Uterine Fibroids: Causes, Symptoms, and Treatment Options
Comprehensive guide to understanding uterine fibroids, their symptoms, diagnosis, and available treatment options.
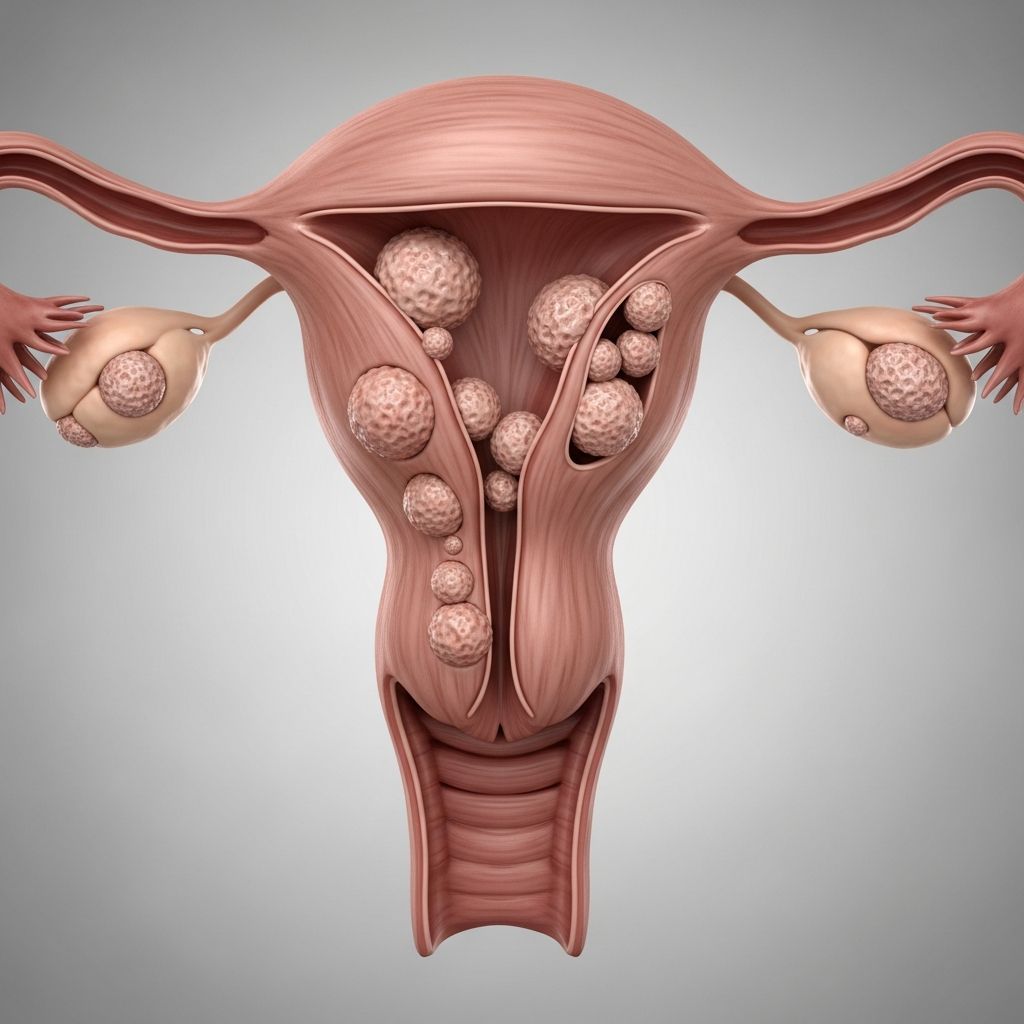
Understanding Uterine Fibroids
Uterine fibroids are noncancerous growths that develop in the muscular wall of the uterus, known as the myometrium. These benign tumors are among the most common pelvic tumors found in women of reproductive age. One in every four women experience symptoms related to uterine fibroids during their lifetime, making this condition a significant health concern for many. While fibroids are not life-threatening, they can substantially impact quality of life through various symptoms and complications.
Fibroids vary dramatically in size, number, and location within the uterus. Some women may have a single small fibroid that causes no symptoms, while others develop multiple large fibroids that significantly affect their daily activities and reproductive health. Understanding the nature of fibroids, their classification, and available treatment options empowers women to make informed decisions about their healthcare.
What Are Uterine Fibroids?
Uterine fibroids are solid, compact, benign tumors composed of smooth muscle cells and fibrous connective tissue. They develop in or on the uterus and can range in size from microscopic to several inches in diameter. Despite their potential to grow quite large, fibroids remain noncancerous and do not develop into cancer.
The prevalence of uterine fibroids is higher than many women realize. By age 50, approximately 70-80% of women will have developed at least one fibroid, though not all will experience symptoms. The condition is more common in African American women and those with a family history of fibroids, suggesting both genetic and racial factors play a role in fibroid development.
Classification and Location of Fibroids
Fibroids are classified based on their location within and around the uterus. This classification is clinically important because location directly determines symptoms and influences treatment decisions.
Types of Fibroids by Location
Submucosal Fibroids: These fibroids develop just beneath the innermost lining of the uterus (endometrium). They extend into the uterine cavity and are closest to where menstrual tissue sheds monthly. Submucosal fibroids can be pedunculated, meaning they hang from a stalk like a polyp. These fibroids most commonly cause abnormal uterine bleeding and heavy menstrual periods.
Intramural Fibroids: Located entirely within the muscular wall of the uterus, intramural fibroids are the most common type, accounting for approximately 60% of all cases. These fibroids can enlarge the uterus and may distort the uterine cavity, particularly if they grow toward the inner lining. Large intramural fibroids can press on surrounding organs and contribute to pelvic pressure and pain.
Subserosal Fibroids: These fibroids develop on the outer surface of the uterus, beneath the peritoneum. They can extend outward, sometimes appearing on stalks (pedunculated), giving them a distinctive appearance. Subserosal fibroids may cause pelvic pressure but typically do not affect menstrual bleeding significantly.
Symptoms and Complications
Fibroid symptoms vary considerably among women and depend on the size, number, and location of growths. Many women with fibroids experience no symptoms at all and discover them incidentally during routine pelvic examinations or imaging studies.
Common Symptoms Include:
Heavy Menstrual Bleeding: Submucosal and intramural fibroids, particularly those close to the uterine lining, frequently cause excessive menstrual bleeding. Women may experience periods lasting longer than seven days, soaking through one or more pads or tampons every hour, or passing blood clots larger than a quarter. This excessive bleeding can lead to iron-deficiency anemia over time.
Pelvic Pain and Pressure: Large fibroids or multiple fibroids can enlarge the uterus significantly, creating sensations of heaviness, pressure, or fullness in the pelvis and lower abdomen. This pressure may worsen during menstruation and can interfere with normal activities.
Dysmenorrhea: Many women with fibroids experience severe menstrual cramps and pain during periods. This pain can be debilitating and significantly reduce quality of life.
Urinary and Bowel Dysfunction: When fibroids enlarge the uterus substantially, they can press on adjacent organs including the bladder and bowel. This pressure may cause urinary frequency or urgency, difficulty emptying the bladder completely, or constipation and other gastrointestinal symptoms.
Fertility and Pregnancy Complications: Fibroids that distort the uterine cavity can interfere with egg implantation and embryo development, potentially affecting fertility. Some women with fibroids experience difficulty conceiving, though many achieve pregnancy successfully. During pregnancy, fibroids may increase the risk of miscarriage, preterm labor, abnormal fetal position, and cesarean delivery.
Diagnosis of Uterine Fibroids
Clinical Evaluation
Diagnosis often begins when women report symptoms such as heavy bleeding or pelvic pain. During a pelvic examination, healthcare providers may detect an enlarged or irregularly shaped uterus, raising suspicion for fibroids. A thorough medical history including menstrual patterns, pain characteristics, and family history provides important diagnostic clues.
Imaging Techniques
Pelvic Ultrasound: Transvaginal or transabdominal pelvic ultrasound is typically the first imaging modality used to diagnose fibroids. This non-invasive technique uses sound waves to create images of the uterus and surrounding structures. Ultrasound can identify fibroids, determine their size and location, and count the number of growths present. This information is essential for treatment planning.
Magnetic Resonance Imaging (MRI): MRI provides more detailed imaging than ultrasound and is particularly useful when ultrasound findings are inconclusive or when treatment planning requires precise anatomical information. MRI can clearly delineate fibroid location relative to the uterine cavity and adjacent organs, making it valuable for surgical planning.
Hysterosalpingography (HSG): This radiographic technique involves injecting contrast dye into the uterus through the cervix to visualize the uterine cavity and fallopian tubes. HSG is particularly useful for evaluating women with fertility concerns, as it can demonstrate how fibroids distort the cavity.
Treatment Options
Treatment decisions for uterine fibroids depend on multiple factors including symptom severity, fibroid characteristics, desire for future pregnancy, age, and personal preferences. Many effective treatment options exist, ranging from conservative management to definitive surgical interventions.
Watchful Waiting
For women with asymptomatic fibroids or mild symptoms, periodic monitoring without active treatment may be appropriate. Regular pelvic examinations and imaging studies every 1-2 years can track fibroid growth. Many fibroids grow slowly or remain stable, particularly after menopause when estrogen levels decline.
Medical Management
Nonsteroidal Anti-inflammatory Drugs (NSAIDs):strong> Over-the-counter NSAIDs such as ibuprofen and naproxen can reduce menstrual pain and cramping associated with fibroids. These medications do not reduce fibroid size but provide symptomatic relief for many women.
Hormonal Contraceptives: Oral contraceptive pills and hormonal intrauterine devices (IUDs) containing progestin can help regulate menstrual bleeding and reduce heavy periods. These methods do not shrink existing fibroids but can minimize bleeding-related symptoms.
Gonadotropin-Releasing Hormone (GnRH) Agonists: These medications suppress estrogen and progesterone production, effectively stopping menstruation and causing fibroid shrinkage. GnRH agonists can reduce fibroid volume by 40-60% but are typically used short-term due to side effects similar to menopause, including hot flashes and bone loss.
Selective Progesterone Receptor Modulators: Newer medications in this class show promise in reducing fibroid size and controlling bleeding with fewer side effects than GnRH agonists.
Minimally Invasive Procedures
Uterine Artery Embolization (UAE):strong> This interventional radiologic procedure involves injecting particles into the uterine arteries that supply fibroids, cutting off their blood supply. The fibroids shrink over time as they lose their vascular support. UAE is effective for symptom relief and can preserve the uterus for future pregnancy, though pregnancy outcomes may be affected.
Magnetic Resonance-Guided Focused Ultrasound (MRgFUS):strong> This innovative technique uses ultrasound waves guided by MRI imaging to precisely target and destroy fibroid tissue without surgical incisions. Treatment is performed as an outpatient procedure with minimal downtime.
Hysteroscopic Myomectomy: For submucosal fibroids, this minimally invasive surgical technique involves removing fibroids protruding into the uterine cavity through the cervix. The procedure preserves the uterus and can improve fertility prospects.
Surgical Interventions
Abdominal or Laparoscopic Myomectomy: This surgery involves removing fibroids while preserving the uterus. It is the preferred surgical approach for women desiring future pregnancy. Recovery is more extensive than minimally invasive procedures, but the procedure effectively removes fibroid tissue.
Hysterectomy: Complete removal of the uterus is the definitive treatment for uterine fibroids, as fibroids cannot recur without the uterus. Hysterectomy is appropriate for women who have completed childbearing or do not desire future pregnancy. This procedure can be performed abdominally, vaginally, or laparoscopically.
Frequently Asked Questions
Can uterine fibroids become cancerous?
No. Uterine fibroids are benign growths and do not transform into cancer. However, a rare malignant smooth muscle tumor called leiomyosarcoma can occur in the uterus. This condition is distinct from fibroids and occurs independently.
Do all women with fibroids need treatment?
No. Women with asymptomatic fibroids may not require treatment and can be monitored periodically. Treatment is individualized based on symptoms, fibroid characteristics, and personal preferences.
Can fibroids affect fertility?
Some fibroids can impact fertility, particularly submucosal fibroids that distort the uterine cavity. However, many women with fibroids conceive and carry pregnancies successfully. Consultation with a fertility specialist is recommended for women concerned about pregnancy prospects.
What happens to fibroids after menopause?
After menopause, when estrogen levels decline significantly, fibroids typically stop growing and may shrink. Symptoms often improve during this period.
Can fibroids recur after removal?
Following myomectomy, new fibroids can develop in approximately 20-30% of women within five years. Hysterectomy eliminates the possibility of recurrence since the uterus is removed.
References
- Understanding Endometriosis and Uterine Fibroids Webinar — Johns Hopkins Medicine. 2024. https://www.youtube.com/watch?v=99kd3p51nQA
- Uterine Fibroids: The Complete Guide — Elizabeth A. Stewart, Johns Hopkins Press. 2001. https://www.hopkinsmedicine.org
Read full bio of Sneha Tete











