Tinea Cruris (Jock Itch): Symptoms, Diagnosis, Treatment Guide
Comprehensive guide to jock itch: causes, symptoms, diagnosis, treatment, and prevention strategies for effective management.
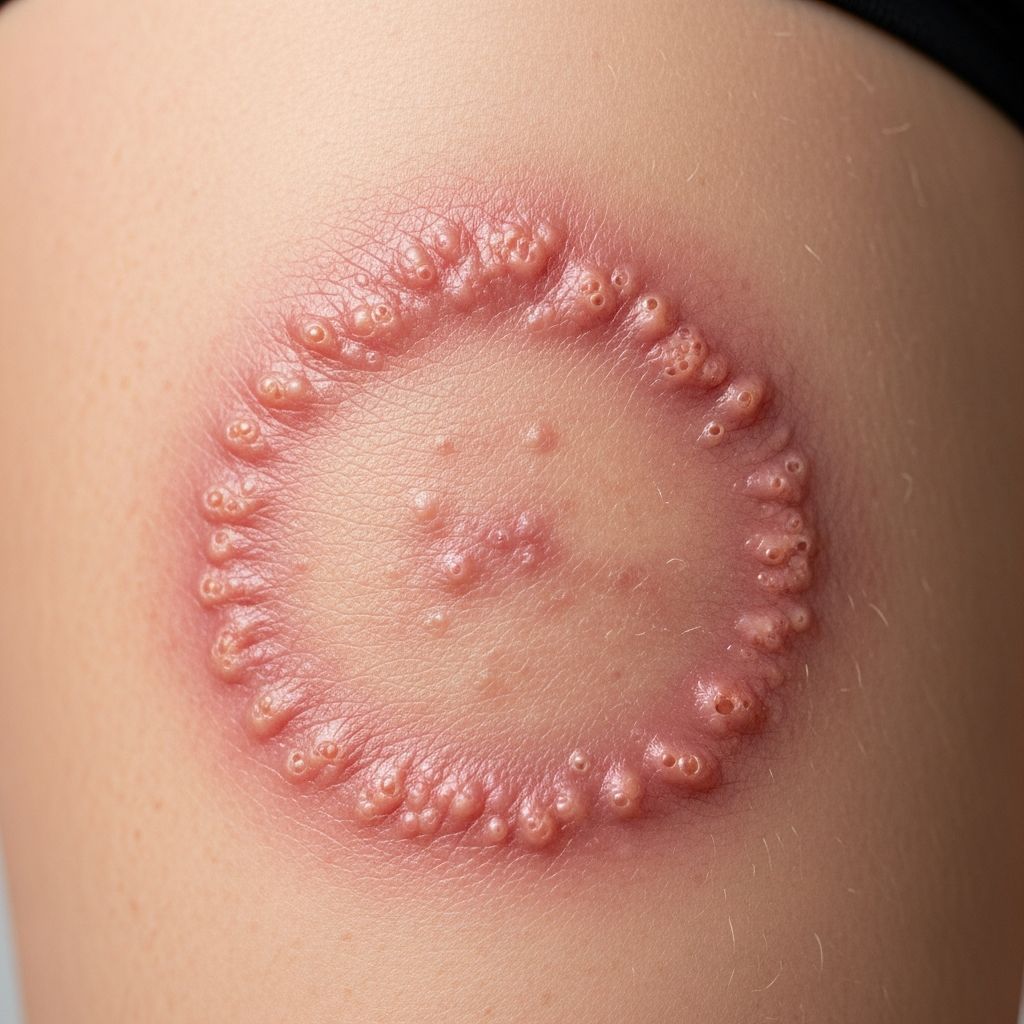
Tinea Cruris
Tinea cruris, commonly known as
jock itch
, is a superficial fungal infection caused by dermatophytes affecting the groin, pubic region, and adjacent thighs. This condition thrives in warm, moist environments, leading to an itchy, erythematous rash that can significantly impact quality of life if untreated.Introduction
**Tinea cruris** represents a dermatophyte infection specifically targeting intertriginous areas of the inguinal folds, perineum, and perianal region. Dermatophytes are keratinophilic fungi that invade the stratum corneum, hair, and nails, producing a characteristic annular rash with scaling and inflammation. The infection is more prevalent in males due to anatomical factors but can affect anyone in humid climates or with predisposing risk factors.
Globally, tinea cruris accounts for a substantial portion of superficial mycoses consultations. Its asymmetrical presentation and tendency to spare the scrotum distinguish it clinically. Early recognition and appropriate management are crucial to prevent chronicity and complications.
Demographics
Tinea cruris predominantly affects adult males, particularly those aged 20-50 years, with a higher incidence in tropical and subtropical regions. Risk is elevated among athletes, obese individuals, and those engaging in activities promoting sweating, such as sports or manual labor.
- Male-to-female ratio: Approximately 3:1, attributed to tighter clothing and scrotal involvement being less common in women.
- Geographic prevalence: Higher in humid climates; up to 20-30% of dermatology consultations in endemic areas.
- Age distribution: Rare in prepubertal children; peaks in young adulthood.
- Socioeconomic factors: More common in lower socioeconomic groups due to shared facilities and hygiene challenges.
Causes
The primary causative agents are anthropophilic dermatophytes, with
Trichophyton rubrum
being the most frequent isolate worldwide (50-90% of cases), followed byEpidermophyton floccosum
andTrichophyton mentagrophytes
complex. Zoophilic species likeTrichophyton verrucosum
are less common but more inflammatory.Infection typically spreads autogenously from distant sites such as tinea pedis (athlete’s foot) via contaminated hands, towels, or clothing. Direct person-to-person transmission occurs in communal settings like locker rooms. Fungi proliferate in occluded, macerated skin with elevated pH.
Risk Factors
- Excessive sweating (hyperhidrosis)
- Tight, occlusive clothing (e.g., synthetic underwear)
- Obesity and diabetes mellitus
- Immunosuppression (HIV, corticosteroids)
- Concurrent tinea pedis or onychomycosis
- Poor hygiene and shared facilities
Clinical Features
The hallmark is an
erythematous, annular plaque
with a scaly, raised advancing border and central clearing, originating in the inguinal crease and extending to the inner thighs, rarely crossing the midline or involving the scrotum.Symptoms include intense pruritus, burning, and stinging, exacerbated by sweating or friction. Acute lesions are bright red and vesiculopustular; chronic forms show hyperpigmentation and lichenification.
| Feature | Description |
|---|---|
| Shape | Annular with trailing scale |
| Color | Erythematous border, paler center |
| Symptoms | Itch, burn; pustules possible |
| Distribution | Unilateral/bilateral groin, spares scrotum |
Complications
Untreated tinea cruris can lead to secondary bacterial superinfection, chronic lichenified plaques, and rarely
Majocchi’s granuloma
—a deep follicular invasion causing nodular lesions. Misuse of topical steroids may induce tinea incognito, masking the fungal etiology and promoting dissemination.- Cellulitis from scratching
- Post-inflammatory hyperpigmentation
- Recurrent episodes eroding quality of life
- Dermatophytid (id) reactions—distant eczematous flares
Diagnosis
Diagnosis is primarily clinical but confirmed by
KOH microscopy
revealing hyphae or fungal culture/skin scraping PCR. Wood’s lamp may fluoresce green with Microsporum species (rare).- History: Itch, risk factors, tinea elsewhere
- Examination: Annular scaly plaques
- Microscopy: 10-20% KOH prep showing septate hyphae
- Culture: Sabouraud agar for speciation (if resistant)
- Biopsy: Rarely for atypical cases
Differential Diagnoses
| Condition | Key Distinguishing Features |
|---|---|
| Candidiasis | Satellite pustules, beefy red, no central clearing |
| Erythrasma | Coral-red Wood’s lamp fluorescence, no scale |
| Psoriasis | Symmetrical, nail pits, extensor involvement |
| Seborrhoeic dermatitis | Greasy scales, central face involvement |
| Contact dermatitis | Irregular borders, allergen history |
| Intertrigo | Bacterial overgrowth, foul odor |
Treatment
Topical antifungals are first-line for localized disease, with
allylamines
(terbinafine 1% cream BID x2 weeks) superior to azoles due to fungicidal action and shorter duration. Azoles (clotrimazole, miconazole) are alternatives.Topical Therapy
- Terbinafine/butenafine: 1-2 weeks, highest cure rates
- Azoles: 2-4 weeks
- Extend 1-2 cm beyond lesion; continue 1 week post-clearing
Systemic Therapy
Indicated for extensive, recalcitrant, or immunocompromised cases.
| Agent | Dose | Duration | Notes |
|---|---|---|---|
| Terbinafine | 250 mg daily | 2 weeks | First-line; monitor LFTs |
| Fluconazole | 150-200 mg weekly | 2-4 weeks | Alternative |
| Itraconazole | 200 mg daily | 1 week | Short course |
Avoid combination steroid-antifungals long-term due to atrophy risk; nystatin ineffective against dermatophytes.
Adjunctive Measures
- Keep dry: Absorbent powders (talc-free)
- Loose cotton underwear
- Treat concurrent tinea pedis
- Hygiene: Daily showers, dry thoroughly
Outcome
With appropriate therapy, cure rates exceed 80-90% within 2-4 weeks. Recurrence occurs in 20-50% without prevention; patient education is key. Monitor diabetics and immunocompromised for dissemination.
Frequently Asked Questions (FAQs)
Q: Is tinea cruris contagious?
A: Yes, via direct contact or fomites; avoid sharing towels.
Q: Can I use over-the-counter creams?
A: Yes, terbinafine or clotrimazole for mild cases; see doctor if no improvement in 2 weeks.
Q: How long until symptoms resolve?
A: 1-4 weeks with treatment; continue therapy post-resolution.
Q: Does jock itch affect women?
A: Less commonly, but possible in perineal folds.
Q: Can steroids treat jock itch?
A: No, they worsen it; use antifungals only.
References
- Tinea Cruris – StatPearls — NCBI Bookshelf. 2023-08-08. https://www.ncbi.nlm.nih.gov/books/NBK554602/
- Understanding Tinea Cruris — UMass Memorial Health. 2023. https://www.ummhealth.org/health-library/understanding-tinea-cruris
- Tinea Cruris — DermNet NZ. 2023. https://dermnetnz.org/topics/tinea-cruris
- Diagnosis and Management of Tinea Infections — American Academy of Family Physicians (AAFP). 2014-11-15. https://www.aafp.org/pubs/afp/issues/2014/1115/p702.html
- Jock Itch (Tinea Cruris) — Cleveland Clinic. 2023. https://my.clevelandclinic.org/health/diseases/22141-jock-itch-tinea-cruris
Read full bio of medha deb












