Trochanteric Bursitis: Symptoms, Causes & Treatments
Complete guide to understanding trochanteric bursitis, its causes, symptoms, and effective treatment options.
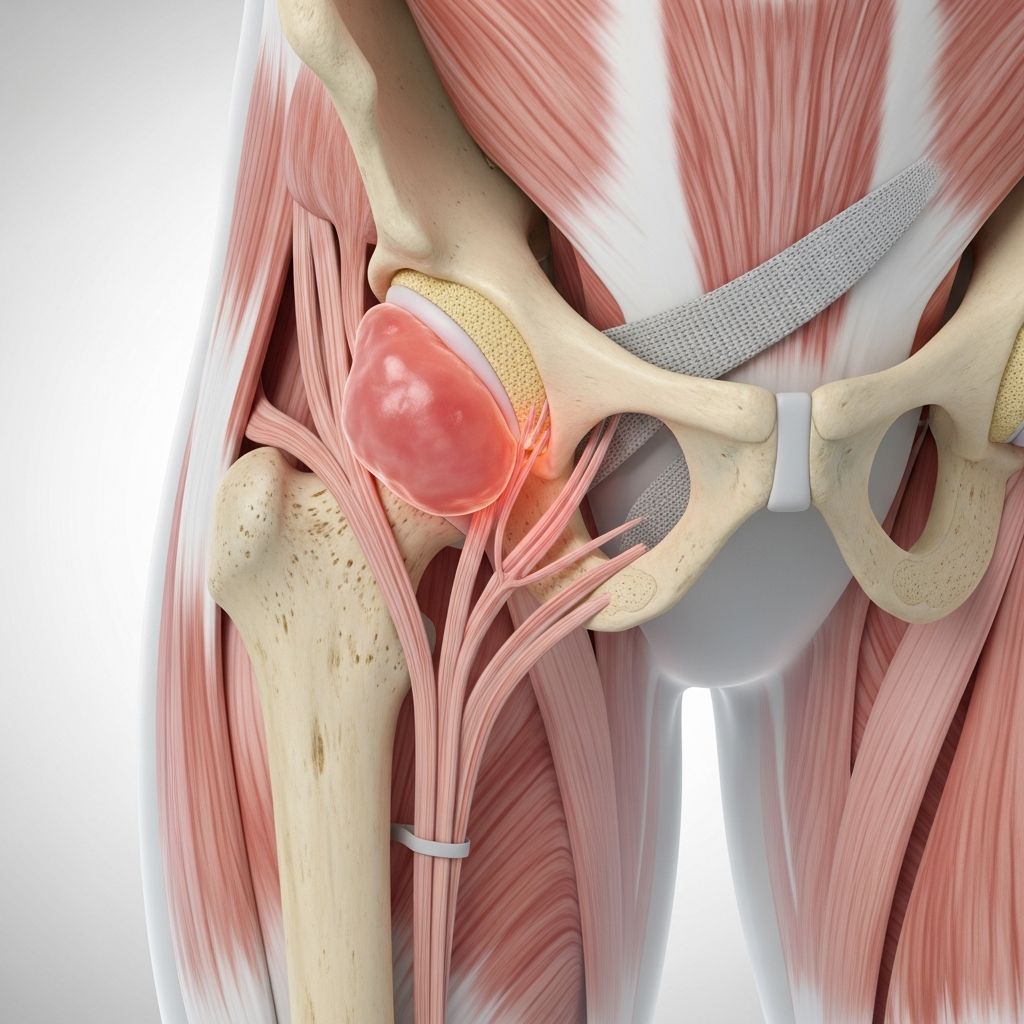
Understanding Trochanteric Bursitis
Trochanteric bursitis is a common condition that affects the hip, causing pain on the outside of the hip joint. The condition develops when the bursa—a small, fluid-filled sac that cushions the greater trochanter (the bony prominence at the top of your thighbone)—becomes inflamed. This inflammation can range from mild discomfort to severe pain that significantly impacts daily activities and quality of life.
The greater trochanteric bursa is located between the greater trochanter and the iliotibial band, a thick band of tissue that runs along the outside of the leg from the hip to the knee. When this bursa becomes irritated or inflamed, it produces pain that is typically felt on the lateral side of the hip. While trochanteric bursitis can develop suddenly following an injury, it often develops gradually due to repetitive stress and strain on the hip joint.
What Causes Trochanteric Bursitis?
Trochanteric bursitis develops when the bursa becomes irritated or damaged. Several factors can contribute to the development of this condition. Understanding these causes can help you take preventive measures and identify risk factors in your own life.
Common causes of trochanteric bursitis include:
- Falls or direct trauma to the hip area
- Repetitive activities such as running, cycling, or prolonged standing
- Tight iliotibial (IT) band that rubs against the bursa
- Poor posture and body mechanics
- Previous hip injury or surgery
- Spinal alignment issues such as scoliosis
- Unequal leg lengths affecting gait and posture
- Inflammatory conditions like rheumatoid arthritis
- Sudden increases in activity level
The hip joint bears significant loads during everyday activities—up to 6 to 8 times your body weight—making it particularly vulnerable to wear and tear. Repetitive microtrauma and mechanical overload between the greater trochanter and the iliotibial band commonly stem from overuse, trauma, or altered gait patterns. In recent years, imaging studies have revealed that abductor muscle tears, tendinosis, and thickening of the iliotibial band are frequently identified as primary sources of pain, representing what is now understood as greater trochanteric pain syndrome (GTPS).
Recognizing the Symptoms
The primary symptom of trochanteric bursitis is hip pain, typically felt on the outside of the hip. This pain can vary in character and intensity depending on the severity of the inflammation and individual factors.
Common symptoms include:
- Sharp, intense pain that may develop suddenly or gradually
- Dull, aching pain that may develop over time
- Pain that worsens with prolonged sitting, especially with legs crossed
- Increased discomfort when climbing stairs
- Pain during high-impact exercises or running
- Tenderness when pressure is applied to the outer hip
- Pain that radiates down the outside of the thigh
- Difficulty sleeping on the affected side
- Stiffness and reduced range of motion in the hip
The pain may start as sharp and intense but can settle into a dull ache over time. Many patients find that their symptoms worsen with specific activities and improve with rest. If you experience persistent hip pain that lasts more than a couple of weeks or continues to worsen despite conservative care, it is important to visit a healthcare provider for evaluation.
Diagnosis of Trochanteric Bursitis
Healthcare providers typically diagnose trochanteric bursitis based on a clinical evaluation combined with imaging studies when necessary. During your appointment, your doctor will review your medical history, ask about your symptoms, and perform a physical examination of the hip joint. They may apply pressure to specific areas around the greater trochanter or perform special maneuvers to reproduce your symptoms.
Imaging studies such as X-rays, ultrasound, or MRI may be used to differentiate trochanteric bursitis from other potential causes of hip pain and to confirm the diagnosis. A deep understanding of the relevant anatomy, clinical examination findings, and imaging results is essential in managing cases resistant to conservative treatment. Your healthcare provider will use this information to develop an appropriate treatment plan tailored to your specific condition.
Treatment Options for Trochanteric Bursitis
The good news is that trochanteric bursitis is highly treatable. The goal of treatment is to manage your symptoms and get you back to doing the activities you love, pain-free. Most cases resolve with conservative management, though some may require more advanced interventions.
Initial Home Treatment
Trochanteric bursitis often resolves itself with home treatment. These initial steps are important for managing inflammation and pain:
- Rest: Taking a break from activities that aggravate your symptoms is crucial for allowing the bursa to heal. Avoid high-impact exercises and repetitive hip movements temporarily.
- Ice therapy: Applying ice packs to the area can lessen symptoms by reducing inflammation. Initially, ice can be applied every three to four hours, and is especially helpful following exercise and physical therapy sessions.
- Nonsteroidal anti-inflammatory drugs (NSAIDs): Over-the-counter medications such as ibuprofen or naproxen can decrease inflammation and pain. However, before starting NSAIDs, confirm that you have no contraindications, especially if you take blood thinners or have a history of gastrointestinal bleeding.
- Stretching exercises: Gentle stretching routines can help reduce tension in the hip muscles and promote healing.
Physical Therapy and Exercise
Physical therapy is particularly effective in treating trochanteric bursitis and is recommended for most patients. A physical therapist can teach you proper exercises for increasing hip and leg strength and explore simple stretching routines. Stretching and strengthening the muscles around the hip joint can provide long-term relief from hip bursitis symptoms and prevent recurrence.
Your physical therapist may recommend specific exercises targeting the hip abductors, gluteal muscles, and other stabilizing muscles. These therapeutic exercises help restore proper biomechanics and reduce stress on the bursa. Physical therapy combined with lifestyle modifications has proven highly effective for most patients.
Lifestyle Modifications
Making changes to your daily activities can significantly improve your symptoms. Consider the following modifications:
- Avoid prolonged sitting, especially with legs crossed
- Maintain proper posture throughout the day
- Use ergonomic furniture and support pillows
- Sleep on your back or unaffected side
- Avoid high-impact activities until symptoms improve
- Gradually return to activities with proper form
- Wear supportive footwear with proper arch support
Pharmacologic Therapy
When initial home treatments are insufficient, pharmacologic therapy can provide additional relief. Oral NSAIDs are crucial for inhibiting the inflammatory cascade and providing symptomatic pain relief for trochanteric bursitis. These medications can be obtained over-the-counter or prescribed by your healthcare provider in higher doses if needed. Some studies have suggested that topical NSAIDs are as beneficial as oral NSAIDs in managing symptoms of greater trochanteric pain syndrome.
Corticosteroid Injections
Trochanteric bursitis can be effectively managed with steroid injections when conservative measures prove insufficient. These injections administer a localized dose of cortisone, frequently combined with a local anesthetic such as lidocaine. This treatment offers targeted relief and directly addresses local inflammation.
Orthopedic surgeons and primary care clinicians can administer these minor outpatient procedures using standard sterile techniques. Corticosteroid injections have been widely studied, with improvements from treatment ranging significantly among patients. Conservative management has proven highly effective, with studies showing rapid and enduring pain relief after local corticosteroid and anesthetic injections in approximately 90% of patients. Long-term outcomes are comparable between individuals who receive corticosteroid injections and those who undergo physical therapy alone.
Advanced Injection Therapies
For cases resistant to standard conservative measures, advanced therapies have been explored. Platelet-rich plasma (PRP) injections concentrate healing factors from your own blood and may promote tissue repair. Extracorporeal shock wave therapy (ESWT) uses sound waves to stimulate healing and has shown particular promise when combined with exercise regimens. These advanced therapies are typically reserved for patients who have not responded adequately to more conventional treatments.
Surgical Treatment
Surgery is rarely needed for trochanteric bursitis and is reserved only for people who don’t respond to any other treatment and have chronic pain they cannot manage. When surgery is considered, it is usually an outpatient, arthroscopic procedure requiring only small incisions. Studies of bursitis patients undergoing surgical intervention have noted significant improvement in functional scores and pain with few recurrences or revisions needed.
Multiple small case series demonstrate good outcomes after open iliotibial band release and bursectomy. Isolated arthroscopic bursectomy also shows favorable results, with significant improvement in pain and function reported by most patients. The minimally invasive nature of these procedures means patients generally go home the same day and can usually walk the following day with only mild discomfort.
When to See a Healthcare Provider
Visit a healthcare provider if you’re experiencing hip pain, especially if the pain gets worse or doesn’t go away in a couple of weeks. Seeking professional evaluation is important if:
- Hip pain is severe or sudden
- Symptoms don’t improve with home treatment
- Pain significantly limits your daily activities
- You cannot bear weight on the affected hip
- The condition is affecting your sleep quality
- You have a history of hip problems or injuries
Prevention Strategies
While not all cases of trochanteric bursitis can be prevented, several strategies can help reduce your risk:
- Maintain proper posture and body mechanics during daily activities
- Gradually increase intensity and duration of exercise
- Incorporate regular stretching and strengthening exercises
- Wear appropriate footwear with proper support
- Take frequent breaks during prolonged sitting
- Manage your weight to reduce hip joint stress
- Address any gait abnormalities with professional help
- Avoid repetitive movements that stress the hip
Frequently Asked Questions
Q: How long does trochanteric bursitis typically last?
A: With appropriate treatment, most cases of trochanteric bursitis resolve within several weeks to a few months. However, some cases may take longer to heal, and recurrence is possible if preventive measures are not maintained.
Q: Can trochanteric bursitis go away on its own?
A: Yes, trochanteric bursitis often resolves itself with conservative home treatment including rest, ice, NSAIDs, and stretching exercises. However, professional treatment can accelerate healing and prevent recurrence.
Q: Is it safe to exercise with trochanteric bursitis?
A: Gentle exercises and physical therapy are beneficial for healing. However, high-impact activities should be avoided during the acute phase. Work with a physical therapist to develop an appropriate exercise program.
Q: What is the difference between trochanteric bursitis and greater trochanteric pain syndrome?
A: Greater trochanteric pain syndrome (GTPS) is a broader term that encompasses trochanteric bursitis, external coxa saltans (snapping hip), and abductor tendinopathy. GTPS represents a more accurate understanding of lateral hip pain.
Q: Are corticosteroid injections permanent?
A: Corticosteroid injections provide temporary relief by reducing inflammation. While they can be highly effective, they typically provide benefits for several weeks to months. Additional injections may be needed if symptoms recur.
Q: Can tight IT bands cause trochanteric bursitis?
A: Yes, a tight iliotibial band can rub against the trochanteric bursa and cause inflammation and pain. Stretching and physical therapy targeting IT band tightness can help prevent or manage this condition.
Q: Is surgery necessary for trochanteric bursitis?
A: Surgery is rarely necessary for trochanteric bursitis and is reserved only for chronic cases that have not responded to conservative treatment. The majority of cases resolve with non-surgical management.
Conclusion
Trochanteric bursitis is a manageable condition that responds well to conservative treatment in most cases. By understanding the causes, recognizing symptoms early, and pursuing appropriate treatment, most people can achieve significant pain relief and return to their normal activities. Whether through rest and physical therapy or more advanced interventions like corticosteroid injections, effective treatment options are available. If you suspect you have trochanteric bursitis, consult with a healthcare provider to develop a personalized treatment plan that addresses your specific needs and helps you achieve long-term relief.
References
- Greater Trochanteric Pain Syndrome (Greater Trochanteric Bursitis) — National Center for Biotechnology Information, National Library of Medicine. 2024. https://www.ncbi.nlm.nih.gov/books/NBK557433/
- Hip Bursitis — American Academy of Orthopaedic Surgeons (AAOS). 2024. https://orthoinfo.aaos.org/en/diseases–conditions/hip-bursitis/
- Trochanteric Bursitis: Causes, Symptoms, and Treatments — UPMC Orthopaedics. 2024. https://www.upmc.com/services/orthopaedics/conditions/trochanteric-bursitis
- Trochanteric Bursitis — UCSF Health. 2024. https://www.ucsfhealth.org/conditions/trochanteric-bursitis
- Hip Bursitis: Symptoms, Causes & Treatment — Hoag Orthopedic Institute. 2024. https://www.hoagorthopedicinstitute.com/what-hurts-/hip/conditions/hip-bursitis/
- Trochanteric Bursitis: Causes, Treatments and Exercises — UC Health. 2024. https://www.uchealth.com/en/conditions/trochanteric-bursitis
Read full bio of Sneha Tete











