Transesophageal Echocardiogram: Purpose, Procedure & Safety
Complete guide to TEE testing: how it works, what to expect, and why doctors use it.
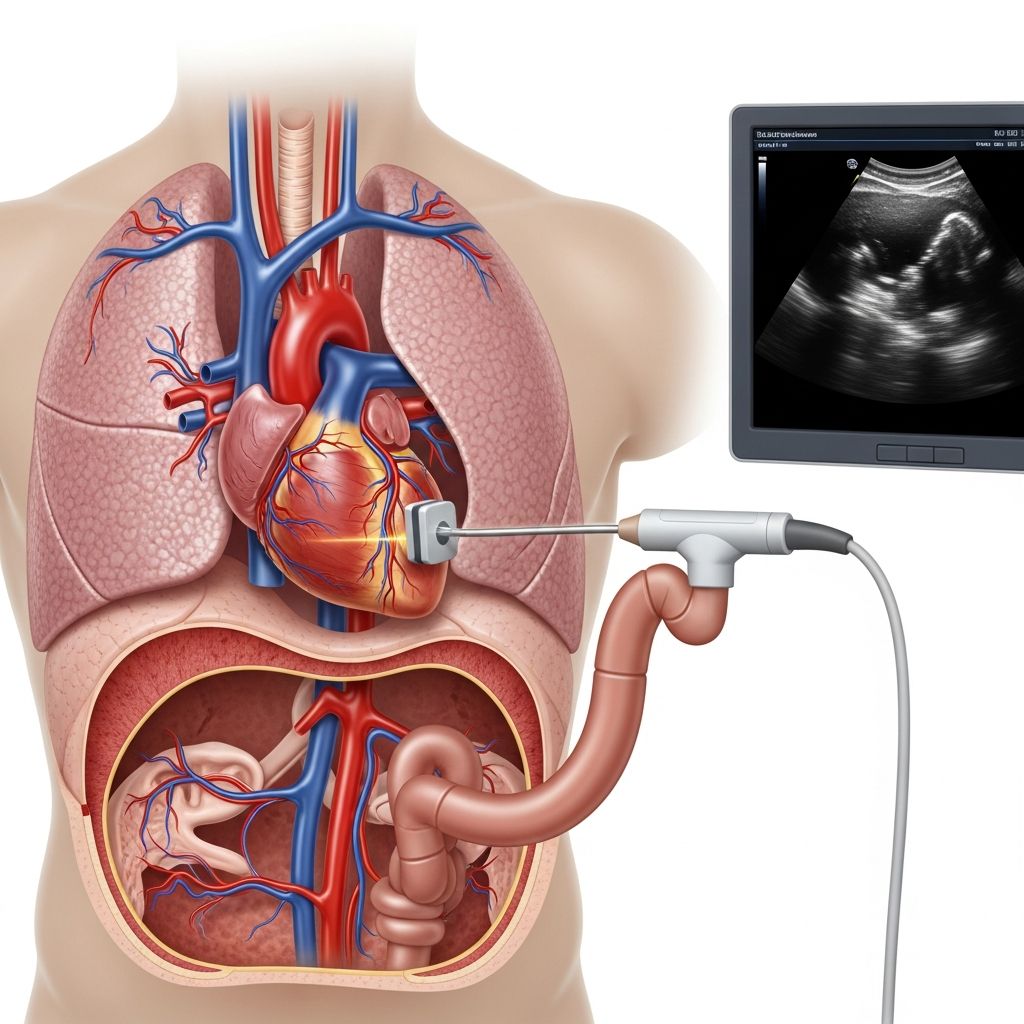
Understanding Transesophageal Echocardiogram (TEE)
A transesophageal echocardiogram, commonly referred to as TEE, is a specialized cardiac imaging test that uses high-frequency sound waves to create detailed pictures of your heart and its structures. Unlike standard echocardiograms that are performed on the chest’s surface, a TEE provides images from inside your body by positioning the ultrasound transducer in your esophagus, which lies directly behind your heart. This unique positioning allows physicians to obtain exceptionally clear and detailed images of the heart’s chambers, valves, and surrounding blood vessels that might be difficult to visualize with traditional surface-based imaging techniques.
The esophagus’s proximity to the heart makes it an ideal location for obtaining high-quality cardiac images. When the transducer is positioned in the esophagus, it can send and receive ultrasound waves with minimal interference from bone, tissue, or air. This results in superior image quality compared to transthoracic echocardiograms, making TEE particularly valuable for diagnosing complex cardiac conditions and evaluating the effectiveness of cardiac treatments.
Why Your Doctor May Recommend TEE
Your healthcare provider may recommend a transesophageal echocardiogram for various clinical reasons. TEE is especially useful when standard echocardiographic imaging is inconclusive or when your doctor needs to examine specific heart structures in greater detail. The test is particularly valuable for assessing conditions that require exceptional image clarity and precision.
Diagnostic Applications
TEE can effectively diagnose and evaluate numerous cardiac conditions. Your physician may order this test if they suspect valve disease, need to assess the structure and function of artificial heart valves, or want to investigate potential heart murmurs. The test is also instrumental in detecting blood clots within the heart chambers, particularly those associated with atrial fibrillation. Additionally, TEE can identify infections of the heart’s inner lining and valves, detect tumors or abnormal tissue growth, evaluate aortic aneurysms, and assess congenital heart defects.
Intraoperative Monitoring
Beyond diagnostic applications, TEE plays a critical role during cardiac surgery. Many heart surgeons use real-time TEE imaging during procedures to repair heart valves, correct aortic tears, repair congenital heart lesions, or treat bacterial heart infections. This intraoperative monitoring allows surgeons to visualize their work in real time and make adjustments as needed to ensure optimal surgical outcomes.
What TEE Can Reveal About Your Heart
The detailed images produced by transesophageal echocardiography provide comprehensive information about your heart’s anatomy and function. TEE can assess the size of your heart and the thickness of its walls, determining whether your heart chambers are enlarged or the walls have become abnormally thick. The test evaluates how effectively your heart pumps blood throughout your body, helping physicians determine your heart’s overall function.
TEE provides excellent visualization of your heart valves, including the mitral valve, tricuspid valve, and aortic valve. It can detect valve regurgitation, a condition where blood leaks backward through a valve, or stenosis, where a valve becomes abnormally narrowed or blocked. For patients with artificial heart valves, TEE can assess how well these prosthetic valves are functioning. The test can also identify abnormal tissue around valves that might indicate bacterial, viral, or fungal infections or malignant growths.
Additional diagnostic capabilities include detecting blood clots within the heart chambers, identifying defects in the heart’s structure that may cause abnormal heart sounds, visualizing the aorta and its branches, and assessing the pericardium, the membrane surrounding your heart.
Preparation for Your TEE Procedure
Proper preparation is essential for ensuring your TEE procedure goes smoothly and produces optimal results. Your healthcare team will provide specific instructions tailored to your individual situation.
Before Your Test
You will be instructed to fast for four to six hours before your procedure. This typically means avoiding food and beverages, though you may take prescribed medications with a small sip of water. It’s crucial to arrange transportation home after your test, as sedation used during the procedure will affect your ability to drive safely. Plan to have someone available to drive you home and potentially stay with you for several hours afterward.
Inform your healthcare team about all medications you’re taking, including blood thinners and aspirin. Let them know if you have any allergies to medications, particularly to sedatives or local anesthetics. If you have any dental work or have had recent throat surgery, inform your medical team as this may affect the procedure.
Medication Considerations
Some patients may need to adjust their medication schedule before TEE. Blood-thinning medications might need to be temporarily discontinued, though your physician will provide specific guidance. Never stop taking prescribed medications without consulting your healthcare provider first.
What to Expect During the Procedure
Understanding what happens during your TEE can help reduce anxiety and prepare you mentally for the experience. The procedure typically takes 20 to 90 minutes, though the actual image-acquisition portion usually lasts only 15 minutes.
Pre-Procedure Setup
When you arrive for your TEE, you’ll be taken to a specialized cardiac imaging suite. A healthcare professional will start an intravenous (IV) line in your forearm or hand. Through this IV, you’ll receive sedation medication to help you relax and stay comfortable throughout the procedure. Your throat will be numbed using a spray or gel to suppress your gag reflex and make swallowing easier when the probe is inserted.
You’ll be asked to lie on your left side on an examination table. Small adhesive pads called electrodes will be placed on your chest. These electrodes connect to a machine that continuously monitors your electrocardiogram, tracking your heart’s electrical activity and rhythm throughout the procedure. A blood pressure cuff will be placed on your arm to monitor your blood pressure, and a pulse oximeter will be attached to your finger to monitor your oxygen level. If needed, oxygen will be provided through a face mask or nasal cannula.
During the Test
Once you’re properly prepared and sedated, your doctor will gently guide a thin, flexible tube called an endoscope down your throat and into your esophagus. A mouthpiece may be placed between your teeth to prevent accidental biting of the probe. You may feel slight pressure or discomfort as the tube passes through your throat, but the numbing medication and sedation minimize discomfort. You’ll be instructed to swallow gently to help advance the tube.
Once positioned properly in your esophagus, the transducer at the end of the probe sends ultrasound waves toward your heart. These sound waves bounce off your heart structures and return to the transducer as echoes. A computer processes these echoes and converts them into moving images displayed on a video monitor. Your cardiologist can manipulate the probe, moving it up, down, and sideways to capture images of different heart structures from various angles.
Your doctor will continuously monitor your vital signs throughout the procedure. You’ll remain sedated but somewhat aware of what’s happening. Most patients tolerate the procedure well and don’t remember significant details afterward.
After the Procedure
When imaging is complete, the probe, IV line, and electrodes are removed. You’ll be monitored in a recovery area until the sedation wears off and you’re fully alert. This typically takes 30 minutes to an hour. You may feel drowsy or slightly disoriented initially, but these effects gradually resolve. Once your medical team confirms you’re stable, you’ll be cleared to leave with your designated driver.
Potential Risks and Complications
While transesophageal echocardiography is generally safe, as with any medical procedure, certain risks exist. Most patients experience no complications, but it’s important to understand potential issues.
Sore throat is the most common post-procedure complaint, typically mild and resolving within a few days. Rarely, the probe can cause injury to the esophagus, teeth, or throat structures. Bleeding in the throat or esophagus is uncommon but possible. Serious complications such as esophageal perforation are very rare.
Sedation carries inherent risks, though serious reactions are uncommon. Some patients may experience temporary confusion, nausea, or vomiting. Patients with certain medical conditions—such as severe esophageal disease, upper gastrointestinal bleeding, or certain swallowing disorders—may face elevated risks and should discuss these with their physician beforehand.
Discuss any concerns about risks with your healthcare provider before the procedure. They can assess your individual risk factors and provide personalized guidance.
Recovery and Aftercare
Recovery from a transesophageal echocardiogram is generally straightforward. Your throat may feel slightly sore for a day or two—sucking on throat lozenges or drinking warm tea can provide relief. Avoid eating or drinking for at least two hours after the procedure, allowing your throat’s numbing medication to wear off completely.
You cannot drive or operate machinery for 24 hours after the procedure due to residual sedation effects. Arrange for someone to drive you and ideally remain with you for several hours. Avoid strenuous activity for the remainder of the day.
Most patients can resume normal activities the following day. Contact your healthcare provider if you experience severe throat pain, difficulty swallowing that persists beyond a few days, chest pain, shortness of breath, or any other concerning symptoms.
Understanding Your TEE Results
Your cardiologist will review the images and prepare a detailed report of findings. Your healthcare provider will discuss results with you, explaining what the images reveal about your heart’s structure and function. Results typically become available within a few days of your procedure.
The report will indicate the size and function of your heart chambers, describe the appearance and function of your heart valves, note any abnormalities detected, and provide an overall assessment of your heart’s condition. Depending on findings, your doctor may recommend additional testing, lifestyle modifications, medications, or procedures.
TEE Versus Other Cardiac Imaging Tests
Understanding how TEE compares to other cardiac imaging options helps clarify why your doctor may have recommended this specific test.
| Test Type | Location | Image Quality | Best For |
|---|---|---|---|
| Transthoracic Echo | Chest surface | Good for routine screening | Initial cardiac assessment |
| Transesophageal Echo | Inside esophagus | Excellent detail | Detailed evaluation, surgery guidance |
| Stress Echocardiogram | Chest surface | Good; evaluates function with stress | Assessing coronary artery disease |
| Cardiac CT/MRI | Imaging booth | Excellent anatomic detail | Complex structural assessment |
Frequently Asked Questions About TEE
Q: Will I be awake during the TEE procedure?
A: You’ll receive sedation to help you relax and feel comfortable. Most patients are drowsy but somewhat aware during the procedure. You typically won’t remember many details afterward. General anesthesia (deep sleep) is used only rarely and requires longer recovery time.
Q: How long does a TEE take?
A: The entire procedure, including preparation and recovery, typically takes 1-2 hours. The actual imaging portion usually takes only 15-20 minutes.
Q: Is TEE painful?
A: The procedure is not painful. Your throat will be numbed, and you’ll receive sedation. You may feel pressure or mild discomfort as the probe is inserted, but this is temporary and minimized by numbing medication and sedation.
Q: What are the risks of TEE?
A: TEE is generally safe with low complication rates. Mild sore throat is common. Serious complications like esophageal perforation are rare. Discuss your individual risk factors with your healthcare provider.
Q: Can I eat before my TEE?
A: No. You must fast for 4-6 hours before the procedure. This reduces aspiration risk during sedation. You may take essential medications with a small sip of water.
Q: How soon will I get my results?
A: Your cardiologist will typically review the images and prepare a report within a few days. Your healthcare provider will discuss findings and next steps with you.
Q: When can I return to normal activities?
A: You must avoid driving for 24 hours after sedation. Most patients can resume normal activities the next day, though you should avoid strenuous activity for the rest of the day of the procedure.
Q: Is TEE better than a regular echocardiogram?
A: TEE isn’t necessarily better, but rather different. It provides superior detail of certain heart structures, particularly those behind the breastbone. Your doctor chooses the appropriate test based on what needs to be evaluated.
Conclusion
Transesophageal echocardiography represents an invaluable diagnostic tool in modern cardiology. By positioning the ultrasound transducer directly in the esophagus, physicians can obtain exceptionally detailed images of heart structures that may be difficult to visualize with surface-based imaging. Whether used for diagnostic purposes or intraoperative guidance during cardiac surgery, TEE provides critical information that helps cardiologists accurately diagnose heart conditions and monitor treatment effectiveness.
While the procedure requires sedation and involves inserting a probe into your esophagus, most patients tolerate it well with minimal complications. Understanding what to expect before, during, and after your TEE can help you feel more confident and prepared. Discuss any concerns or questions with your healthcare team, as they can provide personalized guidance based on your specific medical situation and help ensure the best possible outcome.
References
- Echocardiogram — Mayo Clinic. 2024-08-15. https://www.mayoclinic.org/tests-procedures/echocardiogram/about/pac-20393856
- Transesophageal Echocardiography — American Heart Association. 2024. https://www.heart.org/en/health-topics/heart-attack/diagnosing-a-heart-attack/transesophageal-echocardiography
- Transesophageal Echocardiogram (TEE) — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diagnostics/4992-echocardiogram-transesophageal-tee
- Transesophageal Echocardiogram (TEE) — Heart and Stroke Foundation of Canada. 2024. https://www.heartandstroke.ca/heart-disease/tests/transesophageal-echocardiogram-tee
- Transesophageal Echocardiogram — Stanford Healthcare. 2024. https://stanfordhealthcare.org/medical-tests/t/transesophageal-echocardiogram.html
- Transesophageal Echocardiogram — StatPearls, National Center for Biotechnology Information. 2024-08-20. https://www.ncbi.nlm.nih.gov/books/NBK442026/
Read full bio of Sneha Tete













