Type 2 Diabetes: What It Is, Causes, Symptoms & Treatment
Complete guide to understanding Type 2 diabetes, its causes, symptoms, and evidence-based management strategies.
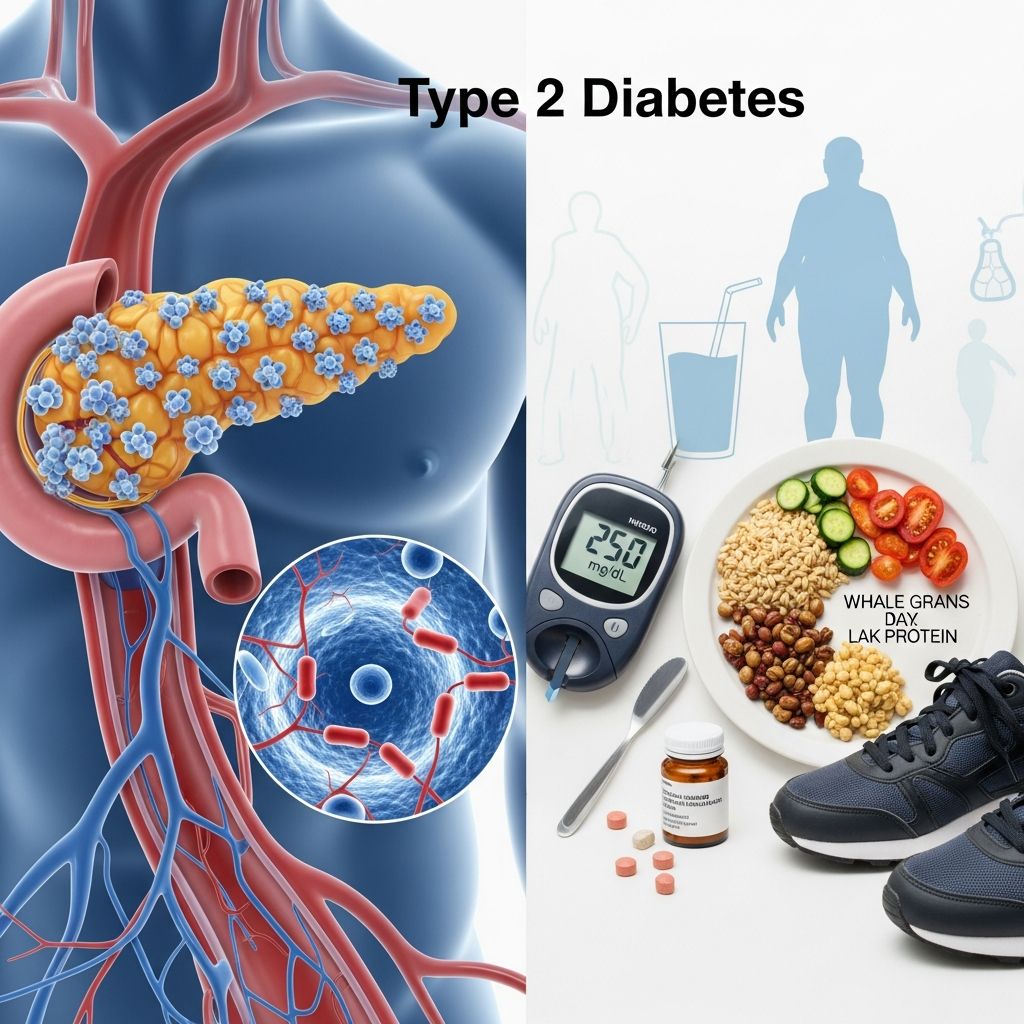
Type 2 diabetes (T2D) is a chronic condition that happens when you have constant high blood sugar. This occurs because your body cannot use insulin properly, a condition known as insulin resistance. Unlike Type 1 diabetes, which involves the pancreas failing to produce sufficient insulin, Type 2 diabetes develops when your body’s cells do not respond adequately to the insulin your pancreas produces. This metabolic disorder affects millions of people worldwide and can significantly impact your quality of life if left unmanaged. However, with proper management through lifestyle modifications, medications, and regular medical supervision, you can keep your blood sugar levels in a healthy range and prevent serious complications.
Understanding Type 2 Diabetes
Type 2 diabetes is a progressive disease that develops gradually over time. Your pancreas initially continues to produce insulin, but your body’s cells become resistant to it, requiring the pancreas to work harder to maintain normal blood sugar levels. Eventually, the pancreas may struggle to keep up with the body’s demands, leading to elevated blood glucose levels. This condition accounts for approximately 90% of all diabetes cases and is increasingly common among both adults and children.
Risk Factors and Causes
Several factors contribute to the development of Type 2 diabetes, including genetic predisposition, obesity, sedentary lifestyle, age (risk increases with age), and certain ethnic backgrounds. Family history plays a significant role—if your parents or siblings have Type 2 diabetes, your risk is substantially higher. Additionally, conditions such as gestational diabetes during pregnancy, polycystic ovary syndrome (PCOS), and high blood pressure increase your likelihood of developing Type 2 diabetes later in life.
Obesity and excess body weight, particularly abdominal fat, are major risk factors. Excess fat tissue produces hormones and substances that can interfere with your body’s ability to use insulin effectively. A sedentary lifestyle compounds this problem, as physical activity helps your muscles use glucose more efficiently and improves insulin sensitivity.
Recognizing Symptoms of Type 2 Diabetes
Type 2 diabetes often develops gradually, and many people may not experience noticeable symptoms in the early stages. When symptoms do appear, they typically include:
- Increased thirst and frequent urination
- Increased hunger, even after eating
- Persistent fatigue or weakness
- Blurred vision
- Slow-healing cuts or sores
- Tingling or numbness in the hands or feet
- Unexplained weight loss
- Darkened skin patches, typically in body creases (acanthosis nigricans)
Because Type 2 diabetes can progress without obvious symptoms, regular screening is particularly important if you have risk factors. Many people discover they have Type 2 diabetes during routine medical examinations or blood tests performed for other reasons.
Diagnosis of Type 2 Diabetes
Healthcare providers use several blood tests to diagnose Type 2 diabetes. These tests measure your blood glucose levels and provide insight into your average blood sugar control over time. The primary diagnostic tests include:
| Test Type | Description | Diagnostic Range |
|---|---|---|
| Fasting Blood Sugar Test | Measures blood glucose after eight hours of fasting | 126 mg/dL or higher indicates diabetes |
| A1C Test | Shows your average blood sugar over the past two to three months | 6.5% or higher indicates diabetes |
| Random Blood Sugar Test | Measures blood glucose at any time during the day | 200 mg/dL or higher with symptoms indicates diabetes |
| Glucose Tolerance Test | Tests blood sugar before and after drinking glucose solution | 200 mg/dL or higher two hours after drinking indicates diabetes |
In some cases, your provider may order an autoantibody blood test to determine whether you have Type 1 diabetes instead of Type 2 diabetes, as the treatments differ significantly.
Key Components of Type 2 Diabetes Management
The key parts of managing Type 2 diabetes include lifestyle modifications, medication management, blood sugar monitoring, and regular healthcare provider appointments. You primarily manage Type 2 diabetes on your own with medical guidance and support from your healthcare team. This comprehensive team-based approach ensures you receive personalized care tailored to your specific needs and circumstances.
Building Your Healthcare Team
Your care team may include:
- Your primary care provider
- An endocrinologist (diabetes specialist)
- A certified diabetes educator
- A registered dietitian
- A pharmacist
- Other specialists as needed
This collaborative approach ensures comprehensive care addressing all aspects of your condition, from blood sugar management to cardiovascular health and complication prevention.
Nutrition and Meal Planning
What and when you eat significantly impact your blood sugar levels. Creating an effective meal plan is one of the most important aspects of managing Type 2 diabetes. Most providers recommend eating a variety of nutritious foods using the American Diabetes Association’s “Plate Method” approach.
The Plate Method for Balanced Meals
The Plate Method provides a simple visual guide for portion control and balanced nutrition. When planning your meals, divide your plate as follows:
- One-quarter non-starchy vegetables: Include leafy greens, broccoli, cauliflower, bell peppers, and zucchini
- One-quarter lean protein: Choose chicken breast, fish, lean beef, tofu, or legumes
- One-quarter carbohydrates: Select whole grains, sweet potatoes, or beans
- Healthy fats and beverages: Include olive oil, nuts, and water or unsweetened beverages
Foods That Support Healthy Glucose Levels
In general, the following types of foods can help support healthy glucose levels:
- Non-starchy vegetables (at least half your plate)
- Whole grains instead of refined carbohydrates
- Lean proteins including poultry, fish, and plant-based options
- Healthy fats from sources like avocados, nuts, and olive oil
- Low-fat dairy products
- Fruits in moderation, emphasizing those with lower glycemic index
Working with a registered dietitian can help you create a personalized meal plan that considers your food preferences, allergies, and lifestyle. A dietitian can figure out what the healthiest diet looks like in your life and help you develop sustainable eating habits.
Physical Activity and Exercise
Regular physical activity is crucial for managing Type 2 diabetes. Exercise helps your muscles use glucose more efficiently, improves insulin sensitivity, and supports weight management. Most experts recommend at least 150 minutes of moderate-intensity aerobic activity per week, combined with resistance training two to three times weekly.
Physical activity can include walking, swimming, cycling, dancing, or any activity that elevates your heart rate. Even short bouts of activity throughout the day provide benefits. Start gradually if you are sedentary, and work with your healthcare team to develop an appropriate exercise plan.
Medication Management
Your provider may recommend taking medication for Type 2 diabetes. Several classes of medications work through different mechanisms to help control blood sugar levels. Modern diabetes medication management emphasizes a complications-centric approach, treating not just glucose levels but also considering cardiovascular health, weight management, and kidney function.
Common Type 2 Diabetes Medications
Medication options include metformin (first-line therapy), sulfonylureas, meglitinides, thiazolidinediones, DPP-4 inhibitors, GLP-1 receptor agonists, SGLT2 inhibitors, and insulin therapy. Your healthcare provider will select medications based on your individual health profile, considering factors such as kidney function, cardiovascular disease risk, and weight.
Many patients benefit from combinations of medications targeting different mechanisms of hyperglycemia. Some combinations of background insulin and GLP-1 medications are available specifically for people with Type 2 diabetes.
Blood Sugar Monitoring
Regular monitoring of your blood glucose levels helps you understand how your body responds to food, activity, and medications. The two main ways you can monitor your glucose at home are with a glucose meter and/or a continuous glucose monitor (CGM).
Glucose Meters
Traditional glucose meters require a small blood sample from a finger prick. You can test at various times throughout the day—before meals, two hours after meals, before exercise, or when experiencing symptoms of high or low blood sugar.
Continuous Glucose Monitors
CGMs are wearable devices that measure glucose levels automatically throughout the day and night, providing real-time data and trend information. Many people find CGMs helpful for understanding their glucose patterns and making real-time management adjustments.
Work with your healthcare team to determine the appropriate monitoring schedule and which device works best for your lifestyle and management needs.
Long-Term Diabetes Management
Type 2 diabetes is a chronic (long-term) disease, meaning you must manage it for the rest of your life. There is no cure for Type 2 diabetes. However, you can manage it in a way that keeps your blood sugar levels in a healthy range. If you stop managing it or undermanage it, your blood sugar levels will return to elevated levels.
You will need regular appointments with your healthcare team to ensure you remain on track with your management plan. As your body, life, and routines change, your management will change as well. Your healthcare team can provide new strategies tailored to your evolving needs.
Preventing Complications
Proper management of Type 2 diabetes is essential for preventing serious complications. Long-term complications include heart disease, stroke, kidney disease, vision problems, and nerve damage (neuropathy). If you develop symptoms of any complications, see your provider as soon as possible.
Regular dental care is also important, as diabetes increases your risk of gum disease. See your dentist every six months, and report any bleeding in your gums, loose teeth, sores, or ulcers in your mouth immediately.
Frequently Asked Questions (FAQs)
Q: Is Type 2 diabetes curable?
A: There is currently no cure for Type 2 diabetes. However, with proper management through lifestyle changes, medications, and regular medical supervision, you can keep your blood sugar levels in a healthy range and prevent serious complications. Some people achieve remission through significant weight loss and intensive lifestyle changes, but this requires maintaining these changes long-term.
Q: Can I develop Type 2 diabetes even if it does not run in my family?
A: Yes, you can develop Type 2 diabetes without a family history. While genetics increase risk, lifestyle factors such as obesity, physical inactivity, and diet play significant roles. Age is also a risk factor, as Type 2 diabetes becomes more common as people get older.
Q: How often should I check my blood sugar?
A: The frequency of blood sugar monitoring depends on your individual circumstances, whether you are taking medications, and your provider’s recommendations. Some people monitor multiple times daily, while others check less frequently. Your healthcare team can help determine the appropriate monitoring schedule for you.
Q: Can I prevent Type 2 diabetes?
A: Yes, you can significantly reduce your risk of developing Type 2 diabetes through lifestyle modifications. Maintaining a healthy weight, exercising regularly, eating a balanced diet, quitting smoking, and managing stress can all help prevent or delay the onset of Type 2 diabetes, particularly if you have prediabetes.
Q: Is insulin therapy only for Type 1 diabetes?
A: No, insulin therapy is also used in Type 2 diabetes management. While many people with Type 2 diabetes can initially manage their condition with oral medications and lifestyle changes, some eventually require insulin therapy as the disease progresses and the pancreas produces less insulin.
Q: How does stress affect Type 2 diabetes?
A: Stress hormones like cortisol can raise blood sugar levels, making diabetes management more challenging. Managing stress through relaxation techniques, exercise, adequate sleep, and professional support can help maintain better blood sugar control.
References
- Managing Diabetes – Treatment Guide — Cleveland Clinic. 2024. https://my.clevelandclinic.org/-/scassets/files/org/endocrinology-metabolism/managing-diabetes-treatment-guide.ashx
- Type 2 Diabetes Adult Management — Cleveland Clinic. 2024. https://my.clevelandclinic.org/services/type-2-diabetes-management
- Comprehensive Type 2 Diabetes Management Algorithm — American Association of Clinical Endocrinologists (AACE). 2023. https://pubmed.ncbi.nlm.nih.gov/37150579/
- Healthy You – A Guide to Diabetes Self-Care — Cleveland Clinic. 2024. https://my.clevelandclinic.org/-/scassets/files/org/endocrinology-metabolism/diabetes-self-care-guide.pdf
- Type 2 Diabetes: What It Is, Causes, Symptoms & Treatment — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/21501-type-2-diabetes
- Meal Planning for Type 2 Diabetes — Cleveland Clinic Health. 2024. https://health.clevelandclinic.org/meal-plan-for-type-2-diabetes
- Type 2 Diabetes: Evolving Concepts and Treatment — Cleveland Clinic Journal of Medicine. 2023. https://www.ccjm.org/content/86/7/494
Read full bio of medha deb











