Upper Abdominal Pain: Causes, Symptoms & Treatment
Understanding upper abdominal pain: Digestive, biliary, and muscular causes explained.
What is Upper Abdominal Pain?
Upper abdominal pain refers to discomfort or pain that occurs in the area of your belly roughly between your ribs and your belly button. This region is medically significant because it contains numerous vital organs and systems that can be sources of pain. Healthcare providers divide the abdomen into specific regions to help narrow down the many possible causes of abdominal pain. Understanding which region is affected helps guide diagnosis and treatment decisions.
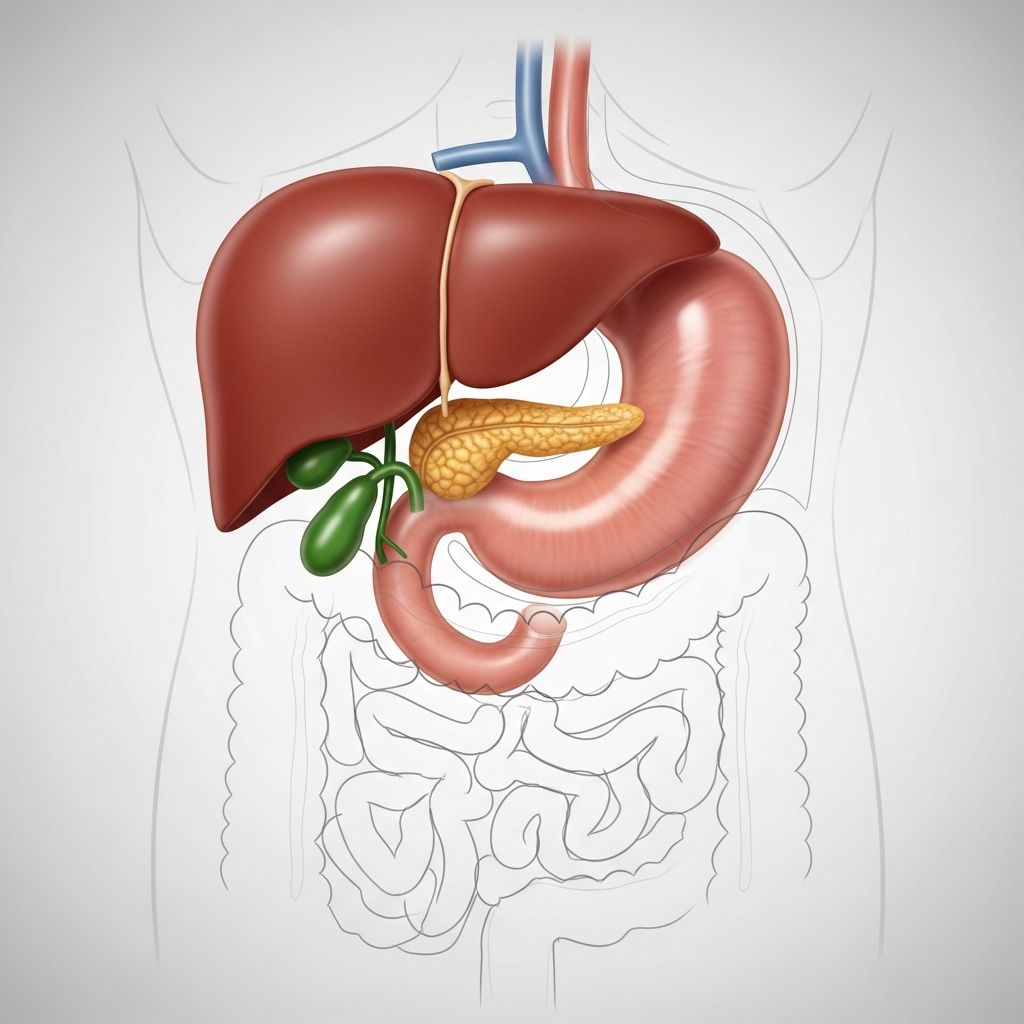
Your upper abdomen is the largest cavity in your body, containing several important organs including your stomach, liver, pancreas, gallbladder, spleen, and parts of your intestines. When you experience upper abdominal pain, it’s more likely to be related to the organs located in that specific region. The pain could literally be a simple stomachache related to digestion, but it could also involve your biliary system—the network of organs responsible for bile production and storage—or even your muscles.
Common Causes of Upper Abdominal Pain
Upper abdominal pain most often involves your digestive system or your biliary system, but sometimes it’s something else entirely. Understanding the various causes can help you better communicate your symptoms to a healthcare provider and potentially identify the underlying issue.
Digestive System Issues
The digestive system is one of the primary sources of upper abdominal pain. Several conditions can cause discomfort in this region:
Indigestion (Dyspepsia): Indigestion is pain or discomfort that happens while your stomach digests food. It’s also called dyspepsia, which means impaired digestion. Occasional indigestion is common and not serious. If you get a stomachache after a large meal, you can usually relieve it with an antacid. But if you have indigestion often, there might be more going on. Sometimes, it means you have a treatable condition, like acid reflux or peptic ulcer disease. Most people have occasional indigestion. For others, it happens often enough to affect daily life.
The most common cause of indigestion is stomach acid—especially when there’s too much of it or when it gets where it doesn’t belong. Acid can irritate the lining of your stomach, esophagus or small intestine, causing that familiar burning or painful sensation. This extra acid often results from underlying conditions like GERD (acid reflux) or peptic ulcer disease, which are among the most common causes of chronic indigestion.
Peptic Ulcer Disease: Peptic ulcers are sores that develop on the lining of your stomach or small intestine. The classic symptom is burning epigastric pain after meals. Pain that occurs immediately after meals is a classic symptom of gastric ulcer. Pain that occurs 2 to 3 hours after meals and that is relieved by food or antacids is a strong indicator of duodenal ulcer. Other symptoms include dyspepsia, bloating, distention, heartburn, and chest discomfort.
Functional Dyspepsia: When testing rules out acid-related disease, the diagnosis is often functional dyspepsia—a condition where overly sensitive gut nerves misinterpret normal digestion as pain or discomfort. Typical symptoms of dyspepsia include burning stomach pain, over-fullness and bloating. These symptoms resemble peptic ulcer disease or GERD.
Gas and Bloating: Excess gas can cause abdominal pain, cramping or a feeling of fullness or tightness (bloating). Your belly may feel like an overinflated balloon on the verge of popping.
Biliary System Disorders
Your biliary system, which includes your gallbladder and bile ducts, is another common source of upper abdominal pain, particularly in the upper right quadrant:
Biliary Colic: Biliary colic is a pattern of periodic abdominal pain that’s caused by an obstruction in your biliary tract, usually in your bile ducts or gallbladder. This is intermittent abdominal pain that comes from your biliary tract, usually from your gallbladder or bile ducts. You might feel it under your right ribcage or in your right shoulder. It’s often accompanied by nausea. Biliary colic pain is typically intermittent, moderate to severe, and may last from 30 minutes to several hours. Most people feel the pain in their upper abdomen, under their right ribcage, which is where your gallbladder and most of your biliary system are located. But it can also radiate to your right shoulder or back.
Cholecystitis: In cholecystitis, the primary complaint is pain, usually in the right upper quadrant of the abdomen. Patients describe sudden, sharp, and intense pain that radiates to the back or shoulder. Patients may report pain after heavy meals, and some report nausea and vomiting.
Other Potential Causes
Beyond digestive and biliary issues, upper abdominal pain can stem from several other sources including liver problems, pancreatic inflammation, mesenteric ischemia (reduced blood flow to the intestines), musculoskeletal issues, or even referred pain from conditions affecting other areas of your body.
Symptoms Associated with Upper Abdominal Pain
The symptoms you experience alongside upper abdominal pain can provide important clues about the underlying cause. Healthcare providers define indigestion (dyspepsia) by specific symptoms that typically show up within minutes to a few hours after a meal.
Many people who experience upper abdominal pain also report additional symptoms, including:
- Nausea or vomiting
- Bloating or feeling unusually full
- Heartburn or acid reflux
- Belching or gas
- Changes in bowel habits
- Loss of appetite
- Fatigue or weakness
These symptoms can overlap with various conditions, or they may occur on their own. The specific combination of symptoms you experience can help your healthcare provider narrow down potential causes.
Red-Flag Symptoms Requiring Emergency Care
While most cases of upper abdominal pain are manageable with conservative treatment, certain warning signs require immediate medical attention. Sometimes, a heart attack can feel like indigestion—called a silent heart attack. Seek emergency care if you have upper abdominal pain along with:
- Chest pain or pressure
- Severe, sudden onset pain
- Pain accompanied by shortness of breath
- Vomiting blood
- Blood in your stool
- Persistent or worsening pain despite treatment
- Fever combined with abdominal pain
- Jaundice (yellowing of skin and eyes)
- Signs of severe dehydration
Diagnostic Approaches for Upper Abdominal Pain
If your upper abdominal pain is mild or only happens once in a while, you probably don’t need a formal diagnosis. But if it’s frequent, severe or interfering with your daily life, your provider will start by asking about your symptoms. They’ll likely begin with a comprehensive history, asking about when the pain started, what makes it better or worse, what it feels like, and what other symptoms accompany it.
Your healthcare provider will also inquire about your medical history, current medications, dietary habits, stress levels, and lifestyle factors. This information helps them build a complete picture of your condition.
Physical Examination
During a physical examination, your provider will palpate (feel) your abdomen to identify areas of tenderness, swelling, or masses. They may also listen with a stethoscope to check for normal bowel sounds. For certain conditions, they may perform specialized exams such as digital rectal exams for gastrointestinal or prostate issues, pelvic exams for gynecological issues, or other targeted assessments.
Diagnostic Testing
In some cases, your provider may prescribe acid-blocking medication first to see if it helps. If it does, your symptoms are likely related to stomach acid. If it doesn’t—or if you have other concerning symptoms—your provider may recommend further testing to check for an underlying condition.
Tests might include:
- Blood tests to check liver function, pancreatic enzymes, and other markers
- H. pylori testing to identify bacterial infection
- Upper gastrointestinal endoscopy to visualize the stomach and duodenum
- Ultrasound imaging of the abdomen
- CT scans for more detailed imaging
- Radiography with barium swallow studies
- Gastric emptying studies
Treatment Options for Upper Abdominal Pain
Treatment approaches depend on the underlying cause of your upper abdominal pain. If your symptoms are mild or occasional, you can often manage them with simple changes to your lifestyle and diet.
Lifestyle and Dietary Modifications
Simple changes can significantly improve symptoms for many people:
- Eat smaller, more frequent meals instead of large meals
- Avoid foods that trigger your symptoms, such as spicy or fatty foods
- Limit caffeine and alcohol consumption
- Avoid eating close to bedtime
- Manage stress through relaxation techniques, exercise, or meditation
- Maintain good posture, especially after eating
- Don’t smoke or use tobacco products
- Stay hydrated with water
Medications
If you have traditional acid-related indigestion, your provider may prescribe medications to reduce or manage stomach acid. These can include antacids, H2-receptor blockers, or proton pump inhibitors. These medications work by neutralizing or reducing stomach acid production, providing relief from symptoms.
Medications that reduce stomach acid are often effective, but they can have side effects. You may need to work with your provider to find the right balance between symptom relief and minimizing side effects. Depending on the underlying issue, you may need occasional or daily treatment—sometimes long-term.
When Medications May Not Help
If tests don’t show any clear cause and acid-reducing medications don’t help, your provider may diagnose functional dyspepsia. This diagnosis means your symptoms are real, but they’re not caused by a structural problem like an ulcer or clear acid reflux disease. In these cases, your healthcare provider may recommend other approaches, such as stress management techniques, dietary modifications, or medications that work on nerve function.
Prognosis and Long-Term Outlook
Not all causes of upper abdominal pain are curable, but most are treatable. The prognosis depends on the underlying condition causing your pain. Many people find significant relief through medication, lifestyle changes, or a combination of approaches.
For acid-related conditions like GERD or peptic ulcer disease, modern treatments are highly effective. For functional dyspepsia, while there may not be a cure, symptoms can often be well-managed with lifestyle modifications and appropriate medications.
Frequently Asked Questions
Q: How long does it normally take for the stomach to digest food?
A: It normally takes three to five hours for your stomach to digest food before passing it to your small intestine. During this time, your pancreas and gallbladder release enzymes and bile to help break food down.
Q: What should I do if I have mild upper abdominal pain after eating?
A: If you have occasional indigestion after eating, you can usually relieve it with an antacid or simple dietary changes. However, if the pain persists or becomes frequent, consult with a healthcare provider.
Q: When should I seek emergency care for upper abdominal pain?
A: Seek emergency care immediately if your upper abdominal pain is accompanied by chest pain, severe pain, vomiting blood, shortness of breath, or other red-flag symptoms that may indicate a serious condition.
Q: Can upper abdominal pain be a sign of a heart attack?
A: Yes, sometimes a heart attack can feel like indigestion, called a silent heart attack. This is why any severe upper abdominal pain accompanied by chest discomfort or other cardiac symptoms requires immediate medical attention.
Q: What is the difference between biliary colic and cholecystitis?
A: Biliary colic is intermittent pain caused by an obstruction in the biliary tract, while cholecystitis is inflammation of the gallbladder, typically causing more severe, persistent pain in the right upper quadrant.
Q: What lifestyle factors can increase my risk of upper abdominal pain?
A: Risk factors include smoking, excessive alcohol consumption, poor diet high in fatty or spicy foods, high stress levels, irregular eating patterns, and certain medications that affect stomach acid production.
References
- Upper Abdominal Pain — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/symptoms/24736-upper-abdominal-pain
- Indigestion (Dyspepsia): What It Is, Symptoms & Causes — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/symptoms/7316-indigestion-dyspepsia
- Biliary Colic: What It Is, Symptoms & Treatment — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/symptoms/biliary-colic
- Functional Dyspepsia: What It Is, Symptoms & Treatment — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/22248-functional-dyspepsia
- Acute Abdomen: What It Is, Symptoms & Causes — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/diseases/25064-acute-abdomen
- Not All Abdominal Pain is Gastrointestinal — Cleveland Clinic Journal of Medicine. 2016-01-01. https://www.ccjm.org/content/83/1/29
Read full bio of medha deb











