Tinea Capitis Pathology: Essential Clinical Guide
Detailed histopathological examination of tinea capitis, revealing fungal invasion patterns and host responses in scalp infections.
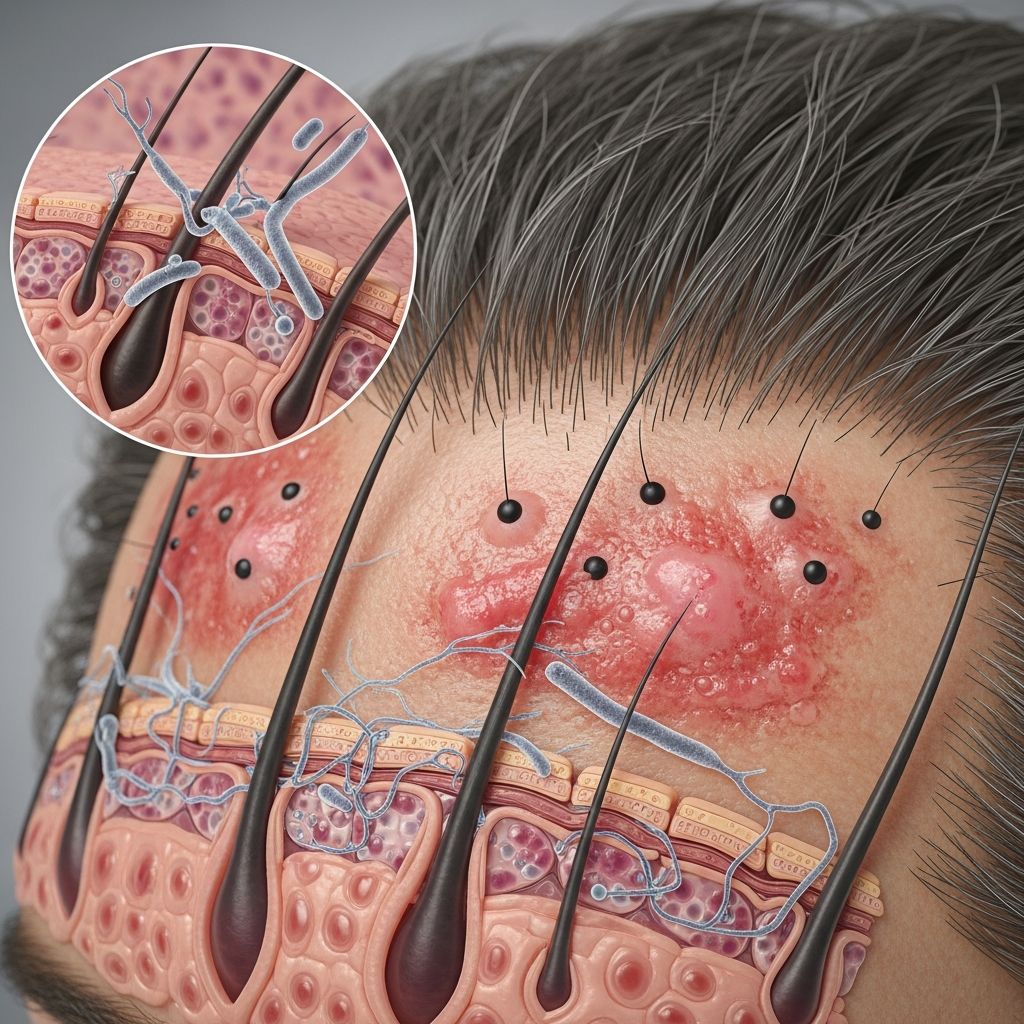
Tinea Capitis Pathology
Dermatophytic infections of the scalp, known as tinea capitis, are characterized by the involvement of the hair shaft by pathogenic fungi. This condition primarily affects children and manifests through distinct patterns of fungal invasion into the hair structure, leading to various clinical and histological features. The pathology is determined by the causative dermatophyte species, which dictate whether the infection is endothrix or ectothrix, influencing the host’s inflammatory response and disease progression.
Authoritative Facts
- Primary Causative Agents: Tinea capitis is caused by dermatophytes such as Trichophyton tonsurans, Trichophyton violaceum, and Microsporum canis, which invade keratinized tissues including hair shafts.
- Age Predominance: Most common in children aged 3-14 years, though it can affect any age, especially immunocompromised individuals.
- Transmission: Spread via direct contact with infected persons, animals, or fomites like combs and hats.
- Histological Hallmarks: Features include hyperkeratosis, parakeratosis, spongiosis, and fungal elements visible with PAS stain.
Introduction to Tinea Capitis Pathology
Tinea capitis, or scalp ringworm, represents a superficial fungal infection targeting the scalp’s hair follicles and shafts. Pathologically, it is defined by the dermatophytes’ ability to penetrate the hair cuticle and colonize the keratin-rich hair structure. Unlike other dermatophytoses, topical treatments are ineffective due to poor penetration to the follicle base, necessitating systemic antifungals. The pathology hinges on the fungus’s invasion pattern: endothrix (internal spores) or ectothrix (external spores), each producing characteristic microscopic appearances.
Endothrix infections, typically from anthropophilic species like T. tonsurans and T. violaceum, show hyphae and spores confined within the hair shaft, leading to brittle hairs that fracture, resulting in ‘black dot’ alopecia. Ectothrix infections, often zoophilic like M. canis, feature hyphae on the hair surface with arthrospores encasing the shaft, causing more visible fluorescence under Wood’s lamp and less severe inflammation. These patterns are crucial for diagnosis, as clinical features alone may mimic bacterial folliculitis or psoriasis.
Pathophysiology of Fungal Invasion
Dermatophytes invade the stratum corneum, descending into the hair follicle. They produce keratinases that degrade the hair shaft’s keratin, allowing proliferation. In endothrix patterns, the fungus grows inside the shaft, forming chains of rectangular spores that distort the hair structure, making it fragile. Ectothrix invasion destroys the cuticle, sheath-like spores form externally, often sheathing the hair in a mosaic pattern visible under microscopy.
The host response varies: non-inflammatory types show minimal epidermal change, while inflammatory kerion forms feature intense granulomatous reactions with abscesses, neutrophils, and potential scarring alopecia. Immunosuppression exacerbates invasion, impairing hair growth and facilitating deeper colonization. Transmission occurs via arthroconidia, resilient spores surviving on fomites for months.
Histological Features
Histopathology of tinea capitis reveals a spectrum from subtle to florid changes. Key findings include:
- Epidermal Changes: Mild hyperkeratosis, parakeratosis, and spongiosis in endothrix types with minimal response.
- Follicular Involvement: Suppurative folliculitis, destruction of follicles, and perivascular lymphocytic infiltrates.
- Fungal Elements: Hyphae and spores within the hair shaft (endothrix) or surrounding it (ectothrix), best highlighted by periodic acid-Schiff (PAS) or Grocott’s methenamine silver (GMS) stains.
- Inflammatory Patterns: Neutrophilic microabscesses in the papillary dermis, granulomatous inflammation in kerions.
| Feature | Endothrix | Ectothrix |
|---|---|---|
| Epidermal Response | Mild hyperkeratosis | Moderate inflammation |
| Hair Shaft | Internal spores, no sheath | External arthrospores sheath |
| Common Agents | T. tonsurans, T. violaceum | M. canis, M. audouinii |
| Wood’s Lamp | Non-fluorescent | Fluorescent green |
Inflammatory variants show chronic dermatitis with follicular suppuration, contrasting the subdued changes in non-inflammatory forms. Dermoscopy aids in vivo diagnosis, revealing ‘comma hairs,’ ‘zigzag hairs,’ and ‘Morse code hairs’ indicative of broken, infected shafts.
Clinical-Pathological Correlation
Pathological patterns correlate with clinical subtypes. Grey patch (ectothrix) shows scaly plaques with dull hairs; black dot (endothrix) features fractured hairs leaving dots; kerion presents boggy, pustular masses with intense histopathology including abscesses and scarring potential. Favus, rare, shows scutula (crusty nodules) with endothrix invasion. Regional lymphadenopathy and eyebrow involvement underscore systemic spread.
Differential Diagnosis in Pathology
- Bacterial Folliculitis: More acute neutrophilic infiltrates without fungal elements.
- Psoriasis: Parakeratosis with Munro microabscesses, no fungi.
- Alopecia Areata: No inflammation or fungi; preserved follicles.
- Seborrheic Dermatitis: Less alopecia, no hair invasion.
Definitive diagnosis requires culture, KOH prep, or biopsy with special stains.
Treatment Implications from Pathology
Understanding invasion patterns guides therapy: oral griseofulvin or terbinafine for 6-8 weeks targets endothrix deeply; adjunctive steroids for kerions reduce inflammation. Screening household contacts prevents reservoirs.
Frequently Asked Questions (FAQs)
Q: What causes the different pathology patterns in tinea capitis?
A: The causative dermatophyte determines endothrix (internal spores, e.g., T. tonsurans) or ectothrix (external sheath, e.g., M. canis) invasion.
Q: How is fungal invasion confirmed histologically?
A: PAS or GMS stains highlight hyphae and spores within or around the hair shaft.
Q: Can tinea capitis pathology lead to permanent hair loss?
A: Yes, inflammatory kerion types cause scarring alopecia due to follicular destruction.
Q: Is Wood’s lamp useful in pathological diagnosis?
A: It fluoresces ectothrix infections green but not endothrix, aiding preliminary assessment.
Q: What is the role of dermoscopy in pathology?
A: Reveals zigzag, comma, and corkscrew hairs correlating with shaft weakening and invasion.
Conclusion
Tinea capitis pathology underscores the intricate interplay between dermatophytes and host hair structures, with invasion patterns dictating clinical severity and management. Early histopathological recognition ensures targeted therapy, preventing complications like scarring.
References
- Tinea Capitis – StatPearls — NCBI Bookshelf/StatPearls Publishing. 2023-10-01. https://www.ncbi.nlm.nih.gov/books/NBK536909/
- Tinea Capitis — DermNet NZ. 2023. https://dermnetnz.org/topics/tinea-capitis
- Tinea Capitis – Fungal Skin Infections — DermNet NZ CME. 2023. https://dermnetnz.org/cme/fungal-infections/tinea-capitis
- Tinea Capitis Pathology — DermNet NZ. 2023. https://dermnetnz.org/topics/tinea-capitis-pathology
- Tinea Capitis — DermNet NZ Image Detail. 2023. https://dermnetnz.org/imagedetail/2118-tinea-capitis
- Tinea Capitis Images — DermNet NZ. 2023. https://dermnetnz.org/images/tinea-capitis-images
Read full bio of Sneha Tete











