Ureteral Stents: Purpose, Procedure, Results & Removal
Complete guide to ureteral stents: how they work, placement procedure, recovery, and removal options.
Understanding Ureteral Stents
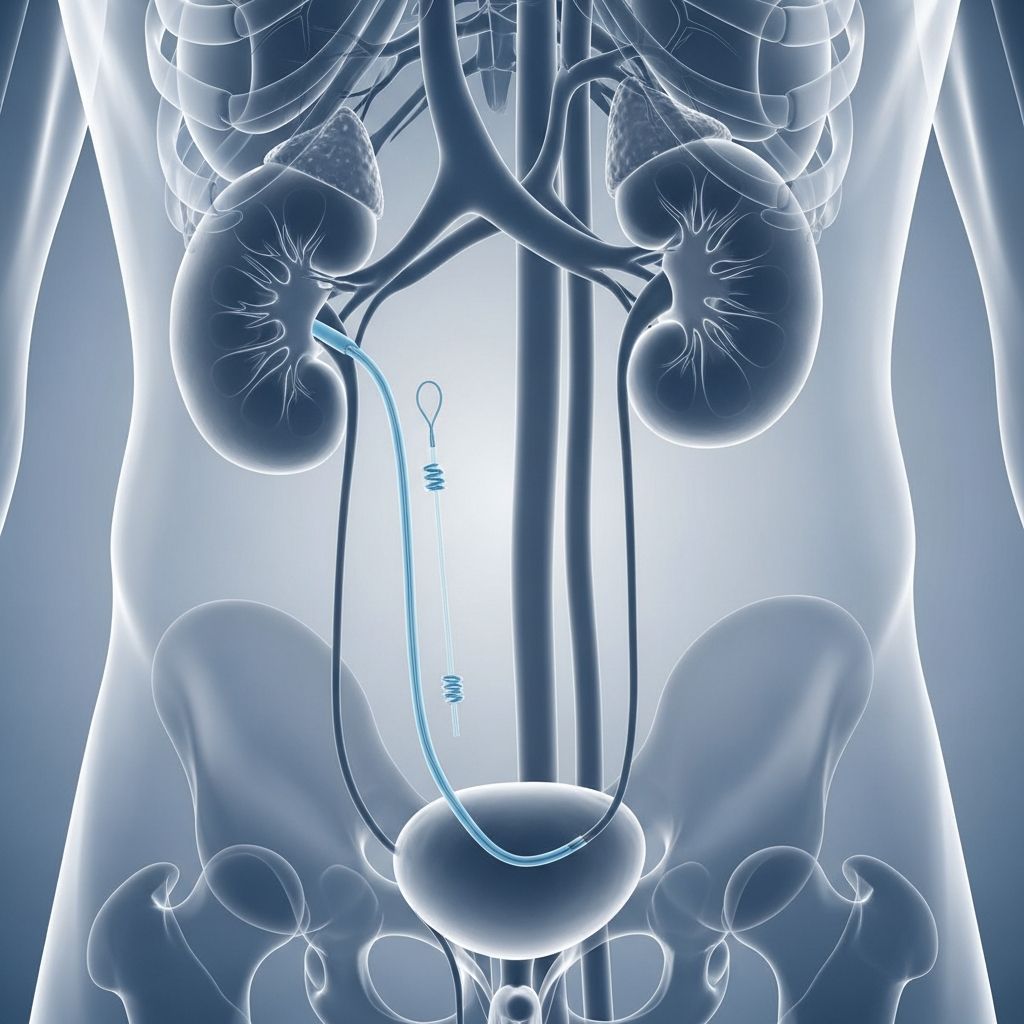
A ureteral stent is a small, flexible tube that plays a crucial role in modern urology by maintaining proper urine flow from your kidneys to your bladder. This minimally invasive device opens your ureter, allowing urine to pass freely even when obstructions, narrowed passages, or swelling would otherwise block the natural flow. Ureteral stents are temporary solutions in most cases, though some patients may require them for extended periods depending on their specific medical conditions.
What Is a Ureteral Stent?
A ureteral stent is a thin, hollow tube typically made of medical-grade plastic or silicone. The design of a ureteral stent is ingeniously simple yet effective. The stent has a coiled end that sits inside your kidney and a looped end that rests in your bladder. These two ends anchor the stent in place, ensuring it remains properly positioned throughout its duration in your body. The hollow center of the stent allows urine to flow around and through it, maintaining normal kidney and bladder function even when urinary pathways are compromised.
Purpose and Benefits of Ureteral Stenting
Ureteral stents serve several important medical purposes. They are used to treat various conditions affecting urinary flow and kidney function:
- Relief from urinary obstructions caused by kidney stones or debris
- Management of narrowed or strictured ureters
- Treatment of swelling in the urinary tract following surgery or injury
- Drainage assistance in cases of ureteral obstruction from tumors or other masses
- Prevention of urine backup into the kidneys, which can cause kidney damage
The benefits of ureteral stenting include protecting kidney function, reducing pain from urinary obstruction, preventing infection, and allowing healing in damaged urinary tissues. By maintaining proper urine flow, stents help prevent complications such as hydronephrosis, which occurs when urine backs up and causes kidney swelling.
The Ureteral Stent Placement Procedure
Pre-Procedure Preparation
Before undergoing ureteral stent placement, your healthcare provider will explain the procedure in detail and obtain your informed consent. A comprehensive physical examination ensures you are healthy enough for the procedure. Your medical team may request that you:
- Stop eating and drinking several hours before the procedure (fasting)
- Arrange for someone to drive you home, as general anesthesia will be used
- Wear comfortable, loose-fitting clothing
- Remove jewelry, glasses, and other personal items
- Inform your provider about current medications and allergies
The Placement Procedure
Ureteral stent placement is typically performed as a minimally invasive outpatient procedure, meaning you will return home the same day. The entire procedure usually takes less than 30 minutes, though you may spend several hours at the surgical center for preparation and post-operative monitoring.
Once you are asleep under general anesthesia, your urologist will use a cystoscope—a small, flexible camera—to visualize the inside of your bladder and ureter. Through this instrument, your doctor guides the ureteral stent into position. The coiled end of the stent is carefully placed inside your kidney, while the looped end is positioned in your bladder. These strategically designed ends anchor the stent securely, preventing migration or displacement. The entire stent remains inside your body and is not visible externally.
Recovery After Stent Placement
Immediate Recovery
After your urologist places the ureteral stent and removes the cystoscope, the anesthesiologist will discontinue anesthesia administration. You will regain consciousness after a few minutes, though you may feel groggy and disoriented initially. Medical staff will monitor your vital signs and manage any pain or discomfort with appropriate medications while you fully awaken.
Post-Procedure Care
During your recovery period, healthcare providers recommend:
- Drinking plenty of water over the next few days to support kidney and bladder function
- Taking prescribed pain medications as directed
- Resting and avoiding strenuous activity for at least a few days
- Refraining from lifting anything heavier than 10 pounds (approximately the weight of a gallon of water)
- Monitoring your urination patterns and urine color
Most people can return to their typical daily activities within one week after receiving a ureteral stent. However, individual recovery times may vary depending on the underlying condition and overall health status.
Managing Stent-Related Discomfort
Common Side Effects
While ureteral stents are generally well-tolerated, they can cause discomfort in some patients. Common side effects include urinary frequency, urgency, and burning sensations during urination. Some patients experience mild to moderate pain, which typically resolves within a few days to weeks. When you urinate, your bladder shrinks, and the looped end of the stent may rub against the bladder wall, causing this discomfort.
Additional side effects may include cramps in the kidney and bladder area, blood-tinged urine (which indicates the need to increase fluid intake), and mild discomfort in the lower back or abdomen.
Pain Management Strategies
Several effective strategies can help manage stent-related discomfort:
- Over-the-counter pain relievers such as ibuprofen or acetaminophen
- Prescription medications like tamsulosin (Flomax), which was originally designed for prostate problems but effectively reduces stent-related pain in both men and women
- Heating pads or warm baths to relieve localized pain and muscle tension
- Increased fluid intake to promote regular urination and reduce irritation
Your body’s reaction to a ureteral stent is unique. Some individuals experience only minor discomfort, while others feel more significant pain. Your healthcare provider can help develop a personalized pain management plan based on your specific needs and response to treatment.
Duration of Stent Placement
Temporary Stent Placement
In most cases, ureteral stents are temporary devices. Your urologist will remove the stent after your condition improves and normal urinary function is restored. For many patients, the stent remains in place for only a few days to a few weeks. The duration depends on the reason for placement, the severity of the obstruction or injury, and your body’s healing response.
Extended Stent Placement
Some patients may need to keep their ureteral stent for months or even years. This extended placement may be necessary if you have conditions such as tumors pressing on your ureters, chronically narrowed ureters, or recurrent obstructions. In these cases, your urologist will replace the stent every three to six months to prevent serious complications, including urinary tract infections and kidney stone formation.
Ureteral Stent Removal
Removal Procedure
When your condition has sufficiently improved, your urologist will remove the ureteral stent. The most common removal method uses a cystoscope, the same instrument used for placement. Your doctor inserts this small, flexible scope through the urethra to visualize and remove the stent. The entire removal process typically takes only 2 to 3 minutes and is performed under local anesthesia, making it a quick and minimally invasive procedure.
Preparation for Stent Removal
Before stent removal, your healthcare provider may recommend:
- Drinking 3 to 4 cups of water before the procedure
- Taking prescribed pain relievers before arrival
- Taking medications to relax the ureter as directed by your physician
- Arranging for transportation home if sedation is used
Post-Removal Recovery
During stent removal, the area will be numbed with topical anesthetic, so you should feel minimal pain during the procedure itself. However, many patients experience moderate discomfort or pain after the numbing medication wears off. This discomfort typically subsides within a few days. You may notice some blood-tinged urine or mild burning with urination, which is normal and should resolve quickly.
String Removal at Home
In some cases, a ureteral stent may have a small string extending from the urethra. If your stent has this feature, your doctor may allow you to remove it yourself at home. However, this should only be done following explicit instructions from your healthcare provider. Your doctor will inform you of the correct timing for removal and provide detailed, safe guidelines to ensure proper removal technique.
Potential Risks and Complications
While ureteral stents are generally safe, potential risks include infection, bleeding, and injury to the ureter. The risk of major injury requiring extensive surgical repair is approximately one in 1,000 cases. Bacterial colonization of the stent can lead to urinary tract infections, particularly if the stent remains in place for extended periods. Regular stent replacement every 3 to 6 months significantly reduces the likelihood of infection and other complications.
Your healthcare provider will discuss your individual risk factors and provide guidance on managing any concerning symptoms that may develop while the stent is in place. Prompt reporting of fever, severe pain, inability to urinate, or signs of infection ensures rapid intervention if complications arise.
Frequently Asked Questions
Q: How long does it take to place a ureteral stent?
A: The actual stent placement procedure typically takes less than 30 minutes. However, you should plan to spend several hours at the surgical center for pre-operative preparation and post-operative monitoring before discharge.
Q: Will I need anesthesia for stent removal?
A: Stent removal typically uses local anesthesia, making it a quick outpatient procedure. The numbing medication ensures minimal discomfort during the removal process, which usually takes just 2-3 minutes.
Q: Can I return to work after stent placement?
A: Most people can return to typical daily activities within one week. However, avoid strenuous activities and heavy lifting for at least a few days. Your urologist can provide specific recommendations based on your job and condition.
Q: What should I do if I experience severe pain with the stent?
A: Contact your healthcare provider immediately if you develop severe pain, fever, inability to urinate, or persistent bleeding. These symptoms may indicate complications requiring urgent evaluation and treatment.
Q: How do I know if my stent is working properly?
A: Normal stent function is indicated by regular urination, clear or slightly blood-tinged urine initially, and gradual resolution of any back pain related to obstruction. Your healthcare provider will monitor stent function through imaging and clinical assessment.
Q: Are there alternatives to ureteral stents?
A: Depending on your condition, alternatives may include percutaneous nephrostomy, ureteroscopy with stone removal, or observation with medical management. Your urologist will discuss the most appropriate treatment option for your specific situation.
References
- Ureteral Stent: Purpose, Procedure, Results & Removal — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/treatments/21795-ureteral-stents
- Ureteroscopy + Kidney Stones — Cleveland Clinic. 2024. https://my.clevelandclinic.org/health/treatments/16213-ureteroscopy
- Ureteral Stent Removal: Steps & Recovery — Riyadh Fakeeh Care. 2024. https://en.dsfhriyadh.fakeeh.care/blog/ureteral-stent-removal-steps-recovery
- Less-Invasive Ways to Remove Stones from the Kidneys and Ureters — Canadian Canadian Journal of Medicine, 2009. https://www.ccjm.org/content/ccjom/76/10/592.full.pdf
- Ureteral Stent: What to Expect and How to Manage — Music Urology. 2022. https://musicurology.com/wp-content/uploads/2022/02/MUSIC-ROCKS-Stent-Leaflet_EMR-friendly.pdf
Read full bio of Sneha Tete













