects.
- Family history: Having a parent or sibling with TOF slightly increases the risk of developing the condition.
Symptoms and Signs
The severity of symptoms in TOF varies widely depending on the degree of pulmonary stenosis and the size of the ventricular septal defect. Some infants present with severe symptoms immediately after birth, while others may have mild symptoms that develop gradually.
Cyanosis (“Blue Baby” Appearance)
The most distinctive sign of TOF is cyanosis, a bluish or purplish discoloration of the skin, lips, and fingernails caused by insufficient oxygen in the blood. However, only a small percentage of TOF patients present with deep cyanosis in the neonatal period. Cyanosis may worsen with crying, feeding, or exertion as the condition affects oxygen delivery throughout the body.
Other Common Symptoms
- Shortness of breath or rapid breathing
- Difficulty feeding or failure to thrive
- Fatigue and poor exercise tolerance
- Chest pain or discomfort during activity
- Squatting position (children may instinctively squat to improve blood flow)
- Clubbing of fingers and toes (thickening and enlargement)
- Fainting or loss of consciousness
- Irritability or difficulty sleeping
Diagnosis
Diagnosis of Tetralogy of Fallot typically begins with clinical evaluation and is confirmed through advanced imaging techniques.
Physical Examination
A pediatric cardiologist will listen for abnormal heart sounds (murmurs) using a stethoscope and observe for signs of cyanosis or other physical indicators of heart disease.
Echocardiography
Transthoracic echocardiography is the primary diagnostic tool, using ultrasound waves to visualize the heart structure and blood flow patterns. This non-invasive technique clearly shows the four characteristic defects of TOF and assesses the severity of each abnormality. Fetal echocardiography may detect TOF during prenatal screening.
Chest X-ray
A chest X-ray may show characteristic features including a boot-shaped heart appearance and reduced pulmonary blood flow.
Electrocardiogram (ECG)
An ECG records the electrical activity of the heart, often showing right ventricular hypertrophy patterns typical of TOF.
Cardiac Catheterization
In some cases, cardiac catheterization may be performed to measure oxygen saturation levels in different heart chambers and assess the precise anatomy before surgery.
Treatment Options
Treatment of Tetralogy of Fallot depends on the severity of symptoms and the degree of cardiac compromise. While medication may provide temporary relief, surgical repair is the definitive treatment.
Medical Management
Before surgical repair, certain medications may improve symptoms and stabilize the patient:
- Prostaglandin E1 (PGE1): Keeps the ductus arteriosus (a fetal blood vessel) open, improving pulmonary blood flow in critically ill newborns.
- Beta-blockers: Reduce the force of heart contractions and improve diastolic filling, decreasing right-to-left shunting.
- Diuretics: Help manage fluid overload if heart failure develops.
- Antibiotics: Prophylactic antibiotics prevent endocarditis (heart infection) in some patients.
Surgical Repair
Surgical correction of TOF is the definitive treatment and represents one of the major advances in pediatric cardiac surgery. The landmark “blue baby operation,” performed by Dr. Alfred Blalock in 1944 at Johns Hopkins Hospital, revolutionized TOF treatment. This historic procedure involved creating a shunt to temporarily improve pulmonary blood flow in severely affected infants.
Complete Intracardiac Repair
Modern surgical practice employs complete intracardiac repair, typically performed in infancy or early childhood. This procedure involves:
- Closing the VSD: The ventricular septal defect is closed with a synthetic patch or tissue graft.
- Relieving pulmonary stenosis: The narrowed pulmonary valve and outflow tract are enlarged through valvulotomy or placement of a patch.
- Restoring normal blood flow: The procedure restores normal separation between oxygenated and deoxygenated blood streams.
Successful complete repair typically eliminates the need for future palliative procedures and provides excellent long-term outcomes. The timing of surgery depends on the severity of symptoms, with critically ill neonates requiring urgent intervention while more stable infants may be scheduled electively.
Long-term Management and Outcomes
Advances in surgical technique and postoperative care have dramatically improved survival rates and quality of life for TOF patients. Most children who undergo successful surgical repair lead normal, active lives.
Follow-up Care
Regular cardiology follow-up is essential to monitor for complications and ensure optimal cardiac function:
- Serial echocardiograms assess valve function and ventricular performance
- Periodic ECGs monitor for arrhythmias
- Exercise stress testing evaluates functional capacity
- Endocarditis prophylaxis may be recommended for certain activities
Potential Late Complications
Some individuals may develop complications years after successful repair, including pulmonary regurgitation, right ventricular dysfunction, arrhythmias, or residual obstruction. These may require additional surgical or catheter-based interventions.
Pregnancy and Reproductive Considerations
For women with repaired TOF, pregnancy outcomes are generally favorable if hemodynamics are near normal before conception. However, pregnancy is considered high-risk for untreated or severely affected individuals, with fetal mortality rates reaching 30% and maternal mortality as high as 15% in unoperated patients. Women with TOF should consult with their cardiologist before attempting pregnancy to assess individual risk and determine if additional interventions are necessary.
Frequently Asked Questions
Q: Is Tetralogy of Fallot fatal if untreated?
A: Without treatment, TOF is a serious condition with significant mortality risk, particularly in severely affected individuals. However, many children with mild forms survive into adulthood, though with progressive symptoms. Surgical repair dramatically improves survival and quality of life.
Q: At what age is TOF surgery typically performed?
A: Complete intracardiac repair is usually performed in infancy or early childhood, often between 3 to 6 months of age for stable patients. Critically ill newborns may require earlier intervention or initial palliative procedures.
Q: Can TOF be detected during pregnancy?
A: Yes, fetal echocardiography can detect TOF during prenatal screening, typically in the second or third trimester. This allows for delivery planning at a facility equipped for neonatal cardiac care.
Q: What is the long-term survival rate for TOF?
A: Survival rates have improved dramatically since the introduction of surgical repair. Most children who undergo successful complete intracardiac repair achieve excellent long-term survival and can lead normal, active lives into adulthood.
Q: Can people with repaired TOF participate in sports?
A: Most individuals with successfully repaired TOF can participate in regular recreational activities and sports. However, activity restrictions may be recommended based on individual cardiac status, residual defects, or rhythm abnormalities. Consultation with a cardiologist is essential.
Q: Is TOF hereditary?
A: While most TOF cases are sporadic, having a family history of TOF or other congenital heart defects slightly increases recurrence risk. Genetic counseling may be beneficial for families with multiple affected members.
References
- Tetralogy of Fallot: The first 300 years — National Center for Biotechnology Information (NCBI), National Institutes of Health. 2004. https://pmc.ncbi.nlm.nih.gov/articles/PMC325189/
- Johns Hopkins celebrates 75 years since historic ‘blue baby’ operation — Johns Hopkins Hub. 2019-11-26. https://hub.jhu.edu/2019/11/26/blue-baby-operation/
- Tetralogy of Fallot — Johns Hopkins University, Pediatric Cardiac Surgery, Fifth Edition. 2023. https://pure.johnshopkins.edu/en/publications/tetralogy-of-fallot-6
- Tetralogy of Fallot: Congenital Heart Disease — Cove Point Foundation (Patient Education and Transition to Adulthood for Congenital Heart Disease Patients). https://www.pted.org/?id=tetralogyfallot7
Read full bio of Sneha Tete











