Toxic Erythema Of The Newborn: Causes, Signs, When To Worry
A comprehensive guide to recognising, understanding, and managing this common, harmless newborn rash.
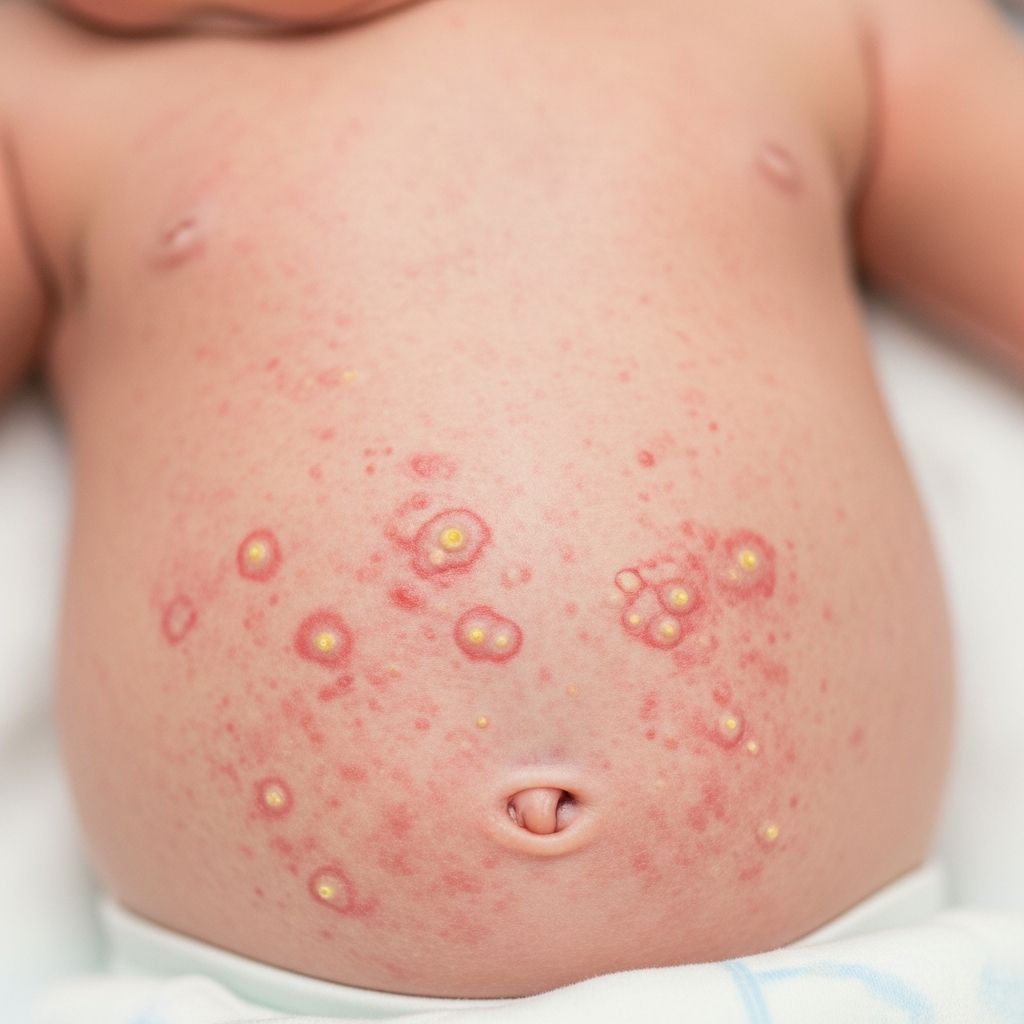
Toxic Erythema of the Newborn
Toxic erythema of the newborn, also known as erythema toxicum neonatorum (ETN), is a common, benign, and self-limiting skin condition that affects approximately 48-72% of full-term newborns. It typically manifests as fleeting erythematous macules, papules, and pustules within the first two weeks of life, sparing the palms and soles, with the infant remaining otherwise well.
What is toxic erythema of the newborn?
Toxic erythema of the newborn is a transient inflammatory skin eruption characterised by various combinations of erythematous macules (flat red patches), papules (small raised bumps), and pustules (small pus-filled lesions). The individual lesions are evanescent, often waxing and waning over hours to days, with few persisting beyond 24 hours. Despite its alarming appearance, the condition is harmless, causes no discomfort, and requires no specific treatment.
The term “toxic erythema” is a historical misnomer; it does not result from toxins, infections, or allergies. “Erythema” refers to skin redness, “toxicum” alludes to its reaction-like appearance, and “neonatorum” indicates its occurrence in newborns. ETN is more prevalent in full-term infants (up to 72%) than preterm babies (less than 2500g birth weight), with onset most commonly on day 2-3 of life, though it can appear as late as two weeks.
Who gets toxic erythema of the newborn?
ETN affects healthy, full-term newborns almost exclusively, with incidence rates reported as high as 40-70% in various studies. It is uncommon in premature infants and rarely seen beyond the neonatal period (first 28 days). There is no gender predilection, and it occurs across all ethnicities. Risk factors may include higher birth weight and vaginal delivery, though evidence is inconsistent.
- Peak incidence: Day 2-3 of life (48-72% of cases)
- Full-term infants: Most affected (up to 72%)
- Preterm infants: Less common (<7% if <2500g)
- Recurrence: Rare after initial episode, though new crops may appear in first 1-2 weeks
What causes toxic erythema of the newborn?
The precise aetiology of toxic erythema of the newborn remains unknown, but several theories have been proposed based on histopathological and immunohistochemical studies.
- Immune response to bacterial colonisation: Activation of hair follicle immune cells (e.g., eosinophils, IL-1, IL-8) in response to maternal/newborn skin flora entering follicles post-birth.
- Hormonal withdrawal: Maternal hormone discontinuation triggering transient skin inflammation.
- Graft-versus-host-like reaction: Historical theory of maternal-fetal cell exchange, though recent studies refute maternal cells in lesions.
- Inflammatory mediators: Elevated levels of eotaxin, nitric oxide synthetases, HMGB-1, and mast cell tryptase in lesional skin.
Histology confirms the diagnosis: flat patches show upper dermal eosinophil/neutrophil infiltrates; papules reveal perifollicular eosinophilic spongiosis; pustules contain subcorneal eosinophil-rich collections. No infectious agents are identified.
What are the clinical features of toxic erythema of the newborn?
The eruption typically begins on the face and rapidly spreads to the trunk and proximal limbs. Palms and soles are characteristically spared. Lesions evolve dynamically:
- Macules: Erythematous (red) flat patches, 1-3mm
- Papules: Firm white-yellow 1-3mm bumps on erythematous base (‘flea-bite’ appearance)
- Pustules: Fragile white-yellow vesicles/pustules (2-4mm) with surrounding flare
Lesions appear in successive crops, migrating across the skin over days. The infant is systemically well—no fever, irritability, poor feeding, or distress. Duration: 5-14 days total, with full resolution without scarring.
| Lesion Type | Description | Typical Duration |
|---|---|---|
| Erythematous macule | Flat red patch | Hours |
| Papule | Small raised white-yellow on red base | 1-2 days |
| Pustule | Fluid/pus-filled vesicle | <24 hours |
Diagnosis
Diagnosis is clinical, based on characteristic morphology, distribution, and well infant status. Wright’s stain of pustule smear shows eosinophils (not neutrophils, distinguishing from infection). Skin biopsy is rarely needed but confirmatory if performed.
Differential diagnosis
Although benign, ETN must be differentiated from serious conditions:
- Infectious pustulosis: Bacterial (S. aureus), herpes, candida—systemic signs, neutrophils on smear
- Eosinophilic pustular folliculitis: Preterm infants, persistent scalp lesions
- Miliaria: Heat-related, non-follicular
- Neonatal acne: Later onset (2-4 weeks), comedones
- Sepsis/meningitis: Ill infant, petechiae
- Incontinentia pigmenti: Linear vesicles → hyperpigmentation
When to worry: Persistent lesions >2 weeks, systemic illness, palm/sole involvement, or neutrophil predominance.
What is the treatment for toxic erythema of the newborn?
No treatment is required; the condition is self-limiting and resolves spontaneously within 1-2 weeks. Reassurance is key—educate parents on its benign nature to prevent unnecessary interventions.
- Skincare: Gentle cleansing with fragrance-free products; avoid irritants, excessive bathing
- Avoid: Topical steroids, antibiotics, antifungals—may irritate
- Monitoring: Observe for resolution; seek review if atypical features
Prognosis and prevention
Excellent prognosis with complete resolution without sequelae. No long-term skin or health effects. Prevention is not possible due to unknown aetiology, but prompt parental reassurance minimises anxiety.
Frequently Asked Questions
Is toxic erythema of the newborn dangerous?
No, it is entirely benign and harmless. The baby remains well throughout.
Does it cause itching or pain?
No, infants experience no discomfort and feed/sleep normally.
Will it scar or recur?
No scarring occurs. Recurrence is rare after the neonatal period.
When should I see a doctor?
If the baby is unwell, lesions persist >2 weeks, or spread to palms/soles.
Is it contagious?
No, it is not infectious or transmissible.
References
- Erythema Toxicum Neonatorum: Causes, Symptoms & Treatment — Metropolis India. 2023-10-15. https://www.metropolisindia.com/blog/preventive-healthcare/erythema-toxicum-neonatorum-causes-symptoms-treatment
- Toxic Erythema of the Newborn — DermNet NZ. 2024-05-20. https://dermnetnz.org/topics/toxic-erythema-of-the-newborn
- Erythema Toxicum — StatPearls, NCBI Bookshelf. 2023-07-17. https://www.ncbi.nlm.nih.gov/books/NBK470222/
- Erythema Toxicum Neonatorum — Cleveland Clinic. 2023-11-08. https://my.clevelandclinic.org/health/diseases/24390-erythema-toxicum-neonatorum
- Newborn Skin: Part I. Common Rashes — American Academy of Family Physicians. 2008-01-01. https://www.aafp.org/pubs/afp/issues/2008/0101/p47.html
Read full bio of medha deb