Ulcerative Colitis Causes: 4 Leading Factors Explained
Unraveling the complex factors behind ulcerative colitis, from immune dysfunction to genetics and environmental triggers.
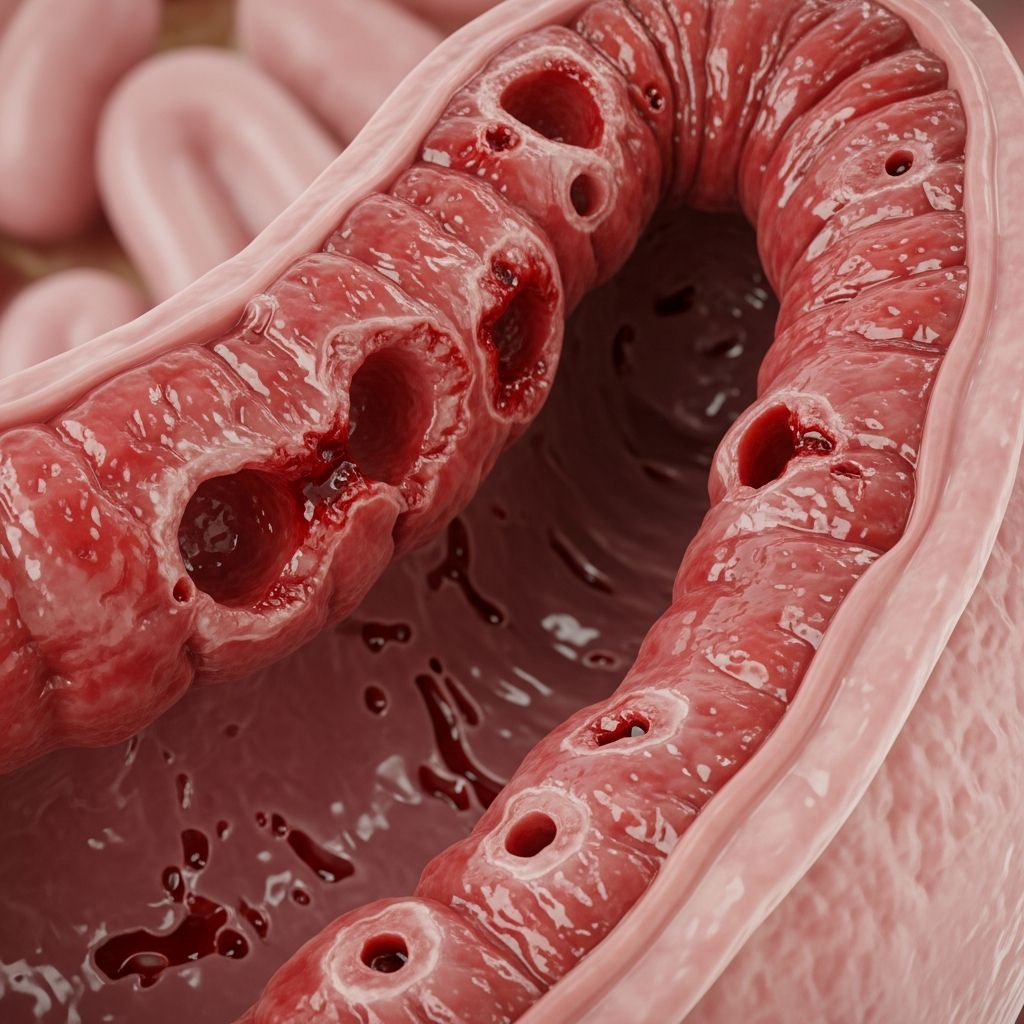
Ulcerative Colitis Causes
Ulcerative colitis (UC) is a chronic inflammatory bowel disease (IBD) that triggers long-lasting inflammation and ulcers in the innermost lining of the large intestine (colon) and rectum. While the precise cause remains unknown, research points to a combination of immune system malfunctions, genetic predispositions, gut microbiome imbalances, and environmental factors. Affecting approximately one million Americans, UC leads to symptoms like bloody diarrhea, abdominal pain, fatigue, and weight loss, significantly impacting quality of life. This article delves into the multifaceted causes and risk factors, drawing from authoritative medical sources to provide a comprehensive overview.
What Is Ulcerative Colitis?
Ulcerative colitis specifically targets the colon and rectum, starting at the rectum and potentially extending continuously upward. Unlike Crohn’s disease, which can affect any part of the gastrointestinal tract and deeper bowel layers, UC is confined to the mucosal layer of the large intestine. The condition manifests in varying extents:
- Ulcerative proctitis: Limited to the rectum.
- Left-sided colitis: Extends to the sigmoid and descending colon.
- Subtotal colitis: Involves the descending colon up to the transverse colon.
- Widespread colitis (pancolitis): Affects the entire colon, often causing severe bloody diarrhea, cramps, fatigue, and weight loss.
UC prevalence exceeds 5 million cases worldwide, making it a significant global health concern. It differs from microscopic colitis, which requires microscopic examination for diagnosis, and Crohn’s, which has skip lesions and transmural involvement.
Symptoms of Ulcerative Colitis
Common symptoms include persistent diarrhea mixed with blood, rectal bleeding, abdominal cramps, urgency to defecate, inability to defecate despite urgency, weight loss, fatigue, and fever. Symptoms often develop gradually but can onset suddenly. During remission, individuals may experience few or no symptoms, but flares can be triggered by various factors. In children, growth failure may occur due to chronic inflammation and malnutrition. Severe cases risk complications like dehydration, anemia, and toxic megacolon—a life-threatening colon dilation.
Causes of Ulcerative Colitis
The exact etiology of UC eludes researchers, but it’s not caused by diet or stress alone, though these can exacerbate flares. Instead, a multifactorial interplay is implicated.
Immune System Malfunction
A leading theory posits an abnormal immune response where the body attacks its own colon cells while fighting an infection. In UC, the immune system misfires, causing chronic inflammation in the digestive tract. This irregular reaction targets the mucosal lining, leading to ulcers and ongoing damage. Unlike typical infections, this autoimmune-like response persists, suggesting dysregulation in both innate and adaptive immunity.
Genetics and Heredity
UC clusters in families; individuals with first-degree relatives (parents, siblings, children) affected face heightened risk. Multiple genetic markers are linked to UC, increasing susceptibility, though no single gene causes it. Research confirms heredity’s role, with genetic testing not yet diagnostic. Whites, particularly Ashkenazi Jews, show higher genetic predisposition.
Gut Microbiome Imbalance
The gut microbiome—comprising bacteria, viruses, and fungi aiding digestion—differs in UC patients. Dysbiosis, or microbial imbalance, may provoke immune overreactions. Studies highlight microbiome alterations in IBD, though causation versus correlation remains under investigation.
Environmental Factors
Environment influences UC risk, including geography, diet, antibiotic use, and lifestyle. Urban living, Western diets high in processed foods, and early-life exposures may contribute. NSAIDs (e.g., ibuprofen) and prior gut infections slightly elevate risk. Researchers explore gene-environment-microbiome interactions.
Risk Factors for Ulcerative Colitis
Beyond causes, specific risks heighten UC likelihood:
- Age: Peaks before 30, with a secondary rise after 60.
- Family history: Close relatives with IBD significantly increase odds.
- Ethnicity: Highest in whites, especially Ashkenazi Jews.
- Prior infections/NSAIDs: Gastrointestinal infections or chronic NSAID use may trigger onset.
UC affects all ages, genders, and races but follows these patterns.
Ulcerative Colitis vs. Other Conditions
| Feature | Ulcerative Colitis | Crohn’s Disease | Microscopic Colitis |
|---|---|---|---|
| Affected Area | Colon/rectum (continuous) | Any GI tract (skip lesions) | Colon (microscopic) |
| Depth | Mucosa only | Full thickness | Mucosa (normal gross) |
| Common Symptoms | Bloody diarrhea | Non-bloody diarrhea, fistulas | Watery diarrhea |
This table highlights key distinctions for accurate diagnosis.
Complications of Ulcerative Colitis
Untreated UC risks severe issues:
- Dehydration/anemia: From chronic bloody diarrhea.
- Bone loss (osteoporosis): Due to malabsorption/steroids.
- Colon cancer: Long-term inflammation elevates risk.
- Strictures/fistulas: Scar tissue or abnormal connections.
- Primary sclerosing cholangitis: Liver/bile duct inflammation.
Diagnosis and When to See a Doctor
Diagnosis involves colonoscopy, biopsy, blood/stool tests, and imaging to rule out infections/cancer. Seek care for persistent diarrhea (>4 weeks), rectal bleeding, abdominal pain, or unexplained weight loss. Early intervention prevents complications.
Treatment Overview
No cure exists, but treatments induce remission: anti-inflammatories (mesalamine), corticosteroids, immunomodulators, biologics, Janus kinase inhibitors, and surgery (colectomy) for refractory cases. Diet, stress management, and probiotics aid symptom control.
Living with Ulcerative Colitis
Manage flares with trigger avoidance, balanced nutrition (supplements if needed), exercise, and mental health support. Track symptoms via apps/journals. Support groups like Mayo Clinic Connect foster community.
Frequently Asked Questions (FAQs)
What causes ulcerative colitis?
Unknown exactly, but involves immune dysfunction, genetics, microbiome dysbiosis, and environment.
Is ulcerative colitis genetic?
Partly; family history raises risk via multiple genes.
Does diet cause UC?
No, but certain foods worsen symptoms.
Can stress trigger UC flares?
Stress doesn’t cause UC but aggravates symptoms by impacting immunity/gut function.
Who is at risk for ulcerative colitis?
Those under 30, with family history, white/Ashkenazi Jewish ethnicity.
Is UC curable?
No, but manageable with treatments for remission.
References
- Ulcerative colitis – Symptoms and causes — Mayo Clinic. 2023-10-12. https://www.mayoclinic.org/diseases-conditions/ulcerative-colitis/symptoms-causes/syc-20353326
- Symptoms & Causes of Ulcerative Colitis — National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). 2023-07-25. https://www.niddk.nih.gov/health-information/digestive-diseases/ulcerative-colitis/symptoms-causes
- Ulcerative Colitis: Causes, Symptoms and Treatment Options — American Journal of Public Health International. 2023. https://ajphi.org/ajphi/article/view/40
Read full bio of medha deb











